Abstract
Myeloid-derived suppressor cells (MDSCs), major components maintaining the immune suppressive microenvironment in lung cancer, are relevant to the invasion, metastasis, and poor prognosis of lung cancer, through the regulation of epithelial-mesenchymal transition, remodeling of the immune microenvironment, and regulation of angiogenesis. MDSCs regulate T-cell immune functions by maintaining a strong immunosuppressive microenvironment and promoting tumor invasion. This raises the question of whether reversing the immunosuppressive effect of MDSCs on T cells can improve lung cancer treatment. To understand this further, this review explores the interactions and specific mechanisms of different MDSCs subsets, including regulatory T cells, T helper cells, CD8 + T cells, natural killer T cells, and exhausted T cells, as part of the lung cancer immune microenvironment. Second, it focuses on the guiding significance confirmed via clinical liquid biopsy and tissue biopsy that different MDSC subsets improve the prognosis of lung cancer. Finally, we conclude that targeting MDSCs through action targets or signaling pathways can help regulate T-cell immune functions and suppress T-cell exhaustion. In addition, immune checkpoint inhibitors targeting MDSCs may serve as a new approach for enhancing the efficiency of immunotherapy and targeted therapy for lung cancer in the future, providing better comprehensive options for lung cancer treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Various types of immune responses, including those in cancer, involve T cells, such as CD8+ T cells and CD4+ T helper (Th)1 cells. These T cells act as the main immune cells against cancer [1]. Particularly, CD8 + T cells are the main targets of immune checkpoint inhibitors (ICIs) within the immune microenvironment. Myeloid-derived suppressor cells (MDSCs) are major immune precursor cells that influence T-cell differentiation and immune function either directly or indirectly through interactions with T cells during the formation of the immunosuppressive microenvironment of a tumor, thus maintaining the immunosuppressive microenvironment of lung cancer. MDSCs mediate the epithelial-mesenchymal transition (EMT) and regulate the invasion and metastasis of lung cancer. They also weaken the efficacy of T-cell ICIs through immune regulation, which is an obstacle in immunotherapy [2]. The incidence and mortality rates of lung cancer are among the highest in the world [3], and a large amount of MDSCs often accumulate in the peripheral blood and tumor tissues of patients with lung cancer [4]. With the stage of lung cancer increasing over time, the degree of infiltration of MDSCs into the immune microenvironment of tumor tissues gradually increases, and the rise in the number of MDSCs is related to the degree of immunosuppression and a poor prognosis [5, 6]. Other suppressive or regulatory cells can be recruited and induced by MDSCs, such as regulatory T (Treg) cells, which inhibit the immune function of various T-cell types, including natural killer T (NKT) and CD8+ T cells, through multiple pathways. MDSCs can encourage the depletion of CD8+, CD4+, and memory T cells (T-cell exhaustion), thus affecting the immune function of patients with tumors. These findings raise the question of whether reversing the immunosuppressive effect of MDSCs on T cells can lead to improved lung cancer treatment. To understand this further, this study reviews recent research on the interactions and specific mechanisms of different MDSCs subsets, including Treg, Th, CD8+ T, NKT, and exhausted T cells, as part of the lung cancer immune microenvironment. The review also focuses on the guiding significance confirmed via clinical liquid biopsy and tissue biopsy that different MDSC subsets improve the prognosis of lung cancer.
2 Phenotype of MDSCs
MDSCs are heterogeneous immature bone marrow cell (IMC) populations at different stages of differentiation. Normally, IMCs differentiate into mature granulocytes, monocytes, and dendritic cells (DCs), after they migrate to peripheral organs. However, within the tumor microenvironment (TME), tumor cells and their targets such as STAT3, IRF8, C/EBPβ, and Notch can inhibit the differentiation of IMCs. Specific factors produced by activated T cells, tumor, and tumor stromal cells, such as VEGF, CSF, IL-6, IL-10, MMP-9, TGF-β, NF-kB, and other immune-suppressive mediators, can stimulate the proliferation and activation of MDSCs [7, 8]. Activated MDSCs selectively accumulate in the peripheral blood and tumor tissues from patients with cancer and exert immunosuppressive activity [8].
Animal experiments have shown that MDSCs express different surface antigens in animals and humans. In 2010, Dolcetti proposed that MDSCs can be divided into two subgroups—monocytic MDSCs (M-MDSCs) and polymorphonuclear MDSCs (PMN-MDSCs)—and confirmed that MDSCs are a heterogenous population of cells that can be dissolved using Ly6C and Ly6G in mice [9]. MDSCs express the membrane antigens CD11b and Gr1 in mice and can be subdivided into two subpopulations based on different Gr1 epitopes: CD11b+Ly6G+Ly6Clow and CD11b+Ly6G−Ly6Chigh [10,11,12]. Haverkamp JM demonstrated that MDSCs can be defined independently of their phenotype [13]. In humans, MDSCs are of mainly two types: M-MDSCs and PMN-MDSCs, according to their differentiation. PMN-MDSCs are defined as CD11b+CD14−CD15+ or CD11b+CD14−CD66b+, whereas, M-MDSCs are defined as CD11b+ CD14+ CD15− HLA− DR−/low. Bronte et al. proposed naming a mixed group of MDSCs consisting of a greater number of immature progenitor cells with the phenotype of early stage MDSCs (e-MDSCs) [10, 12] (Table 1).
3 Significance of MDSCs in patients with lung cancer
Single-cell RNA-seq, flow cytometry, and cell mass spectrometry have been used to determine the heterogeneity of polymorphonuclear neutrophils (PMNs) in patients with lung cancer. PMN-MDSCs in such patients resemble activated PMN-MDSCs in mice in terms of genetic characteristics and have negative prognostic outcomes in the patients [14]. With the increasing number of clinical histopathology and liquid biopsy studies, previous studies on the phenotypes of MDSCs in tumor tissues or peripheral blood from patients with non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC) have been diverse, as shown in Table 2. Despite the different phenotypes studied, the percentage of MDSCs in the tumor tissues and peripheral blood of patients with lung cancer is found to be increased, compared with that in healthy people. With an increase in the stage of lung cancer, the degree of MDSC infiltration into the tumor tissue immune microenvironment gradually increases. Compared with early stage patients, advanced stage patients have higher concentrations of MDSCs present in their peripheral blood [5], and increased numbers of MDSCs are linked with the degree of immunosuppression and a poor prognosis [6]. Patients with high MDSCs infiltration concentrations tend to have a shorter overall survival, lower survival rates, and poorer prognoses [15,16,17,18]. Kohsuke used single-cell level 16- or 17-color multiplex immunohistochemistry (mIHC) spatial analysis to assess the tumor immune microenvironment in patients with advanced NSCLC resistant to treatment with ICIs. The results demonstrated that resistance to ICIs was associated with a substantial infiltration of MDSCs and M2 type tumor-associated macrophages in the TME [19]. The immune function of lung cancer patients can be inhibited by a large amount of infiltration by MDSCs, promote disease progression and induce distant metastasis [20, 21]. In patients with elevated levels of MDSCs,their peripheral blood often exhibits resistance to multiple therapies such as immunotherapy, targeted therapy, and chemotherapy [22,23,24,25] (Table 2).
MDSCs and their specific molecules, such as TIE2+ [15], S100A9+ [22], PD-L1, and CCR5 [4], can be used as predictive markers for the recurrence and metastasis of lung cancer, and as monitoring indicators to judge the efficacy of chemotherapy, targeted therapy, and immunotherapy. MDSCs exert immunosuppressive effects by inhibiting T-cell function. Therefore, identifying the mechanism of the interaction between MDSCs and T cells and targeting MDSCs to inactivate them and reverse the failure of T cells and the treatment of lung cancer is dependent upon the body's immune function.
4 Interaction of MDSCs with T cells
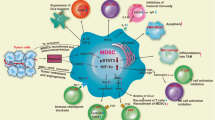
Activation of MDSCs is the major cause of lung cancer immune suppression. The mechanism of MDSC-mediated immunosuppression is closely related to the dysregulation of T-cell immune functions, and the mechanism by which MDSCs inhibit T-cell immune functions can be summarized as follows: (1) The immune function of T cells is inhibited by MDSCs by affecting the amino acid metabolism. MDSCs have been shown to affect amino acid metabolism in T cells; they consume arginine, cysteine, tryptophan, and other essential amino acids necessary for T-cell proliferation and activation; and they affect T-cell immune function. MDSCs deplete L( +)-arginine, which plays a critical role in T-cell activation and metabolism in the immune microenvironment, T-cell receptor (TCR) CD3ζ chain downregulation and signaling is due to a high expression of arginase 1 (ARG1) by the MDSCs, and T-cell dysfunction. In addition, L ( +)-arginine depletion prevents T cells from entering the G1 phase by inhibiting cyclin D3 expression, which induces T-cell cycle arrest [26, 27]. Cysteine is an indispensable amino acid for T-cell activation and function. Because T cells have a cysteine transporter defect, they can only obtain cysteine from antigen-presenting cells (APCs) such as macrophages and DCs, whereas MDSCs are known to compete with APCs for extracellular cysteine and do not export cysteines. It thereby prevents T-cell proliferation and activation [28]. MDSCs degrade the tryptophan required for T-cell proliferation to N-formyl epinephrine by overexpressing indoleamine 2,3-dioxygenase (IDO). The lack of tryptophan leads to the arrest of the T-cell cycle [29], which inhibits T-cells immune function. (2) MDSCs inhibit T cells immune functions by secreting a variety of reactive oxygen species and immunosuppressive factors. MDSCs express various enzymes involved in the production of reactive oxygen species (ROS) and nitric oxide (NO). The production of MDSCs induces the upregulation of Arg-1 activity and ROS production in a pathway dependent on Signal Transducers and Activators of Transcription 3 (STAT3). Indicating that the STAT3 activator signal plays a critical role in MDSC functions. Peroxynitrite (the product of ROS reacting with NO) alters TCR and CD8 molecules, and deprives cytotoxic T lymphocytes (CTLs) of the ability to specifically bind to the major histocompatibility complex (MHC) class I molecules, leading to further loss of their ability to kill tumor cells [30,31,32,33]. In addition, inducible NO synthase (iNOS) expressed by MDSCs can produce large amounts of NO, which blocks both the phosphorylation and the subsequent activation of IL-2 receptor-related proteins. NO also reduces the stability and release of IL-2 mRNA, further blocking the activation of T cells and inhibiting their proliferation [31, 34]. (3) MDSCs inhibit T-cell immune functions by elevating PD-L1 receptor expression. It is well known that the tumor immune microenvironment often presents an oxygen-deficient state, and in this hypoxic TME, hypoxia-inducible factor-1α (HIF-1α) is highly expressed. HIF-1α can induce programmed death ligand-1 (PD-L1) expression on the surface of MDSCs by binding to the programmed death factor-1 (PD-1) on the T-cell surface, which causes T-cell immune dysfunction and induces T-cell depletion and apoptosis [35, 36].
4.1 Immune regulation of Tregs by MDSCs
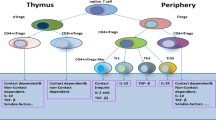
Tregs are a subgroup of CD4+ T lymphocytes cells that express CD25 and Foxp3 (CD4+CD25+ FoxP3+) [37], and are known for their modulatory effects on the T cell-killing function. Tregs exert a dual regulatory effect on T-cell autoimmunity. When Tregs inhibit T-cell death function, T cells display immune inertia, and the recognition of alloantigens and the production of cytotoxic particles and killer factors are weakened. When Tregs are known to promote T-cell immune activity, T cells will show immune hyperactivity and release excessive cytotoxic particles and killing factors, leading to the abnormal recognition of antigens, and even the killing of autologous cells. In the tumor immune microenvironment, owing to their ability to inhibit autogenic responses, Treg cells may impede antitumor immune responses. Moreover, specific depletion or functional changes in Treg cells can experimentally evoke effective tumor immunity [38]. Previous clinical studies have confirmed that a higher proportion of Tregs are found in the peripheral blood of patients with lung cancer [39, 40]. Tregs are key to the immune escape of lung cancer cells and are correlated with the progression and distant metastasis of lung cancer [41, 42]. At the same time, MDSCs and Tregs, two important immune cell populations in the immune microenvironment, also interact with each other. Granulocytes become sensitive to hypoxic conditions and are more likely to adopt immunosuppressive behaviors toward T cells [35]. Mark et al. found that in high-grade tumors, the immunosuppressive capacity of neutrophils is enhanced, and there is a tendency to interact with Treg cells [43]. MDSCs Isolated from in the peripheral blood of tumor-bearing mice have been shown to express elevated levels of chemokines such as CCL3, CCL4, and CCL5 [44], and the production of these chemokines is closely related to the recruitment of Tregs [44, 45]. Adoptive transfer experiments showed that MDSCs can induce Treg recruitment and generation and inhibit the antitumor T-cell response, while Treg cell content decreased significantly after treatment with anti-IL-10 or anti-IFN-γ [46], In a study conducted by Pan, the levels of IL-10 and TGF-β secreted by MDSCs were found to be significantly increased under IFN-γ stimulation, and the recruitment and production of Tregs also increased. Anti-CD40 was applied to inhibit CD40 expression on the MDSC surface and reduce the specific binding of MDSCs to the CD40 ligand (CD40L) expressed on Tregs, resulting in the reduction of the level of Treg expansion [47]. The application of IL-2/anti-CD40 effectively reduces the levels of Tregs and Treg-related chemokines in mice with tumors [48]. IL-10 and IFN-γ, as well as the expression of CD40 on the MDSC surface, are necessary for the development and expansion of Tregs. Furthermore, immunosuppressive factors like Arg1, NO, IL-10, and TGF-β produced by MDSCs can participate in the recruitment of Tregs by upregulating HIF-1α protein [49]. IL-10 can induce CD4+ T cells to express Foxp3 and increase the number of Tregs [50, 51]. It can also enhance the differentiation of Tregs and to promote their immune suppressive functions by promoting STAT3 phosphorylation [52]. TGF-β released from MDSCs can induce the expression of CD25 and Foxp3, and convert naive CD4 + T cells into Tregs [53, 54].
4.2 Interaction between MDSCs and Th cells
Th cells are different subsets formed from naive CD4 + cells upon activation. They produce cytokines and play important roles in immune regulation via the secreted cytokines. They can be divided into Th1, Th2, and Th17 cells, depending on the specific cytokines that they produce. Th1 cells regulate viruses, bacterial infections, and the development of specific autoimmunity and secrete vital cytokines such as INF-α, IFN-γ, and IL-12. Their immune action is mainly achieved through the activation of immune cells such as macrophages, CD8 + T, and NK cells, to mediate protective immune responses within the TME [55, 56]. The Th1/Th2 cell ratio differs in different diseases, and the proportion of Th2 cells in cancer patients is relatively high [57]. Additionally, Th2 cells mediate reactions such as parasitic infection, inflammation, and allergy, by promoting the humoral immune response and secreting cytokines such as IL-4, IL5, IL-10, and IL-13, which not only inhibit the Th1 cell immune tumor infiltrating T-cell response but also benefit Treg development. A large amount of Th2 aggregation is associated with the tumor escape mechanism [58]. Finally, Th17 cells are mainly responsible for bacterial-fungal infections and some autoimmune responses [58, 59]. However, the role of Th17 cells in the lung cancer immune microenvironment remains controversial. Martin-Orozco [60] found that Th17 cells can promote the recruitment of T cells to tumor sites, participate in antitumor immunity, and activate the production of CCL2 and CCL20 by secreting IL-17-activated border cells. These chemokines mobilize dendritic cells (DCs) and other leukocytes to the site of the tumor and further activate tumor-specific CD8+ T cells. Immunohistochemical tests among lung cancer patients showed that a large amount of immunosuppressive CD4+ T cells, including Th2 cells and Tregs, accumulated in the epithelium and stroma, whereas only a small number of Th1, Tfh, and Th17 cells were observed [61]. However, most studies have suggested that Th17 cells negatively affect the immune function in lung cancer patients. In lung cancer cells of mice, Th17 lymphocytes induce EMT, thereby promoting the migration and diffusion of metastases [62]. Peng et al. found that Th17 cell infiltration is linked to treatment resistance in patients with lung cancer. Th17 cells can secrete IL-17 and IL-22, which promote lung cancer cell metastasis and MEK inhibitor resistance [63]. In another study, the density of IL-17 producing cells in the tumor stroma was reported to be negatively correlated with the survival of NSCLC patients [64].
Promotive and inhibitory regulatory relationships exist among MDSCs and Th cells within the lung cancer TME. A mutual inhibitory relationship between MDSCs and Th1 cells has been reported. Coculture experiments have found that Th1 produces cytokines such as IL-2 and IFN-γ, which are capable of reducing the number of MDSCs and inhibiting their function by inducing the production of chemokines like CXCL9 and CXCL10, and reducing the levels of immune factors like IL-6 and IL-1β that promote MDSC proliferation and activation [65]. Yu et al. found that IDO expression in MDSCs isolated from tumor tissues was significantly upregulated and that MDSCs inhibited the polarization of Th1 cells by promoting IDO expression [66]. IFN-γ secreted by Th1 cells is an important cytokine that plays a significant role in inhibiting and killing tumor cells, as well as retarding the growth of tumors. TGF-β, secreted by MDSCs, is an immunosuppressive cytokine that is a key player in carcinogenesis and tumor progression. According to some studies, different mechanisms are used by TGF-β to inhibit the expression of IFN-γ in CD4+ Th1 cells at the time of initiation and recall [67], which then block the body’s autoimmune response to promote tumor growth and progression [68]. Additionally, with a reduction in MDSCs infiltration in the TME, Th1 polarization of CD4 + T cells increased, as did the cytotoxicity of CD8 + T cells [69]. In vivo and in vitro experiments have confirmed that MDSCs can promote the differentiation of Th2 cells, which may be achieved by the Th2-related immunosuppressive molecule IL-13 [70, 71]. Coculture experiments with MDSCs and Th17 cells showed that MDSCs promoted Th17 cell transformation into Tregs by secreting TGF-β and retinoic acid (RA). Thus, blocking RA or TGF-β can reduce the transformation of Th17 cells into Tregs [72].
4.3 CD8+ T-cells immune function is inhibited by MDSCs
Naive CD8+ T cells, after activation by APC and recognition by the TCR of peptide-specific MHC-I complexes, activate and differentiate into effector CTLs, which are then capable of targeting and killing cells (such as infected cells and cancer cells) and secreting protective cytokines [73]. In the TME, two key processes are involved in the antitumor effects of CD8+ T cells: migration and differentiation [74, 75]. Upon entry into the TME, the initial population of CD8+ T cells differentiates into effector CD8 + T cells, which are then activated and further differentiated into cytotoxic and memory CD8+ T cells [75, 76], During this process, transcription factors from the internal and external environments regulate the expression of their surface receptors and clones, and secrete many effectors to kill tumors in the microenvironment [75]. Tumor patients with lung cancer can induce immune dysfunction in CD8 + T cells and affect their immune function [77].
Increased numbers of MDSCs in patients with lung cancer may inhibit the generation of protective immune CD8+ T cells, and the highly expressed iNOS and L-arginase I (Arg-1) of MDSCs promote the downregulation of CD3ζ chain expression of CD8+ T cells and inhibit the immune function of CD8+ T cells [78]. MDSCs generate large quantities of ROS and peroxynitrite, and can also produce large amounts of NO, which can combine with ROS to form reactive nitrogen species (RNS). Moreover, it can interact with major histocompatibility complex class one (MHC-I) molecules, leading to a decrease in the response of CD8 + T cells to antigen-specific stimuli of tumors [79, 80]. The production of RNS can lead to post-translational modification of chemokine CCL2 and reduce the recruitment of CD8 + T cells in tumors [81], and inhibiting the generation of RNS can promote the function of CTLs [82]. Combining animal and in vitro experiments, studies have demonstrated that MDSCs in mouse tumors upregulated the expression of PD-L1 and secreted immunosuppressive cytokines due to hypoxia. MDSC-mediated inhibition of T-cell proliferation was enhanced in vivo, compared with that under normoxia [35]. Further, MDSCs upregulate PD-1 receptors on CD8+ T cells in vitro [5]. PD-1 receptor expression is a significant indicator of T-cell exhaustion. PD-1 interacts with its ligand, PD-L1, to reduce the proliferation and survival ability of CD8+ T cells and inhibit their secretion of cytokines, which in turn prevents CD8+ T cells from exerting their immune response, promotes resistance to ICIs, and promotes tumor progression. The oversecretion of IL-10 by MDSCs may inhibit the production of protective factors such as IL-2, IFN-γ, and IL-12 by CD8+ T cells, thereby inhibiting their proliferation, leading to impaired antitumor immunity, and inducing apoptosis of CD8+ T cells [50, 80]. There are contradictory claims regarding in the regulatory effect of IFN-γ on CD8+ T cells. CTLS may produce IFN-γ, which in turn may inhibit the immune function of CTLS [83], However, Wu et al. found that silymarin can reduce the level of IL-10 in the immune microenvironment of mice with lung cancer, as well as induce mRNA expression of nitric oxide synthase-2 (iNOS2), MMP9, and alginase -1 (Arg-1), further reducing the proportion of MDSCs and inhibiting their function. At the same time, IL-2 and IFN-γ levels were increased in mouse tumor sera, and the infiltration and function of CD8+ T cells were promoted [84], It has been demonstrated that interferon (IFN) promotes the increase of Treg cells and MDSCs in TME and is detrimental to the therapeutic effectiveness of PD-1 by inducing nitric oxide synthase 2 (NOS2) expression [33]. Schouppe demonstrated that MO-MDSC in the spleen could effectively reduce CTL-mediated antitumor immune function by increasing IFN-γ production, decreasing IL-2 responsiveness, affecting early CD8+ T-cell activation, reducing T-cell proliferation, and decreasing the expression of cytotoxic molecules [85].
Exosomes secreted by MDSCs deplete CD8 + T cells in mice. In vitro experiments have revealed that exosomes secreted by MDSCs can inhibit the proliferation of CD8+ T cells and induce apoptosis of CD8 + T cells by increasing ROS secretion and activating the Fas/Fas-L pathway [86]. This mechanism of action could involve iNOS expression and NO release, promoting CD8+ T-cell DNA damage and activating the p53 pathway [87]. In addition, MDSCs may influence the immune function of CD8+ T cells through transcription factors: Marigo's experimental study found that the immunomodulatory activity of MDSC was dependent on C/EBP-β transcription factors, and the immune tolerance of CD8+ T cells was reversed after C/EBP-β was cleared from the bone marrow of tumor mice [88].
4.4 Interaction between MDSCs and NKT cells
NKT cells are a subpopulation of T cells that express both the TCR and NK cell receptor NKR-P1. NKT cells produce large numbers of cytokines and, like NK cells, NKT cells can exert cytotoxic effects. They play immunomodulatory roles in cancer, autoimmunity, allergies, infections, and other diseases. Similar to Th1/Th2 cells, NKT cells can be divided into type I NKT cells for protective immunity, type II NKT cells for suppressing immunity, and invariant NKT (iNKT) cells. The glycolipid ligand galactose ceramide (GalCer) activates iNKT cells in a cd1-dependent manner [89, 90], and can secrete cell death-inducing factors such as perforin and Fas/FasL. It can also activate and recruit a variety of antitumor effector cells to the TME, which have direct and indirect antitumor activities and can increase the antitumor immune function of patients with lung cancer [91], The increased expression of CD11b, CD40, CD11c, CD86, and MHC II on MDSCs results from the interaction of α-GalCer presented by MDSCs with iNKT cells, which can be converted to immunostimulatory APCs upon presentation with α-GalCer and tumor antigens [92]. The injection of iNKT cell agonists into mice with tumors led to a significant reduction in the frequency of MDSCs and the removal of the immunosuppressive factor IL-10 from MDSCs, leading to an increase in the frequency of tumor-specific T cells as well as inhibiting tumor progression [93]. The immunosuppressive function of MDSCs is abrogated by INKT cells in a CD1d-dependent fashion and can not only manipulate MDSCs but can also promote the acquisition of resistance to MDSCs by CD8 + T cells during their proliferation in vitro [94]. The main protective role played based on type I NKT cells in autoimmunity is produced by the production of IFN-γ, while MDSCs can selectively reduce the production of IFN-γ by NKT cells through membrane-bound TGF-β, thereby inhibiting the immune function of type I NKT cells. The capacity of the NKT cells to produce IFN-γ is also restored after the depletion of MDSCs [95]. Type II NKT cells are lipid-specific CD1d-restricted T cells that do not normally recognize-GalCer. Type II NKT cells upregulate IL-13 expression to inhibit CTL-mediated tumor immune surveillance and tumor-specific CD8+ T cells, which are involved in cancer progression [96]. Type II NKT cells can induce TGF-β secretion from MDSCs by producing IL-13 [97,98,99], and blocking IL-13 or TGF-β.Eliminating NKT or myeloid cells may interrupt this immunosuppressive circuit and uncover immune surveillance to prevent tumor recurrence [97] (Fig. 1).
Interaction of MDSCs with T cells a MDSCs secrete IL-10 and TGF-β and express chemokines such as CCL3, CCL4 and CCL5 to promote the recruitment of Tregs; MDSCs express CD40 binding with CD40L on the surface of Tregs to promote the activation and expansion of Tregs. b The expression of IDO by MDSC inhibited the polarization of Th1 cells, and the production of TGF-β by MDSCs inhibited the function of Th1 cells. MDSCs promote Th2 cell differentiation through secretion of IL-13; MDSCs promote the transformation of Th17 cells into Treg cells by secreting TGF-β and RA. c MDSCs produce ROS and NO and secrete IL-10. Exosomes can inhibit CD8 + T cells’ function; MDSCs can upregulate PD-1 receptor on the surface of CD8 + T cells and promote CD8 exhaustion. d MDSCs inhibited the immune function of type I NKT cells by secreting TGF-β, and type II NKT cells inhibited the immune function of type I NKT cells by producing IL-13, and also induced MDSC to secrete TGF-β
4.5 MDSCs promote T-cell exhaustion
T-cell exhaustion refers to the excessive activation of T cells in response to persistent antigenic stimulation, such as viral or tumor stimulation, the continuous co-expressing multiple inhibitory receptors on their surfaces, the inactivation of cellular effector effects, and the inability to differentiate into memory T cells and perform immune functions, such as tumor cell killing or virus clearance. The most significant features are the loss of effector cytotoxic functions (decreased secretion of the antitumor cytokines IL-2, IFN-γ, and TNF-α), leading to changes in the expression of key transcriptional factors, and the upregulation or coexpression of multiple inhibitory molecular receptors (such as PD-1, BTLA, CTLA4, TIM-3, LAG3, TIGIT) [100, 101], and most current studies focus on CD8+ effector T cells. Under normal immune conditions, immunosuppressive molecule receptors can be temporarily expressed on the surface of activated effector T cells, but are quickly downregulated as T cells are activated. However, these inhibitory molecules cannot be downregulated during T-cell exhaustion and continue being strongly expressed on the effector T-cell surface. T-cell exhaustion is one of the major factors affecting the efficacy of immunotherapy; it not only causes effector T cells to lose their antitumor immune function but also causes ICIs and other immunotherapy methods to lose their roles and targets [102]. Studies have shown that patients with lung cancer with a high expression of exhausted T cells have a worse prognosis, and improving the exhaustion status of T cells can improve the therapeutic effect in patients with lung cancer [103].
General control nonderepressible (GCN) is a serine/threonine kinase found in eukaryotic cells that may influence bone marrow function by regulating metabolism or protein production. It is a key driver of macrophage and MDSC polarization within the TME. Halaby found that the ability of GCN2 cKO tumors to express the T-cell exhaustion ligands CD206 and PD-L1 was significantly decreased. Simultaneously, the expression levels of PD-1 in CD4 + and CD8 + T cells decreased significantly. Flow cytometry showed that the expression of PD-1, LAG3, TIM3, and TIGIT on the surface of CD8 + T cells also decreased significantly. Thus, GCN, which promotes the polarization of MDSCs, can induce T-cell exhaustion [104].
MDSCs negatively correlate with CD8+ T-cell expression in lung cancer patients, and MDSCs can directly induce CD8+ T cells to express T-cell exhaustion inhibitory receptors such as PD-1, TIGIT, LAG3, CTLA4, and TIM3 [5, 105, 106]. MDSCs in the blood of NSCLC patients can inhibit the immune function of T cells, promote T-cell exhaustion, and affect the effectiveness of immunotherapy by expressing Galectin-9, a ligand of Tim-3 [23]. CD155, expressed as MDSCs binds to TIGIT on CD8+ T cells, deprives effector T cells of glucose utilization, reduces the expression on CD8+ T cells, and inhibits antitumor functions [107].
MDSCs can cause T-cell cycle arrest by secreting IDO. However, the application of IDO1-shRNA to inhibit the expression of IDO1 in lung cancer mice downregulates the expression of the inhibitory receptors PD-1 and BTLA on T cells, positively regulates the secretion of cytokines such as IL-2 and TNF-α, reverses T-cell exhaustion, delays the onset of tumors, and inhibits tumor growth [108]. Cytokines secreted by MDSCs such as IL-10 and TGF-β are also associated with T-cell failure. IL-10 is a STAT-3 inducing cytokine that normally attenuates T-cell activation. IL-10 can produce various downstream effects through the IL-10R-STAT3 signaling pathway. Blocking the IL-10R-STAT3 signaling pathway can change the chromatin of CD8 + T cells, thereby promoting the activation of CD8 + T cells and inhibiting their exhaustion [109]. IL-10 may directly affect T cells through the STAT-3 pathway, indirectly affect T cells through APC regulation of T cells, or both. TGF-β, like IL-10, can activate downstream SMAD transcription factors to further attenuate or inhibit immune cell activation. Enhancement of the TGF-β signaling pathway results in a significant decrease in the number of antigen-specific CD8+ T cells and in the production of antitumor cytokines, both of which are evidence of CD8+ T-cell exhaustion [110, 111] The attenuation of TGF-β signaling increases the amount of antigen-specific CD8+ Tex cells, thereby enhancing viral control [100].
MDSCs can also induce T cells exhaustion through an immunosuppressive microenvironment. MDSCs can induce primary CD4+ T cells to proliferate and differentiate into Tregs and release immunosuppressive factors like TGF-β, IL-10 and IDO [112]. Transcription factors like Blimp-1 and T-bet are regulated by MDSCs, and promote the expression of immunosuppressive molecule receptors in effector T cells [113], or inhibit effector T-cell immune function through direct cell–cell contact, and assist tumor cells in evading immunity.
Memory T-cell exhaustion is a new direction in tumor immunotherapy research. The degree of exhaustion of early memory T cells and T cells has been reported to correlate with the therapeutic efficacy of chimeric antigen receptor (CAR) T cells [114]. Reversing T-cell exhaustion can restore memory T -cells functions, improve the efficacy of CAR-T cell therapy, and enhance the inhibitory effects of CAR-T cells on solid tumors [115]. Antigen-specific CD4+ or CD8+ T cellsare activated upon exposure to antigens and can differentiate into effector and memory T cells. Effector T cells bind specifically to antigens and memory T cells, which persist as a heterogeneous population at multiple sites, and can coordinate protective immune responses to re-exposure. There are two subgroups of memory T cells: central memory T cells (Tcm) and effector memory T cells (Tem). Tcm is primarily located in secondary lymphoid organs and can rapidly proliferate and differentiate into effector T-cells in response to antigens. Tem cells are mainly located in the peripheral tissues and can rapidly produce effector cytokines once stimulated by antigens [116]. Both Tem and Tcm respond rapidly to antigens, generating a variety of effector molecules, and generating effector and memory cells. There are also lymphocytes called stem memory T cells (TSCM), which are associated with the naive-like surface marker TCF-1 high memory T cells and memory precursor-like T cells [117]. They have a higher proliferative capacity, reorganize the immunodeficient host more effectively, and mediate a superior antitumor response [118]. TSCM is considered suitable for adoptive T-cell immunotherapy [119]. The metabolism of CD4+ and CD8+ memory T cells in lung cancer patients contributes to long-term immunity [120]. However, the oxidative stress response caused by the increased ROS produced by MDSCs can produce related free radicals and immunomodulatory cytokines, which can inhibit host CD8+ and CD4+ T-cell responses, thus promoting the metastasis and the progression of lung cancer [121, 122]. Intratumor-infiltrating MDSCs are able to induce CD4+ TEM PD-1 expression, which promotes CD4+ TEM exhaustion [123]. When MDSCs and ROS are exhausted in the TME, the percentages of Tem, Tcm, and TSCM increase significantly and rapidly, the cytotoxicity and activity of memory CD8+ T cells increase, and the STAT-3 pathway can also be activated to maintain long-term memory and improve antitumor immune mechanisms [124] (Fig. 2).
MDSCs and T-cell exhaustion. a MDSCs can induce CD8 + T cells to express T-cell exhaustion inhibitory receptors and secrete IDO, IL-10, and TGF-β to promote CD8 + T-cell exhaustion; b MDSCs can induce primary CD4 + T cells to differentiate and proliferate into Tregs; c MDSCs can induce PD-1 expression on Tem and promote CD4 + Tem depletion
4.6 MDSCs inhibit T cells immune function by promoting EMT
EMT refers to the morphological transformation of epithelial cells to a fibroblast or mesenchymal phenotype in response to physiological or pathological stimuli. Loss of cell polarity, rearrangement of the cytoskeleton, increased migratory motility, and resistance to apoptosis are important processes that mediate tumor invasion and metastasis [99]. When MDSCs are co-cultured with tumor cells, cancer cells undergo morphological, behavioral, and phenotypic changes that are typical of EMT. MDSCs can mediate EMT in the tumor cells of various cancers, thereby promoting tumor progression. MDSCs in the lung cancer microenvironment can activate the AKT and ERK signaling pathways by highly expressing chemokines such as CCL11, which promote NSCLC cell invasion and induce EMT, thus further promoting NSCLC metastasis [125]. Li [126] found that MDSCs in contact with tumor cells can enhance the expression of Cyclooxygenase-2 (COX-2) in tumor cells, activate the β-catenin/TCF4 pathway, and promote the occurrence of EMT in tumor cells. However, reducing iNOS and TGF-β expression can reverse the promoting effects of MDSCs on EMT. In vitro experiments by Toh et al. [127] have found that the expression of epidermal growth factor (EGF), hepatocyte growth factor (HGF), and TGF-β1 in MDSCs were significantly upregulated after coculture with tumor cells, while the inhibitory effect of MDSCs on the EMT of tumor cells was significantly decreased after simultaneous application of inhibitors of the above three factors. The results of these studies demonstrate that EGF, HGF, and TGF-β1 play important roles in the induction of EMT in PMN-MDSCs. The IL-6/STAT3 signaling pathway can effectively trigger EMT and increase the number of tumor stem cells [128]. A study by Panni [129] has shown that M-MDSCs play a significant role in promoting tumor stemness and EMT by regulating the STAT3 pathway through the secretion of IL-6, and MDSCs also induce angiogenesis in a STAT3-dependent manner [106]. Studies have also confirmed that Ginsenoside Rg3 (Rg3) can effectively reduce the incidence of tumor cell stemness and the EMT by depleting MDSCs in the tumor and downregulating the STAT3 pathway [130].
MDSCs can inhibit T-cell immune functions in various ways, and the EMT process mediated by MDSCs is linked to the reduction of CD4+ and CD8+ T cells in the TME, recruitment of Tregs, and the exhaustion of T cells [131, 132]. The occurrence of EMT promotes the predominant metabolism of tumor cells in an aerobic glycolytic manner, which promotes the formation of an acidic tumor environment and the activation of HIF-1α, a transcription factor related to hypoxia [133], and the HIF-1α protein can participate in the recruitment of Tregs [49]. EMT-activated tumor cells express low MHC-I levels and elevated PD-L1 levels, exhaust CD8 + T cells, and recruit Treg cells [134]. EMT is closely linked to the inflammatory lung adenocarcinoma TME. In lung adenocarcinoma with the EMT phenotype, inflammatory factors were secreted and there was increased infiltration of multiple T-cell-exhausted immune checkpoint molecules, including the increased infiltration of PD-1, BTLA, CTLA-4, and TIM-3, as well as CD4 + Foxp3 + Tregs [135]. High levels of TGF-β and IL-10 expression can directly inhibit the immune function of CD4+ and CD8+ T cells and promote CD4+FOXP3+ Treg differentiation, inhibiting the function of Th1 cells [136,137,138], and blocking TGF-β, which increases the infiltration of CD8 + T cells into the TME and reduces the levels of MDSCs and Tregs [139]. In addition, EMT is closely related to the mechanisms of drug resistance that occur during lung cancer treatment [140, 141] (Fig. 3).
4.7 Targeting MDSCs restores the immune function of T cells
Koh et al. used anti-Gr1 or anti-Ly6G to deplete MDSCs in mice with lung cancer; the activity and number of CD4+ and CD8+ T cells, memory T cells, and other immune cells were increased, and the secreted antitumor factors were also increased, which could promote the antitumor immune response [5, 6]. Studies have found that Resveratrol (RSV) can reduce the accumulation of MDSCs, promote their differentiation, induce the apoptosis of MDSCs, damage the inhibitory ability of CD8+ T cells, and improve antitumor immunity [142, 143]. Indomethacin (IND), a nonsteroidal anti-inflammatory drug, reduces tumor-induced MDSC accumulation, increases CD8+ T-cell infiltration, reduces Treg infiltration, alleviates chronic inflammation, and inhibits tumor progression and metastasis [144]. L-name, an iNOS inhibitor, can effectively reduce the recruitment and aggregation of MDSCs, and-galactosyl ceramide (GalCer) acts as a ligand for NKT cells. It enhances the host immune system by activating NKT cells. L-NAME combined with GalCer significantly increased the tumor antigen-specific response of mice with lung metastasis, increased the proportion of CD8+ T cells in the bronchoalveolar lavage fluid, and increased the antitumor effect of GalCer in a model of lung metastasis [145].
MDSCs immunosuppressive effect in the TME affects the long-term efficacy of lung cancer chemotherapy [146]. Gemcitabine combined with a superoxide dismutase (SOD) mimetic can reduce the activation of the IDO pathway, deplete MDSCs in mice with lung cancer, reduce Treg infiltration, inhibit CD8+ and CD4+ T-cell exhaustion, and improve the quantity and quality of memory T cells, to further promote the T-cell-mediated antitumor immune response and enhance the therapeutic efficacy of chemotherapy [124, 147].
ICIs have achieved some efficacy in NSCLC, and inhibitors targeting PD-L1 and/or PD-1 have been approved for use in NSCLC. Targeting PD-L1 and PD-1 increases tumor-specific T-cell immunity. PD-1/PD-L1 checkpoint inhibitors have demonstrated efficacy in advanced and refractory NSCLC in several clinical studies [148]. MDSCs can destroy the PD-1 therapy efficacy and depletion of MDSCs increases the amount of effector CD8+ T cells in multiple immune organs in mice, thereby enhancing the antitumor effect of anti-PD-1 treatment [149]. MEKi, CCL2 antagonists, entinostat, and other medications in conjunction with PD-1/PD-L1 mAbs can reduce the number of MDSCs, preventing differentiation of MDSCs, inhibiting immune function of MDSCs, and enhancing anti-PD-1 to induce an antitumor response. Moreover, it promotes antitumor immunity by enhancing CD4+ and CD8+ T-cell infiltration and inhibiting Treg cell expression (Table 3) [150,151,152].
5 Clinical application of targeting MDSCs to reshape lung cancer immune microenvironment
Products that target MDSCs have also been shown to have inhibitory effects on the number and function of MDSCs. One of the most prominent features of MDSCs is ARG1. In recent years, vaccination for antibodies against ARG1, coupled with inhibitors of the immune checkpoint, have been found to increase T-cell infiltration, restore the function of CD8 + T cells, and promote antitumor immune responses [153, 154]. Clinical evidence suggests that MDSCs, like anti-PD-1/PD-L1 and anti-CTLA-4, can weaken the response to immunotherapy. Tracking the dynamics of MDSCs during immunotherapy and controlling their expansion, recruitment, and function in tumors are crucial for treating immunotherapy-resistant patients [155]. ROS are also one of the products that influence the function of the MDSCs; the application of mitochondria-targeted and ultrasound-responsive PIO-NH nanoparticles can effectively improve hypoxia, inhibit ROS production, decrease the level of MDSCs in tumors, increase CD8+ T cell activity, activate the antitumor immune response, and inhibit metastasis [156]. There are relatively few clinical trials directly targeting MDSCs; however, clinical trials have investigated whether different drugs can decrease the number of MDSCs in peripheral blood from lung cancer patients (Table 4). PD-1 blockers can effectively eliminate MDSCs from the peripheral blood of NSCLC patients. Gemcitabine combined with the PD-1 blocker nivolumab can also effectively reduce MDSC levels in the peripheral blood from patients with NSCLC. All-trans retinoic acid (ATRA), which is used as a therapeutic compound targeting MDSCs, can deplete MDSCs in the TME [157]. Clinical studies have confirmed that patients with extensive-stage SCLC treated with ATRA and vaccinated with wild-type p53-transduced DC vaccines can effectively deplete MDSCs, increase the proportion of immune CD8+ T cells, promote antitumor immune responses, and enhance the effect of chemotherapy [158]. Currently, the number of clinical studies on MDSCs is relatively small and the number of patients included in the existing studies are relatively few. Therefore, multicenter studies with large sample sizes are required for more definitive results.
6 Conclusions
In general, MDSCs in the peripheral blood and tumor tissues of lung cancer patients are often higher than those of healthy people. MDSCs inhibit the T-cell immune functions by upregulating the immunosuppressive pathway and secreting immunosuppressive molecules and chemokines, which promote the immunosuppression and treatment resistance of lung cancer patients, which then leads to tumor progression and metastasis. Therefore, MDSCs have been identified as a major impediment in treating patients with lung cancer, and the depletion of MDSCs in the lung cancer microenvironment has certain clinical implications for the treatment of lung cancer. Drugs targeting MDSCs have been developed, but there are still many open questions about their mode and mechanism. The mechanism of relevant drugs should be clarified in future experiments to ensure positive results in all lung cancer patient populations.
Data availability
Not applicable.
Abbreviations
- APCs:
-
Antigen-presenting cells
- ARG1:
-
Arginase 1
- ATRA:
-
All-trans retinoic acid
- CD40L:
-
CD40 ligand
- CTL:
-
Cytotoxic T lymphocyte
- COX-2:
-
Cyclooxygenase-2
- EGF:
-
Epidermal growth factor
- EMT:
-
Epithelial mesenchymal transition
- GalCer:
-
α-Garactosyl ceramide
- HGF:
-
Hepatocyte growth factor
- HIF-1α:
-
Hypoxia inducible factor-1α
- IDO:
-
Indoleamine 2,3-dioxygenase
- IMC:
-
Immature myeloid cells
- IND:
-
Indomethacin
- iNOS:
-
Inducible nitric oxide synthase
- MDSCs:
-
Myeloid-derived suppressor cells
- MHC-I:
-
Major histocompatibility complex class one
- M-MDSCs:
-
Monocytic MDSCs
- NKT cell:
-
Natural killer T cells
- NO:
-
Nitric oxide
- NSCLC:
-
Non-small cell lung cancer
- PD-1:
-
Programmed death factor-1
- PD-L1:
-
Programmed death ligand-1
- PMN-MDSCs:
-
Polymorphonuclear MDSCs
- Rg3:
-
Ginsenoside Rg3
- RNS:
-
Reactive nitrogen species
- ROS:
-
Reactive oxygen species
- RSV:
-
Resveratrol
- SCLC:
-
Small cell lung cancer
- SOD:
-
Superoxide dismutase
- STAT3:
-
Signal transducers and activators of transcription3
- TCM:
-
Central memory T cells
- TCR:
-
T cell receptor
- TEM:
-
Effector memory T cells
- Th cell:
-
T helper cells
- Treg:
-
Regulatory T cells
- TSCM:
-
Stem memory T cells
- αGalCer:
-
α-Galactosylceramide
References
Speiser DE, Ho PC, Verdeil G. Regulatory circuits of T cell function in cancer. Nat Rev Immunol. 2016;16:599–611.
Talmadge JE, Gabrilovich DI. History of myeloid-derived suppressor cells. Nat Rev Cancer. 2013;13:739–52.
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 Countries. CA Cancer J Clin. 2021;71:209–49.
Yamauchi Y, Safi S, Blattner C, Rathinasamy A, Umansky L, Juenger S, Warth A, Eichhorn M, Muley T, Herth FJF, et al. Circulating and tumor myeloid-derived suppressor cells in resectable non-small cell lung cancer. Am J Respir Crit Care Med. 2018;198:777–87.
Koh J, Kim Y, Lee KY, Hur JY, Kim MS, Kim B, Cho HJ, Lee YC, Bae YH, Ku BM, et al. MDSC subtypes and CD39 expression on CD8(+) T cells predict the efficacy of anti-PD-1 immunotherapy in patients with advanced NSCLC. Eur J Immunol. 2020;50:1810–9.
Srivastava MK, Andersson Å, Zhu L, Harris-White M, Lee JM, Dubinett S, Sharma S. Myeloid suppressor cells and immune modulation in lung cancer. Immunotherapy. 2012;4:291–304.
Gabrilovich DI. Myeloid-derived suppressor cells. Cancer Immunol Res. 2017;5:3–8.
Gabrilovich DI, Nagaraj S. Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol. 2009;9:162–74.
Dolcetti L, Peranzoni E, Ugel S, Marigo I, Fernandez Gomez A, Mesa C, Geilich M, Winkels G, Traggiai E, Casati A, et al. Hierarchy of immunosuppressive strength among myeloid-derived suppressor cell subsets is determined by GM-CSF. Eur J Immunol. 2010;40:22–35.
Bronte V, Brandau S, Chen SH, Colombo MP, Frey AB, Greten TF, Mandruzzato S, Murray PJ, Ochoa A, Ostrand-Rosenberg S, et al. Recommendations for myeloid-derived suppressor cell nomenclature and characterization standards. Nat Commun. 2016;7:12150.
Hegde S, Leader AM, Merad M. MDSC: Markers, development, states, and unaddressed complexity. Immunity. 2021;54:875–84.
Veglia F, Perego M, Gabrilovich D. Myeloid-derived suppressor cells coming of age. Nat Immunol. 2018;19:108–19.
Haverkamp JM, Smith AM, Weinlich R, Dillon CP, Qualls JE, Neale G, Koss B, Kim Y, Bronte V, Herold MJ, et al. Myeloid-derived suppressor activity is mediated by monocytic lineages maintained by continuous inhibition of extrinsic and intrinsic death pathways. Immunity. 2014;41:947–59.
Veglia F, Hashimoto A, Dweep H, Sanseviero E, De Leo A, Tcyganov E, Kossenkov A, Mulligan C, Nam B, Masters G, et al. Analysis of classical neutrophils and polymorphonuclear myeloid-derived suppressor cells in cancer patients and tumor-bearing mice. J Exp Med. 2021. https://doi.org/10.1084/jem.20201803.
Lauret Marie Joseph E, Laheurte C, Jary M, Boullerot L, Asgarov K, Gravelin E, Bouard A, Rangan L, Dosset M, Borg C, Adotévi O. Immunoregulation and clinical implications of ANGPT2/TIE2(+) M-MDSC signature in non-small cell lung cancer. Cancer Immunol Res. 2020;8:268–79.
Barrera L, Montes-Servín E, Hernandez-Martinez JM, Orozco-Morales M, Montes-Servín E, Michel-Tello D, Morales-Flores RA, Flores-Estrada D, Arrieta O. Levels of peripheral blood polymorphonuclear myeloid-derived suppressor cells and selected cytokines are potentially prognostic of disease progression for patients with non-small cell lung cancer. Cancer Immunol Immunother. 2018;67:1393–406.
Vetsika EK, Koinis F, Gioulbasani M, Aggouraki D, Koutoulaki A, Skalidaki E, Mavroudis D, Georgoulias V, Kotsakis A. A circulating subpopulation of monocytic myeloid-derived suppressor cells as an independent prognostic/predictive factor in untreated non-small lung cancer patients. J Immunol Res. 2014;2014:659294.
de Goeje PL, Bezemer K, Heuvers ME, Dingemans AC, Groen HJ, Smit EF, Hoogsteden HC, Hendriks RW, Aerts JG, Hegmans JP. Immunoglobulin-like transcript 3 is expressed by myeloid-derived suppressor cells and correlates with survival in patients with non-small cell lung cancer. Oncoimmunology. 2015;4:e1014242.
Isomoto K, Haratani K, Tsujikawa T, Makutani Y, Kawakami H, Takeda M, Yonesaka K, Tanaka K, Iwasa T, Hayashi H, et al. Mechanisms of primary and acquired resistance to immune checkpoint inhibitors in advanced non-small cell lung cancer: A multiplex immunohistochemistry-based single-cell analysis. Lung Cancer. 2022;174:71–82.
Fu XG, Deng J, Xu WJ, Chen JY, Sun J, Deng H. Histidine decarboxylase-expressing PMN-MDSC-derived TGF-β1 promotes the epithelial-mesenchymal transition of metastatic lung adenocarcinoma. Int J Clin Exp Pathol. 2020;13:1361–71.
Li YD, Lamano JB, Lamano JB, Quaggin-Smith J, Veliceasa D, Kaur G, Biyashev D, Unruh D, Bloch O. Tumor-induced peripheral immunosuppression promotes brain metastasis in patients with non-small cell lung cancer. Cancer Immunol Immunother. 2019;68:1501–13.
Feng PH, Yu CT, Chen KY, Luo CS, Wu SM, Liu CY, Kuo LW, Chan YF, Chen TT, Chang CC, et al. S100A9(+) MDSC and TAM-mediated EGFR-TKI resistance in lung adenocarcinoma: the role of RELB. Oncotarget. 2018;9:7631–43.
Limagne E, Richard C, Thibaudin M, Fumet JD, Truntzer C, Lagrange A, Favier L, Coudert B, Ghiringhelli F. Tim-3/galectin-9 pathway and mMDSC control primary and secondary resistances to PD-1 blockade in lung cancer patients. Oncoimmunology. 2019;8:e1564505.
Bronte G, Petracci E, De Matteis S, Canale M, Zampiva I, Priano I, Cravero P, Andrikou K, Burgio MA, Ulivi P, et al. High levels of circulating monocytic myeloid-derived suppressive-like cells are associated with the primary resistance to immune checkpoint inhibitors in advanced non-small cell lung cancer: an exploratory analysis. Front Immunol. 2022;13:866561.
Wang S, Fu Y, Ma K, Liu C, Jiao X, Du W, Zhang H, Wu X. The significant increase and dynamic changes of the myeloid-derived suppressor cells percentage with chemotherapy in advanced NSCLC patients. Clin Transl Oncol. 2014;16:616–22.
Groth C, Hu X, Weber R, Fleming V, Altevogt P, Utikal J, Umansky V. Immunosuppression mediated by myeloid-derived suppressor cells (MDSCs) during tumour progression. Br J Cancer. 2019;120:16–25.
Rodriguez PC, Quiceno DG, Zabaleta J, Ortiz B, Zea AH, Piazuelo MB, Delgado A, Correa P, Brayer J, Sotomayor EM, et al. Arginase I production in the tumor microenvironment by mature myeloid cells inhibits T-cell receptor expression and antigen-specific T-cell responses. Cancer Res. 2004;64:5839–49.
Srivastava MK, Sinha P, Clements VK, Rodriguez P, Ostrand-Rosenberg S. Myeloid-derived suppressor cells inhibit T-cell activation by depleting cystine and cysteine. Cancer Res. 2010;70:68–77.
Fleming V, Hu X, Weber R, Nagibin V, Groth C, Altevogt P, Utikal J, Umansky V. Targeting myeloid-derived suppressor cells to bypass tumor-induced immunosuppression. Front Immunol. 2018;9:398.
Ohl K, Tenbrock K. Reactive oxygen species as regulators of MDSC-mediated immune suppression. Front Immunol. 2018;9:2499.
Gabrilovich DI, Ostrand-Rosenberg S, Bronte V. Coordinated regulation of myeloid cells by tumours. Nat Rev Immunol. 2012;12:253–68.
Bitsch R, Kurzay A, Özbay Kurt F, De La Torre C, Lasser S, Lepper A, Siebenmorgen A, Müller V, Altevogt P, Utikal J, Umansky V. STAT3 inhibitor Napabucasin abrogates MDSC immunosuppressive capacity and prolongs survival of melanoma-bearing mice. J Immunother Cancer. 2022;10(3):e004384. https://doi.org/10.1136/jitc-2021-004384.
Jacquelot N, Yamazaki T, Roberti MP, Duong CPM, Andrews MC, Verlingue L, Ferrere G, Becharef S, Vétizou M, Daillère R, et al. Sustained Type I interferon signaling as a mechanism of resistance to PD-1 blockade. Cell Res. 2019;29:846–61.
Macphail SE, Gibney CA, Brooks BM, Booth CG, Flanagan BF, Coleman JW. Nitric oxide regulation of human peripheral blood mononuclear cells: critical time dependence and selectivity for cytokine versus chemokine expression. J Immunol. 2003;171:4809–15.
Noman MZ, Desantis G, Janji B, Hasmim M, Karray S, Dessen P, Bronte V, Chouaib S. PD-L1 is a novel direct target of HIF-1α, and its blockade under hypoxia enhanced MDSC-mediated T cell activation. J Exp Med. 2014;211:781–90.
Lu C, Redd PS, Lee JR, Savage N, Liu K. The expression profiles and regulation of PD-L1 in tumor-induced myeloid-derived suppressor cells. Oncoimmunology. 2016;5:e1247135.
Whiteside TL. FOXP3+ Treg as a therapeutic target for promoting anti-tumor immunity. Expert Opin Ther Targets. 2018;22:353–63.
Wing JB, Tanaka A, Sakaguchi S. Human FOXP3(+) regulatory T cell heterogeneity and function in autoimmunity and cancer. Immunity. 2019;50:302–16.
Kurose K, Ohue Y, Sato E, Yamauchi A, Eikawa S, Isobe M, Nishio Y, Uenaka A, Oka M, Nakayama E. Increase in activated Treg in TIL in lung cancer and in vitro depletion of Treg by ADCC using an antihuman CCR4 mAb (KM2760). J Thorac Oncol. 2015;10:74–83.
Woo EY, Chu CS, Goletz TJ, Schlienger K, Yeh H, Coukos G, Rubin SC, Kaiser LR, June CH. Regulatory CD4(+)CD25(+) T cells in tumors from patients with early-stage non-small cell lung cancer and late-stage ovarian cancer. Cancer Res. 2001;61:4766–72.
Marshall EA, Ng KW, Kung SH, Conway EM, Martinez VD, Halvorsen EC, Rowbotham DA, Vucic EA, Plumb AW, Becker-Santos DD, et al. Emerging roles of T helper 17 and regulatory T cells in lung cancer progression and metastasis. Mol Cancer. 2016;15:67.
Ganesan AP, Johansson M, Ruffell B, Yagui-Beltrán A, Lau J, Jablons DM, Coussens LM. Tumor-infiltrating regulatory T cells inhibit endogenous cytotoxic T cell responses to lung adenocarcinoma. J Immunol. 2013;191:2009–17.
Sorin M, Rezanejad M, Karimi E, Fiset B, Desharnais L, Perus LJM, Milette S, Yu MW, Maritan SM, Doré S, et al. Single-cell spatial landscapes of the lung tumour immune microenvironment. Nature. 2023;614:548–54.
Wang X, Li X, Wei X, Jiang H, Lan C, Yang S, Wang H, Yang Y, Tian C, Xu Z, et al. PD-L1 is a direct target of cancer-FOXP3 in pancreatic ductal adenocarcinoma (PDAC), and combined immunotherapy with antibodies against PD-L1 and CCL5 is effective in the treatment of PDAC. Signal Transduct Target Ther. 2020;5:38.
Schlecker E, Stojanovic A, Eisen C, Quack C, Falk CS, Umansky V, Cerwenka A. Tumor-infiltrating monocytic myeloid-derived suppressor cells mediate CCR5-dependent recruitment of regulatory T cells favoring tumor growth. J Immunol. 2012;189:5602–11.
Huang B, Pan PY, Li Q, Sato AI, Levy DE, Bromberg J, Divino CM, Chen SH. Gr-1+CD115+ immature myeloid suppressor cells mediate the development of tumor-induced T regulatory cells and T-cell anergy in tumor-bearing host. Cancer Res. 2006;66:1123–31.
Pan PY, Ma G, Weber KJ, Ozao-Choy J, Wang G, Yin B, Divino CM, Chen SH. Immune stimulatory receptor CD40 is required for T-cell suppression and T regulatory cell activation mediated by myeloid-derived suppressor cells in cancer. Cancer Res. 2010;70:99–108.
Weiss JM, Back TC, Scarzello AJ, Subleski JJ, Hall VL, Stauffer JK, Chen X, Micic D, Alderson K, Murphy WJ, Wiltrout RH. Successful immunotherapy with IL-2/anti-CD40 induces the chemokine-mediated mitigation of an immunosuppressive tumor microenvironment. Proc Natl Acad Sci U S A. 2009;106:19455–60.
Li L, Yu R, Cai T, Chen Z, Lan M, Zou T, Wang B, Wang Q, Zhao Y, Cai Y. Effects of immune cells and cytokines on inflammation and immunosuppression in the tumor microenvironment. Int Immunopharmacol. 2020;88:106939.
Cheng JN, Yuan YX, Zhu B, Jia Q. Myeloid-derived suppressor cells: a multifaceted accomplice in tumor progression. Front Cell Dev Biol. 2021;9:740827.
Heo YJ, Joo YB, Oh HJ, Park MK, Heo YM, Cho ML, Kwok SK, Ju JH, Park KS, Cho SG, et al. IL-10 suppresses Th17 cells and promotes regulatory T cells in the CD4+ T cell population of rheumatoid arthritis patients. Immunol Lett. 2010;127:150–6.
Hsu P, Santner-Nanan B, Hu M, Skarratt K, Lee CH, Stormon M, Wong M, Fuller SJ, Nanan R. IL-10 potentiates differentiation of human induced regulatory T cells via STAT3 and Foxo1. J Immunol. 2015;195:3665–74.
Kanamori M, Nakatsukasa H, Okada M, Lu Q, Yoshimura A. Induced regulatory T cells: their development, stability, and applications. Trends Immunol. 2016;37:803–11.
Schramm C, Huber S, Protschka M, Czochra P, Burg J, Schmitt E, Lohse AW, Galle PR, Blessing M. TGFbeta regulates the CD4+CD25+ T-cell pool and the expression of Foxp3 in vivo. Int Immunol. 2004;16:1241–9.
Knutson KL, Disis ML. Tumor antigen-specific T helper cells in cancer immunity and immunotherapy. Cancer Immunol Immunother. 2005;54:721–8.
Zhu J. T helper cell differentiation, heterogeneity, and plasticity. Cold Spring Harb Perspect Biol. 2018;10(10):a030338. https://doi.org/10.1101/cshperspect.a030338.
Tatsumi T, Kierstead LS, Ranieri E, Gesualdo L, Schena FP, Finke JH, Bukowski RM, Mueller-Berghaus J, Kirkwood JM, Kwok WW, Storkus WJ. Disease-associated bias in T helper type 1 (Th1)/Th2 CD4(+) T cell responses against MAGE-6 in HLA-DRB10401(+) patients with renal cell carcinoma or melanoma. J Exp Med. 2002;196:619–28.
Hamilton DH, Bretscher PA. Different immune correlates associated with tumor progression and regression: implications for prevention and treatment of cancer. Cancer Immunol Immunother. 2008;57:1125–36.
Ji Y, Zhang W. Th17 cells: positive or negative role in tumor? Cancer Immunol Immunother. 2010;59:979–87.
Martin-Orozco N, Muranski P, Chung Y, Yang XO, Yamazaki T, Lu S, Hwu P, Restifo NP, Overwijk WW, Dong C. T helper 17 cells promote cytotoxic T cell activation in tumor immunity. Immunity. 2009;31:787–98.
Frafjord A, Buer L, Hammarström C, Aamodt H, Woldbæk PR, Brustugun OT, Helland Å, Øynebråten I, Corthay A. The immune landscape of human primary lung tumors is Th2 skewed. Front Immunol. 2021;12:764596.
Salazar Y, Zheng X, Brunn D, Raifer H, Picard F, Zhang Y, Winter H, Guenther S, Weigert A, Weigmann B, et al. Microenvironmental Th9 and Th17 lymphocytes induce metastatic spreading in lung cancer. J Clin Invest. 2020;130:3560–75.
Peng DH, Rodriguez BL, Diao L, Gaudreau PO, Padhye A, Konen JM, Ochieng JK, Class CA, Fradette JJ, Gibson L, et al. Th17 cells contribute to combination MEK inhibitor and anti-PD-L1 therapy resistance in KRAS/p53 mutant lung cancers. Nat Commun. 2021;12:2606.
Chen X, Wan J, Liu J, Xie W, Diao X, Xu J, Zhu B, Chen Z. Increased IL-17-producing cells correlate with poor survival and lymphangiogenesis in NSCLC patients. Lung Cancer. 2010;69:348–54.
Thakur A, Schalk D, Sarkar SH, Al-Khadimi Z, Sarkar FH, Lum LG. A Th1 cytokine-enriched microenvironment enhances tumor killing by activated T cells armed with bispecific antibodies and inhibits the development of myeloid-derived suppressor cells. Cancer Immunol Immunother. 2012;61:497–509.
Yu J, Du W, Yan F, Wang Y, Li H, Cao S, Yu W, Shen C, Liu J, Ren X. Myeloid-derived suppressor cells suppress antitumor immune responses through IDO expression and correlate with lymph node metastasis in patients with breast cancer. J Immunol. 2013;190:3783–97.
Lin JT, Martin SL, Xia L, Gorham JD. TGF-beta 1 uses distinct mechanisms to inhibit IFN-gamma expression in CD4+ T cells at priming and at recall: differential involvement of Stat4 and T-bet. J Immunol. 2005;174:5950–8.
Zamarron BF, Chen W. Dual roles of immune cells and their factors in cancer development and progression. Int J Biol Sci. 2011;7:651–8.
Pushalkar S, Hundeyin M, Daley D, Zambirinis CP, Kurz E, Mishra A, Mohan N, Aykut B, Usyk M, Torres LE, et al. The pancreatic cancer microbiome promotes oncogenesis by induction of innate and adaptive immune suppression. Cancer Discov. 2018;8:403–16.
Gabitass RF, Annels NE, Stocken DD, Pandha HA, Middleton GW. Elevated myeloid-derived suppressor cells in pancreatic, esophageal and gastric cancer are an independent prognostic factor and are associated with significant elevation of the Th2 cytokine interleukin-13. Cancer Immunol Immunother. 2011;60:1419–30.
Messmann JJ, Reisser T, Leithäuser F, Lutz MB, Debatin KM, Strauss G. In vitro-generated MDSCs prevent murine GVHD by inducing type 2 T cells without disabling antitumor cytotoxicity. Blood. 2015;126:1138–48.
Hoechst B, Gamrekelashvili J, Manns MP, Greten TF, Korangy F. Plasticity of human Th17 cells and iTregs is orchestrated by different subsets of myeloid cells. Blood. 2011;117:6532–41.
Zhang N, Bevan MJ. CD8(+) T cells: foot soldiers of the immune system. Immunity. 2011;35:161–8.
van der Leun AM, Thommen DS, Schumacher TN. CD8(+) T cell states in human cancer: insights from single-cell analysis. Nat Rev Cancer. 2020;20:218–32.
Reina-Campos M, Scharping NE, Goldrath AW. CD8(+) T cell metabolism in infection and cancer. Nat Rev Immunol. 2021;21:718–38.
Philip M, Schietinger A. CD8(+) T cell differentiation and dysfunction in cancer. Nat Rev Immunol. 2022;22:209–23.
Prado-Garcia H, Romero-Garcia S, Aguilar-Cazares D, Meneses-Flores M, Lopez-Gonzalez JS. Tumor-induced CD8+ T-cell dysfunction in lung cancer patients. Clin Dev Immunol. 2012;2012:741741.
Liu CY, Wang YM, Wang CL, Feng PH, Ko HW, Liu YH, Wu YC, Chu Y, Chung FT, Kuo CH, et al. Population alterations of L-arginase- and inducible nitric oxide synthase-expressed CD11b+/CD14−/CD15+/CD33+ myeloid-derived suppressor cells and CD8+ T lymphocytes in patients with advanced-stage non-small cell lung cancer. J Cancer Res Clin Oncol. 2010;136:35–45.
Nagaraj S, Gupta K, Pisarev V, Kinarsky L, Sherman S, Kang L, Herber DL, Schneck J, Gabrilovich DI. Altered recognition of antigen is a mechanism of CD8+ T cell tolerance in cancer. Nat Med. 2007;13:828–35.
Legorreta-Herrera M, Rivas-Contreras S, Ventura-Gallegos J, Zentella-Dehesa A. Nitric oxide is involved in the upregulation of IFN-γ and IL-10 mRNA expression by CD8+ T cells during the blood stages of P. chabaudi AS infection in CBA/Ca mice. Int J Biol Sci. 2011;7:1401–11.
Molon B, Ugel S, Del Pozzo F, Soldani C, Zilio S, Avella D, De Palma A, Mauri P, Monegal A, Rescigno M, et al. Chemokine nitration prevents intratumoral infiltration of antigen-specific T cells. J Exp Med. 2011;208:1949–62.
De Sanctis F, Lamolinara A, Boschi F, Musiu C, Caligola S, Trovato R, Fiore A, Frusteri C, Anselmi C, Poffe O, et al. Interrupting the nitrosative stress fuels tumor-specific cytotoxic T lymphocytes in pancreatic cancer. J Immunother Cancer. 2022;10(1):e003549. https://doi.org/10.1136/jitc-2021-003549.
Gallina G, Dolcetti L, Serafini P, De Santo C, Marigo I, Colombo MP, Basso G, Brombacher F, Borrello I, Zanovello P, et al. Tumors induce a subset of inflammatory monocytes with immunosuppressive activity on CD8+ T cells. J Clin Invest. 2006;116:2777–90.
Wu T, Liu W, Guo W, Zhu X. Silymarin suppressed lung cancer growth in mice via inhibiting myeloid-derived suppressor cells. Biomed Pharmacother. 2016;81:460–7.
Schouppe E, Mommer C, Movahedi K, Laoui D, Morias Y, Gysemans C, Luyckx A, De Baetselier P, Van Ginderachter JA. Tumor-induced myeloid-derived suppressor cell subsets exert either inhibitory or stimulatory effects on distinct CD8+ T-cell activation events. Eur J Immunol. 2013;43:2930–42.
Rashid MH, Borin TF, Ara R, Piranlioglu R, Achyut BR, Korkaya H, Liu Y, Arbab AS. Critical immunosuppressive effect of MDSC-derived exosomes in the tumor microenvironment. Oncol Rep. 2021;45:1171–81.
Cartwright ANR, Suo S, Badrinath S, Kumar S, Melms J, Luoma A, Bagati A, Saadatpour A, Izar B, Yuan GC, Wucherpfennig KW. Immunosuppressive myeloid cells induce nitric oxide-dependent DNA damage and p53 pathway activation in CD8(+) T cells. Cancer Immunol Res. 2021;9:470–85.
Marigo I, Bosio E, Solito S, Mesa C, Fernandez A, Dolcetti L, Ugel S, Sonda N, Bicciato S, Falisi E, et al. Tumor-induced tolerance and immune suppression depend on the C/EBPbeta transcription factor. Immunity. 2010;32:790–802.
Kawano T, Cui J, Koezuka Y, Toura I, Kaneko Y, Motoki K, Ueno H, Nakagawa R, Sato H, Kondo E, et al. CD1d-restricted and TCR-mediated activation of valpha14 NKT cells by glycosylceramides. Science. 1997;278:1626–9.
Brossay L, Chioda M, Burdin N, Koezuka Y, Casorati G, Dellabona P, Kronenberg M. CD1d-mediated recognition of an alpha-galactosylceramide by natural killer T cells is highly conserved through mammalian evolution. J Exp Med. 1998;188:1521–8.
Motohashi S, Okamoto Y, Yoshino I, Nakayama T. Anti-tumor immune responses induced by iNKT cell-based immunotherapy for lung cancer and head and neck cancer. Clin Immunol. 2011;140:167–76.
Ko HJ, Lee JM, Kim YJ, Kim YS, Lee KA, Kang CY. Immunosuppressive myeloid-derived suppressor cells can be converted into immunogenic APCs with the help of activated NKT cells: an alternative cell-based antitumor vaccine. J Immunol. 2009;182:1818–28.
Mussai F, De Santo C, Cerundolo V. Interaction between invariant NKT cells and myeloid-derived suppressor cells in cancer patients: evidence and therapeutic opportunities. J Immunother. 2012;35:449–59.
Kmieciak M, Basu D, Payne KK, Toor A, Yacoub A, Wang XY, Smith L, Bear HD, Manjili MH. Activated NKT cells and NK cells render T cells resistant to myeloid-derived suppressor cells and result in an effective adoptive cellular therapy against breast cancer in the FVBN202 transgenic mouse. J Immunol. 2011;187:708–17.
Zhang H, Li Z, Wang L, Tian G, Tian J, Yang Z, Cao G, Zhou H, Zhao L, Wu Z, Yin Z. Critical role of myeloid-derived suppressor cells in tumor-induced liver immune suppression through inhibition of NKT cell function. Front Immunol. 2017;8:129.
Ambrosino E, Terabe M, Halder RC, Peng J, Takaku S, Miyake S, Yamamura T, Kumar V, Berzofsky JA. Cross-regulation between type I and type II NKT cells in regulating tumor immunity: a new immunoregulatory axis. J Immunol. 2007;179:5126–36.
Terabe M, Berzofsky JA. Tissue-specific roles of NKT cells in tumor immunity. Front Immunol. 1838;2018:9.
Terabe M, Matsui S, Noben-Trauth N, Chen H, Watson C, Donaldson DD, Carbone DP, Paul WE, Berzofsky JA. NKT cell-mediated repression of tumor immunosurveillance by IL-13 and the IL-4R-STAT6 pathway. Nat Immunol. 2000;1:515–20.
Lamouille S, Xu J, Derynck R. Molecular mechanisms of epithelial-mesenchymal transition. Nat Rev Mol Cell Biol. 2014;15:178–96.
McLane LM, Abdel-Hakeem MS, Wherry EJ. CD8 T cell exhaustion during chronic viral infection and cancer. Annu Rev Immunol. 2019;37:457–95.
Dolina JS, Van Braeckel-Budimir N, Thomas GD, Salek-Ardakani S. CD8(+) T cell exhaustion in cancer. Front Immunol. 2021;12:715234.
Jiang W, He Y, He W, Wu G, Zhou X, Sheng Q, Zhong W, Lu Y, Ding Y, Lu Q, et al. Exhausted CD8+T cells in the tumor immune microenvironment: new pathways to therapy. Front Immunol. 2020;11:622509.
Kim CG, Kim G, Kim KH, Park S, Shin S, Yeo D, Shim HS, Yoon HI, Park SY, Ha SJ, Kim HR. Distinct exhaustion features of T lymphocytes shape the tumor-immune microenvironment with therapeutic implication in patients with non-small-cell lung cancer. J Immunother Cancer. 2021;9(12):e002780. https://doi.org/10.1136/jitc-2021-002780.
Halaby MJ, Hezaveh K, Lamorte S, Ciudad MT, Kloetgen A, MacLeod BL, Guo M, Chakravarthy A, Medina TDS, Ugel S, et al. GCN2 drives macrophage and MDSC function and immunosuppression in the tumor microenvironment. Sci Immunol. 2019. https://doi.org/10.1126/sciimmunol.aax8189.
Anestakis D, Petanidis S, Domvri K, Tsavlis D, Zarogoulidis P, Katopodi T. Carboplatin chemoresistance is associated with CD11b(+)/Ly6C(+) myeloid release and upregulation of TIGIT and LAG3/CD160 exhausted T cells. Mol Immunol. 2020;118:99–109.
Zhu H, Gu Y, Xue Y, Yuan M, Cao X, Liu Q. CXCR2(+) MDSCs promote breast cancer progression by inducing EMT and activated T cell exhaustion. Oncotarget. 2017;8:114554–67.
Wu L, Mao L, Liu JF, Chen L, Yu GT, Yang LL, Wu H, Bu LL, Kulkarni AB, Zhang WF, Sun ZJ. Blockade of TIGIT/CD155 signaling reverses T-cell exhaustion and enhances antitumor capability in head and neck squamous cell carcinoma. Cancer Immunol Res. 2019;7:1700–13.
Shang K, Wang Z, Hu Y, Huang Y, Yuan K, Yu Y. Gene silencing of indoleamine 2,3-dioxygenase 1 inhibits lung cancer growth by suppressing T-cell exhaustion. Oncol Lett. 2020;19:3827–38.
Hanna BS, Llaó-Cid L, Iskar M, Roessner PM, Klett LC, Wong JKL, Paul Y, Ioannou N, Öztürk S, Mack N, et al. Interleukin-10 receptor signaling promotes the maintenance of a PD-1(int) TCF-1(+) CD8(+) T cell population that sustains anti-tumor immunity. Immunity. 2021;54:2825-2841.e2810.
Gabriel SS, Tsui C, Chisanga D, Weber F, Llano-León M, Gubser PM, Bartholin L, Souza-Fonseca-Guimaraes F, Huntington ND, Shi W, et al. Transforming growth factor-β-regulated mTOR activity preserves cellular metabolism to maintain long-term T cell responses in chronic infection. Immunity. 2021;54:1698-1714.e1695.
Huang Y, Jia A, Wang Y, Liu G. CD8(+) T cell exhaustion in anti-tumour immunity: the new insights for cancer immunotherapy. Immunology. 2023;168:30–48.
Zhao Y, Wu T, Shao S, Shi B, Zhao Y. Phenotype, development, and biological function of myeloid-derived suppressor cells. Oncoimmunology. 2016;5:e1004983.
Sawant DV, Yano H, Chikina M, Zhang Q, Liao M, Liu C, Callahan DJ, Sun Z, Sun T, Tabib T, et al. Adaptive plasticity of IL-10(+) and IL-35(+) T(reg) cells cooperatively promotes tumor T cell exhaustion. Nat Immunol. 2019;20:724–35.
Fraietta JA, Lacey SF, Orlando EJ, Pruteanu-Malinici I, Gohil M, Lundh S, Boesteanu AC, Wang Y, O’Connor RS, Hwang WT, et al. Determinants of response and resistance to CD19 chimeric antigen receptor (CAR) T cell therapy of chronic lymphocytic leukemia. Nat Med. 2018;24:563–71.
Zhang X, Zhang C, Qiao M, Cheng C, Tang N, Lu S, Sun W, Xu B, Cao Y, Wei X, et al. Depletion of BATF in CAR-T cells enhances antitumor activity by inducing resistance against exhaustion and formation of central memory cells. Cancer Cell. 2022;40:1407-1422.e1407.
Farber DL, Yudanin NA, Restifo NP. Human memory T cells: generation, compartmentalization and homeostasis. Nat Rev Immunol. 2014;14:24–35.
Miron M, Kumar BV, Meng W, Granot T, Carpenter DJ, Senda T, Chen D, Rosenfeld AM, Zhang B, Lerner H, et al. Human lymph nodes maintain TCF-1(hi) memory t cells with high functional potential and clonal diversity throughout life. J Immunol. 2018;201:2132–40.
Gattinoni L, Lugli E, Ji Y, Pos Z, Paulos CM, Quigley MF, Almeida JR, Gostick E, Yu Z, Carpenito C, et al. A human memory T cell subset with stem cell-like properties. Nat Med. 2011;17:1290–7.
Gattinoni L, Speiser DE, Lichterfeld M, Bonini C. T memory stem cells in health and disease. Nat Med. 2017;23:18–27.
Hong H, Gu Y, Sheng SY, Lu CG, Zou JY, Wu CY. The distribution of human stem cell-like memory t cell in lung cancer. J Immunother. 2016;39:233–40.
Hiramoto K, Satoh H, Suzuki T, Moriguchi T, Pi J, Shimosegawa T, Yamamoto M. Myeloid lineage-specific deletion of antioxidant system enhances tumor metastasis. Cancer Prev Res (Phila). 2014;7:835–44.
Cruz-Bermúdez A, Laza-Briviesca R, Vicente-Blanco RJ, García-Grande A, Coronado MJ, Laine-Menéndez S, Alfaro C, Sanchez JC, Franco F, Calvo V, et al. Cancer-associated fibroblasts modify lung cancer metabolism involving ROS and TGF-β signaling. Free Radic Biol Med. 2019;130:163–73.
Dubinski D, Wölfer J, Hasselblatt M, Schneider-Hohendorf T, Bogdahn U, Stummer W, Wiendl H, Grauer OM. CD4+ T effector memory cell dysfunction is associated with the accumulation of granulocytic myeloid-derived suppressor cells in glioblastoma patients. Neuro Oncol. 2016;18:807–18.
Sawant A, Schafer CC, Jin TH, Zmijewski J, Tse HM, Roth J, Sun Z, Siegal GP, Thannickal VJ, Grant SC, et al. Enhancement of antitumor immunity in lung cancer by targeting myeloid-derived suppressor cell pathways. Cancer Res. 2013;73:6609–20.
Lin S, Zhang X, Huang G, Cheng L, Lv J, Zheng D, Lin S, Wang S, Wu Q, Long Y, et al. Myeloid-derived suppressor cells promote lung cancer metastasis by CCL11 to activate ERK and AKT signaling and induce epithelial-mesenchymal transition in tumor cells. Oncogene. 2021;40:1476–89.
Li ZL, Ye SB, OuYang LY, Zhang H, Chen YS, He J, Chen QY, Qian CN, Zhang XS, Cui J, et al. COX-2 promotes metastasis in nasopharyngeal carcinoma by mediating interactions between cancer cells and myeloid-derived suppressor cells. Oncoimmunology. 2015;4:e1044712.
Toh B, Wang X, Keeble J, Sim WJ, Khoo K, Wong WC, Kato M, Prevost-Blondel A, Thiery JP, Abastado JP. Mesenchymal transition and dissemination of cancer cells is driven by myeloid-derived suppressor cells infiltrating the primary tumor. PLoS Biol. 2011;9:e1001162.
Li L, Han R, Xiao H, Lin C, Wang Y, Liu H, Li K, Chen H, Sun F, Yang Z, et al. Metformin sensitizes EGFR-TKI-resistant human lung cancer cells in vitro and in vivo through inhibition of IL-6 signaling and EMT reversal. Clin Cancer Res. 2014;20:2714–26.
Panni RZ, Sanford DE, Belt BA, Mitchem JB, Worley LA, Goetz BD, Mukherjee P, Wang-Gillam A, Link DC, Denardo DG, et al. Tumor-induced STAT3 activation in monocytic myeloid-derived suppressor cells enhances stemness and mesenchymal properties in human pancreatic cancer. Cancer Immunol Immunother. 2014;63:513–28.
Song JH, Eum DY, Park SY, Jin YH, Shim JW, Park SJ, Kim MY, Park SJ, Heo K, Choi YJ. Inhibitory effect of ginsenoside Rg3 on cancer stemness and mesenchymal transition in breast cancer via regulation of myeloid-derived suppressor cells. PLoS ONE. 2020;15:e0240533.
Dudas J, Ladanyi A, Ingruber J, Steinbichler TB, Riechelmann H. Epithelial to mesenchymal transition: a mechanism that fuels cancer radio/chemoresistance. Cells. 2020;9(2):428. https://doi.org/10.3390/cells9020428.
Chae YK, Chang S, Ko T, Anker J, Agte S, Iams W, Choi WM, Lee K, Cruz M. Epithelial-mesenchymal transition (EMT) signature is inversely associated with T-cell infiltration in non-small cell lung cancer (NSCLC). Sci Rep. 2018;8:2918.
Taddei ML, Giannoni E, Comito G, Chiarugi P. Microenvironment and tumor cell plasticity: an easy way out. Cancer Lett. 2013;341:80–96.
Dongre A, Rashidian M, Reinhardt F, Bagnato A, Keckesova Z, Ploegh HL, Weinberg RA. Epithelial-to-mesenchymal transition contributes to immunosuppression in breast carcinomas. Cancer Res. 2017;77:3982–9.
Lou Y, Diao L, Cuentas ER, Denning WL, Chen L, Fan YH, Byers LA, Wang J, Papadimitrakopoulou VA, Behrens C, et al. Epithelial-mesenchymal transition is associated with a distinct tumor microenvironment including elevation of inflammatory signals and multiple immune checkpoints in lung adenocarcinoma. Clin Cancer Res. 2016;22:3630–42.
Zhang S. The role of transforming growth factor β in T helper 17 differentiation. Immunology. 2018;155:24–35.
Maimela NR, Liu S, Zhang Y. Fates of CD8+ T cells in tumor microenvironment. Comput Struct Biotechnol J. 2019;17:1–13.
Fan QM, Jing YY, Yu GF, Kou XR, Ye F, Gao L, Li R, Zhao QD, Yang Y, Lu ZH, Wei LX. Tumor-associated macrophages promote cancer stem cell-like properties via transforming growth factor-beta1-induced epithelial-mesenchymal transition in hepatocellular carcinoma. Cancer Lett. 2014;352:160–8.
Canè S, Van Snick J, Uyttenhove C, Pilotte L, Van den Eynde BJ. TGFβ1 neutralization displays therapeutic efficacy through both an immunomodulatory and a non-immune tumor-intrinsic mechanism. J Immunother Cancer. 2021;9(2):e001798. https://doi.org/10.1136/jitc-2020-001798.
Erin N, Grahovac J, Brozovic A, Efferth T. Tumor microenvironment and epithelial mesenchymal transition as targets to overcome tumor multidrug resistance. Drug Resist Updat. 2020;53:100715.
Tulchinsky E, Demidov O, Kriajevska M, Barlev NA, Imyanitov E. EMT: A mechanism for escape from EGFR-targeted therapy in lung cancer. Biochim Biophys Acta Rev Cancer. 2019;1871:29–39.
Zhao Y, Shao Q, Zhu H, Xu H, Long W, Yu B, Zhou L, Xu H, Wu Y, Su Z. Resveratrol ameliorates Lewis lung carcinoma-bearing mice development, decreases granulocytic myeloid-derived suppressor cell accumulation and impairs its suppressive ability. Cancer Sci. 2018;109:2677–86.
Zheng Y, Xu M, Li X, Jia J, Fan K, Lai G. Cimetidine suppresses lung tumor growth in mice through proapoptosis of myeloid-derived suppressor cells. Mol Immunol. 2013;54:74–83.
Blidner AG, Salatino M, Mascanfroni ID, Diament MJ, de Kier Bal, Joffé E, Jasnis MA, Klein SM, Rabinovich GA. Differential response of myeloid-derived suppressor cells to the nonsteroidal anti-inflammatory agent indomethacin in tumor-associated and tumor-free microenvironments. J Immunol. 2015;194:3452–62.
Ito H, Ando T, Seishima M. Inhibition of iNOS activity enhances the anti-tumor effects of alpha-galactosylceramide in established murine cancer model. Oncotarget. 2015;6:41863–74.
Adah D, Hussain M, Qin L, Qin L, Zhang J, Chen X. Implications of MDSCs-targeting in lung cancer chemo-immunotherapeutics. Pharmacol Res. 2016;110:25–34.
Schafer CC, Wang Y, Hough KP, Sawant A, Grant SC, Thannickal VJ, Zmijewski J, Ponnazhagan S, Deshane JS. Indoleamine 2,3-dioxygenase regulates anti-tumor immunity in lung cancer by metabolic reprogramming of immune cells in the tumor microenvironment. Oncotarget. 2016;7:75407–24.
Peters S, Gettinger S, Johnson ML, Jänne PA, Garassino MC, Christoph D, Toh CK, Rizvi NA, Chaft JE, Carcereny Costa E, et al. Phase II trial of atezolizumab as first-line or subsequent therapy for patients with programmed death-ligand 1-selected advanced non-small-cell lung cancer (BIRCH). J Clin Oncol. 2017;35:2781–9.
Feng J, Chen S, Li S, Wu B, Lu J, Tan L, Li J, Song Y, Shi G, Shi YG, Jiang J. The association between monocytic myeloid-derived suppressor cells levels and the anti-tumor efficacy of anti-PD-1 therapy in NSCLC patients. Transl Oncol. 2020;13:100865.
Lee JW, Zhang Y, Eoh KJ, Sharma R, Sanmamed MF, Wu J, Choi J, Park HS, Iwasaki A, Kaftan E, et al. The combination of MEK inhibitor with immunomodulatory antibodies targeting programmed death 1 and programmed death ligand 1 results in prolonged survival in Kras/p53-driven lung cancer. J Thorac Oncol. 2019;14:1046–60.
Wang Y, Zhang X, Yang L, Xue J, Hu G. Blockade of CCL2 enhances immunotherapeutic effect of anti-PD1 in lung cancer. J Bone Oncol. 2018;11:27–32.
Orillion A, Hashimoto A, Damayanti N, Shen L, Adelaiye-Ogala R, Arisa S, Chintala S, Ordentlich P, Kao C, Elzey B, et al. Entinostat neutralizes myeloid-derived suppressor cells and enhances the antitumor effect of PD-1 inhibition in murine models of lung and renal cell carcinoma. Clin Cancer Res. 2017;23:5187–201.
Aaboe Jørgensen M, Ugel S, Linder Hübbe M, Carretta M, Perez-Penco M, Weis-Banke SE, Martinenaite E, Kopp K, Chapellier M, Adamo A, et al. Arginase 1-based immune modulatory vaccines induce anticancer immunity and synergize with Anti-PD-1 checkpoint blockade. Cancer Immunol Res. 2021;9:1316–26.
Canè S, Barouni RM, Fabbi M, Cuozzo J, Fracasso G, Adamo A, Ugel S, Trovato R, De Sanctis F, Giacca M, et al. Neutralization of NET-associated human ARG1 enhances cancer immunotherapy. Sci Transl Med. 2023;15:eabq6221.
Peranzoni E, Ingangi V, Masetto E, Pinton L, Marigo I. Myeloid cells as clinical biomarkers for immune checkpoint blockade. Front Immunol. 2020;11:1590.
Ji C, Si J, Xu Y, Zhang W, Yang Y, He X, Xu H, Mou X, Ren H, Guo H. Mitochondria-targeted and ultrasound-responsive nanoparticles for oxygen and nitric oxide codelivery to reverse immunosuppression and enhance sonodynamic therapy for immune activation. Theranostics. 2021;11:8587–604.
Gabrilovich DI, Velders MP, Sotomayor EM, Kast WM. Mechanism of immune dysfunction in cancer mediated by immature Gr-1+ myeloid cells. J Immunol. 2001;166:5398–406.
Iclozan C, Antonia S, Chiappori A, Chen DT, Gabrilovich D. Therapeutic regulation of myeloid-derived suppressor cells and immune response to cancer vaccine in patients with extensive stage small cell lung cancer. Cancer Immunol Immunother. 2013;62:909–18.
Feng PH, Lee KY, Chang YL, Chan YF, Kuo LW, Lin TY, Chung FT, Kuo CS, Yu CT, Lin SM, et al. CD14(+)S100A9(+) monocytic myeloid-derived suppressor cells and their clinical relevance in non-small cell lung cancer. Am J Respir Crit Care Med. 2012;186:1025–36.
Zahran AM, Hetta HF, Zahran ZAM, Rashad A, Rayan A, Mohamed DO, Elhameed ZAA, Khallaf SM, Batiha GE, Waheed Y, et al. Prognostic role of monocytic myeloid-derived suppressor cells in advanced non-small-cell lung cancer: relation to different hematologic indices. J Immunol Res. 2021;2021:3241150.
Zhang G, Huang H, Zhu Y, Yu G, Gao X, Xu Y, Liu C, Hou J, Zhang X. A novel subset of B7–H3(+)CD14(+)HLA-DR(-/low) myeloid-derived suppressor cells are associated with progression of human NSCLC. Oncoimmunology. 2015;4:e977164.
Cheng Y, Li H, Zhao D, Han Q, Liu Y, Liu X, Ma L, Liu J. Identification and clinical significance of myeloid-derived suppressor cells in peripheral blood of small-cell lung cancer patients. Zhonghua Zhong Liu Za Zhi. 2014;36:592–6.
Tian T, Gu X, Zhang B, Liu Y, Yuan C, Shao L, Guo Y, Fan K. Increased circulating CD14(+)HLA-DR-/low myeloid-derived suppressor cells are associated with poor prognosis in patients with small-cell lung cancer. Cancer Biomark. 2015;15:425–32.
Huang A, Zhang B, Wang B, Zhang F, Fan KX, Guo YJ. Increased CD14(+)HLA-DR (-/low) myeloid-derived suppressor cells correlate with extrathoracic metastasis and poor response to chemotherapy in non-small cell lung cancer patients. Cancer Immunol Immunother. 2013;62:1439–51.
Wang J, Yang L, Yu L, Wang YY, Chen R, Qian J, Hong ZP, Su XS. Surgery-induced monocytic myeloid-derived suppressor cells expand regulatory T cells in lung cancer. Oncotarget. 2017;8:17050–8.
Acknowledgements
We sincerely thank all support from all authors.
Funding
This study was supported by National Natural Science Foundation of China (Nos. 82174465 and 82205226).
Author information
Authors and Affiliations
Contributions
BJH designed the research. CYZ, YWZ and YL performed literature search. SLH, JQH and BLS performed article selection and figure production. ZNH finished the manuscript draft. RZQ and BJH reviewed and edited the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
He, ZN., Zhang, CY., Zhao, YW. et al. Regulation of T cells by myeloid-derived suppressor cells: emerging immunosuppressor in lung cancer. Discov Onc 14, 185 (2023). https://doi.org/10.1007/s12672-023-00793-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12672-023-00793-1