Abstract
Objectives
Mindfulness is a proven therapeutic practice for reducing anxiety, depression, and chronic pain, which are factors that influence the success of hip/knee replacement surgery. The present study aimed to investigate the effect of mindfulness bibliotherapy in rehabilitation on anxiety, depression, and health status. The objective was to determine whether there is a connection between the level of mindfulness before rehabilitation and the health status after rehabilitation.
Method
Ninety-three patients (M age = 63.34, SD = 10.49) from an outpatient rehabilitation clinic participated in the study. Forty-three patients were included in the mindfulness bibliotherapy group, and 45 were included in the waitlist control group. Anxiety, depression (both measured with the Hospital Anxiety and Depression Scale), quality of life (measured with the SF-36), and walking ability (measured with the Timed “Up and Go”-Test), as well as orthopedic measurements and dispositional mindfulness, were measured before and after the intervention. A follow-up measurement was carried out 4 weeks after the end of rehabilitation.
Results
A significant interaction effect between test time (pre- and post-test) and group (mindfulness bibliotherapy and waitlist control group) was detected for the measurement of Anxiety. The Anxiety score decreased in the intervention group from the pre-test to the post-test and the follow-up. In addition, the five subscales of dispositional mindfulness, age, and gender predicted mental health status (measured with the mental health scale of the SF-36) at the end of rehabilitation, F(7, 85) = 2.52, p = 0.021, even though no individual predictor reached significance.
Conclusions
Mindfulness diary practice can be a helpful therapy approach to support patients and to regain the goal of full capacity for working life and everyday life after surgery. Further studies need to investigate more intensively the relationships between the mode of action of mindfulness interventions in the setting of orthopedic rehabilitation.
Preregistration
This study was preregistered in OSF (https://osf.io/4tmwq/).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
In 2021, over 300,000 joint replacement operations were performed on knee and hip joints in Germany despite the existing COVID-19 pandemic. An artificial joint, an endoprosthesis, is implanted to replace a diseased joint wholly or partially (Endoprothesenregister Deutschland, 2022). After successful treatment, follow-up rehabilitation (AHB) is usually carried out in an outpatient (the patient received the treatment but did not spend the night there) or inpatient rehabilitation clinic to restore health. The therapy concept includes functional, educational, psychotherapeutic, and psychosocial aspects. Depending on the funding agency and indication, there are different specifications for the content of the rehabilitation measure. With the rehabilitation therapy standards for the various indication groups, the German Pension Insurance has developed a treatment protocol based on scientific findings to improve the quality of care. In addition to exercise therapy and physiotherapeutic measures to improve joint mobility and function, as well as training of daily living (ADL training), relaxation methods and psychological interventions are also part of the therapy plan for knee and hip total endoprosthesis (TEP) care (Deutsche Rentenversicherung, 2020). Illness, pain, and rehabilitation are conceptualized as a complex interaction of social, biological, and psychological factors (Bhatia et al., 2020; Gatchel et al., 2007).
The relevance of the biopsychosocial model in orthopedic research has been shown in several studies: The diagnosis of depression, together with other factors, represents an increased risk of reoperation for total knee arthroplasty (Walter et al., 2021). Perceived pain in gonarthrotic patients is influenced by psychological and psychosocial factors (Eberly et al., 2018). In addition, despite extensive post-operative therapies, patients are not satisfied with the outcome in approximately 20% of cases (Gunaratne et al., 2017). Fear, pain, and long-term functional limitations can cause this dissatisfaction.
Regarding the mental state of the patients before the surgery, the results showed that the mental state before the operation already influences the pre-operative state of health of the affected joint and the general condition (Lavernia et al., 2015). At the same time, it plays a decisive role in the success and course after the intervention (Benditz et al., 2017; Khatib et al., 2015). Furthermore, in knee arthroplasty patients, higher pre-operative pain amplification is associated with increased post-operative pain. A correlation between poor pre-operative mental health and long-term lower post-operative functioning can be established (Vissers et al., 2012). Pre-operatively measured depression and anxiety in patients usually means an increased risk of complications after surgery, as well as lower functional improvements (La et al., 2020). A review of pre-operative psychological factors in knee TEP surgery written in 2016 showed that increased anxiety and pre-operative pain were the most significant factors indicating poorer outcomes in TEP surgery (Alattas et al., 2017). Kinesiophobia, an excessive irrational fear of movement and physical activity, is also a negative influencing factor (Filardo et al., 2017). Low levels of depression and high mental and physical health scores are associated with significant improvements in quality of life after surgery (Moghtadaei et al., 2020). A study published in 2020 identified a group wherein psychological markers predicted short- and long-term satisfaction after surgery (Xu et al., 2020). In addition, hospital stays lasted 1 day longer in dissatisfied patients than satisfied patients (Ali et al., 2017).
Apart from these results in inpatient, there are also long-term effects of pre-operative anxiety and depression. These include functional limitations and poorer quality of life even 1 year after knee TEP (Utrillas-Compaired et al., 2014), as well as higher dissatisfaction even months after surgery (Duivenvoorden et al., 2013). However, studies on psychological interventions in outpatient rehabilitation centers after orthopedic surgery are lacking. Nevertheless, they are essential because they investigate the relevance of psychological aspects of the healing process.
To achieve the long-term success of a joint operation, mindfulness training, which involves being aware of the present moment (Kabat-Zinn, 2013), could supplement previous therapy methods. Targeted mindfulness training is widely used in the form of standardized procedures such as Mindfulness-Based Stress Reduction (MBSR) and Mindfulness-Based Cognitive Therapy (MBCT), whose effectiveness has been confirmed by numerous studies and meta-analyses (Abbott et al., 2014; Fjorback et al., 2011; Grossman et al., 2004). These manuals are used in therapy for stress (Chang et al., 2004), anxiety (Grossman et al., 2014), depression (Strauss et al., 2014), and pain patients (Bakhshani et al., 2016). These psychological factors impact the long-term success of knee and hip surgery. Elevated anxiety levels represent an increased risk of dissatisfaction after surgery (Alattas et al., 2017); in turn, the lower the depression level and the better the mental constitution, the higher the improvement in quality of life (Moghtadaei et al., 2020). However, it remains unknown whether the proven effects of targeted mindfulness training could also occur specifically in orthopedic rehabilitation and thus improve the success of therapy after knee/hip joint replacement.
While the MBSR program, a standardized mindfulness intervention, may not be practical for everyday use in a rehabilitation clinic due to its high time and financial costs, the emergence of “self-help” methods has provided a more feasible alternative. One such method is bibliotherapy, a therapy presented as a book or workbook, which has shown effectiveness in treating various conditions. Notably, studies have found that “self-help” interventions can be as effective as “face-to-face” ones. This underscores the practicality and potential of bibliotherapy in a rehabilitation setting.
A viable solution could be bibliotherapy incorporating mindfulness elements, as demonstrated by Tavallaei et al. (2018). This uses a written-down version of the MBSR program, performed independently by the study participants. Included are various mindfulness elements, for example, mindful sitting, walking, and eating, as well as loving-kindness meditation (Tavallaei et al., 2018). The mode of action and concept of this mindfulness bibliotherapy would be a valuable practice for the rehabilitation of knee and hip surgery to ensure long-term patient satisfaction. In addition, implementing such a form of therapy into the existing daily therapy routine is relatively easy, as no additional therapist capacities are needed. For this purpose, the period of the intervention would have to be compressed to a duration of 3 to 4 weeks to establish compatibility with the duration of rehabilitation.
The study presented here aimed to investigate the effectiveness of a mindfulness bibliotherapy intervention in orthopedic rehabilitation after knee/hip joint replacement. With the help of mindfulness bibliotherapy adapted to the duration of rehabilitation, the therapy success of patients after knee/hip joint surgery should be improved regarding anxiety and depression, physical function, and the state of health, as well as motoric aspects. Those outcomes were chosen because they represent biological, physical, and social aspects investigated in the framework of the biopsychosocial model. The variety of measurements gives the possibility to obtain a more holistic view of the effectiveness of the intervention. The selection of tests used for this purpose was based on comparable studies (Alattas et al., 2017; Vissers et al., 2012; Xu et al., 2020). For the intervention, we used the workbook on MBCT (Teasdale et al., 2020) because MBCT was primarily established to reduce anxiety and depression. Similar to the study by Tavallaei et al. (2018), it includes mindfulness elements. In addition to the previously mentioned measures, dispositional mindfulness was assessed due to its inverse relationship with psychopathological symptoms such as depression (Tomlinson et al., 2018). Furthermore, the effect of a mindfulness intervention might depend on dispositional mindfulness: In a study with university students, the anxiety level decreased only in those individuals with a high level of dispositional mindfulness (Sousa et al., 2021).
The following hypotheses were formulated: Referring to the study by Tavallaei et al. (2018), we hypothesized that mindfulness bibliotherapy would positively influence the rehabilitation process in terms of joint mobility (measured with knee- and hip functionality scores), motor function (measured with the Timed “Up and Go”-Test), and quality of life (measured with the SF-36) (Hypothesis 1). According to the evidence on the effectiveness of mindfulness training in the treatment of anxiety (Grossman et al., 2014) and depression (Strauss et al., 2014), an improved emotional state (e.g., lower anxiety and depression, measured with the Hospital Anxiety and Depression Scale) was hypothesized after implementation of the intervention (Hypothesis 2). In addition, higher levels of mindfulness, as measured by the Five Facet Mindfulness Questionnaire (FFMQ; Baer et al., 2006), were expected to correlate with post-rehab health status (Hypothesis 3) positively. Exploratory regression analysis was conducted using the five different subscales of the FFMQ and two demographic variables (gender and age) (Hypothesis 4).
Method
Participants
During the recruitment period from mid-January to early April 2022, 93 patients from an outpatient rehabilitation center in Germany (ZAR Regensburg) were recruited for the study. Individuals undergoing rehabilitation for knee or hip TEP who met the following inclusion criteria were included: at least 18 years of age and sufficient reading and comprehension ability. All patients who met the inclusion criteria were automatically scheduled to receive information about the study on the first rehabilitation day and could decide whether to participate. All participants (M age = 63.34 years, SD = 10.49) volunteered to participate in the study and signed an informed consent form. The cause of rehabilitation was knee joint surgery in 46.20% of cases and hip joint surgery in 53.80%. Of the 43 patients with knee surgery, 53.50% were female and 46.50% male (M age = 64.30). 44.00% of the 50 hip surgery patients were female and 56.00% male (M age = 62.52).
For Hypotheses 1 and 2, the appropriate number of participants was calculated using G*power (Faul et al., 2007). A small to medium effect size has been chosen. With an effect size of f = 0.15, a power of 1 − β = 0.80, and an alpha standard probability of 0.05, a power analysis for the ANOVA of our main Hypotheses 1 and 2 with the within-subjects factor time of measurement (pre and post intervention) and one between-subjects factor group (control and intervention) factor resulted in a required sample size of n = 90. The sample sizes were calculated for two measurement points as it was preregistered. However, because we got the possibility to analyze the data at a follow-up measurement after 4 weeks, we conducted 3 (pre-, post, and follow-up) *2 (intervention, control group) analyses of variance for the variables except for the Timed “Up and Go”-Test (pre and post). For this, the required sample size was n = 74. For Hypothesis 3, two linear regressions with seven predictors (five FFMQ scales, sex, and age) and the criteria mental and physical health at post-test, a small to moderate effect size of f = 0.15, a power of 1 − β = 0.80, and an alpha standard probability of 0.05 resulted in a required sample size of n = 80.
Procedure
The intervention takes the form of mindfulness bibliotherapy. Bibliotherapy is a form of therapy intended to lead to recovery with the help of a reading. Based on the MBCT workbook by Teasdale et al. (2020), the workbook was compressed to 24 days and tailored to outpatient rehabilitation after knee and hip surgery. To meet the scientific standards of a mindfulness intervention, the created intervention was reviewed by both a practicing mindfulness teacher and an experienced mindfulness researcher and mindfulness mediation teacher. The book content can be obtained from the authors. Patients receive this “self-help” book on the first day of rehabilitation and work through it for 24 days; see supplementary material. The book contains both active exercises and written tasks. The active exercises include, for example, mindful breathing and walking, as well as a mindfulness eating exercise. The practical exercises are also reflected in writing.
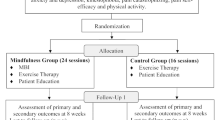
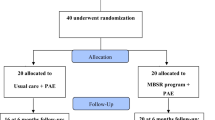
The study was a randomized controlled trial. Participants were randomly assigned to the intervention group (IG) or control group (CG). Patients in the mindfulness intervention received the baseline questionnaires and the mindfulness workbook during the informational interview. The questionnaires were completed and handed in on the same day. Intervention also began on the first day of rehabilitation and was carried out parallel to standard rehabilitation. In the case of assignment to the control group, only the questionnaires were handed out, and standard rehabilitation was carried out. In both cases, the Timed “Up and Go”-Test was performed during the first day of the rehabilitation. On the last day of rehabilitation, the patients received the questionnaires for the second measurement, completed on-site; the motor function test was also completed a second time. If study-related questions arose among the participants during or after the study period, personal contact with the study management was always possible. During the study, there was also the possibility of a follow-up measurement 4 weeks after rehabilitation, which deviates from the preregistration. The follow-up was carried out for the HADS, SF-36, FFMQ, and KOOS/HOOS.
Measures
The data collection of all parameters took place at the measurement points at the beginning of rehabilitation (T0) and the end of rehabilitation (T1). Five questionnaires and one practical test were used, presented in more detail below. A follow-up survey (T2) was conducted for the questionnaires. The follow-up measurement was not mentioned in the OSF pre-registration. During the study, however, the possibility for a follow-up measurement arose. This resulted in an unplanned follow-up measurement.
To collect demographic data, a self-constructed questionnaire was used to determine age, gender, and reason for rehabilitation (knee/hip TEP) as well as employment, physical activity, and level of knowledge about mindfulness and existing meditation practice.
Self-reported mindfulness was assessed using the German version of the Five Facet Mindfulness Questionnaire (FFMQ-D) (Michalak et al., 2016). Through 39 items, the five factors observing, describing, acting with attention, accepting without evaluation, and non-reactivity are measured. The items must be answered on a 5-point Likert scale ranging from rarely (1) to almost always (5) (Michalak et al., 2016). The internal consistency of the five scales and the total score in our study varied between 0.66 and 0.71 for Cronbach’s α and between 0.65 and 0.69 for McDonald’s ω.
The Timed “Up and Go”-Test is a performance test for measuring mobility. It measures the time in seconds from standing up from a sitting position, walking 3 m, turning around, walking back, and sitting down again without outside assistance (Podsiadlo & Richardson, 1991).
Anxiety and depression were assessed by the German version of the Hospital Anxiety and Depression Scale (HADS; Zigmond & Snaith, 1983; German version by Herrmann-Lingen et al., 2019). It is used for patients with physical complaints or diseases and comprises 14 items, which are divided into the subscale Anxiety (7 items) and Depression (7 items). The internal consistency of the two scales in our study varied between 0.83 and 0.87 for both Cronbach’s α and McDonald’s ω.
The SF-36 was used to assess health-related quality of life (Morfeld et al., 2011). The extended version used, with 36 items, assesses eight dimensions of subjective health. These include physical functioning, role functioning, and pain, as well as general health perception, vitality, social functioning, emotional role functioning, and psychological well-being. In the study, the acute version was used to determine the past week’s health status. The internal consistency of the subscales in our study varied between 0.73 and 0.78 for Cronbach’s α and between 0.81 and 0.83 for McDonald’s ω.
The Knee Injury and Osteoarthritis Outcome Score (KOOS) (Roos et al., 1998) or the Hip Disability and Osteoarthritis Outcome Score (HOOS) (Nilsdotter et al., 2003) was used to record the diagnosis-specific condition depending on the affected joint. With five subscales of Symptoms, Pain, Activities of daily living, Sports and Leisure, and Quality of life affected by the affected knee, the KOOS collects information through a total of 42 items with a 5-point Likert scale (KOOS, 2023). Analogous to the KOOS, the HOOS asks these questions about the affected hip joint.
Data Analyses
IBM SPSS 28 was used for data analyses. For descriptive analyses, demographic variables, such as age and gender distributions, will be reported. Furthermore, variables of interest for our present study, such as profession, physical activity, and knowledge of mindfulness, will be reported.
The effectiveness of the intervention was investigated with a repeated-measures ANOVA. The level of significance is set at 5%. The between-subject factor was group (IG, CG), and the within-subject factor time of measurement (pre, post, and follow-up intervention). The dependent variables were the following: mindfulness (FFMQ), anxiety and depression (HADS), the effect of osteoarthritis of the knee/hip joint on affected patients (KOOS, HOOS), motor function (Timed “Up and Go”-Test), and health status (SF-36).
To investigate the relationship between dispositional mindfulness at the pre-test and health (physical and mental) at the post-test, a regression analysis was conducted using the FFMQ scales and two demographic variables (sex and age).
Results
A total of 93 patients participated in the study, of which 48.40% were women, 51.60% were men, and 0% identified as non-binary or another gender. The mean age of the patients was 63.34 years (SD = 10.49); see Table 1 for relevant demographic variables. Five patients were excluded because they did not complete the follow-up measurement. Participants were free to participate in the follow-up survey and did not have to explain why they no longer wanted to participate.
The test for normal distribution (Kolmogorov–Smirnov) showed that the normal distribution was violated for anxiety, depression, and mindfulness in the pre-test but not for the measurement of the SF-36. In the post-test, normal distribution was violated for the mental health component of the quality-of-life test and depression and anxiety but not for the physical component of the SF-36 and mindfulness. Since simulation studies have shown that ANOVA with repeated-measures analyses is relatively robust against violations of the normal distribution assumption (Vasey & Thayer, 1987), we continue with the data. The original sample (n = 95) has been reduced because five patients did not complete the questionnaire at follow-up. Sphericity was given in the case of the Timed “Up and Go.” The following variables showed sphericity according to the Mauchly test for sphericity: SF-36 physical health (p = 0.946), HADS Anxiety (p = 0.367), FFMQ total (p = 0.070), FFMQ Describing (p = 0.101), FFMQ Attention (p = 0.092), FFMQ Accepting (p = 0.279), and Quality of Life associated with the affected joint (p = 0.187). In the remaining cases, the condition of sphericity was violated, so a Greenhouse–Geisser correction for degrees of freedom was applied. Results for the repeated-measures analyses of all variables are listed in Table 2.
The relevant results were two statistically significant interactions. The first interaction was between the factor time (pre-, post, and follow-up test) and group for the dependent variable HADS Anxiety F(2, 172) = 3.41, p = 0.035, ηp2 = 0.038. The second interaction was between the factor time (pre-test, post-test) and group for the dependent variable Timed “Up and Go”-Test F(1, 91) = 5.05, p = 0.027, ηp2 = 0.053. To determine the differences in more detail, Bonferroni-corrected t-tests were carried out. For the HADS, there was a significant difference for the intervention group between the pre- and post-test, t(44) = 3.53, p < 0.001, Cohen’s d = 2.53, and the pre-test and follow-up, t(42) = 3.98, p < 0.001, Cohen’s d = 2.45 but not between post-test and follow-up, p = 0.086. For the control group, there were no differences between the pre- and post-test and the post-test and the follow-up, both p > 0.06 (Fig. 1).
Regarding the Timed “Up and Go”-Test, both the intervention and control group improved significantly from pre- (IG: M = 17.58 s, SD = 6.39, CG: M = 21.45, SD = 7.43) to post-test (IG: M = 10.25 s, SD = 1.98, CG: M = 11.10, SD = 2.08). The improvement in the control group was higher than in the intervention group (d = 0.431).
Regression analysis for the dependent variables mental and physical health (SF-36) at the post-test was calculated with the predictors age, gender, and the five mindfulness subscales. The Durbin-Watson statistic had a value of 1.94 in the case of SF-36-PSK (Mental Health) and 1.80 in the case of SF-36-KSK (Physical Health), according to which there was no autocorrelation in the residuals. There was also a normal distribution of the residuals. The model has a medium goodness of fit for SF-36 PSK with an R2 = 0.17 (adjusted R2 = 0.10) and a low goodness of fit for SF-36 KSK with an R2 = 0.05 (adjusted R2 = − 0.03) (Cohen, 1988). The overall model including predictors of gender, age, and the five subscales of mindfulness was statistically significant in predicting the SF-36 mental health criterion, F(7, 85) = 2.52, p = 0.021 (Table 3). However, none of the investigated predictors significantly predicted the physical health criterion.
Discussion
The present study investigated the effect of mindfulness bibliotherapy on physical and psychological parameters after hip/knee TEP fitting in an outpatient rehabilitation setting. The basis for the hypotheses raised was the current state of research on the effectiveness of mindfulness interventions in different settings, specifically the use of bibliotherapy and the importance of mental health status in orthopedic rehabilitation. In the study, significant effects were measured for anxiety and motor skills. However, only the effect on anxiety was interpretable. In addition, a correlation between self-reported mindfulness, age, gender, and mental health status at the end of rehabilitation was identified.
Mindfulness has been successfully used in treating anxiety (Grossman et al., 2014) and depression (Strauss et al., 2014), but targeted mindfulness training has also been shown to bring about success in the treatment of chronic pain (Bakhshani et al., 2016). Furthermore, it has been shown that mindfulness-based interventions are feasible for use in surgical patient populations (Hymowitz et al., 2022). Thus, mindfulness as a therapeutic approach appears to be a good complement to the relaxation methods used so far, such as autogenic training and progressive muscle relaxation, as well as the complementary movement therapy measures such as Qi Gong, Tai Chi, and yoga (Deutsche Rentenversicherung, 2020). The integration of relaxation methods (Lin, 2012) and the mentioned exercise therapies into the rehabilitation therapy standards show the importance of psychological factors for successful rehabilitation, which is confirmed by numerous studies, for example, on the influence of anxiety and depression on the therapy outcome in orthopedic diseases (Ali et al., 2017).
The present study provides evidence that mindfulness bibliotherapy in outpatient orthopedic rehabilitation as an additional therapy offer is easy to implement from an organizational and economic point of view and can be a good support for the users. Significant effects of the intervention could be demonstrated for anxiety (HADS Anxiety), indicating that the intervention has a positive effect, at least on the psychological factor of anxiety. This is partly in line with the study of Ali et al. (2017). For all other measured variables, no advantage could be shown for the mindfulness bibliotherapy group.
There is an accumulation of evidence supporting the hypothesis that a higher level of mindfulness measured by the FFMQ at the beginning of rehabilitation correlates positively with the state of mental health after rehabilitation. This aligns with a study by university students showing that trait mindfulness is related to psychological aspects after a short mindfulness intervention (Sousa et al., 2021). However, no single predictor was significant, and the explained variance was relatively small. One reason for this might be that the patients included in this study have little mindfulness experience.
Limitations and Future Research
The effect of mindfulness on various parameters and in therapeutic application has been proven by many studies, as was made clear in the introduction. Nevertheless, the established hypotheses could not be completely confirmed. This may be due to some limitations of the present study.
This includes first the chosen intervention. Although bibliotherapy has the advantage of a resource-saving and easy-to-organize implementation in the regular rehabilitation routine, the participants’ actual implementation and engagement intensity could not be objectively tracked. However, the actual effects of the intervention can only be achieved if it is also sufficiently used. An alternative could be a digital form (app-based), which could be used, for example, to reproduce the frequency of the call, duration of the processing, etc., and thus make precise statements about the use. Due to the selected target group and the associated expected higher age, an analog intervention was deliberately preferred to the digital variant to achieve a higher acceptance of the intervention. The expectations of the sample are reflected in the actual sample, which had an average age of 63.34 years, of which over 50% of the participants were already retired at the start of rehab. For future interventions, however, the use of a digital alternative could make sense since, on the one hand, the proportion of surgical interventions on knee and hip joints in the younger age groups is increasing significantly (Rupp et al., 2020), and on the other hand, the coming potential patients are already increasingly using mobile end devices. Even before the COVID-19 pandemic, the number of users over 65 increased significantly from 2009 (37.80%) to 2019 (74.20%) (Seifert, 2022). Nevertheless, the extent to which mindfulness fits with mobile end devices and other technical presentations should be considered. Many mindfulness apps offer a cheaper alternative to mindfulness courses. The effectiveness of some mindfulness apps has already been proven by scientific studies (Gál et al., 2021). However, incoming push messages or calls on the smartphone can disrupt learning, making it more difficult. In addition, bibliotherapy may not be sufficient for people who have had no previous contact with the topic of mindfulness (84%). After all, this is a complex concept that requires much practice. Even in guided mindfulness therapies, implementation in daily life often fails once the therapist is no longer present (Derra & Schilling, 2017).
In addition to the intervention, the selected setting might be a limiting factor. Due to the outpatient rehabilitation measure, both groups (IG and CG) may be influenced by several factors that were not recorded during the data collection. In outpatient orthopedic rehabilitation, the patients are picked up by the patient transport in the morning and are driven home again at the end of the rehabilitation day around 3:00 p.m. In exceptional cases, the transport is taken over by relatives. The fact that the assessment of therapy outcomes occurred close to the patients’ homes has numerous advantages, such as the assessment in a familiar environment and the availability of support by relatives. Nevertheless, the influences of the social environment, the different living situations, the distance, and the associated daily travel time cannot be excluded in outpatient rehabilitation. For this reason, the form of rehabilitation must be chosen according to the needs of the rehabilitant (Spies et al., 2020).
Limitations such as a very small or selective sample, which most studies on mindfulness interventions in physical rehabilitation have (Hardison & Roll, 2016), do not apply in the present study at first glance. However, the statistical power could have been influenced by the low reliability of the mindfulness measurement (but see Zimmerman & Zumbo, 2015).
Finally, if we consider the current state of research on the application and effect of mindfulness and the importance of psychological health in orthopedic diseases, mindfulness training presents itself as a helpful therapeutic approach. The conducted study also showed that mindfulness bibliotherapy has positive effects on psychological and physiological parameters. Furthermore, the level of mindfulness at the beginning of rehabilitation is related to psychological health status after rehabilitation. Due to the importance of psychological health for long-term success after TEP surgery in conjunction with the identified correlation, one’s mindfulness before surgery may also predict long-term success after surgery. To investigate this assumption and, thus, the more precise meaning of mindfulness in orthopedics, further hypothesis-guided research is needed. The limitations of the present study provide hints for the planning and implementation of further scientific investigations based on this hypothesis.
Data Availability
Data can be obtained at OSF, https://osf.io/4tmwq/.
References
Abbott, R. A., Whear, R., Rodgers, L. R., Bethel, A., Coon, J. T., Kuyken, W., Stein, K., & Dickens, C. (2014). Effectiveness of mindfulness-based stress reduction and mindfulness based cognitive therapy in vascular disease: A systematic review and metaanalysis of randomised controlled trials. Journal of Psychosomatic Research, 76, 341–351. https://doi.org/10.1016/j.jpsychores.2014.02.012
Alattas, S. A., Smith, T., Bhatti, M., Wilson-Nunn, D., & Donell, S. (2017). Greater pre-operative anxiety, pain and poorer function predict a worse outcome of a total knee arthroplasty. Knee Surgery, Sports Traumatology, Arthroscopy, 25(11), 3403–3410. https://doi.org/10.1007/s00167-016-4314-8
Ali, A., Lindstrand, A., Sundberg, M., & Flivik, G. (2017). Preoperative anxiety and depression correlate with dissatisfaction after total knee arthroplasty: A prospective longitudinal cohort study of 186 patients, with 4-year follow-up. The Journal of Arthroplasty, 32(3), 767–770. https://doi.org/10.1016/j.arth.2016.08.033
Bakhshani, N. M., Amirani, A., Amirifard, H. & Shahrakipoor, M. (2016). The effectiveness of mindfulness-based stress reduction on perceived pain intensity and quality of life in patients with chronic headache. Global Journal of Health Science, 8, 142. https://doi.org/10.5539/gjhs.v8n4p142
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13(1), 27–45. https://doi.org/10.1177/1073191105283504
Benditz, A., Jansen, P., Schaible, J., Roll, C., Grifka, J., & Götz, J. (2017). Psychological factors as risk factors for poor hip function after total hip arthroplasty. Therapeutics and Clinical Risk Management, 13, 237–244. https://doi.org/10.2147/TCRM.S127868
Bhatia, S., Karvannan, H., & Prem, V. (2020). The effect of bio psychosocial model of rehabilitation on pain and quality of life after total knee replacement: A randomized controlled trial. Journal of Arthroscopy and Joint Surgery, 7(4), 177–188. https://doi.org/10.1016/j.jajs.2020.09.005
Chang, V. Y., Palesh, O., Caldwell, R., Glasgow, N., Abramson, M., Luskin, F., Gill, M., Burke, A. & Koopman, C. (2004). The effects of a mindfulness‐based stress reduction program on stress, mindfulness self‐efficacy, and positive states of mind. Stress and Health, 20, 141–147. https://psycnet.apa.org/doi/10.1002/smi.1011
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). L. Erlbaum Associates.
Cuijpers, P., Donker, T., Johansson, R., Mohr, D. C., van Straten, A. & Andersson, G. (2011). Selfguided psychological treatment for depressive symptoms: A meta-analysis. PLoS ONE, 6(6), e21274. https://doi.org/10.1371/journal.pone.0021274
Derra, C. & Schilling, C. (2017). Achtsamkeit und Schmerz. Stress, Schlafstörungen, Stimmungsschwankungen und Schmerz wirksam lindern. Klett-Cotta.
Deutsche Rentenversicherung (2020). Reha-Therapiestandards Hüft- und Knie-TEP. Für die medizinische Rehabilitation der Rentenversicherung. Available online: https://www.deutsche-rentenversicherung.de/DRV/DE/Experten/Infos-fuer-Reha-Einrichtungen/Grundlagen-und-Anforderungen/Reha-Qualitaetssicherung/rts.html (Accessed on 09 February 2021).
Duivenvoorden, T., Vissers, M. M., Verhaar, J. A. N., Busschbach, J. J. V., Gosens, T., Bloem, R. M., Bierma-Zeinstra, S. M. A., & Reijman, M. (2013). Anxiety and depressive symptoms before and after total hip and knee arthroplasty: A prospective multicentre study. Ostheoarthritis and Cartilage, 21(12), 1834–1840. https://doi.org/10.1016/j.joca.2013.08.022
Endoprothesenregister Deutschland (2022). Jahresbericht 2022. Mit Sicherheit mehr Qualität. EPRD Deutsche Endoprothesenregister GmbH.
Eberly, L., Richter, D., Comerci, G., Ocksrider, J., Mercer, D., Mlady, G., Wascher, D. & Schenck, R. (2018). Psychosocial and demographic factors influencing pain scores of patients with knee osteoarthritis. PLoS ONE, 13(4), e0195075. https://doi.org/10.1371/journal.pone.0195075
Fanner, D., & Urquhart, C. (2008). Bibliotherapy for mental health service users part 1: A systematic review. Health Information and Libraries Journal, 25, 237–252. https://doi.org/10.1111/j.1471-1842.2008.00821.x
Faul, F., Erdfelder, E., Lang, A.-G., & Buchner, A. (2007). G*power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods, 39(2), 175–191. https://doi.org/10.3758/BF03193146
Filardo, G., Merli, G., Roffi, A., Marcacci, T., Berti Ceroni, F., Raboni, D., Bortolotti, B., Kon, E., & Marcacci, M. (2017). Kinesiophobia and depression affect total knee arthroplasty outcome in a multivariate analysis of psychological and physical factors on 200 patients. Knee Surgery, Sports Traumatology, Arthroscopy, 25(11), 3417–3423. https://doi.org/10.1007/s00167-016-4201-3
Fjorback, L., Arendt, M., Ørnbøl, E., Fink, P., & Walach, H. (2011). Mindfulness-based stress reduction and mindfulness-based cognitive therapy: A systematic review of randomized controlled trials. Acta Psychiatrica Scandinavica, 124, 102–119. https://doi.org/10.1111/j.1600-0447.2011.01704.x
Gál, E., Ștefan, S., & Cristea, I. A. (2021). The efficacy of mindfulness meditation apps in enhancing users’ well-being and mental health related outcomes: A meta-analysis of randomized controlled trials. Journal of Affective Disorders, 279, 131–142. https://doi.org/10.1016/j.jad.2020.09.134
Gatchel, R. J., Peng, Y. B., Peters, M. L., Fuchs, P. N., & Turk, D. C. (2007). The biopsychosocial approach to chronic pain: Scientific advances and future directions. Psychological Bulletin, 133(4), 581–624. https://doi.org/10.1037/0033-2909.133.4.581
Grossman, P., Niemann, L., Schmidt, S., & Walach, H. (2004). Mindfulness-based stress reduction and health benefits: A meta-analysis. Journal of Psychosomatic Research, 57, 35–43. https://doi.org/10.1016/s0022-3999(03)00573-7
Grossman, P., Zwahlen, D., Halter, J. P., Passweg, J. R., Steiner, C., & Kiss, A. (2014). A mindfulness-based program for improving quality of life among hematopoietic stem cell transplantation survivors: Feasibility and preliminary findings. Supportive Care Cancer, 23(4), 1105–1112. https://doi.org/10.1007/s00520-014-2452-4
Gunaratne, R., Pratt, D. N., Banda, J., Fick, D. P., Khan, R. J. K., & Robertson, B. W. (2017). Patient dissatisfaction following total knee arthroplasty: A systematic review of the literature. The Journal of Arthroplasty, 32(12), 3854–3860. https://doi.org/10.1016/j.arth.2017.07.021
Hardison, M. E. & Roll, S. C. (2016). Mindfulness interventions in physical rehabilitation; A scoping review. The American Journal of Occupational Therapy, 70(3), 1–9. https://doi.org/10.5014/ajot.2016.018069
Herrmann-Lingen, C., Buss, U., & Snaith, R. P. (2019). Hospital Anxiety and Depression Scale - Deutsche version. Hogrefe.
Hirschmann, M. T., Testa, E., Amsler, F., & Friederich, N. F. (2013). The unhappy total knee arthroplasty (TKA) patient: Higher WOMAC and lower KSS in depressed patients prior and after TKA. Knee Surgery, Sports Traumatolology, Arthroscopy, 21(10), 2405–2411. https://doi.org/10.1007/s00167-013-2409-z
Hymowitz, G., Hasan, F., Yerramalli, G., & Cervoni, C. (2022). Mindfulness-based interventions for surgical patients and impact on postoperative outcomes, patient wellbeing, and satisfaction. The American Surgeon, 90(5), 947–953. https://doi.org/10.1177/00031348221117025
Kabat-Zinn, J. (2013). Full catastrophe living: Using the wisdom of your body and mind to face 497 stress, pain, and illness (revised and updated edition). Bantam Books.
Khatib, Y., Madan, A., Naylor, J. M., & Harris, I. A. (2015). Do psychological factors predict poor outcome in patients undergoing TKA? A systematic review. Clinical Orthopaedics and Related Research, 473(8), 2630–2638. https://doi.org/10.1007/s11999-015-4234-9
KOOS (2023). KOOS. Available online: http://www.koos.nu/. Accessed 27 Feb 2023.
Kramer, K. (2009). Using self-help bibliotherapy in counselling. University of Lethbridge.
La, A., Nadarajah, V., Jauregui, J. J., Shield, W. P., 3rd., Medina, S. H., Dubina, A. G., Meredith, S. J., Packer, J. D., & Henn, F., 3rd. (2020). Clinical characteristics associated with depression or anxiety among patients presenting for knee surgery. Journal of Clinical Orthopaedics and Trauma, 11(1), 164–170. https://doi.org/10.1016/j.jcot.2019.08.009
Lavernia, C. J., Villa, J. M., & Iacobelli, D. A. (2015). What is the role of mental health in primary total knee arthroplasty? Clinical Orthopaedics and Related Research, 473(1), 159–163. https://doi.org/10.1007/s11999-014-3769-5
Lin, P.- C. (2012). An evaluation of the effectiveness of relaxation therapy for patients receiving joint replacement surgery. Journal of Clinical Nursing, 21, 601–608.https://doi.org/10.1111/j.1365-2702.2010.03406.x.
Marrs, R. W. (1995). A meta-analysis of bibliotherapy studies. American Journal of Community Psychology, 23, 843–870. https://doi.org/10.1007/bf02507018
Michalak, J., Zarbock, G., Drews, M., Otto, D., Mertens, D., Ströhle, G., Schwinger, M., Dahme, B. & Heidenreich, T. (2016). Erfassung von Achtsamkeit mit der deutschen Version des Five Facet Mindfulness Questionnaires (FFMQ-D). Zeitschrift für Gesundheitspsychologie, 24 (1), 1–12. https://econtent.hogrefe.com/doi/pdf/10.1026/0943-8149/a000149
Moghtadaei, M., Yeganeh, A., Hosseinzadeh, N., Khazanchin, A., Moaiedfar, M., Jolfaei, A. G., & Nasiri, S. (2020). The impact of depression, personality, and mental health on outcomes of total knee arthroplasty. Clinics Orthopedic Surgery, 12(4), 456–463. https://doi.org/10.4055/cios19148
Morfeld, M., Kirchberger, I., & Bullinger, M. (2011). SF-36. Hogrefe.
Nilsdotter, A. K., Lohmander, L. S., Klässbo, M., & Roos, E. M. (2003). Hip Disability and Osteoarthritis Outcome Score (HOOS)–Validity and responsiveness in total hip replacement. BMC Musculoskeletal Disorders, 4, 10. https://doi.org/10.1186/1471-2474-4-10
Podsiadlo, D., & Richardson, S. (1991). The timed “up and go”: A test of basic functional mobility for frail elderly persons. Journal of the American Geriatrics Society, 39(2), 142–148. https://doi.org/10.1111/j.1532-5415.1991.tb01616.x
Roos, E. M., Roos, H. P., Lohmander, L. S., Ekdahl, C., & Beynnon, B. D. (1998). Knee injury and osteoarthritis outcome score (KOOS)–Development of a self-administered outcome measure. The Journal of Orthopaedic and Sports Physical Therapy, 28(2), 88–96. https://doi.org/10.2519/jospt.1998.28.2.88
Rupp, M., Lau, E., Kurtz, S. M., & Alt, V. (2020). Projections of primary TKA and THA in Germany from 2016 through 2040. Clinical Orthopaedics and Related Research, 478(7), 1622–1633. https://doi.org/10.1097/CORR.0000000000001214
Seifert, A. (2022). Digitale Transformation in den Haushalten älterer Menschen. Zeitschrift für Gerontologie und Geriatrie, 55, 305–311. https://doi.org/10.1007/s00391-021-01897-5
Sharma, V., Sood, A., Prasad, K., Loehrer, L., Schroeder, D., & Brent, B. (2014). Bibliotherapy to decrease stress and anxiety and increase resilience and mindfulness: A pilot trial. Explore, 10, 248–252. https://doi.org/10.1016/j.explore.2014.04.002
Sousa, G. M., Lima-Araújo, G. L., Araújo, D. B., & Sousa, M. B. C. (2021). Brief mindfulness-based training and mindfulness trait attenuate psychological stress in university students: A randomized controlled trial. BMC Psychology, 9(1), 21. https://doi.org/10.1186/s40359-021-00520-x
Spies, M., Kulisch, K., Streibelt, M., Pohl, A., Schulz, H., & Brütt, A. L. (2020). Wie bewerten Versicherte unterschiedliche Ausgestaltungen der medizinischen Rehabilitation? Rehabilitation, 59(5), 282–290. https://doi.org/10.1055/a-1148-5051
Strauss, C., Chavanagh, K., Oliver, A. & Pettman, D. (2014). Mindfulness-based interventions for people diagnosed with a current episode of an anxiety or depressive disorder: A meta-analysis of randomised controlled trials. PLoS ONE, 9(4), e96110. https://doi.org/10.1371/journal.pone.0096110
Tavallaei, V., Rezapour, Y., Rezaiemaram, P., & Saadat, S. H. (2018). Mindfulness for female outpatients with chronic primary headaches: An internet-based bibliotherapy. European Journal of Translational Myology, 28(2), 175–184. https://doi.org/10.4081/ejtm.2018/7380
Teasdale, J., Williams, M. & Segal, Z. (2020). Das MBCT-Arbeitsbuch. Ein 8-Wochen-Programm zur Selbstbefreiung von Depressionen und emotionalem Stress. Arbor Verlag GmbH.
Tomlinson, E. R., Yousaf, O., Vittersø, A. D., & Jones, L. (2018). Dispositional mindfulness and psychological health: A systematic review. Mindfulness, 9(1), 23–43. https://doi.org/10.1007/s12671-017-0762-6
Utrillas-Compaired, A., De la Torre-Escuredo, B. J., Tebar-Martínez, A. J., & Asúnsolo-Del Barco, Á. (2014). Does preoperative psychologic distress influence pain, function, and quality of life after TKA? Clinical Orthopaedics and Related Research, 472(8), 2457–2465. https://doi.org/10.1007/s11999-014-3570-5
Vasey, M. W., & Thayer, J. F. (1987). The continuing problem of false positives in repeated measures ANOVA in psychophysiology: A multivariate solution. Psychophysiology, 24(4), 479–486. https://doi.org/10.1111/j.1469-8986.1987.tb00324.x
Vissers, M. M., Bussmann, J. B., Verhaar, J. A., Busschbach, J. J., Bierma-Zeinstra, S. M., & Reijman, M. (2012). Psychological factors affecting the outcome of total hip and knee arthroplasty: A systematic review. Seminars in Arthritis and Rheumatism, 41(4), 576–588. https://doi.org/10.1016/j.semarthrit.2011.07.003
Walter, N., Rupp, M., Hinterberger, T., & Alt, V. (2021). Prosthetic infections and the increasing importance of psychological comorbidities: An epidemiological analysis for Germany from 2009 through 2019. Der Orthopäde, 50(10), 859–865. https://doi.org/10.1007/s00132-021-04088-7
Xu, J., Twiggs, J., Parker, D., & Negus, J. (2020). The association between anxiety, depression, and locus of control with patient outcomes following total knee arthroplasty. The Journal of Arthroplasty, 35(3), 720–724. https://doi.org/10.1016/j.arth.2019.10.022
Zigmond, A. S., & Snaith, R. P. (1983). The Hospital Anxiety and Depression Scale. Acta Psychiatrica Scandinavica, 67, 361–370. https://doi.org/10.1111/j.1600-0447.1983.tb09716.x
Zimmerman, D. W. & Zumbo, B. D. (2015). Resolving the issue of how reliability is related to statistical power: Adhering to mathematical definitions. Journal of Modern Applied Statistical Methods, 14(2), 9–26. https://doi.org/10.22237/jmasm/1446350640
Acknowledgements
We are grateful for all the patients taking part in this project and for the rehabilitation clinic that allowed us to carry out the study.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Franziska Schäffer: conceptualization, implementation, analyzing, writing, editing. Petra Jansen: conceptualization, supervision, analyzing, writing, editing.
Corresponding author
Ethics declarations
Ethics Approval
The responsible ethics committee of the University of Regensburg approved the study (21–2539-101). The experiment was conducted according to the guidelines set forth by the Declaration of Helsinki.
Informed Consent
The rehabilitation clinic was informed about the project. After providing the patients with an information sheet and a consent form, they gave their written informed consent, and data were processed anonymously.
Conflict of Interest
The authors declare no competing interests.
Use of Artificial Intelligence
AI was not used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schäffer, F., Jansen, P. Mindfulness in Orthopedic Rehabilitation: Can the Use of a Mindfulness Diary Positively Influence the Therapeutic Outcome of Orthopedic Rehabilitation?. Mindfulness (2024). https://doi.org/10.1007/s12671-024-02396-5
Accepted:
Published:
DOI: https://doi.org/10.1007/s12671-024-02396-5