Abstract
Background
Primary vesicoureteral reflux (VUR) is a common congenital anomaly of the kidney and urinary tract (CAKUT) in childhood. The present study identified the possible genetic contributions to primary VUR in children.
Methods
Patients with primary VUR were enrolled and analysed based on a national multi-center registration network (Chinese Children Genetic Kidney Disease Database, CCGKDD) that covered 23 different provinces/regions in China from 2014 to 2019. Genetic causes were sought using whole-exome sequencing (WES) or targeted-exome sequencing.
Results
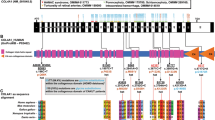
A total of 379 unrelated patients (male: female 219:160) with primary VUR were recruited. Sixty-four (16.9%) children had extrarenal manifestations, and 165 (43.5%) patients showed the coexistence of other CAKUT phenotypes. Eighty-eight patient (23.2%) exhibited impaired renal function at their last visit, and 18 of them (20.5%) developed ESRD at the median age of 7.0 (IQR 0.9–11.4) years. A monogenic cause was identified in 28 patients (7.39%). These genes included PAX2 (n = 4), TNXB (n = 3), GATA3 (n = 3), SLIT2 (n = 3), ROBO2 (n = 2), TBX18 (n = 2), and the other 11 genes (one gene for each patient). There was a significant difference in the rate of gene mutations between patients with or without extrarenal complications (14.1% vs. 6%, P = 0.035). The frequency of genetic abnormality was not statistically significant based on the coexistence of another CAKUT (9.6% vs. 5.6%, P = 0.139, Chi-square test) and the grade of reflux (9.4% vs. 6.7%, P = 0.429). Kaplan–Meier survival curve showed that the presence of genetic mutations did affect renal survival (Log-rank test, P = 0.01). PAX2 mutation carriers (HR 5.1, 95% CI 1.3–20.0; P = 0.02) and TNXB mutation carriers (HR 20.3, 95% CI 2.4–168.7; P = 0.01) were associated with increased risk of progression to ESRD.
Conclusions
PAX2, TNXB, GATA3 and SLIT2 were the main underlying monogenic causes and accounted for up to 46.4% of monogenic VUR. Extrarenal complications and renal function were significantly related to the findings of genetic factors in children with primary VUR. Like other types of CAKUT, several genes may be responsible for isolated VUR.


Similar content being viewed by others
References
Baracco R, Mattoo TK. Diagnosis and management of urinary tract infection and vesicoureteral reflux in the neonate. Clin Perinatol. 2014;41:633–42.
Van der Ven AT, Vivante A, Hildebrandt F. Novel insights into the pathogenesis of monogenic congenital anomalies of the kidney and urinary tract. J AM Soc Nephrol. 2018;29:36–50.
Nicolaou N, Renkema KY, Bongers EM, Giles RH, Knoers NV. Genetic, environmental, and epigenetic factors involved in CAKUT. Nat Rev Nephrol. 2015;11:720–31.
Puri P, Gosemann JH, Darlow J, Barton DE. Genetics of vesicoureteral reflux. Nat Rev Urol. 2011;8:539–52.
Song R, Yosypiv IV. Genetics of congenital anomalies of the kidney and urinary tract. Pediatr Nephrol. 2011;26:353–64.
Adamiok-Ostrowska A, Piekiełko-Witkowska A. Ciliary genes in renal cystic diseases. Cells. 2020;9:907.
Connaughton DM, Kennedy C, Shril S, Mann N, Murray SL, Williams PA, et al. Monogenic causes of chronic kidney disease in adults. Kidney Int. 2019;95:914–28.
Van der Ven AT, Connaughton DM, Ityel H, Mann N, Nakayama M, Chen J, et al. Whole-exome sequencing identifies causative mutations in families with congenital anomalies of the kidney and urinary tract. J AM Soc Nephrol. 2018;29:2348–61.
Bekheirnia MR, Bekheirnia N, Bainbridge MN, Gu S, Coban AZ, Gambin T, et al. Whole-exome sequencing in the molecular diagnosis of individuals with congenital anomalies of the kidney and urinary tract and identification of a new causative gene. Genet Med. 2017;19:412–20.
Heidet L, Morinière V, Henry C, De Tomasi L, Reilly ML, Humbert C, et al. Targeted exome sequencing identifies PBX1 as involved in monogenic congenital anomalies of the kidney and urinary tract. J AM Soc Nephrol. 2017;28:2901–14.
Vivante A, Hwang DY, Kohl S, Chen J, Shril S, Schulz J, et al. Exome sequencing discerns syndromes in patients from consanguineous families with congenital anomalies of the kidneys and urinary tract. J AM Soc Nephrol. 2017;28:69–75.
Lei TY, Fu F, Li R, Wang D, Wang RY, Jing XY, et al. Whole-exome sequencing for prenatal diagnosis of fetuses with congenital anomalies of the kidney and urinary tract. Nephrol Dial Transpl. 2017;32:1665–75.
Nicolaou N, Pulit SL, Nijman IJ, Monroe GR, Feitz WF, Schreuder MF, et al. Prioritization and burden analysis of rare variants in 208 candidate genes suggest they do not play a major role in CAKUT. Kidney Int. 2016;89:476–86.
Hwang DY, Dworschak GC, Kohl S, Saisawat P, Vivante A, Hilger AC, et al. Mutations in 12 known dominant disease-causing genes clarify many congenital anomalies of the kidney and urinary tract. Kidney Int. 2014;85:1429–33.
Saisawat P, Kohl S, Hilger AC, Hwang DY, Yung GH, Dworschak GC, et al. Whole-exome resequencing reveals recessive mutations in TRAP1 in individuals with CAKUT and VACTERL association. Kidney Int. 2014;85:1310–7.
Weber S, Moriniere V, Knüppel T, Charbit M, Dusek J, Ghiggeri GM, et al. Prevalence of mutations in renal developmental genes in children with renal hypodysplasia: results of the ESCAPE study. J AM Soc Nephrol. 2006;17:2864–70.
Nino F, Ilari M, Noviello C, Santoro L, Rätsch IM, Martino A, et al. Genetics of vesicoureteral reflux. Curr Genom. 2016;17:70–9.
Lebowitz RL, Olbing H, Parkkulainen KV, Smellie JM, Tamminen-Möbius TE. International system of radiographic grading of vesicoureteric reflux. International Reflux Study in Children. Pediatr Radiol. 1985;15:105–9.
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405–24.
Ahn YH, Lee C, Kim N, Park E, Kang HG, Ha IS, et al. Targeted exome sequencing provided comprehensive genetic diagnosis of congenital anomalies of the kidney and urinary tract. J Clin Med. 2020;9:751.
Ishiwa S, Sato M, Morisada N, Nishi K, Kanamori T, Okutsu M, et al. Association between the clinical presentation of congenital anomalies of the kidney and urinary tract (CAKUT) and gene mutations: an analysis of 66 patients at a single institution. Pediatr Nephrol. 2019;34:1457–64.
Siomou E, Mitsioni AG, Giapros V, Bouba I, Noutsopoulos D, Georgiou I. Copy-number variation analysis in familial nonsyndromic congenital anomalies of the kidney and urinary tract: Evidence for the causative role of a transposable element-associated genomic rearrangement. Mol Med Rep. 2017;15:3631–6.
Sanna-Cherchi S, Kiryluk K, Burgess KE, Bodria M, Sampson MG, Hadley D, et al. Copy-number disorders are a common cause of congenital kidney malformations. AM J Hum Genet. 2012;91:987–97.
Murugapoopathy V, Gupta IR. A primer on congenital anomalies of the kidneys and urinary tracts (CAKUT). Clin J Am Soc Nephrol. 2020;15:723–31.
Acknowledgements
We thank all participating patients and their families. Also, we thank our coordinators from Chigene (Beijing), Translational Medical Research Center Co. Ltd., WuXi NextCODE's Shanghai, Beijing MyGenostics Co. Ltd., for sequencing technology support.
Funding
This work was supported by the Grant NSFC-81800602 from National Natural Science Foundation of China (Dr. Jia-Lu Liu); the Grant 20184Y0176 from Shanghai Municipal Commission of Health and Family Planning Youth Research Program (Dr. Jia-Lu Liu); the Grant SHDC12016107 from Shanghai Shenkang Hospital Developmental Center (Dr. Hong Xu); the Grant NSFC-81670609 from National Natural Science Foundation of China (Dr. Hong Xu); the Grant 2018YFA0801102 from National Key Research and Development Project (Dr. Hong Xu).
Author information
Authors and Affiliations
Consortia
Contributions
JLL, QS, MYW, GHZ, YFL are joint first authors. The roles of JLL, QS, MYW, GHZ and YFL are data curation, formal analysis, investigation, methodology, validation, visualization, writing—original draft, writing—review and editing. The roles of XWW, XST, YLB, YNG, JC, XYF, YHZ, GML, YBS, XJG, CHL, XYJ, SH, YLK, YLG, LPR, DL and SW are investigation and data curation. The role of BBW, DM, JR, QS and HX are writing—review and editing. The role of JLL and HX is funding acquisition. The roles of QS and HX are conceptualization, resources, supervision and project administration. All authors have seen and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the Children’s Hospital of Fudan University’ Ethical Committee (no. 2017-56), and informed consent was obtained for all research individuals.
Conflict of interest
Author Hong Xu is a member of the Editorial Board for World Journal of Pediatrics. The paper was handled by the other Editor and has undergone rigorous peer review process. Author Hong Xu was not involved in the journal's review of, or decisions related to, this manuscript. All the other authors have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, JL., Shen, Q., Wu, MY. et al. Responsible genes in children with primary vesicoureteral reflux: findings from the Chinese Children Genetic Kidney Disease Database. World J Pediatr 17, 409–418 (2021). https://doi.org/10.1007/s12519-021-00428-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-021-00428-x