Abstract
Background
The association between maternal and cord blood zinc level and pregnancy outcomes remains uncertain. The present study aims to assess whether maternal blood zinc level represents cord blood zinc level correctly.
Methods
In this meta-analysis, systematic search was performed in PubMed, Web of Science, and Scopus databases for relevant available English articles which included mean and standard deviation values of cord blood zinc level up to April 2019. For the assessment of the relation between cord blood zinc level and pregnancy outcomes, the pooled standard mean difference with 95% confidence interval (CI) was used and 23 studies were analyzed.
Results
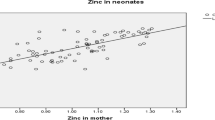
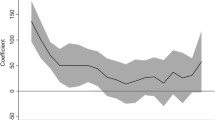
Cumulative analysis showed that cord blood zinc level was found significantly decreased in pregnancies with complications compared with healthy pregnancy controls [REM: P = 0.0007, mean difference − 7.9 (− 12.48, − 3.31)]. For further analysis, maternal serum zinc level status was determined from same studies to compare with cord blood levels and subgroups were detected as “Preterm”, “Preeclampsia”, “Small for gestational age/Intrauterine growth restriction and Low birth weight”. It was observed that cord blood zinc levels in subgroup analysis were also decreased and/or tend to be decreased compared to healthy pregnancies, except for preeclampsia subgroup. Also, a correlation was seen between cord blood and maternal blood zinc level status (R = 0.4365, 95% CI − 0.530, 0.756; P = 0.0351).
Conclusion
It was thought that cord blood zinc level might tend to decrease more than maternal serum zinc level in the pathological conditions during pregnancies.









Similar content being viewed by others
References
Terrin G, Berni Canani R, Di Chiara M, Pietravalle A, Aleandri V, Conte F, et al. Zinc in early life: a key element in the fetus and preterm neonate. Nutrients. 2015;7:10427–46.
Gibson RS. The role of diet-and host-related factors in nutrient bioavailability and thus in nutrient-based dietary requirement estimates. Food Nutr Bull. 2007;28(1 Suppl International):S77–100.
Donangelo CM, King JC. Maternal zinc intakes and homeostatic adjustments during pregnancy and lactation. Nutrients. 2012;4:782–98.
Keshavarz P, Nobakht MGHBF, Mirhafez SR, Nematy M, Azimi-Nezhad M, Afin SA, et al. Alterations in lipid profile, zinc and copper levels and superoxide dismutase activities in normal pregnancy and preeclampsia. Am J Med Sci. 2007;353:552–8.
Acikgoz S, Harma M, Harma M, Mungan G, Can M, Demirtas S. Comparison of angiotensin-converting enzyme, malonaldehyde, zinc, and copper levels in preeclampsia. Biol Trace Elem Res. 2006;113:1–8.
Zadrozna M, Gawlik M, Nowak B, Marcinek A, Mrowiec H, Walas S, et al. Antioxidants activities and concentration of selenium, zinc and copper in preterm and IUGR human placentas. J Trace Elem Med Biol. 2009;23:144–8.
Asano N, Kondoh M, Ebihara C, Fujii M, Nakanishi T, Soares MJ, et al. Expression profiles of zinc transporters in rodent placental models. Toxicol Lett. 2004;154:45–53.
Vargas Zapata CL, Trugo NM, Donangelo CM. Zinc uptake by human placental microvillous membrane vesicles : effects of gestational age and maternal serum zinc levels. Biol Trace Elem Res. 2000;73:127–37.
Zhou C, Zhang R, Cai X, Xiao R, Yu H. Trace elements profiles of maternal blood, umbilical cord blood, and placenta in Beijing. China J Matern Fetal Neonatal Med. 2019;32:1755–61.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Higgins JP, Green S. Cochrane handbook for systematic reviews of interventions. Wiley; 2011. pp. 187–241.
Atinmo T, Mbofung C, Osinusi BO. Relationship of zinc and copper concentrations in maternal and cord blood and birth weight. Int J Gynaecol Obstet. 1980;18:452–4.
Bermúdez L, García-Vicent C, López J, Torró MI, Lurbe E. Assessment of ten trace elements in umbilical cord blood and maternal blood: association with birth weight. J Transl Med. 2015;13:291.
Boskabadi H, Maamouri G, Nori M, Mohsenzadeh H, Ayatollahi H, Ghayour-Mobarhan M, et al. Maternal and neonatal serum concentrations of zinc and copper in preterm delivery: an observational study. Trace Elem Electrol. 2012;29:232.
Elizabeth K, Krishnan V, Vijayakumar T. Umbilical cord blood nutrients in low birth weight babies in relation to birth weight & gestational age. Indian J Med Res. 2008;128:128–33.
Frković A, Međugorac B, Alebić-Juretić A. Umbilical cord blood zinc levels in normal and pathological pregnancies. Int J Gynaecol Obstet. 1997;57:181–2.
Gómez T, Bequer L, Mollineda A, González O, Diaz M, Fernández D. Serum zinc levels of cord blood: relation to birth weight and gestational period. J Trace Elem Med Biol. 2015;30:180–3.
Hosseini SA, Ghalesardi OK, Kamaei Z, Aghili S, Ashtary-Larky D, Hoseininejad SS, et al. Associations of maternal serum zonulin and elements concentrations with neonatal birth weight: a case-control study. J Clin Diagn Res. 2017;11:SC01–4.
Jeswani RM, Vani SN. A study of serum zinc levels in cord blood of neonates and their mothers. Indian J Pediatr. 1991;58:683–6.
Katz O, Paz-Tal O, Lazer T, Aricha-Tamir B, Mazor M, Wiznitzer A, et al. Severe pre-eclampsia is associated with abnormal trace elements concentrations in maternal and fetal blood. J Matern Fetal Neonatal Med. 2012;25:1127–30.
Kiilholma P, Paul R, Pakarinen P, Gränroos M. Copper and zinc in pre-eclampsia. Acta Obstet Gynecol Scand. 1984;63:629–31.
Kumar A, Pandey M, Basu S, Shukla RC, Asthana RK. Thymic size correlates with cord blood zinc levels in low-birth-weight newborns. Eur J Pediatr. 2014;173:1083–7.
Lazer T, Paz-Tal O, Katz O, Aricha-Tamir B, Sheleg Y, Maman R, et al. Trace elements' concentrations in maternal and umbilical cord plasma at term gestation: a comparison between active labor and elective cesarean delivery. J Matern Fetal Neonatal Med. 2012;25:286–9.
Osada H, Watanabe Y, Nishimura Y, Yukawa M, Seki K, Sekiya S. Profile of trace element concentrations in the feto-placental unit in relation to fetal growth. Acta Obstet Gynecol Scand. 2002;81:931–7.
Pintov S, Kohelet D, Arbel E, Goldberg M. Predictive inability of cord zinc, magnesium and copper levels on the development of benign hyperbilirubinemia in the newborn. Acta Pædiatr. 1992;81:868–9.
Sabra S, Malmqvist E, Saborit A, Gratacós E, Gomez Roig MD. Heavy metals exposure levels and their correlation with different clinical forms of fetal growth restriction. PLoS ONE. 2017;12:e0185645.
Schulpis KH, Karakonstantakis T, Vlachos GD, Mentis AF, Karikas GA, Afordakou D, et al. Maternal-neonatal magnesium and zinc serum concentrations after vaginal delivery. Scand J Clin Lab Invest. 2010;70:465–9.
Sharma R, Tewari K, Singhal K, Gupta MV. Zinc levels in maternal and cord blood and in amniotic fluid—a possible marker for foetal malformation. Indian J Physiol Pharmacol. 1994;38:300–2.
Srivastava S, Mehrotra PK, Srivastava SP, Tandon I, Siddiqui MK. Blood lead and zinc in pregnant women and their offspring in intrauterine growth retardation cases. J Anal Toxicol. 2001;25:461–5.
Srivastava S, Mehrotra PK, Srivastava SP, Siddiqui MK. Some essential elements in maternal and cord blood in relation to birth weight and gestational age of the baby. Biol Trace Elem Res. 2002;86:97–105.
Tsuzuki S, Morimoto N, Hosokawa S, Matsushita T. Associations of maternal and neonatal serum trace element concentrations with neonatal birth weight. PLoS One. 2013;8:e75627.
Vigeh M, Yokoyama K, Ramezanzadeh F, Dahaghin M, Sakai T, Morita Y, et al. Lead and other trace metals in preeclampsia: a case–control study in Tehran. Iran Environ Res. 2006;100:268–75.
Zeyrek D, Soran M, Cakmak A, Kocyigit A, Iscan A. Serum copper and zinc levels in mothers and cord blood of their newborn infants with neural tube defects: a case-control study. Indian Pediatr. 2009;46:675–80.
Zheng G, Zhong H, Guo Z, Wu Z, Zhang H, Wang C, et al. Levels of heavy metals and trace elements in umbilical cord blood and the risk of adverse pregnancy outcomes: a population-based study. Biol Trace Elem Res. 2014;160:437–44.
Ota E, Mori R, Middleton P, Tobe-Gai R, Mahomed K, Miyazaki C, et al. Zinc supplementation for improving pregnancy and infant outcome. Cochrane Database Syst Rev. 2015;2:CD000230.
Gebreselassie SG, Gashe FE. A systematic review of effect of prenatal zinc supplementation on birthweight: meta-analysis of 17 randomized controlled trials. J Health Popul Nutr. 2011;29:134–40.
Hess SY, King JC. Effects of maternal zinc supplementation on pregnancy and lactation outcomes. Food Nutr Bull. 2009;30(Suppl 1):S60–78.
Ma Y, Shen X, Zhang D. The relationship between serum zinc level and preeclampsia: a meta-analysis. Nutrients. 2015;7:7806–20.
He L, Lang L, Li Y, Liu Q, Yao Y. Comparison of serum zinc, calcium, and magnesium concentrations in women with pregnancy-induced hypertension and healthy pregnant women: a meta-analysis. Hypertens Pregnancy. 2016;35:202–9.
Zhu Q, Zhang L, Chen X, Zhou J, Liu J, Chen J. Association between zinc level and the risk of preeclampsia: a meta-analysis. Arch Gynecol Obstet. 2016;293:377–82.
Song X, Li B, Li Z, Wang J, Zhang D. High serum copper level is associated with an increased risk of preeclampsia in Asians: a meta-analysis. Nutr Res. 2017;39:14–24.
Lazebnik N, Kuhnert BR, Kuhnert PM. Zinc, cadmium, and hypertension in parturient women. Am J Obstet Gynecol. 1989;161:437–40.
Laine JE, Ray P, Bodnar W, Cable PH, Boggess K, Offenbacher S, et al. Placental cadmium levels are associated with increased preeclampsia risk. PLoS One. 2015;10:e0139341.
Kucukaydin Z, Kurdoglu M, Kurdoglu Z, Demir H, Yoruk IH. Selected maternal, fetal and placental trace element and heavy metal and maternal vitamin levels in preterm deliveries with or without preterm premature rupture of membranes. J Obstet Gynaecol Res. 2018;44:880–9.
Llanos MN, Ronco AM. Fetal growth restriction is related to placental levels of cadmium, lead and arsenic but not with antioxidant activities. Reprod Toxicol. 2009;27:88–92.
Malhotra A, Fairweather-Tait SJ, Wharton PA, Gee H. Placental zinc in normal and intra-uterine growth-retarded pregnancies. Br J Nutr. 1990;63:613–21.
Funding
None.
Author information
Authors and Affiliations
Contributions
NY designed the study and outlined the parts, read through the manuscript and made corrections, and managed the literature searches and discussion. SA wrote the first draft of the manuscript and managed the literature searches. Both authors participated in the analysis of the data, and read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not needed.
Conflict of interest
There is no conflict of interest in connection with this paper. No financial or non-financial benefits have been received or will be received from any party related directly or indirectly to the subject of this article and the material described is not under publication or consideration for publication elsewhere.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Akdas, S., Yazihan, N. Cord blood zinc status effects on pregnancy outcomes and its relation with maternal serum zinc levels: a systematic review and meta-analysis. World J Pediatr 16, 366–376 (2020). https://doi.org/10.1007/s12519-019-00305-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-019-00305-8