Abstract
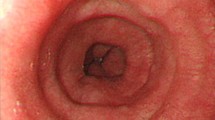
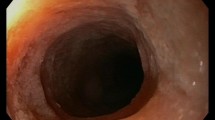
A 46-year-old woman presented at our hospital with anorexia, vomiting, and diarrhea. Blood tests indicated markedly increased eosinophil counts, and esophagogastroduodenoscopy revealed slight erythema in the gastric body. Computed tomography showed edematous thickening of the stomach and small intestinal walls and peritonitis. Thus, eosinophilic gastrointestinal disease was suspected. Endoscopic biopsies from the esophagus, stomach, and duodenum were collected, but no significant increases in eosinophil counts were observed. Little ascites effusion was detected and puncture cytology was difficult to perform. Thus, a sample of the muscularis propria layer was obtained by mucosal incision-assisted biopsy. Histopathological examination of the biopsy revealed significant eosinophilic infiltration within the muscularis propria layer of the stomach, confirming the diagnosis of non-eosinophilic esophagitis eosinophilic gastrointestinal disease. The patient was treated with a leukotriene receptor antagonist and prednisolone, and her clinical symptoms and gastrointestinal wall thickening rapidly improved. The Japanese diagnostic guideline for non-eosinophilic esophagitis eosinophilic gastrointestinal disease requires endoscopic biopsy or eosinophilic infiltration of ascites fluid. When diagnosis is difficult using conventional methods, as in this case, mucosal incision-assisted biopsy is useful as a next step.






Similar content being viewed by others
References
Dellon ES, Gonsalves N, Abonia JP, et al. International consensus recommendations for eosinophilic gastrointestinal disease nomenclature. Clin Gastroenterol Hepatol. 2022;20:2474-84.e3.
Klein NC, Hargrove RL, Sleisenger MH, et al. Eosinophilic gastroenteritis. Med (Balti). 1970;49:299–319.
Talley NJ, Shorter RG, Phillips SF, et al. Eosinophilic gastroenteritis: a clinicopathological study of patients with disease of the mucosa, muscularis propria layer, and subserosal tissues. Gut. 1990;31:54–8.
de Chambrun GP, Gonzalez F, Canva JY, et al. Natural history of eosinophilic gastroenteritis. Clin Gastroenterol Hepatol. 2011;9:950–6.
Yamamoto M, Nagashima S, Yamada Y, et al. Comparison of non-esophageal eosinophilic gastrointestinal disorders with eosinophilic esophagitis: a nationwide survey. J Allergy Clin Immunol Pract. 2021;9:3339–49.
Kinoshita Y, Oouchi S, Fujisawa T. Eosinophilic gastrointestinal disease—pathogenesis, diagnosis, and treatment. Allergol Int. 2019;68:420–9.
Dellon ES, Gonsalves N, Rothenberg ME, et al. Determination of biopsy yield that optimally detects eosinophilic gastritis and/or duodenitis in a randomized trial of lirentelimab. Clin Gastroenterol Hepatol. 2022;20:535-45.e15.
Ingle SB, Hinge Ingle CR. Eosinophilic gastroenteritis: an unusual type of gastroenteritis. World J Gastroenterol. 2013;19:5061–6.
Kinoshita Y, Furuta K, Ishimaru N, et al. Clinical characteristics of Japanese patients with eosinophilic esophagitis and eosinophilic gastroenteritis. J Gastroenterol. 2013;48:333–9.
Mizukami K, Matsunari O, Ogawa R, et al. Examine the availability and safety of mucosal cutting biopsy technique for diagnosis of gastric submucosal tumor. Gastroenterol Res Pract. 2019;2019:3121695.
Dhaliwal A, Kolli S, Dhindsa BS, et al. Clinical efficacy and safety of mucosal incision-assisted biopsy for the diagnosis of upper gastrointestinal subepithelial tumors: a systematic review and meta-analysis. Ann Gastroenterol. 2020;33:155–61.
Sato H, Takeuchi M, Takahashi K, et al. Nutcracker and jackhammer esophagus treatment: a three-case survey, including two novel cases of eosinophilic infiltration into the muscularis propria. Endoscopy. 2015;47:855–7.
Acknowledgements
This work was supported in part by Grants-in-Aid for Research from the National Center for Global Health and Medicine (23A 3002).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions.
Informed consent
Informed consent was obtained from the patient included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Watanabe, R., Yada, T., Yoshida, A. et al. A case of non-esophageal eosinophilic gastrointestinal disease diagnosed by mucosal incision-assisted biopsy. Clin J Gastroenterol 17, 228–233 (2024). https://doi.org/10.1007/s12328-023-01905-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-023-01905-8