Abstract
Purpose
Reverse shoulder arthroplasty becomes more widely used as treatment for patients with complex cuff arthropathy. Theoretically, a higher retroversion of the humeral component leads to an increase in external rotation ROM and a decrease in internal rotation ROM. There is no consensus in optimal retroversion orientation. We retrospectively describe the effect of retroversion of the humeral component. We hypothesize that 20° humeral retroversion improves postoperative ROM, strength or clinical outcome scores compared to neutral retroversion.
Methods
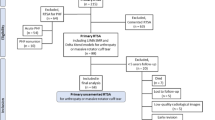
A retrospective clinical study is performed. An Aequalis reverse shoulder prosthesis was placed in 65 shoulders from 58 patients with a mean age of 73.8 years (95% CI 72.0–75.6). Between October 2006 and May 2012, the humeral component was placed in neutral retroversion in 36 shoulders (55%). From June 2012 to June 2014, it was placed in 20° retroversion in 29 shoulders (45%). After a mean follow-up of 36 months with a minimum of 12 months, patients were invited for a study visit. ROM, strength, Constant-Murley and Oxford Scores were measured.
Results
ROM, strength and Constant-Murley and Oxford Scores did not differ significantly between both groups.
Conclusions
With the Aequalis prosthesis, no significant effect of 0° or 20° retroversion on external and internal rotation ROM, strength or functional outcome scores was found.





Similar content being viewed by others
References
Oppermann J, Celik E, Bredow J et al (2016) Shoulder arthroplasty in Germany: 2005–2012. Arch Orthop Trauma Surg 136:723–729. doi:10.1007/s00402-016-2417-9
Boileau P, Watkinson DJ, Hatzidakis AM, Balg F (2005) Grammont reverse prosthesis: design, rationale, and biomechanics. J Shoulder Elb Surg 14(S1):S147–S161. doi:10.1016/j.jse.2004.10.006
Grammont PM, Baulot E (1993) Delta shoulder prosthesis for rotator cuff rupture. Orthopedics 16:65–68
Stephenson DR, Oh JH, Rick Hatch GF, Lee TQ (2011) Effect of humeral component version on impingement in reverse total shoulder arthroplasty. J Shoulder Elb Surg 20:652–658. doi:10.1016/j.jse.2010.08.020
Gulotta LV, Choi D, Marinello P, Knutson Z, Lipman J, Wright T, Cordasco FA, Craig EV, Warren RF (2012) Humeral component retroversion in reverse total shoulder arthroplasty: a biomechanical study. J Shoulder Elb Surg 21:1121–1127. doi:10.1016/j.jse.2011.07.027
Karelse AT, Bhatia DN, De Wilde LF (2008) Prosthetic component relationship of the reverse Delta III total shoulder prosthesis in the transverse plane of the body. J Shoulder Elb Surg 17:602–607. doi:10.1016/j.jse.2008.02.005
Nalbone L, Adelfio R, D’arienzo M et al (2014) Optimal positioning of the humeral component in the reverse shoulder prosthesis. Musculoskelet Surg 98:135–142. doi:10.1007/s12306-013-0274-z
Berhouet J, Garaud P, Favard L (2013) Influence of glenoid component design and humeral component retroversion on internal and external rotation in reverse shoulder arthroplasty: a cadaver study. Orthop Traumatol Surg Res 99:887–894. doi:10.1016/j.otsr.2013.08.008
Rhee YG, Cho NS, Moon SC (2015) Effects of humeral component retroversion on functional outcomes in reverse total shoulder arthroplasty for cuff tear arthropathy. J Shoulder Elb Surg 24:1574–1581. doi:10.1016/j.jse.2015.03.026
Ji JH, Jeong JY, Song HS et al (2013) Early clinical results of reverse total shoulder arthroplasty in the Korean population. J Shoulder Elb Surg 22:1102–1107. doi:10.1016/j.jse.2012.07.019
Constant CR, Murley AH (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 214:160–164. doi:10.1097/00003086-198701000-00023
Dawson J, Fitzpatrick R, Carr A (1996) Questionnaire on the perceptions of patients about shoulder surgery. J Bone Joint Surg Br 78:593–600
Kukkonen J, Kauko T, Vahlberg T, Joukainen A, Aärimaa V (2013) Investigating minimal clinically important difference for constant score in patients undergoing rotator cuff surgery. J Shoulder Elb Surg 22:1650–1655. doi:10.1016/j.jse.2013.05.002
Favre P, Sussmann PS, Gerber C (2010) The effect of component positioning on intrinsic stability of the reverse shoulder arthroplasty. J Shoulder Elb Surg 19:550–556. doi:10.1016/j.jse.2009.11.044
Berliner JL, Regalado-Magdos A, Ma CB, Feeley BT (2015) Biomechanics of reverse total shoulder arthroplasty. J Shoulder Elb Surg 24:150–160. doi:10.1016/j.jse.2014.08.003
Katolik LI, Romeo AA, Cole BJ, Verma NN, Hayden JK, Bach BR (2005) Normalization of the constant score. J Shoulder Elb Surg 14:279–285. doi:10.1016/j.jse.2004.10.009
Berhouet J, Garaud P, Favard L (2014) Evaluation of the role of glenosphere design and humeral component retroversion in avoiding scapular notching during reverse shoulder arthroplasty. J Shoulder Elb Surg 23:151–158. doi:10.1016/j.jse.2013.05.009
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
de Boer, F.A., van Kampen, P.M. & Huijsmans, P.E. Is there any influence of humeral component retroversion on range of motion and clinical outcome in reverse shoulder arthroplasty? A clinical study. Musculoskelet Surg 101, 85–89 (2017). https://doi.org/10.1007/s12306-016-0443-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-016-0443-y