Abstract
Background
Chronic pain is a major complication following breast surgery including breast reconstruction. We previously examined prospective patient-specific and medical/surgical factors that predict chronic pain a year after breast surgery in the Japanese population. Five-year survivorship is essential for breast cancer patients. This report is a 4-year follow-up study following the previous research.
Methods
A follow-up observation study was performed 5 years after breast operations. The subjects were patients who underwent breast surgery, including tissue expander/implant (TE/implant), DIEP procedures and mastectomy only. Pain at 5 years was assessed using the Japanese Version of the Short-Form McGill Pain Questionnaire (SF-MPQ-JV). A multiple linear regression model was used to examine the relationships of clinical factors with chronic pain.
Results
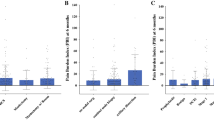
Questionnaires were completed by 132 subjects. No factor related to chronic pain was significantly related to the MPQ pain ratings. Among patient characteristics, a psychotic or neurological medical history was related to significantly lower visual analog scale (p = 0.02) and present pain index (p = 0.04) scores. A history of chemotherapy and/or hormone therapy was significantly associated with the frequency of use of pain medication postoperatively (p = 0.05) and effect on the social life of the patients (p = 0.02).
Conclusions
A psychotic or neurological history and a history of chemotherapy and/or hormone therapy were identified as risk factors for chronic pain after breast surgery, but the type of operation was not associated with chronic pain.


Similar content being viewed by others
Data availability
Data for this study are available upon request.
References
Bell RJ, Robinson PJ, Nazeem F, Panjari M, Fradkin P, Schwarz M, et al. Persistent breast pain 5 years after treatment of invasive breast cancer is largely unexplained by factors associated with treatment. J Cancer Surviv. 2014;8:1–8.
Wallace MS, Wallace AM, Lee J, Dobke MK. Pain after breast surgery: a survey of 282 women. Pain. 1996;66:195–205.
The International Association for the Study of Pain (IASP). Classification of chronic pain. Descriptions of chronic pain syndromes and definitions of pain terms. Prepared by the international association for the study of pain. Subcomm Taxon Pain Suppl. 1986;3:S1-226.
Hickey OT, Nugent NF, Burke SM, Hafeez P, Mudrakouski AL, Shorten GD. Persistent pain after mastectomy with reconstruction. J Clin Anesth. 2011;23:482–8.
Vadivelu N, Schreck M, Lopez J, Kodumudi G, Narayan D. Pain after mastectomy and breast reconstruction. Am Surg. 2008;74:285–96.
Macdonald L, Bruce J, Scott NW, Smith WC, Chambers WA. Long-term follow-up of breast cancer survivors with post-mastectomy pain syndrome. Br J Cancer. 2005;92:225–30.
Waltho D, Rockwell G. Post-breast surgery pain syndrome: establishing a consensus for the definition of post-mastectomy pain syndrome to provide a standardized clinical and research approach–a review of the literature and discussion. Can J Surg. 2016;59:342–50.
Matros E, Albornoz CR, Razdan SN, Mehrara BJ, Macadam SA, Ro T, et al. Cost-effectiveness analysis of implants versus autologous perforator flaps using the BREAST-Q. Plast Reconstr Surg. 2015;135:937–46.
Hu ES, Pusic AL, Waljee JF, Kuhn L, Hawley ST, Wilkins E, et al. Patient-reported aesthetic satisfaction with breast reconstruction during the long-term survivorship period. Plast Reconstr Surg. 2009;124:1–8.
Dean C, Chetty U, Forrest AP. Effects of immediate breast reconstruction on psychosocial morbidity after mastectomy. Lancet. 1983;1:459–62.
Shiraishi M, Sowa Y, Inafuku N. Long-term survey of sexual well-being after breast reconstruction using the BREAST-Q in the Japanese population. Asian J Surg. 2022;S1015–9584(22):00108–17.
Urits I, Lavin C, Patel M, Maganty N, Jacobson X, Ngo AL, et al. Chronic pain following cosmetic breast surgery: a comprehensive review. Pain Ther. 2020;9:71–82.
Roth RS, Qi J, Hamill JB, Kim HM, Ballard TNS, Pusic AL, et al. Is chronic postsurgical pain surgery-induced? A study of persistent postoperative pain following breast reconstruction. Breast. 2018;37:119–25.
Shiraishi M, Sowa Y, Fujikawa K, Kodama T, Okamoto A, Numajiri T, et al. Factors associated with chronic pain following breast reconstruction in Japanese women. J Plast Surg Hand Surg. 2020;54:317–22.
Okuyama A, Barclay M, Chen C, Higashi T. Impact of loss-to-follow-up on cancer survival estimates for small populations: a simulation study using hospital-based cancer registries in japan. BMJ Open. 2020;10: e033510.
Ellington TD, Henley SJ, Wilson RJ, Miller JW. Breast cancer survival among males by race, ethnicity, age, geographic region, and stage—United States, 2007–2016. MMWR Morb Mortal Wkly Rep. 2020;69:1481–4.
Melzack R. The short-form McGill pain questionnaire. Pain. 1987;30:191–7.
Yamaguchi M, Kumano H, Yamauchi Y, Kadota Y, Iseki M. The development of a Japanese version of the short-form McGill pain questionnaire. JJSPC. 2007;14:9–14.
Gärtner R, Jensen MB, Nielsen J, Ewertz M, Kroman N, Kehlet H. Prevalence of and factors associated with persistent pain following breast cancer surgery. JAMA. 2009;302:1985–92.
Schreiber KL, Martel MO, Shnol H, Shaffer JR, Greco C, Viray N, et al. Persistent pain in postmastectomy patients: comparison of psychophysical, medical, surgical, and psychosocial characteristics between patients with and without pain. Pain. 2013;154:660–8.
Andersen KG, Duriaud HM, Jensen HE, Kroman N, Kehlet H. Predictive factors for the development of persistent pain after breast cancer surgery. Pain. 2015;156:2413–22.
Hermesdorf M, Berger K, Baune BT, Wellmann J, Ruscheweyh R, Wersching H. Pain sensitivity in patients with major depression: differential effect of pain sensitivity measures, somatic cofactors, and disease characteristics. J Pain. 2016;17:606–16.
Belfer I, Schreiber KL, Shaffer JR, Shnol H, Blaney K, Morando A, et al. Persistent postmastectomy pain in breast cancer survivors: analysis of clinical, demographic, and psychosocial factors. J Pain. 2013;14:1185–95.
Singh JA, Lewallen DG. Medical and psychological comorbidity predicts poor pain outcomes after total knee arthroplasty. Rheumatology (Oxford). 2013;52:916–23.
Glare PA, Davies PS, Finlay E, Gulati A, Lemanne D, Moryl N, et al. Pain in cancer survivors. J Clin Oncol. 2014;32:1739–47.
Hershman DL, Weimer LH, Wang A, Kranwinkel G, Brafman L, Fuentes D, et al. Association between patient reported outcomes and quantitative sensory tests for measuring long-term neurotoxicity in breast cancer survivors treated with adjuvant paclitaxel chemotherapy. Breast Cancer Res Treat. 2011;125:767–74. https://doi.org/10.1007/s10549-010-1278-0.
Eckhoff L, Knoop A, Jensen MB, Ewertz M. Persistence of docetaxel-induced neuropathy and impact on quality of life among breast cancer survivors. Eur J Cancer. 2015;51:292–300.
Tanabe Y, Hashimoto K, Shimizu C, Hirakawa A, Harano K, Yunokawa M, et al. Paclitaxel-induced peripheral neuropathy in patients receiving adjuvant chemotherapy for breast cancer. Int J Clin Oncol. 2013;18:132–8.
Bao T, Basal C, Seluzicki C, Li SQ, Seidman AD, Mao JJ. Long-term chemotherapy-induced peripheral neuropathy among breast cancer survivors: prevalence, risk factors, and fall risk. Breast Cancer Res Treat. 2016;159:327–33.
Ganz PA, Desmond KA, Leedham B, Rowland JH, Meyerowitz BE, Belin TR. Quality of life in long-term, disease-free survivors of breast cancer: a follow-up study. J Natl Cancer Inst. 2002;94:39–49.
Ganz PA, Rowland JH, Desmond K, Meyerowitz BE, Wyatt GE. Life after breast cancer: understanding women’s health-related quality of life and sexual functioning. J Clin Oncol. 1998;16:501–14.
Ganz PA, Desmond KA, Belin TR, Meyerowitz BE, Rowland JH. Predictors of sexual health in women after a breast cancer diagnosis. J Clin Oncol. 1999;17:2371–80.
Acknowledgements
We thank Toru Ogura, PhD. and Satoshi Tamaru, MD, PhD. from Clinical Research Support Center, Mie University Hospital, Tsu, Japan for their valuable assistance in the bio-statistical analysis.
Funding
Costs related to statistical analysis and manuscript publication were funded by the Department of Plastic and Reconstructive Surgery, Kyoto Prefectural University of Medicine.
Author information
Authors and Affiliations
Contributions
MS and YS designed the study. MS, YS, AS, and NI participated in the acquisition of data. MS, YS, IT, AS, NI, IN, and NM participated in the analysis and interpretation of the data. MS drafted the manuscript. MS, YS, IT, AS, NI, IN, and NM revised the manuscript. All authors approved the final version of the manuscript, and agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors state that they have no conflict of interest.
Ethics statement
The involvement of human participants in the study was reviewed and approved by the KPUM Institutional Review Board and the study was conducted in accordance with the ethical standards of institutional and national research committees (Kyoto Prefectural University of Medicine IRBMED Number ERB-C-563–1). Participants provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Shiraishi, M., Sowa, Y., Tsuge, I. et al. Risk factors associated with chronic pain after mastectomy: a prospective study with a 5-year follow-up in Japan. Breast Cancer 29, 1133–1139 (2022). https://doi.org/10.1007/s12282-022-01392-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-022-01392-8