Abstract
Purpose of Review
This study aimed to isolate and characterize filamentous fungi onychomycosis agents in a military population assisted at a hospital outpatient clinic.
Recent Findings
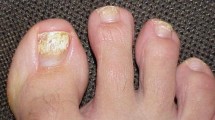
In onychomycosis, the fungi colonize the subungual region causing thickening, discoloration, or cracking of the nail bed. Samples were collected from patients with clinical sights of onychomycosis.
Summary
Among 80 samples collected, 50 (62.5%) had positive culture. Isolated dermatophytes (86%) were Trichophyton rubrum (21; 42%), T. mentagrophytes var. interdigitale (19; 38%), and Microsporum gypseum (3; 6%) and non-dermatophyte molds were Fusarium spp. (1; 2%), Scytalidium spp. (1; 2%), and Chaetomium globosum (5; 10%). Minimal inhibitory concentrations (mg/L) of terbinafine, itraconazole, and fluconazole necessary to inhibit 50/90% of the isolates were respectively 0.015/0.06, 0.06/0.12, and 32/32. Etiological agents of onychomycosis in a military hospital are similar as reported in studies for the general population. High prevalence of non-dermatophytic agents was observed, especially for Chaetomium globosum.
Similar content being viewed by others
References
Ghannoum MA, Hajjeh RA, Scher R, Konnikov N, Gupta AK, Summerbell R, et al. A large-scale North American study of fungal isolates from nails: the frequency of onychomycosis, fungal distribution, and antifungal susceptibility patterns. J Am Acad Dermatol. 2000;43:641–8.
Mahoney JM, Bennet J, Olsen B. The diagnosis of onychomycosis. Dermatol Clin. 2003;21:463–7.
Elewski BE. Onychomycosis: pathogenesis, diagnosis, and management. Clin Microbiol Rev. 1998;11(3):415–29.
Katoh T. Guidelines for diagnosis and treatment of mucocutaneous candidiasis. Jpn J Med Mycol. 2009;50:207–12.
Iorizzo M, Piraccini BM, Rech G, Tosti A. Treatment of onychomycosis with oral antifungal agents. Expert Opin Drug Deliv. 2005;2:435–40.
Stüttgen G, Bauer E. Bioavailability, skin- and nailpenetration of topically applied antimycotics. Mycoses. 1982;25:74–80.
Santos DA, Barros MES, Hamdan JS. Establishing a method of inoculum preparation for susceptibility testing of Trichophyton rubrum and Trichophyton mentagrophytes. J Clin Microbiol. 2006;44:98–101.
Silva Barros ME, de Assis SD, Hamdan JS. Evaluation of susceptibility of Trichophyton mentagrophytes and Trichophyton rubrum clinical isolates to antifungal drugs using a modified CLSI microdilution method (M38-A). J Med Microbiol. 2007;56:514–8.
Ameen M, Lear JT, Madan V, Mohd Mustapa MF, Richardson M. British Association of Dermatologists’ guidelines for the management of onychomycosis. Br J Dermatol. 2014;171:937–58.
Roberts DT. Prevalence of dermatophyte onychomycosis in the United Kingdom: results of an omnibus survey. Br J Dermatol. 1992;126:23–7.
Aly R. Ecology and epidemiology of dermatophyte infections. J Am Acad Dermatol. 1994;31:21–5.
Scher RK, Baran R. Onychomycosis in clinical practice: factors contributing to recurrence. Br J Dermatol. 2003;149:5–9.
Segal R, Shemer A, Hochberg M, et al. Onychomycosis in Israel: epidemiological aspects. Mycoses. 2015;58:133–9.
Drakensjö IT, Chryssanthou E. Epidemiology of dermatophyte infections in Stockholm, Sweden: a retrospective study from 2005–2009. Med Mycol. 2011;49:484–8.
Saunte D, Svejgaard E, Haedersdal M, Frimodt-Møller N, Jensen AM, Arendrup CM. Laboratory-based survey of dermatophyte infections in Denmark over a 10-year period. Acta Derm Venereol. 2008;88:614–6.
Tchernev G, Penev PK, Nenoff P, et al. Onychomycosis: modern diagnostic and treatment approaches. Wien Med Wochenschr. 2013;163:1–12.
Dolenc-Voljc M. Dermatophyte infections in the Ljubljana region, Slovenia, 1995–2002. Mycoses. 2005;48:181–6.
Garg A, Venkatesh V, Singh M, Pathak KP, Kaushal GP, Agrawal SK. Onychomycosis in central India: a clinicoetiologic correlation. Int J Dermatol. 2004;43:498–502.
Nzenze Afene S, Ngoungou EB, Mabika Mamfoumbi M, Bouyou Akotet MK, Avome Mba IM, Kombila M. Les onychomycoses au Gabon: aspects cliniques et mycologiques. J Mycol Med. 2011;21:248–55.
Summerbell RC, Cooper E, Bunn U, Jamieson F, Gupta AK. Onychomycosis: a critical study of techniques and criteria for confirming the etiologic significance of nondermatophytes. Med Mycol. 2005;43:39–59.
Gupta AK, Cooper EA, MacDonald P, Summerbell RC. Utility of inoculum counting (Walshe and English criteria) in clinical diagnosis of onychomycosis caused by nondermatophytic filamentous fungi. J Clin Microbiol. 2001;39:2115–22.
Kemna ASCP, Elewski BE. A U.S. epidemiologic survey of superficial fungal diseases. J Am Acad Dermatol. 1996;35:539–42.
Koussidou T, Devliotou-Panagiotidou D, Karakatsanis G, et al. Onychomycosis in Northern Greece during 1994–1998. Mycoses. 2002;45:29–37.
Gianni C, Cerri A, Crosti C. Non-dermatophytic onychomycosis. An underestimated entity? A study of 51 cases. Mycoses. 2000;43:29–33.
Tosti A, Piraccini BM, Lorenzi S. Onychomycosis caused by nondermatophytic molds: clinical features and response to treatment of 59 cases. J Am Acad Dermatol. 2000;42:217–24.
Heikkila H, Stubb S. The prevalence of onychomycosis in Finland. Br J Dermatol. 1995;133:699–703.
Clayton YM. Clinical and mycological diagnostic aspects of onychomycoses and dermatomycoses. Clin Exp Dermatol. 1992;17:37–40.
Maraki S, Nioti E, Mantadakis E, Tselentis Y. A 7-year survey of dermatophytoses in Crete, Greece. Mycoses. 2007;50:481–4.
El Sayed F, Ammoury A, Haybe RF, Dhaybi R. Onychomycosis in Lebanon: a mycological survey of 772 patients. Mycoses. 2006;49:216–9.
Gupta AK, Jain HC, Lynde CW, Watteel GN, Summerbell RC. Prevalence and epidemiology of unsuspected onychomycosis in patients visiting dermatologists’ offices in Ontario, Canada—a multicenter survey of 2001 patients. Int J Dermatol. 1997;6:783–7.
Araújo AJG, Souza MAJ, Bastos OM, Oliveira JC. Onychomycosis caused by emergent fungi: clinical analysis, diagnosis and revision. An Bras Dermatol. 2003;78:445–55.
Brilhante RSN, Paixão GC, Salvino LK, Diógenes MJN, Bandeira SP, Rocha MFG, et al. Epidemiologia e ecologia das dermatofitoses na cidade de Fortaleza: o Trichophyton tonsurans como importante patógeno emergente da Tinea capitis. Rev Soc Bras Med Trop. 2000;33:417–25.
Costa M, Passos XS, Souza LKH, Miranda ATB, Lemos JÁ, Júnior JGO, et al. Epidemiologia e etiologia das dermatofitoses em Goiânia, GO, Brasil. Rev Soc Bras Med Trop. 2002;35:19–22.
Lacaz CS, Porto E, Melo NT. Guia para identificação: fungos, actimomicetos e algas de interesse medico. 1a edição. São Paulo: Savier; 1998.
Bassiri-Jahromi S, Khaksar AA. Nondermatophytic moulds as a causative agent of onychomycosis in Tehran. Indian J Dermatol. 2010;55:140–3.
Hilmioğlu-Polat S, Metin DY, Inci R, Dereli T, Kilinç I, Tümbay E. Non-dermatophytic molds as agents of onychomycosis in Izmir, Turkey—a prospective study. Mycopathologia. 2005;160:125–8.
Ramani R, Srinivas CR, Ramani A, Kumari TG, Shivananda PG. Molds in onychomycosis. Int J Dermatol. 1993;32:877–8.
Stiller MJ, Rosenthal S, Summerbell RC, et al. Onychomycosis of the toenails caused by Chaetomium globosum. J Am Acad Dermatol. 1992;26:775–6.
Rippon JW. Medical mycology: the pathogenic fungi and the pathogenic actinomycetes, 3rd ed. Philadelphia: W.B. Saunders Co.; 1988.
Hattori N, Adachi M, Kaneko T, Shimozuma M, Ichinohe M, Iozumi K. Case report. Onychomycosis due to Chaetomium globosum successfully treated with itraconazole. Mycoses. 2000;43:89–92.
Naidu J, Singh SM, Pouranik M. Onychomycosis caused by Chaetomium globosum Kunze. Mycopathologia. 1991;113:31–4.
Fernández-Torres B, Carrillo AJ, Martín E, Del Palacio A, Moore MK, Valverde A, et al. In vitro activities of 10 antifungal drugs against 508 dermatophyte strains. Antimicrob Agents Chemother. 2001;45:2524–8.
Mukherjee PK, Leidich SD, Isham N, Leitner I, Ryder NS, Ghannoum MA. Clinical Trichophyton rubrum strain exhibiting primary resistance to terbinafine. Antimicrob Agents Chemother. 2003;47:82–6.
Tamura T, Asahara M, Yamamoto M, Yamaura M, Matsumura M, Goto K, et al. In vitro susceptibility of dermatomycoses agents to six antifungal drugs and evalution by fractional inhibitory concentration index of combined effects of amorolfine and itraconazole in dematophytes. Microbiol Immunol. 2014;58:1–8.
Carrillo-Muñoz AJ, Guglietta A, Palacín C, Casals J, del Valle O, Guardià C, et al. In vitro antifungal activity of sertaconazole compared with nine other drugs against 250 clinical isolates of dermatophytes and Scopulariopsis brevicaulis. Chemotherapy. 2004;50:308–13.
Yamazaki H, Nakamoto M, Shimizu M, Murayama N, Niwa T. Potential impact of cytochrome P450 3A5 in human liver on drug interactions with triazoles. Br J Clin Pharmacol. 2010;69:593–7.
Jessup CJ, Ryder NS, Ghannoum MA. An evaluation of the in vitro activity of terbinafine. Med Mycol. 2000;38:155–9.
Osborne CS, Hofbauer B, Favre B, Ryder NS. In vitro analysis of the ability of Trichophyton rubrum to become resistant to terbinafine. Antimicrob Agents Chemother. 2003;47:3634–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Clinical Mycology Lab Issues
Rights and permissions
About this article
Cite this article
Bentine, L.L.M., Bonfietti, L.X., Szeszs, M.W. et al. Onychomycoses in a Military Population in Brazil. Curr Fungal Infect Rep 11, 171–175 (2017). https://doi.org/10.1007/s12281-017-0291-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12281-017-0291-8