Abstract
Ultrasound enhancing agents are approved to delineate the endocardial border and opacify the left ventricle cavity (LVC). We present a nested phase change agent (NPCA) designed to enable selective myocardial enhancement without enhancing the LVC by employing a dual-activation mechanism dependent on sufficient ultrasound intensity and the microenvironment of the myocardium. Swine received bolus injections of NPCA while echocardiograms were collected and processed to determine background-subtracted acoustic intensities (AI) in the LVC and septal myocardium. At mechanical index (MI) ≥ 0.8, the NPCA enhanced the myocardium selectively (p < 0.001) while the LVC remained at baseline AI. A 5-mL bolus of NPCA enhanced swine myocardium and enhancement persisted for > 5 min at 1.4 MI, while hemodynamics and EKG remained normal. Our findings demonstrate that the NPCA enhances swine myocardium selectively without enhancing the LVC. The NPCA could have utility for functional and structural echocardiographic studies with clinical ultrasound using standard settings.
Graphical abstract





Similar content being viewed by others
Abbreviations
- LVC:
-
Left ventricle cavity
- NPCA:
-
Nested phase change agent
- MI:
-
Mechanical index
- AI:
-
Acoustic intensity
- SER:
-
Selective enhancement ratio
- EMA:
-
European Medicines Agency
- FDA:
-
Food & Drug Administration
- MPI:
-
Myocardial perfusion imaging
- cMRI:
-
Cardiac magnetic resonance imaging
- PET:
-
Positron emission tomography
- SPECT:
-
Single-photon emission computed tomography
- UEA:
-
Ultrasound enhancing agent
- PCA:
-
Phase change agent
References
DeMaria, A. N., Cotter, B., & Ohmori, K. (1998). Myocardial contrast echocardiography: Too much, too soon? Journal of the American College of Cardiology, 32(5), 1270–1271. https://doi.org/10.1016/S0735-1097(98)00415-X
Thomas, J. D. (2013). Myocardial contrast echocardiography perfusion imaging: Still waiting after all these years. Journal of the American College of Cardiology, 62(15), 1362–1364. https://doi.org/10.1016/j.jacc.2013.05.053
Kaul, S. (2010). Myocardial contrast echocardiography. A wondrous journey! JACC: Cardiovascular Imaging, 3(2), 212–218. https://doi.org/10.1016/j.jcmg.2009.11.003
Porter, T. R., & Xie, F. (2010). Myocardial perfusion imaging with contrast ultrasound. JACC: Cardiovascular imaging, 3(2), 176–187. https://doi.org/10.1016/j.jcmg.2009.09.024
Davidson, B. P., Arthur, S., & Doyle, C. (2019). Making the case for ischemia : Using myocardial contrast echocardiography to understand when the (circumstantial) evidence doesn’t add up. Journal of the American Society of Echocardiography, 32(9), 1102–1104. https://doi.org/10.1016/j.echo.2019.07.009
Gramiak, R., Shah, P. M., & Kramer, D. H. (1969). Ultrasound cardiography: Contrast studies in anatomy and function. Radiology, 92(5), 939–948. https://doi.org/10.1148/92.5.939
Porter, T. R., Mulvagh, S. L., Abdelmoneim, S. S., Becher, H., Belcik, J. T., Bierig, M., & Villanueva, F. (2018). Clinical applications of ultrasonic enhancing agents in echocardiography: 2018 American Society of Echocardiography Guidelines Update. Journal of the American Society of Echocardiography, 31(3), 241–274. https://doi.org/10.1016/j.echo.2017.11.013
Leighton, T. G. (2005). The Acoustic Bubble. The Journal of the Acoustical Society of America (Vol. 96). Harcourt Brace & Company, Publishers. https://doi.org/10.1121/1.410082
Imaging, L. M. (2011). Definity: Perflutren lipid microspheres. U.S. Food and Drug Administration. Retrieved from https://www.accessdata.fda.gov/drugsatfda_docs/label/2015/021064s017lbl.pdf
Porter, T. R., & Xie, F. (1995). Transient myocardial contrast after initial exposure to diagnostic ultrasound pressures with minute doses of intravenously injected microbubbles. Circulation, 92(9), 2391–2395. https://doi.org/10.1161/01.CIR.92.9.2391
Porter, T. R., Li, S., Kricsfeld, D., & Armbruster, R. W. (1997). Detection of myocardial perfusion in multiple echocardiographic windows with one intravenous injection of microtubules using transient response second harmonic imaging. Journal of the American College of Cardiology, 29(4), 791–799. https://doi.org/10.1016/S0735-1097(96)00575-X
Senior, R., Moreo, A., Gaibazzi, N., Agati, L., Tiemann, K., Shivalkar, B., & Kasprzak, J. D. (2013). Comparison of sulfur hexafluoride microbubble (SonoVue)-enhanced myocardial contrast echocardiography with gated single-photon emission computed tomography for detection of significant coronary artery disease: A large European multicenter study. Journal of the American College of Cardiology, 62(15), 1353–1361. https://doi.org/10.1016/j.jacc.2013.04.082
Wei, K., Crouse, L., Weiss, J., Villanueva, F., Schiller, N. B., Naqvi, T. Z., & DeMaria, A. (2003). Comparison of usefulness of dipyridamole stress myocardial contrast echocardiography to technetium-99m sestamibi single-photon emission computed tomography for detection of coronary artery disease (PB127 multicenter phase 2 trial results). American Journal of Cardiology, 91(11), 1293–1298. https://doi.org/10.1016/S0002-9149(03)00316-3
Marwick, T. H., Brunken, R., Meland, N., Brochet, E., Baer, F. M., Binder, T., & Lindvall, K. (1998). Accuracy and feasibility of contrast echocardiography for detection of perfusion defects in routine practice. Journal of the American College of Cardiology, 32(5), 1260–1269. https://doi.org/10.1016/S0735-1097(98)00373-8
Senior, R., Monaghan, M., Main, M. L., Zamorano, J. L., Tiemann, K., Agati, L., & Picard, M. H. (2009). Detection of coronary artery disease with perfusion stress echocardiography using a novel ultrasound imaging agent: Two phase 3 international trials in comparison with radionuclide perfusion imaging. European Journal of Echocardiography, 10(1), 26–35. https://doi.org/10.1093/ejechocard/jen321
Choudhury, S. A., Xie, F., Kutty, S., Lof, J., Stolze, E., & Porter, T. R. (2018). Selective infarct zone imaging with intravenous acoustically activated droplets. PLoS ONE, 13(12), 1–15. https://doi.org/10.1371/journal.pone.0207486
Choudhury, S. A., Xie, F., Dayton, P. A., & Porter, T. R. (2016). Acoustic behavior of a reactivated, commercially available ultrasound contrast agent. Journal of the American Society of Echocardiography, 30(2), 1–9. https://doi.org/10.1016/j.echo.2016.10.015
Cimorelli, M., Angel, B., Fafarman, A., Kohut, A., Andrien, B., Barrett, K., & Wrenn, S. (2018). Introducing a nested phase change agent with an acoustic response that depends on electric field: A candidate for myocardial perfusion imaging and drug delivery. Applied Acoustics, 138(February), 9–17. https://doi.org/10.1016/j.apacoust.2018.03.028
Cimorelli, M., Flynn, M. A., Angel, B., Reimold, E., Fafarman, A., Huneke, R., & Wrenn, S. (2020). A voltage-sensitive ultrasound enhancing agent for myocardial perfusion imaging in a rat model. Ultrasound in Medicine and Biology, 46(9), 2388–2399. https://doi.org/10.1016/j.ultrasmedbio.2020.05.015
Cimorelli, M., Flynn, M. A., Angel, B., Fafarman, A., Kohut, A., & Wrenn, S. (2020). An ultrasound enhancing agent with nonlinear acoustic activity that depends on the presence of an electric field. Ultrasound in Medicine and Biology, 46(9), 2370–2387. https://doi.org/10.1016/j.ultrasmedbio.2020.04.038
Porter, T. R., Arena, C., Sayyed, S., Lof, J., High, R. R., Xie, F., & Dayton, P. A. (2016). Targeted transthoracic acoustic activation of systemically administered nanodroplets to detect myocardial perfusion abnormalities. Circulation: Cardiovascular Imaging, 9(1), 1–9. https://doi.org/10.1161/CIRCIMAGING.115.003770
Seol, S. H., Davidson, B. P., Belcik, J. T., Mott, B. H., Goodman, R. M., Ammi, A., & Lindner, J. R. (2015). Real-time contrast ultrasound muscle perfusion imaging with intermediate-power imaging coupled with acoustically durable microbubbles. Journal of the American Society of Echocardiography, 28(6), 718-726.e2. https://doi.org/10.1016/j.echo.2015.02.002
Matsunaga, T. O., Sheeran, P. S., Luois, S., Streeter, J. E., Mullin, L. B., Banerjee, B., & Dayton, P. A. (2012). Phase-change nanoparticles using highly volatile perfluorocarbons: Toward a platform for extravascular ultrasound imaging. Theranostics, 2(12), 1185–1198. https://doi.org/10.7150/thno.4846
Sheeran, P. S., & Dayton, P. A. (2012). Phase-change contrast agents for imaging and therapy. Current pharmaceutical design, 18(15), 2152–2165. https://doi.org/10.2174/138161212800099883
Porter, T. R., Xie, F., Lof, J., Powers, J., Vignon, F., Shi, W., & White, M. (2017). The thrombolytic effect of diagnostic ultrasound–induced microbubble cavitation in acute carotid thromboembolism. Investigative Radiology, 52(8), 477–481. https://doi.org/10.1097/RLI.0000000000000369
du Sert, N. P., Ahluwalia, A., Alam, S., Avey, M. T., Baker, M., Browne, W. J., … Würbel, H. (2020). Reporting animal research: Explanation and elaboration for the arrive guidelines 2.0. PLoS Biology (Vol. 18). https://doi.org/10.1371/journal.pbio.3000411
Crisóstomo, V., Sun, F., Maynar, M., Báez-Díaz, C., Blanco, V., Garcia-Lindo, M., & Sánchez-Margallo, F. M. (2016). Common swine models of cardiovascular disease for research and training. Lab Animal, 45(2), 67–74. https://doi.org/10.1038/laban.935
Wallace, N., Dicker, S., Lewin, P., & Wrenn, S. P. (2014). Influence of nesting shell size on brightness longevity and resistance to ultrasound-induced dissolution during enhanced B-mode contrast imaging. Ultrasonics, 54(8), 2099–2108. https://doi.org/10.1016/j.ultras.2014.06.019
Beppu, S., Matsuda, H., Shishido, T., Matsumura, M., & Miyatake, K. (1997). Prolonged myocardial contrast echocardiography via peripheral venous administration of QW3600 Injection (EchoGen®): Its efficacy and side effects. Journal of the American Society of Echocardiography, 10(1), 11–24. https://doi.org/10.1016/S0894-7317(97)80028-4
Øistensen, J., Hede, R., Myreng, Y., Ege, T., & Holtz, E. (1992). Intravenous injection of AlbunexR microspheres causes thromboxane mediated pulmonary hypertension in pigs, but not in monkeys or rabbits. Acta Physiologica Scandinavica, 144(3), 307–315. https://doi.org/10.1111/j.1748-1716.1992.tb09299.x
Funding
This study was supported by the Coulter-Drexel Translational Research Partnership Program and the Department of Education (Award No. P200 A150240).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics Approval and Consent to Participate
No human studies were carried out by the authors for this article.
Competing Interests
Drs. Angel, Cimorelli, Fafarman, Kohut, and Wrenn are co-inventors on an issued patent covering the voltage-sensitive nesting architecture described in this study. Drs. Angel, Cimorelli, Fafarman, Kohut, and Wrenn and Mr. Flynn are co-founders and own equity of Sonnest, Inc. Mr. Andrien, Dr. Cimorelli, and Mr. Flynn are employees at Sonnest, Inc., while Drs. Angel, Kohut, and Wrenn are consultants at Sonnest, Inc. All other authors declare no conflicts of interest.
Additional information
Communicated by Associate Editor Paul Jozine ter Maaten oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
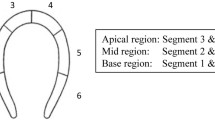
Supplemental video 2 Demonstrationof image processing to quantify acoustic intensity in regions of interest. The Brightness (B)-mode videos are loaded into custom software that was developed in Python 3.8.0 to quantify the average brightness in arbitrary units (a.u.) in the left ventricle cavity (LVC, red) and the septal myocardium (green) by digitizing the pixels from 0 (black) to 255 (white) in an ellipse with a predefined area of 2,000 pixels while tracking their movement throughout the cardiac cycle. The two ellipses are repositioned frame by frame to remain within the LVC and septal myocardium. The average brightness is determined for each 15-second increment and is shown above. (MP4 9088 KB)
Supplemental video 3 (MP4 34423 KB)
Rights and permissions
About this article
Cite this article
Cimorelli, M., Flynn, M.A., Angel, B. et al. Selective Enhancement of Swine Myocardium with a Novel Ultrasound Enhancing Agent During Transthoracic Echocardiography. J. of Cardiovasc. Trans. Res. 15, 722–729 (2022). https://doi.org/10.1007/s12265-022-10207-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-022-10207-2