Abstract
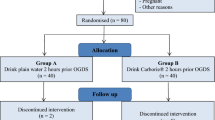
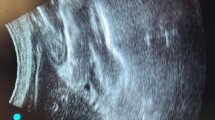
Perioperative aspiration of gastric contents is a rare but serious complication of anaesthesia. Recent fasting guidelines recommend 2 h of fasting for clear fluids before surgery, to avoid aspiration but are often over looked in clinical practice. Our aim is to overcome these issues by using ultrasound to quantify gastric volume as our primary objective. Patients with ASA grade I with age group between 18 and 60 years undergoing elective surgery with general anaesthesia requiring tracheal intubation were randomized in overnight fasting group (group A) and 2-h fasting group with 200 ml of clear apple juice (group B). Ultrasound-guided gastric volume was calculated preoperatively, and gastric pH was measured immediately post-tracheal intubation using pH strip paper. In a total of 60 patients, the mean gastric volume by USG in group A is 29.7 ± 8.0 ml and group B is 19.2 ± 4.9 ml. The reduced gastric volume in group B is statistically significant (< 0.00001). The mean pH of gastric aspirate in group A is 1.4, and group B is 1.6 with statistically insignificant p value (p < 0.1268) which shows that pH in both the groups was almost same. The mean gastric volume in patients who had 200 ml of clear apple juice 2 h prior (group B) to non-abdominal surgery was lesser than patients who fasted overnight (group A). It supports the fasting guidelines which help in reducing the preoperative discomfort of long fasting hours and dehydration of patients, whereas the mean pH was almost the same for both the groups. Clinical trial registration: CTRI/2018/07/014851.
Summary Statement Not applicable.



Similar content being viewed by others
References
Van de Putte P, Perlas A (2014) Ultrasound assessment of gastric content and volume. Br J Anaesth 113(1):12–22
Smith I, Kranke P, Murat I, Smith A, O'Sullivan G, Søreide E, Spies C, in't Veld B, European Society of Anaesthesiology (2011) Perioperative fasting in adults and children: guidelines from the European Society of Anaesthesiology. Eur J Anaesthesiol 28:556–569
Practice guidelines for preoperative fasting, the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures. An updated report by the American Society of Anaesthesiologists Committee on Standards, Practice Parameter. Anesthesiology.2011; 114:495---511
Cotton BR, Smith G (1984) The lower oesophageal sphincter and anaesthesia. Br J Anaesth 56:37–46
Vanner RG, Pryle BJ, O’Dwyer JP, Reynolds F (1992) Upper oesophageal sphincter pressure and the intravenous induction of anesthesia. Anaesthesia 47:371–375
Dalal KS, Rajwade D, Suchak R (2010) “Nil per oral after midnight”: is it necessary for clear fluids? Indian J Anaesth 54:445–447
Splinter WM, Schafer JD (1991) Ingestion of clear fluid safe for adolescents up to 3 hours before anaesthesia. Br J Anaesth 66:48–52
Jayaram A, Bowen MP, Deshpande S, Carp HM (1997) Ultrasound examination of the stomach contents of women in the postpartum period. Anesth Analg 84:522–526
Perlas A (2013) Validation of a mathematical model for ultrasound assessment of gastric volume by gastroscopic examination. Anesth Analg 116(2):357–363
Kwiatek MA, Menne D, Steingoetter A, Goetze O, Forras-Kaufman Z, Kaufman E, Fruehauf H, Boesiger P, Fried M, Schwizer W, Fox MR (2009) Effect of meal volume and calorie load on postprandial gastric function and emptying: studies under physiological conditions by combined fiber-optic pressure measurement and MRI. Am J Physiol Gastrointest Liver Physiol 297:G894–G901
Delgado Aros S, Camilleri M, Castillo EJ, Cremoni F, Stephens D, Ferber I, Baxter K, Burton D, Zinsmeister AR (2005) Effect of gastric volume or emptying on meal related symptoms after liquid nutrients in obesity: a pharmacologic study. Clin Gastroenterol Heptal 3:9971006
Riaz Hussain, Tahir Nazeer, Nasrullah Khan Aziz, Maqsood Ali, Effects of fasting intervals on gastric volume and pH, P j m h s :5(3): 582–86
Bisinottoa FMB, de Araújo Naves A, Lima HM, Peixotoe ACA, Maia GC, Paulo Pacheco Resende LBM Jr, Matias da Silveira LA (2017) Use of ultrasound for gastric volume evaluation after ingestion of different volumes of isotonic solution. Rev Bras Anestesiol 67(4):376–382
Crawford MJ, Christian S, Farroio Gillespie A (1991) Effect of clear liquids on gastric volume and pH and volume in healthy children. Can J Anaesth 38:8
Ploutz-Snyder L, Foley J, Ploutz-Snyder R, Kanaley J, Sagendorf K, Meyer R (1999) Gastric gas and fluid emptying assessed by magnetic resonance imaging. Eur J Appl Physiol Occup Physiol 79:212–220
Lobo DN, Hendry PO, Rodrigues G et al (2009) Gastric emptying of three liquid oral preoperative metabolic preconditioning regimens measured by magnetic resonance imaging in healthy adult volunteers: a randomised double-blind, crossover study. Clin Nutr 28:636–641
Naslund E, Bogefors J, Gryback H (2000) Gastric emptying: comparison of scintigraphic, polyethylene glycol dilution and paracetamol tracer techniques. Scand J Gastroenterol 35:375–379
Hillyard S, Cowman S, Ramasundaram R, Seed PT, O'Sullivan G (2014) Does adding milk to tea delay gastric emptying? Br J Anaesth 112:66–71
Schmitz A, Kellenberger CJ, Neuhaus D et al (2011) Fasting times and gastric contents volume in children undergoing deep propofol sedation—an assessment using magnetic resonance imaging. Paediatr Anaesth 21:685–690
Schwizer W, Maecke H, Fried M (1992) Measurement of gastric emptying by magnetic resonance imaging in humans. Gastroenterology 103:369–376
Fruehauf H, Goetze O, Steingoetter A et al (2007) Intersubject and intrasubject variability of gastric volumes in response to isocaloric liquid meals in functional dyspepsia and health. Neurogastroenterol Motil 19:553–561
Mcgrady EM, Macdonald AG (1988) Effect of the preoperative administration of water on gastric volume and pH. Br J Anaesth 60:803–805
Phillips S, Hutchinson S, Davidson T (1993) Preoperative drinking does not affect gastric contents. Br J Anaesth 70:6–9
Malcolm Scarr J, Maltby R, Jani K, Sutherland LR (1989) Volume and acidity of residual gastric fluid after oral fluid ingestion before elective ambulatory surgery. CMAJ 141(december 1):1151
Availability of Data and Material
Partial availability.
Code Availability
Not applicable.
Funding
Support was provided solely from institutional and departmental sources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Joshi, Y., Dhamija, S. Randomized Control Clinical Trial of Overnight Fasting to Clear Fluid Feeding 2 Hours Prior Anaesthesia and Surgery. Indian J Surg 83, 248–254 (2021). https://doi.org/10.1007/s12262-020-02369-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-020-02369-7