Abstract
Objective
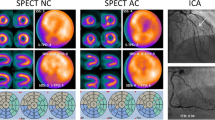
An iterative reconstruction method in combination with resolution recovery, attenuation and scatter corrections (IR-RASC) can improve image quality. It, however, is undetermined whether this technique can improve the detection of coronary artery disease (CAD) when automated quantitative analysis is used. This study evaluated diagnostic values of IR-RASC in combination with automated quantitative analysis in stress myocardial perfusion imaging (MPI) in the CAD detection.
Methods
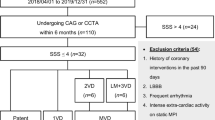
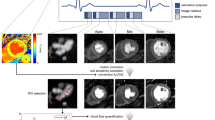
This study enrolled consecutive 64 patients (mean age 66.2 ± 17.3 years, 39 males) who had undergone both 99mTc-labeled tetrofosmin stress MPI and coronary angiography within 3 months. Stress MPI abnormalities quantified as summed stress score (SSS), summed rest score (SRS) and summed difference score (SDS) by Heart Risk View-S (HRV-S) and Quantitative Perfusion SPECT (QPS) softwares using IR-RASC images were compared with those by using conventional filtered back-projection method (FBP) images and angiographic findings.
Results
Based on expert visual assessment, SSS and SRS by HRV-S/QPS softwares with IR-RASC were significantly lower than those by HRV-S/QPS softwares with FBP at mid- and basal left ventricular segments. Receiver-operating characteristics analysis showed that areas under the curve assessed by HRV-S (0.687) and QPS (0.678) with IR-RASC were nearly identical to those (0.717–0.724) by expert assessment with FBP, and were significantly (P < 0.05) greater than those by HRV-S (0.505) and QPS (0.522) with FBP. When HRV-S was used, the specificity and diagnostic accuracy of IR-RASC in the CAD detection were significantly greater than those of FBP: 90.3 versus 51.6%, P < 0.0001 and 79.7 versus 54.7%, P = 0.0027, respectively. Likewise, when QPS was used, the specificity and diagnostic accuracy of IR-RASC in the CAD detection were significantly greater than those of FBP: 80.6 versus 41.9%, P < 0.0001, and 78.1 versus 51.6%, P = 0.0018, respectively. There, however, were no significant differences in sensitivity between IR-RASC and FBP images.
Conclusions
IR-RASC can improve diagnostic accuracy of the CAD detection using an automated scoring system compared to FBP, by reducing false positivity due to artefactual appearance.







Similar content being viewed by others
References
Akalin EN, Yaylali O, Kirac FS, Yuksel D, Kilic M. The role of myocardial perfusion gated SPECT study in women with coronary artery disease: a correlative study. Mol Imaging Radionucl Ther. 2012;21:69–74.
Chen GB, Wu H, He XJ, Huang JX, Yu D, Xu WY, et al. Adenosine stress thallium-201 myocardial perfusion imaging for detecting coronary artery disease at an early stage. J Xray Sci Technol. 2013;21:317–22.
Hachamovitch R, Berman DS, Shaw LJ, Kiat H, Cohen I, Cabico JA, et al. Incremental prognostic value of myocardial perfusion single photon emission computed tomography for the prediction of cardiac death: differential stratification for risk of cardiac death and myocardial infarction. Circulation. 1998;97:535–43.
Nishimura T, Nakajima K, Kusuoka H, Yamashina A, Nishimura S. Prognostic study of risk stratification among Japanese patients with ischemic heart disease using gated myocardial perfusion SPECT: J-ACCESS study. Eur J Nucl Med Mol Imaging. 2008;35:319–28.
Shaw LJ, Berman DS, Maron DJ, Mancini GB, Hayes SW, Hartigan PM, et al. Optimal medical therapy with or without percutaneous coronary intervention to reduce ischemic burden: results from the Clinical Outcomes Utilizing Revascularization and Aggressive Drug Evaluation (COURAGE) trial nuclear substudy. Circulation. 2008;117:1283–91.
Slomka PJ, Nishina H, Berman DS, Akincioglu C, Abidov A, Friedman JD, et al. Automated quantification of myocardial perfusion SPECT using simplified normal limits. J Nucl Cardiol. 2005;12:66–77.
Nanasato M, Morita S, Yoshida R, Niimi T, Sugimoto M, Tsukamoto K, et al. Detection of coronary artery disease using automated quantitation of myocardial perfusion on single-photon emission computed tomography images from patients with angina pectoris without prior myocardial infarction. Circ J. 2012;76:2280–2.
Nakajima K, Matsuo S, Okuda K, Wakabayashi H, Tsukamoto K, Nishimura T. Estimation of cardiac event risk by gated myocardial perfusion imaging and quantitative scoring methods based on a multi-center J-ACCESS database. Circ J. 2011;75:2417–23.
Iwasaki T, Kurisu S, Abe N, Tamura M, Watanabe N, Ikenaga H, et al. Validation of automated quantification of myocardial perfusion single-photon emission computed tomography using Heart Score View in patients with known or suspected coronary artery disease. Int Heart J. 2014;55:350–6.
Nakata T, Hashimoto A, Matsuki T, Yoshinaga K, Tsukamoto K, Tamaki N. Prognostic value of automated SPECT scoring system for coronary artery disease in stress myocardial perfusion and fatty acid metabolism imaging. Int J Cardiovasc Imaging. 2013;29:253–62.
Shepp LA, Vardi Y. Maximum likelihood reconstruction for emission tomography. IEEE Trans Med Imaging. 1982;1:113–22.
Hudson HM, Larkin RS. Accelerated image reconstruction using ordered subsets of projection data. IEEE Trans Med Imaging. 1994;13:601–9.
Narayanan MV, King MA, Pretorius PH, Dahlberg ST, Spencer F, Simon E, et al. Human-observer receiver-operating-characteristic evaluation of attenuation, scatter, and resolution compensation strategies for (99 m)Tc myocardial perfusion imaging. J Nucl Med. 2003;44:1725–34.
Okuda K, Nakajima K, Yamada M, Wakabayashi H, Ichikawa H, Arai H, et al. Optimization of iterative reconstruction parameters with attenuation correction, scatter correction and resolution recovery in myocardial perfusion SPECT/CT. Ann Nucl Med. 2014;28:60–8.
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK, et al. Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart. A statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Int J Cardiovasc Imaging. 2002;18:539–42.
Nakajima K, Kumita S, Ishida Y, Momose M, Hashimoto J, Morita K, et al. Creation and characterization of Japanese standards for myocardial perfusion SPECT: database from the Japanese Society of Nuclear Medicine Working Group. Ann Nucl Med. 2007;21:505–11.
Sampson UK, Dorbala S, Limaye A, Kwong R, Di Carli MF. Diagnostic accuracy of rubidium-82 myocardial perfusion imaging with hybrid positron emission tomography/computed tomography in the detection of coronary artery disease. J Am Coll Cardiol. 2007;49:1052–8.
Imaging guidelines for nuclear cardiology procedures, part 2. American Society of Nuclear Cardiology. J Nucl Cardiol. 1999;6:G47–G84.
Yoshinaga K, Matsuki T, Hashimoto A, Tsukamoto K, Nakata T, Tamaki N. Validation of automated quantitation of myocardial perfusion and fatty acid metabolism abnormalities on SPECT images. Circ J. 2011;75:2187–95.
Zoccarato O, Scabbio C, De Ponti E, Matheoud R, Leva L, Morzenti S, et al. Comparative analysis of iterative reconstruction algorithms with resolution recovery for cardiac SPECT studies. A multi-center phantom study. J Nucl Cardiol. 2014;21:135–48.
Golub RJ, Ahlberg AW, McClellan JR, Herman SD, Travin MI, Mather JF, et al. Interpretive reproducibility of stress Tc-99 m sestamibi tomographic myocardial perfusion imaging. J Nucl Cardiol. 1999;6:257–69.
Sakatani T, Shimoo S, Takamatsu K, Kyodo A, Tsuji Y, Mera K, et al. Usefulness of the novel risk estimation software, Heart Risk View, for the prediction of cardiac events in patients with normal myocardial perfusion SPECT. Ann Nucl Med. 2016;. doi:10.1007/s12149-016-1117-4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared no conflicts of interest.
Rights and permissions
About this article
Cite this article
Chono, T., Onoguchi, M., Shibutani, T. et al. Improvement in automated quantitation of myocardial perfusion abnormality by using iterative reconstruction image in combination with resolution recovery, attenuation and scatter corrections for the detection of coronary artery disease. Ann Nucl Med 31, 181–189 (2017). https://doi.org/10.1007/s12149-016-1146-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-016-1146-z