Abstract
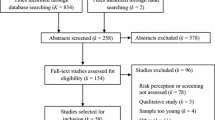
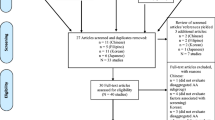
Risk perception, knowledge, and awareness are important predictors of colorectal cancer (CRC) behavior and screening. Misperception appears to be the cause of negative CRC behaviors and refusal to be screened. Here, we systematically reviewed qualitative studies to identify common CRC misperceptions in the general population. The PubMed, Web Of Science, and Scopus databases were searched to answer the research question. Original qualitative articles in English that addressed CRC risk and/or screening were included, whereas review articles and studies on health care provider misperceptions were excluded. The appropriate Health Belief Model (HBM) domains in the included studies were identified with thematic analysis. The quality of the included studies was assessed with the critical appraisal skills program (CASP) checklist. The review included 15 qualitative studies. There were two major HBM domains for misperception of CRC risk: high perceived severity (CRC is fatal and incurable) and low perceived susceptibility (older man’s disease, asymptomatic, sexual behavior). A high perceived barrier was that screening was considered embarrassing, painful, and inappropriate, leading to screening refusal, while a high perceived severity resulted in the belief that CRC is fatal but that screening is ineffective. Identifying the most common misperceptions enables the strategic planning of HBM-based interventions, and more engaging risk communication could improve CRC prevention and control.



Similar content being viewed by others
Data availability
Not applicable.
References
Anderson, R. M., & Funnell, M. M. (2010). Patient empowerment: Myths and misconceptions. Patient Education and Counseling, 79(3), 277–282. https://doi.org/10.1016/j.pec.2009.07.025
Bashirian, S., Barati, M., Mohammadi, Y., Moaddabshoar, L., & Dogonchi, M. (2019). An application of the protection motivation theory to predict breast self-examination behavior among female healthcare workers. European Journal of Breast Health, 15(2), 90–97. https://doi.org/10.5152/ejbh.2019.4537
Besharati, F., Karimi-Shahanjarini, A., Hazavehei, S. M. M., Bagheri, F., & Bashirian, S. (2018). Socio-culturally informed views influencing Iranian adults’ decision about Colorectal cancer screening: A qualitative study. International Journal of Cancer Management, 11(6), https://doi.org/10.5812/ijcm.9546
Betesh, A. L., & Schnoll-Sussman, F. H. (2021). Colorectal cancer screening in the elderly. Clinics in Geriatric Medicine, 37(1), 173–183. https://doi.org/10.1016/J.CGER.2020.08.012
Bettany-Saltikov, J., & McSherry, R. (2016). How to do a sytematic literature review in nursing: A step-by-step guide (2nd ed.). Open University Press.
Biswas, J. (2014). Debunk the myths: Oncologic misconceptions. The Indian Journal of Medical Research, 139(2), 185–187.
Breugom, A. J., Bastiaannet, E., Dekker, J. W. T., Wouters, M. W. J. M., van de Velde, C. J. H., & Liefers, G. J. (2018). Decrease in 30-day and one-year mortality over time in patients aged ≥ 75 years with stage I–III colon Cancer: A population-based study. European Journal of Surgical Oncology, 44(12), 1889–1893. https://doi.org/10.1016/j.ejso.2018.08.010
Butler, A., Hall, H., & Copnell, B. (2016). A guide to writing a qualitative systematic review protocol to Enhance evidence-based practice in nursing and health care. Worldviews on Evidence-Based Nursing, 13(3), 241–249. https://doi.org/10.1111/WVN.12134
Christodoulides, N., Lami, M., Malietzis, G., Rasheed, S., Tekkis, P., & Kontovounisios, C. (2020). Sporadic Colorectal cancer in adolescents and young adults: A scoping review of a growing healthcare concern. International Journal of Colorectal Disease, 35(8), 1413–1421. https://doi.org/10.1007/s00384-020-03660-5
Crawford, J., Ahmad, F., Beaton, D. E., & Bierman, A. S. (2015). Colorectal cancer screening behaviors among south Asian immigrants in Canada: A qualitative study. International Journal of Migration Health and Social Care, 11(2), 130–146. https://doi.org/10.1108/IJMHSC-09-2014-0037
Darker, C. (2013). Risk perception. In M. D. Gellman & J. R. Turner (Eds.), Encyclopedia of behavioral medicine (pp. 1689–1691). Springer. https://doi.org/10.1007/978-1-4419-1005-9_866
Day, L. W., & Velayos, F. (2015). Colorectal cancer screening and surveillance in the elderly: Updates and controversies. Gut and Liver, 9(2), 143–151. https://doi.org/10.5009/gnl14302
Dwyer, A. J., Weltzien, E. S., Harty, N. M., LeGrice, K. E., Pray, S. L. H., & Risendal, B. C. (2022). What makes for successful patient navigation implementation in cancer prevention and screening programs using an evaluation and sustainability framework. Cancer, 128(S13), 2636–2648. https://doi.org/10.1002/CNCR.34058
Ebell, M. H., Thai, T. N., & Royalty, K. J. (2018). Cancer screening recommendations: An international comparison of high income countries. Public Health Reviews, 39(1), 1–19. https://doi.org/10.1186/s40985-018-0080-0
Garcia, A. Z. G., Alvarez Buylla, H., Nicolas-Perez, N., D., & Quintero, E. (2014). Public awareness of colorectal cancer screening: knowledge, attitudes, and interventions for increasing screening uptake. ISRN Oncology, 2014, 1–19. https://doi.org/10.1155/2014/425787
Goldman, R. E., Diaz, J. A., & Kim, I. (2009). Perspectives of colorectal cancer risk and screening among dominicans and puerto ricans: Stigma and misperceptions. Qualitative Health Research, 19(11), 1559–1568. https://doi.org/10.1177/1049732309349359
Greiner, K. A., Born, W., Nollen, N., & Ahluwalia, J. S. (2005). Knowledge and perceptions of colorectal cancer screening among urban African Americans. Journal of General Internal Medicine, 20(11), 977–983. https://doi.org/10.1111/j.1525-1497.2005.0165.x
Gwede, C. K., Jean-Francois, E., Quinn, G. P., Wilson, S., Tarver, W. L., Thomas, K. B., Vadaparampil, S. T., & Meade, C. D. (2011). Perceptions of colorectal cancer among three ethnic subgroups of US blacks: A qualitative study. Journal of the National Medical Association, 103(8), 669–680. https://doi.org/10.1016/S0027-9684(15)30406-5
Han, P. K. J., Lehman, T. C., Massett, H., Lee, S. J. C., Klein, W. M. P., & Freedman, A. N. (2009). Conceptual problems in laypersons’ understanding of individualized cancer risk: A qualitative study. Health Expectations, 12(1), 4–17. https://doi.org/10.1111/J.1369-7625.2008.00524.X
Harkins, M. (2012). Managing Risk and Information Security: Protect to Enable (First edi). Apress. https://doi.org/10.1007/978-1-4302-5114-9_2
Hoffman-Goetz, L., Thomson, M. D., & Donelle, L. (2008). Reasons for declining colorectal cancer screening by older Canadians: A pilot study. Journal of Cancer Education, 23(1), 32–36. https://doi.org/10.1080/08858190701821188
Imperiale, T. F., Wagner, D. R., Lin, C. Y., Larkin, G. N., Rogge, J. D., & Ransohoff, D. F. (2000). Risk of advanced proximal Neoplasms in asymptomatic adults according to the distal colorectal findings. The New England Journal of Medicine, 343(3), 169–174. https://doi.org/10.1056/nejm200007203430302
Jensen, J. D., Scherr, C. L., Brown, N., Jones, C., Christy, K., & Hurley, R. J. (2014). Public estimates of cancer frequency: Cancer incidence perceptions mirror distorted media depictions. Journal of Health Communication, 19(5), 609–624. https://doi.org/10.1080/10810730.2013.837551
Kim, S. B. (2018). Unraveling the determinants to colorectal cancer screening among Asian Americans: A systematic literature review. Journal of Racial and Ethnic Health Disparities, 5(4), 683–699. https://doi.org/10.1007/s40615-017-0413-6
Koo, J. H., Leong, R. W. L., Ching, J., Yeoh, K. G., Wu, D. C., Murdani, A., Cai, Q., Chiu, H. M., Chong, V. H., Rerknimitr, R., Goh, K. L., Hilmi, I., Byeon, J. S., Niaz, S. K., Siddique, A., Wu, K. C., Matsuda, T., Makharia, G., Sollano, J., & Sung, J. J. Y. (2012). Knowledge of, attitudes toward, and barriers to participation of colorectal cancer screening tests in the Asia-Pacific region: A multicenter study. Gastrointestinal Endoscopy, 76(1), 126–135. https://doi.org/10.1016/J.GIE.2012.03.168
Kowalski, P., & Taylor, A. (2017). Reducing students’ misconceptions with Refutational Teaching: For Long-Term Retention, comprehension matters. Scholarship of Teaching and Learning in Psychology, 3. https://doi.org/10.1037/stl0000082
Lasser, K. E., Ayanian, J. Z., Fletcher, R. H., & Good, M. J. D. V. (2008). Barriers to colorectal cancer screening in community health centers: A qualitative study. BMC Family Practice, 9, 1–8. https://doi.org/10.1186/1471-2296-9-15
Lau, J., Lim, T. Z., Jianlin Wong, G., & Tan, K. K. (2020). The health belief model and colorectal cancer screening in the general population: A systematic review. Preventive Medicine Reports, 20,. https://doi.org/10.1016/j.pmedr.2020.101223
Lee, S. Y. (2018). Koreans’ awareness and preventive behaviors regarding colorectal cancer screening. Asian Pacific Journal of Cancer Prevention, 19(9), 2657–2664. https://doi.org/10.22034/APJCP.2018.19.9.2657
Lee, S. Y., & Lee, E. E. (2018). Cancer screening in Koreans: A focus group approach. BMC Public Health, 18(1), 1–12. https://doi.org/10.1186/s12889-018-5147-9
Lewandowska, A., Rudzki, G., Lewandowski, T., Stryjkowska-Góra, A., & Rudzki, S. (2022). Title: Risk factors for the diagnosis of Colorectal Cancer. Cancer Control : Journal of the Moffitt Cancer Center, 29. https://doi.org/10.1177/10732748211056692/ASSET/IMAGES/LARGE/10.1177_10732748211056692-FIG2.JPEG
Long, H. A., French, D. P., & Brooks, J. M. (2020). Optimising the value of the critical appraisal skills programme (CASP) tool for quality appraisal in qualitative synthesis. Research Methods in Medicine & Health Sciences, 1(1), 31–42. https://doi.org/10.1177/2632084320947559
Majidi, A., Majidi, S., Salimzadeh, S., Khazaee- Pool, M., Sadjadi, A., Salimzadeh, H., & Delavari, A. (2017). Cancer screening awareness and practice in a middle income country; a systematic review from Iran. Asian Pacific Journal of Cancer Prevention, 18(12), 3187–3194. https://doi.org/10.22034/APJCP.2017.18.12.3187
McCaffery, K., Borril, J., Williamson, S., Taylor, T., Sutton, S., Atkin, W., & Wardle, J. (2001). Declining the offer of flexible sigmoidoscopy screening for bowel cancer. Social Science & Medicine, 53(5), 679–691. https://doi.org/10.1016/s0277-9536(00)00375-0
Mi Oh, K., Park, B., & Jacobsen, K. H. (2021). A qualitative analysis of barriers to colorectal cancer screening among Korean Americans. Journal of Cancer Education, 36(2), 261–270. https://doi.org/10.1007/s13187-019-01621-3
Oh, K. M., Park, B., & Jacobsen, K. H. (2021). A qualitative analysis of barriers to colorectal cancer screening among Korean Americans. Journal of Cancer Education, 36(2), 261–270. https://doi.org/10.1007/s13187-019-01621-3
Olde Bekkink, M., Donders, A. R. T. R., Kooloos, J. G., de Waal, R. M. W., & Ruiter, D. J. (2016). Uncovering students’ misconceptions by assessment of their written questions. BMC Medical Education, 16(1), 221. https://doi.org/10.1186/s12909-016-0739-5
Paek, H. J., & Hove, T. (2017). Risk perceptions and risk characteristics. Oxford University Press.https://doi.org/10.1093/acrefore/9780190228613.013.283
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., Chou, R., Glanville, J., Grimshaw, J. M., Hróbjartsson, A., Lalu, M. M., Li, T., Loder, E. W., Mayo-Wilson, E., McDonald, S., & Moher, D. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ, 372,. https://doi.org/10.1136/bmj.n71
Qaseem, A., Crandall, C. J., Mustafa, R. A., Hicks, L. A., Wilt, T. J., Forciea, M. A., Fitterman, N., Horwitch, C. A., Kansagara, D., Maroto, M., McLean, R. M., Roa, J., & Tufte, J. (2019). Screening for colorectal cancer in asymptomatic average-risk adults: A guidance statement from the American College of Physicians. Annals of Internal Medicine, 171(9), 643–654. https://doi.org/10.7326/M19-0642
Ratnapradipa, K. L., Napit, K., Ranta, J., Luma, L. B., Dinkel, D., Robinson, T., Schabloske, L., & Watanabe-Galloway, S. (2023). Qualitative analysis of colorectal cancer screening in Rural Nebraska. Journal of Cancer Education: The Official Journal of the American Association for Cancer Education, 38(2), 652–663. https://doi.org/10.1007/s13187-022-02170-y
Rosenstock, I. M. (1974). Historical origins of the health belief model. Health Education Monographs, 2(4), 328–335. https://doi.org/10.1177/109019817400200403
Sawicki, T., Ruszkowska, M., Danielewicz, A., Niedźwiedzka, E., Arłukowicz, T., & Przybyłowicz, K. E. (2021). A review of colorectal cancer in terms of epidemiology, risk factors, development, symptoms and diagnosis. Cancers, 13(9), 1–23. https://doi.org/10.3390/cancers13092025
Shaukat, A., Kahi, C. J., Burke, C. A., Rabeneck, L., Sauer, B. G., & Rex, D. K. (2021). ACG clinical guidelines: Colorectal cancer screening 2021. The American Journal of Gastroenterology, 116(3), 458–479. https://doi.org/10.14309/AJG.0000000000001122
Su, T. T., Goh, J. Y., Tan, J., Muhaimah, A. R., Pigeneswaren, Y., Khairun, N. S., Normazidah, A. W., Tharisini, D. K., & Majid, H. A. (2013). Level of colorectal cancer awareness: A cross sectional exploratory study among multi-ethnic rural population in Malaysia. BMC Cancer 2013, 13(1), 1–8. https://doi.org/10.1186/1471-2407-13-376
Suantika, P. I. R., Hermayanti, Y., & Kurniawan, T. (2018). Factors associated with participation of nurses in early detection of cervical cancer. Belitung Nursing Journal, 5(1), 47–53. https://doi.org/10.33546/bnj.610
Sung, H., Ferlay, J., Siegel, R. L., Laversanne, M., Soerjomataram, I., Jemal, A., & Bray, F. (2021). Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: A Cancer Journal for Clinicians, 71(3), 209–249. https://doi.org/10.3322/CAAC.21660
Swapnajaswanth, M., Suman, G., Suryanarayana, S. P., & Murthy, N. S. (2014). Perception and practices on screening and vaccination for carcinoma cervix among female healthcare professional in Tertiary Care hospitals in Bangalore, India. Asian Pacific Journal of Cancer Prevention, 15(15), 6095–6098. https://doi.org/10.7314/APJCP.2014.15.15.6095
Tan, K. K., Lim, T. Z., Chew, E., Chow, W. M., & Koh, G. C. H. (2020). Colorectal cancer patients can be advocates for Colorectal cancer screening for their siblings: A study on siblings’ perspectives. Psycho-Oncology, 29(12), 2028–2032. https://doi.org/10.1002/pon.5496
Tong, A., Flemming, K., McInnes, E., Oliver, S., & Craig, J. (2012). Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Medical Research Methodology, 12(1). https://doi.org/10.1186/1471-2288-12-181
Unger-Saldaña, K., Saldaña-Tellez, M., Potter, M. B., Van Loon, K., Allen-Leigh, B., & Lajous, M. (2020). Barriers and facilitators for Colorectal cancer screening in a low-income urban community in Mexico City. Implementation Science Communications, 1(1), 1–15. https://doi.org/10.1186/s43058-020-00055-z
Valvo, F., Ciurlia, E., Avuzzi, B., Doci, R., Ducreux, M., Roelofsen, F., Roth, A., Trama, A., Wittekind, C., & Bosset, J. F. (2019). Cancer of the anal region. Critical Reviews in Oncology/Hematology, 135, 115–127. https://doi.org/10.1016/j.critrevonc.2018.12.007
Wilkins, T., McMechan, D., & Talukder, A. (2018). Colorectal cancer screening and prevention. American Family Physician, 97(10), 658–665.
Woudstra, A. J., Dekker, E., Essink-Bot, M. L., & Suurmond, J. (2016). Knowledge, attitudes and beliefs regarding Colorectal cancer screening among ethnic minority groups in the Netherlands – a qualitative study. Health Expectations, 19(6), 1312–1323. https://doi.org/10.1111/hex.12428
Yan, P., Jin Yu, C., Hafiz Haris, A. A., & Shih Yuan, A. (2017). Assessment of the level of knowledge of Colorectal cancer among public at outpatient clinics in Serdang Hospital: A survey based study. Medical Journal of Malaysia, 72(6), 338–344.
Zhang, X., Zhang, Y., Chen, J., Zhang, M., & Gong, N. (2021). Psychological distance: A qualitative study of screening barriers among first-degree relatives of Colorectal cancer patients. BMC Public Health, 21(1), 1–8. https://doi.org/10.1186/s12889-021-10786-w
Acknowledgements
We would like to thank the team for their continuous commitment and efforts in the completion of the manuscript. We also thank the Dean of the Faculty of Medicine, Universiti Kebangsaan Malaysia, for his endless support and motivation.
Funding
The authors received no funding.
Author information
Authors and Affiliations
Contributions
Conceptualization, N.M. and A.M.; methodology, R.H. and A.M.; analysis, All; writing—original draft preparation, N.M.; writing—review and editing, R.H., A.M. and N.M.; visualization, A.M.; supervision, A.M and R.H. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Conflict of interest
All authors declared no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 66.3 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Masdor, N.A., Nawi, A.M. & Hod, R. Understanding misperceptions of colorectal cancer risk and cancer screening based on the health belief model: a systematic review of qualitative literature. Curr Psychol 43, 13729–13741 (2024). https://doi.org/10.1007/s12144-023-05373-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-023-05373-8