Abstract
Background
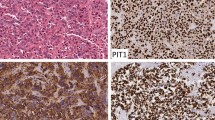
Columnar cell papillary thyroid carcinoma (CC-PTC) is a morphologic subtype of papillary thyroid carcinoma with a variable prognosis. It is characterized by neoplastic thyroid follicular-derived cells with pseudostratified columnar morphology arranged in papillary or follicular structures with supranuclear or subnuclear vacuoles. The molecular profile of this subtype has only recently come under scrutiny, with mixed results. The aim of this study is to further explore the morphologic, immunohistochemical, and genetic profile of CC-PTC, as well as to correlate these features with clinical outcomes.
Methods
CC-PTC cases were identified from 3 institutions. Immunohistochemistry (ER, CDX2) and molecular testing (DNA and RNA sequencing) were performed. Clinicopathologic parameters and patient outcomes were recorded.
Results
Twelve cases (2006–2023) were identified, all in adults (age 45–91). Two presented with disease outside the thyroid gland (neck and mediastinum) and two presented with distant metastasis. Four were high-grade differentiated thyroid carcinomas (necrosis or mitoses), one of which died of disease. Four were noninvasive or minimally invasive, one of which locally recurred. Three patients had lymph node metastases. ER and CDX2 were positive in 73% and 50%, respectively. Pathogenic mutations were found in TERT promoter (n = 3), RAS (n = 2), ATM, NOTCH1, APC, and ESR1, along with cases bearing AGK::BRAF fusion (n = 1), BRAF VE1 expression (n = 1), and NF2 loss (n = 1).
Conclusions
This study represents the largest molecularly defined cohort of non-oncocytic thyroid carcinomas with columnar cell morphology. These tumors represent a genetically and behaviorally heterogeneous group of neoplasms, some of which have RAS-like or follicular neoplasm-like genetics, some of which have BRAF-p.V600E-like or classic papillary thyroid carcinoma-like genetics, and some of which remain unclear. Noninvasive or minimally invasive tumors showed an indolent course compared to those with angioinvasion, gross extrathyroidal growth, or high-grade morphology. Consideration could be given to reclassification of this neoplasm outside of the subtyping of papillary thyroid carcinoma in light of its genetic diversity, distinct morphology, and clinical behavior more closely aligned with follicular thyroid neoplasms.


Similar content being viewed by others
Availability of Data and Materials
No additional data or materials are available outside this manuscript. Specific requests for data can be made to the corresponding author(s) if necessary.
References
WHO Classification of Tumours Editorial Board. Endocrine and neuroendocrine tumours [Internet]., 5th ed. International Agency for Research on Cancer., Lyon (France).
Evans HL (1986) Columnar-cell carcinoma of the thyroid. A report of two cases of an aggressive variant of thyroid carcinoma. Am J Clin Pathol 85:77–80. https://doi.org/10.1093/ajcp/85.1.77
Janovitz T, Williamson DFK, Wong KS et al (2021) Genomic profile of columnar cell variant of papillary thyroid carcinoma. Histopathology 79:491–498. https://doi.org/10.1111/his.14374
Sujoy V, Pinto A, Nosé V (2013) Columnar cell variant of papillary thyroid carcinoma: a study of 10 cases with emphasis on CDX2 expression. Thyroid 23:714–719. https://doi.org/10.1089/thy.2012.0455
Chen JH, Faquin WC, Lloyd RV, Nosé V (2011) Clinicopathological and molecular characterization of nine cases of columnar cell variant of papillary thyroid carcinoma. Mod Pathol 24:739–749. https://doi.org/10.1038/modpathol.2011.2
Barton CP, Brennan JA, Lowry TR, Russell MJ (2006) Columnar cell variant of papillary thyroid carcinoma. Ear Nose Throat J 85(640):643
Jiang C, Cheng T, Zheng X et al (2018) Clinical behaviors of rare variants of papillary thyroid carcinoma are associated with survival: a population-level analysis. Cancer Manag Res 10:465–472. https://doi.org/10.2147/CMAR.S157823
Ylagan LR, Dehner LP, Huettner PC, Lu D (2004) Columnar cell variant of papillary thyroid carcinoma. Report of a case with cytologic findings. Acta Cytol 48:73–77. https://doi.org/10.1159/000326287
Rottuntikarn W, Wangsiricharoen S, Rangdaeng S (2017) Cytomorphology and immunocytochemistry of columnar cell variant of papillary thyroid carcinoma. Cytopathology 28:338–341
Cho J, Shin JH, Hahn SY, Oh YL (2018) Columnar cell variant of papillary thyroid carcinoma: ultrasonographic and clinical differentiation between the indolent and aggressive types. Korean J Radiol 19:1000–1005. https://doi.org/10.3348/kjr.2018.19.5.1000
Verma R, Paul P (2016) Columnar cell variant of papillary thyroid carcinoma: a diagnostic dilemma in fine-needle aspiration cytology. Diagn Cytopathol 44:816–819. https://doi.org/10.1002/dc.23517
Jayaram G (2000) Cytology of columnar-cell variant of papillary thyroid carcinoma. Diagn Cytopathol 22:227–229. https://doi.org/10.1002/(SICI)1097-0339(200004)22:4%3c227::AID-DC5%3e3.0.CO;2-4
Kini H, Pai RR, Kalpana S (2003) Solitary parotid metastasis from columnar cell carcinoma of the thyroid: a diagnostic dilemma. Diagn Cytopathol 28:72–75. https://doi.org/10.1002/dc.10226
Gaertner EM, Davidson M, Wenig BM (1995) The columnar cell variant of thyroid papillary carcinoma. Case report and discussion of an unusually aggressive thyroid papillary carcinoma. Am J Surg Pathol 19:940–947. https://doi.org/10.1097/00000478-199508000-00010
Wenig BM, Thompson LDR, Adair CF et al (1998) Thyroid papillary carcinoma of columnar cell type: a clinicopathologic study of 16 cases. Cancer 82:740–753. https://doi.org/10.1002/(SICI)1097-0142(19980215)82:4%3c740::AID-CNCR18%3e3.0.CO;2-Y
Enriquez ML, Baloch ZW, Montone KT et al (2012) CDX2 expression in columnar cell variant of papillary thyroid carcinoma. Am J Clin Pathol 137:722–726. https://doi.org/10.1309/AJCPXE3PUBWVZCGZ
Bongiovanni M, Mermod M, Canberk S et al (2017) Columnar cell variant of papillary thyroid carcinoma: cytomorphological characteristics of 11 cases with histological correlation and literature review. Cancer Cytopathol 125:389–397. https://doi.org/10.1002/cncy.21860
Garcia-Rendueles MER, Ricarte-Filho JC, Untch BR et al (2015) NF2 loss promotes oncogenic RAS-induced thyroid cancers via YAP-dependent transactivation of RAS proteins and sensitizes them to MEK inhibition. Cancer Discov 5:1178–1193. https://doi.org/10.1158/2159-8290.CD-15-0330
Guenter R, Patel Z, Chen H (2021) Notch signaling in thyroid cancer. Adv Exp Med Biol 1287:155–168. https://doi.org/10.1007/978-3-030-55031-8_10
Cracolici V, Cipriani NA (2023) High-grade non-anaplastic thyroid carcinomas of follicular cell origin: a review of poorly differentiated and high-grade differentiated carcinomas. Endocr Pathol 34:34–47
Zeng PYF, Prokopec SD, Lai SY et al (2024) The genomic and evolutionary landscapes of anaplastic thyroid carcinoma. Cell Rep 43:113826. https://doi.org/10.1016/j.celrep.2024.113826
Xu B, David J, Dogan S et al (2022) Primary high-grade non-anaplastic thyroid carcinoma: a retrospective study of 364 cases. Histopathology 80:322–337. https://doi.org/10.1111/his.14550
Cracolici V, Ritterhouse LL, Segal JP et al (2020) Follicular thyroid neoplasms: comparison of clinicopathologic and molecular features of atypical adenomas and follicular thyroid carcinomas. Am J Surg Pathol. https://doi.org/10.1097/PAS.0000000000001489
Boyraz B, Sadow PM, Asa SL et al (2021) Cribriform-morular thyroid carcinoma is a distinct thyroid malignancy of uncertain cytogenesis. Endocr Pathol 32:327–335. https://doi.org/10.1007/s12022-021-09683-0
Nikiforov YE, Seethala RR, Tallini G et al (2016) Nomenclature revision for encapsulated follicular variant of papillary thyroid carcinoma a paradigm shift to reduce overtreatment of indolent tumors. JAMA Oncol 2:1023–1029. https://doi.org/10.1001/jamaoncol.2016.0386
Nikiforov YE, Baloch ZW, Hodak SP et al (2018) Change in diagnostic criteria for noninvasive follicular thyroid neoplasm with papillarylike nuclear features. JAMA Oncol 4:1125–1126
Chu Y-H, Sadow PM (2022) Kinase fusion-related thyroid carcinomas: towards predictive models for advanced actionable diagnostics. Endocr Pathol 33:421–435. https://doi.org/10.1007/s12022-022-09739-9
Chu Y-H, Sadow PM (2021) Kinase fusion-related thyroid carcinomas: distinct pathologic entities with evolving diagnostic implications. Diagn Histopathol (Oxf) 27:252–262. https://doi.org/10.1016/j.mpdhp.2021.03.003
Funding
This study was not supported by any funding.
Author information
Authors and Affiliations
Contributions
KEH and NAC wrote the main manuscript text and tables. NAC prepared figures. PMS, DNJ, PW, and PW contributed data and manuscript revision. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
Peter M. Sadow is co-editor of the journal and Nicole A. Cipriani is an officer of the North American Society of Head and Neck Pathology, a sponsor of the journal and an ad hoc editorial board member.
Ethical Approval
IRB approval from Northwestern, UChicago, and MGH have been obtained. For this type of study, formal consent is not required.
Informed Consent
For this type of study, informed consent is not required.
Consent for Publication
For this type of study, consent for publication is not required. No statistical analysis was performed in the preparation of this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Higgins, K.E., Sadow, P.M., Johnson, D.N. et al. Columnar Cell Thyroid Carcinoma: A Heterogeneous Entity Demonstrating Overlap Between Papillary Thyroid Carcinoma and Follicular Neoplasms. Head and Neck Pathol 18, 39 (2024). https://doi.org/10.1007/s12105-024-01645-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12105-024-01645-2