Abstract
Background
Ectomesenchymomas (EMs) are extremely rare neoplasms composed of malignant mesenchymal components and neuroectodermal derivatives. They are described in a wide variety of locations, with the head and neck region being one of the most frequently involved areas. EMs are usually managed as high-risk rhabdomyosarcomas and have similar outcomes.
Methods
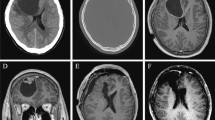
We present the case of a 15-year-old female with an EM that arose in the parapharyngeal space and extended into the intracranial space.
Results
Histologically, the tumor presented an embryonal rhabdomyosarcomatous mesenchymal component and the neuroectodermal component was constituted by isolated ganglion cells. Next-generation sequencing (NGS) revealed a p.Leu122Arg (c.365 T > G) mutation in the MYOD1 gene, a p.Ala34Gly mutation in the CDKN2A gene, and CDK4 gene amplification. The patient was treated with chemotherapy. She died 17 months after the debut of symptoms.
Conclusion(s)
To our knowledge, this is the first reported case in English literature of an EM with this MYOD1 mutation. We suggest combining PI3K/ATK pathway inhibitors in these cases. NGS should be performed in EMs cases to detect mutations with potential treatment options.



Similar content being viewed by others
Data Availability
Data will be available upon request from the authors.
References
Boué DR, Parham DM, Webber B et al (2000) Clinicopathologic study of ectomesenchymomas from intergroup rhabdomyosarcoma study groups III and IV. Pediatr Dev Pathol 3(3):290–300. https://doi.org/10.1007/s100249910039
Holimon JL, Rosenblum WI (1971) “Gangliorhabdomyosarcoma”: a tumor of ectomesenchyme: case report. J Neurosurg 34(3):417–422. https://doi.org/10.3171/jns.1971.34.3.0417
Nael A, Siaghani P, Wu WW, Nael K, Shane L, Romansky SG (2014) Metastatic malignant ectomesenchymoma initially presenting as a pelvic mass: report of a case and review of literature. Case Rep Pediatr 2014:1–9. https://doi.org/10.1155/2014/792925
Dantonello TM, Leuschner I, Vokuhl C et al (2013) Malignant ectomesenchymoma in children and adolescents: report from the cooperative weichteilsarkom studiengruppe (CWS): malignant pediatric ectomesenchymoma. Pediatr Blood Cancer 60(2):224–229. https://doi.org/10.1002/pbc.24174
Matsko TH, Schmidt RA, Milam AH, Orcutt JC (1992) Primary malignant ectomesenchymoma of the orbit. Br J Ophthalmol 76(7):438–441. https://doi.org/10.1136/bjo.76.7.438
Bittinger A, Rossberg C, Rodehüser M (1997) Primary malignant ectomesenchymoma of the orbit. Gen Diagn Pathol 142(3–4):221–225
Paikos P, Papathanassiou M, Stefanaki K, Fotopoulou M, Grigorios S, Tzortzatou F (2002) Malignant ectomesenchymoma of the orbit in a child. Surv Ophthalmol 47(4):368–374. https://doi.org/10.1016/S0039-6257(02)00313-2
Medina LS, Barnes PD, Donovan MJ, Taylor GA (1997) Radiologic-pathologic conference of children’s hospital boston: intraconal mass in the orbit of an infant. Pediatr Radiol 27(8):682–684. https://doi.org/10.1007/s002470050211
Patil CN, Cyriac S, Majhi U, Rajendranath R, Sagar TG (2011) Malignant ectomesenchymoma of the nasal cavity. Indian J Med Paediatr Oncol 32(04):242–243. https://doi.org/10.4103/0971-5851.95164
Cergnul M, La Rosa S, Bandera M et al (2007) Malignant ectomesenchymoma of the nasal cavity. Lancet Oncol 8(4):358–360. https://doi.org/10.1016/S1470-2045(07)70105-5
Brehmer D, Overhoff HM, Marx A (2003) Malignant ectomesenchymoma of the nose. ORL 65(1):52–56. https://doi.org/10.1159/000068666
Majhi U, Murhekar K, Sundersingh S, Krishnamurthy A (2012) Malignant ectomesenchymoma of paranasal sinuses with proptosis and nodal involvement. J Can Res Ther 8(3):465. https://doi.org/10.4103/0973-1482.103541
Vinck AS, Lerut B, Hermans R, Nuyts S, Sciot R, Jorissen M (2011) Malignant ectomesenchymoma of the paranasal sinuses with proptosis. B-ENT 7(3):201–204
Shuangshoti S, Chutchavaree A (1980) Parapharyngeal neoplasm of mixed mesenchymal and neuroepithelial origin. Arch Otolaryngol 106(6):361–364. https://doi.org/10.1001/archotol.1980.00790300049010
Kasantikul V, Shuangshoti S, Cutchavaree A, Bunyaphiphat P (1987) Parapharyngeal malignant ectomesenchymoma: combined malignant fibrous histiocytoma and primitive neuroectodermal tumour with neuroglial differentiation. J Laryngol Otol 101(5):508–515. https://doi.org/10.1017/s0022215100102105
Milano GM, Orbach D, Casanova M et al (2020) Malignant ectomesenchymoma in children: the European pediatric Soft tissue sarcoma study group experience. Pediatric Blood & Cancer. https://doi.org/10.1002/pbc.30116
VandenHeuvel KA, Carpentieri DF, Chen J, Fung KM, Parham DM (2014) Ectomesenchymoma with embryonal rhabdomyosarcoma and ganglioneuroma, arising in association with benign triton tumor of the tongue. Pediatr Dev Pathol 17(3):226–230. https://doi.org/10.2350/14-01-1433-CR.1
Karcioglu Z, Someren A, Mathes SJ (1977) Ectomesenchymoma: a malignant tumor of migratory neural crest (ectomesenchyme) remnants showing ganglionic, schwannian, melanocytic and rhabdomyoblastic differentiation. Cancer 39(6):2486–2496. https://doi.org/10.1002/1097-0142(197706)39
Schmidt D, Mackay B, Osborne BM, Jaffe N (1982) Recurring congenital lesion of the cheek. Ultrastruct Pathol 3(1):85–90. https://doi.org/10.3109/01913128209016628
Huang S, Antonescu C (2020) Ectomesenchymoma. In: WHO classification of tumours editorial board. Soft tissue and bone tumours, 5th edn. Agency for research on cancer pp 214–215
Cornejo P, Egelhoff J, Kaye R et al (2020) Malignant ectomesenchymoma of the scalp. Appl Radiol 49(3):40–42
Howley S, Stack D, Morris T et al (2012) Ectomesenchymoma with t(1;12)(p32;p13) evolving from embryonal rhabdomyosarcoma shows no rearrangement of ETV6. Hum Pathol 43(2):299–302. https://doi.org/10.1016/j.humpath.2011.03.010
Huang SC, Alaggio R, Sung YS et al (2016) Frequent HRAS mutations in malignant ectomesenchymoma: overlapping genetic abnormalities with embryonal rhabdomyosarcoma. Am J Surg Pathol 40(7):876–885. https://doi.org/10.1097/PAS.0000000000000612
Griffin BB, Chou PM, George D, Jennings LJ, Arva NC (2018) Malignant ectomesenchymoma: series analysis of a histologically and genetically heterogeneous tumor. Int J Surg Pathol 26(3):200–212. https://doi.org/10.1177/1066896917734915
Kleinschmidt-DeMasters BK, Lovell MA, Donson AM et al (2007) Molecular array analyses of 51 pediatric tumors shows overlap between malignant intracranial ectomesenchymoma and MPNST but not medulloblastoma or atypical teratoid rhabdoid tumor. Acta Neuropathol 113(6):695–703. https://doi.org/10.1007/s00401-007-0210-0
PDQ Pediatric Treatment Editorial Board. Childhood Soft Tissue Sarcoma Treatment (PDQ®): Health Professional Version. In: PDQ Cancer Information Summaries. National Cancer Institute (US); 2002. Accessed 5 Feb 2022. http://www.ncbi.nlm.nih.gov/books/NBK65923/
Bahrami A, Gown AM, Baird GS, Hicks MJ, Folpe AL (2008) Aberrant expression of epithelial and neuroendocrine markers in alveolar rhabdomyosarcoma: a potentially serious diagnostic pitfall. Mod Pathol 21(7):795–806. https://doi.org/10.1038/modpathol.2008.86
Apostolides PJ, Spetzler RF, Johnson PC (1995) Ectomesenchymal hamartoma (Benign “Ectomesenchymoma”) of the VIIIth nerve. Neurosurgery 37(6):1204–1207. https://doi.org/10.1227/00006123-199512000-00022
Kohsaka S, Shukla N, Ameur N et al (2014) A recurrent neomorphic mutation in MYOD1 defines a clinically aggressive subset of embryonal rhabdomyosarcoma associated with PI3K-AKT pathway mutations. Nat Genet 46(6):595–600. https://doi.org/10.1038/ng.2969
Rekhi B, Upadhyay P, Ramteke MP, Dutt A (2016) MYOD1 (L122R) mutations are associated with spindle cell and sclerosing rhabdomyosarcomas with aggressive clinical outcomes. Mod Pathol 29(12):1532–1540. https://doi.org/10.1038/modpathol.2016.144
Agaram NP, Chen CL, Zhang L, LaQuaglia MP, Wexler L, Antonescu CR (2014) Recurrent MYOD1 mutations in pediatric and adult sclerosing and spindle cell rhabdomyosarcomas: evidence for a common pathogenesis. Genes Chromosom Cancer 53(9):779–787. https://doi.org/10.1002/gcc.22187
Iolascon A, Faienza MF, Coppola B et al (1996) Analysis of cyclin-dependent kinase inhibitor genes (CDKN2A, CDKN2B, andCDKN2C) in childhood rhabdomyosarcoma. Genes Chromosom Cancer 15(4):217–222. https://doi.org/10.1002/(SICI)1098-2264(199604)15
Xia SJ, Pressey JG, Barr FG (2002) Molecular pathogenesis of rhabdomyosarcoma. Cancer Biol Ther 1(2):97–104. https://doi.org/10.4161/cbt.51
He Y, Sun MM, Zhang GG et al (2021) Targeting PI3K/Akt signal transduction for cancer therapy. Signal Transduct Target Ther 6(1):425. https://doi.org/10.1038/s41392-021-00828-5
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or non-profit sectors.
Author information
Authors and Affiliations
Contributions
Conception and design of the study and acquisition and analysis of data: P-BEM and P-KJJ. Drafting the manuscript: P-BEM, P-LDSD, UC, P-KJJ, SA, RP, EA, M-SM, and P-MA. Radiology images: UC. Pathology figures: P-BEM and P-KJJ. Molecular studies: M-SM.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical Approval
Not applicable.
Consent for Publication
Consent for publication was obtained from the family.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pena-Burgos, E.M., De Sabando, D.PL., Utrilla, C. et al. First Reported Case of Malignant Ectomesenchymoma with p.Leu122Arg Mutation in MYOD1 Gene: Extensive Intra- and Extracranial Tumor in a 15-Year-Old Female. Head and Neck Pathol 17, 855–863 (2023). https://doi.org/10.1007/s12105-023-01542-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-023-01542-0