Abstract
Objectives
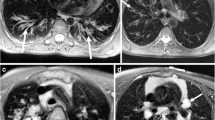
To compare and evaluate the usefulness of magnetic resonance imaging (MRI) with computed tomography (CT) in bronchiectasis; to compare MRI and CT scores with pulmonary function tests (PFT) and to evaluate the role of Diffusion-weighted imaging (DWI) in bronchiectasis.
Methods
In this prospective study, 25 patients between 7–21 y of age with a clinical/radiological diagnosis of bronchiectasis underwent MDCT and MRI chest. MRI and CT scoring was performed using modified Bhalla-Helbich’s score by two independent radiologists for all parameters. A final consensus score was recorded. The overall image quality of different MRI sequences to identify pathologies was also assessed. Appropriate statistical tests were used for inter-observer agreements, and correlation amongst CT and MRI; as well as CT, MRI and PFT.
Results
Strong agreement (ICC 0.80–0.95) between CT and MRI was seen for extent and severity of bronchiectasis, number of bullae, sacculation/abscess, emphysema, collapse/ consolidation, mucus plugging, and mosaic perfusion. Overall CT and MRI scores had perfect concordance (ICC 0.978). Statistically significant (p-value <0.01) intra-observer and inter-observer agreement for all CT and MRI score parameters were seen. A strong negative correlation was seen between total CT and MRI severity scores and forced expiratory volume in 1 s (FEV1), forced vital capacity (FVC), forced expiratory flow (FEF) 25–75%. DWI MR, with an apparent diffusion coefficient (ADC) cut-off of 1.62 × 10–3 mm3/s had a sensitivity of 70% and specificity of 75% in detecting true mucus plugs.
Conclusions
MRI with DWI can be considered as a radiation-free alternative in the diagnostic algorithm for assessment of lung changes in bronchiectasis, especially in follow-up.


Similar content being viewed by others
References
Causes of Bronchiectasis in Children - UpToDate [Internet]. 2019. Available at: https://www.uptodate.com/contents/causes-of-bronchiectasis-in-children?search=bronchiectasis&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1#H4. Accessed on 28 Mar 2019.
Singh A, Bhalla AS, Jana M. Bronchiectasis revisited: Imaging-based pattern approach to diagnosis. Curr Probl Diagn Radiol. 2019;48:53–60.
Endpoints for Clinical Trials in Young Children with Cystic Fibrosis. 2019. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2647606/. Accessed on 30 Apr 2019.
Computed Tomography Reflects Lower Airway Inflammation and Tracks Changes in Early Cystic Fibrosis. 2019. Available at: https://www.ncbi.nlm.nih.gov/pubmed/17303797. Accessed on 30 Apr 2019.
de Jong PA, Mayo JR, Golmohammadi K, et al. Estimation of cancer mortality associated with repetitive computed tomography scanning. Am J Respir Crit Care Med. 2006;173:199–203.
Loeve M, Lequin MH, de Bruijne M, et al. Cystic fibrosis: Are volumetric ultra-low-dose expiratory CT scans sufficient for monitoring related lung disease? Radiology. 2009;253:223–9.
Pearce MS, Salotti JA, Little MP, et al. Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: A retrospective cohort study. Lancet. 2012;380:499–505.
Eichinger M, Optazaite DE, Kopp-Schneider A, et al. Morphologic and functional scoring of cystic fibrosis lung disease using MRI. Eur J Radiol. 2012;81:1321–9.
Puderbach M, Eichinger M, Haeselbarth J, et al. Assessment of morphological MRI for pulmonary changes in cystic fibrosis (CF) patients: Comparison to thin-section CT and chest x-ray. Invest Radiol. 2007;42:715–25.
Helbich TH, Heinz-Peer G, Eichler I, et al. Cystic fibrosis: CT assessment of lung involvement in children and adults. Radiology. 1999;213:537–44.
Bhalla M, Turcios N, Aponte V, et al. Cystic fibrosis: Scoring system with thin-section CT. Radiology. 1991;179:783–8.
Sileo C, Corvol H, Boelle P-Y, Blondiaux E, Clement A, Le Pointe HD. HRCT and MRI of the lung in children with cystic fibrosis: Comparison of different scoring systems. J Cyst Fibros. 2014;13:198–204.
Renz DM, Scholz O, Böttcher J, et al. Comparison between magnetic resonance imaging and computed tomography of the lung in patients with cystic fibrosis with regard to clinical, laboratory, and pulmonary functional parameters. Invest Radiol. 2015;50:733–42.
Montella S, Santamaria F, Salvatore M, et al. Assessment of chest high-field magnetic resonance imaging in children and young adults with noncystic fibrosis chronic lung disease: Comparison to high-resolution computed tomography and correlation with pulmonary function. Invest Radiol. 2009;44:532–8.
Ma W, Sheikh K, Svenningsen S, et al. Ultra-short echo-time pulmonary MRI: Evaluation and reproducibility in COPD subjects with and without bronchiectasis. J Magn Reson Imaging. 2015;41:1465–74.
Dournes G, Grodzki D, Macey J, et al. Quiet submillimeter MR imaging of the lung is feasible with a PETRA sequence at 1.5 T. Radiology. 2015;276:258–65.
Ciet P, Serra G, Andrinopoulou ER, et al. Diffusion weighted imaging in cystic fibrosis disease: Beyond morphological imaging. Eur Radiol. 2016;26:3830–9.
Bauman G, Puderbach M, Heimann T, et al. Validation of Fourier decomposition MRI with dynamic contrast-enhanced MRI using visual and automated scoring of pulmonary perfusion in young cystic fibrosis patients. Eur J Radiol. 2013;82:2371–7.
Stahl M, Steinke E, Graeber SY, et al. Magnetic resonance imaging detects progression of lung disease and impact of newborn screening in preschool children with cystic fibrosis. Am J Respir Crit Care Med. 2021;204:943–53.
Murphy KP, Maher MM, O’Connor OJ. Imaging of cystic fibrosis and pediatric bronchiectasis. Am J Roentgenol. 2016;206:448–54.
Sodhi KS, Sharma M, Lee EY, et al. Diagnostic utility of 3T lung MRI in children with interstitial lung disease: A prospective pilot study. Acad Radiol. 2018;25:380–6.
Sodhi KS, Sharma M, Saxena AK, Mathew JL, Singh M, Khandelwal N. MRI in thoracic tuberculosis of children. Indian J Pediatr. 2017;84:670–6.
Kapur S, Jana M, Gupta L, Bhalla AS, Naranje P, Gupta AK. Chest MRI using multivane-XD, a novel T2-weighted free breathing MR sequence. Curr Probl Diagn Radiol. 2021;50:41–7.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15:155–63.
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1:307–10.
Ciet P, Serra G, Bertolo S, et al. Assessment of CF lung disease using motion corrected PROPELLER MRI: A comparison with CT. Eur Radiol. 2016;26:780–7.
Sodhi KS, Khandelwal N, Saxena AK, et al. Rapid lung MRI in children with pulmonary infections: Time to change our diagnostic algorithms: Rapid lung MRI in children. J Magn Reson Imaging. 2016;43:1196–206.
Teufel M, Ketelsen D, Fleischer S, et al. Comparison between high-resolution CT and MRI using a very short echo time in patients with cystic fibrosis with extra focus on mosaic attenuation. Respiration. 2013;86:302–11.
Milito C, Pulvirenti F, Serra G, et al. Lung magnetic resonance imaging with diffusion weighted imaging provides regional structural as well as functional information without radiation exposure in primary antibody deficiencies. J Clin Immunol. 2015;35:491–500.
Author information
Authors and Affiliations
Contributions
L: Literature search, manuscript preparation and editing and data curation; MJ: Conceptualization, manuscript editing and contribution to figures; PN, ASB: Manuscript editing and contribution to figures; SKK, VH, AKG: Manuscript editing and review. MJ will act as guarantor for this manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lokesh, Jana, M., Naranje, P. et al. MDCT and MRI in Bronchiectasis in Older Children and Young Adults – A Non-Inferiority Trial. Indian J Pediatr (2023). https://doi.org/10.1007/s12098-023-04921-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12098-023-04921-1