Abstract
India is committed to achieve a single-digit neonatal mortality rate (NMR) and stillbirth rate (SBR) by 2030 through India Newborn Action Plan (INAP) 2014. However, the current rate of decline is not enough to achieve the target neonatal mortality rate. Course correction and renewed efforts are required. This review outlines the current scenario and proposed scale-up of services included during labour, childbirth, and the immediate newborn period. The article summarises the challenges and bottlenecks in achieving a reduction in neonatal mortality rate and INAP targets. India has achieved over 80% coverage of three of the four ENAP coverage targets, but antenatal care coverage is still poor. There are concerns about the quality and completeness of antenatal care visits and other program interventions. The ongoing quality assurance should be strengthened through continuous supportive supervision by involving the medical colleges in a hub and spoke model and other key stakeholders. There is a need for effective and strategic engagement of the private sector in these initiatives. The states need to systematically assess the gaps as per population requirements and find effective solutions to overcome them quickly. The state and district-wise data maps show immense variations in coverage between states and within states, mirroring the variations in NMR. This indicates the need to ensure contextual micro-plans and provides an opportunity for the districts and states to learn from each other. The recent initiatives to strengthen primary healthcare should be used as a platform for all stillbirth and neonatal mortality prevention interventions in India.



Similar content being viewed by others
References
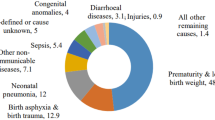
Lahariya C, Paul VK. Burden, differentials, and causes of child deaths in India. Indian J Pediatr. 2010;77:1312–21.
Lahariya C, Sudfeld CR, Tomar SS. Causes of child deaths in India, 1985–2008: A systematic review of literature. Indian J Pediatr. 2010;77:1303–11.
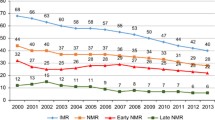
Collaborators I-L. Subnational mapping of under-5 and neonatal mortality trends in India: The Global Burden of Disease Study 2000–17. Lancet. 2020;395:1640–58.
Dhaded SM, Saleem S, Goudar SS, et al. The causes of preterm neonatal deaths in India and Pakistan (PURPOSe): A prospective cohort study. Lancet Glob Health. 2022;10:e1575–81.
Lozano R, Naghavi M, Foreman K, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:2095–128.
India Newborn Action Plan (INAP). National Health Mission. Available at: https://nhm.gov.in/images/pdf/programmes/inap-final.pdf. Accessed on 22 Jan 2023.
Ending Preventable Newborn Deaths and Stillbirths by 2030. WHO and UNICEF September 2020. Available at: https://data.unicef.org/resources/resource-type/publications/. Accessed on 23 May 2023.
Tyagi M, Hanson C, Schellenberg J, Chamarty S, Singh S. Hand hygiene in hospitals: An observational study in hospitals from two southern states of India. BMC Public Health. 2018;18:1299.
WASH in Health Care Facilities. Available at: https://www.unicef.org/india/what-we-do/wash-facilities. Accessed on 21 Oct 2022.
Chawanpaiboon S, Vogel JP, Moller A-B, et al. Global, regional, and national estimates of levels of preterm birth in 2014: A systematic review and modelling analysis. Lancet Glob Health. 2019;7:e37–46.
WHO ACTION Trials Collaborators; Oladapo OT, Vogel JP, Piaggio G, et al. Antenatal Dexamethasone for early preterm birth in low-resource countries. N Engl J Med. 2020;383:2514–25.
Kankaria A, Duggal M, Chauhan A, et al. Readiness to provide antenatal corticosteroids for threatened preterm birth in public health facilities in northern India. Glob Health Sci Pract. 2021;9:575–89.
Menon R, Richardson LS. Preterm prelabor rupture of the membranes: A disease of the fetal membranes. Semin Perinatol. 2017;41:409–19.
Kenyon S, Boulvain M, Neilson JP. Antibiotics for preterm rupture of membranes. Cochrane Database Syst Rev. 2010;8:CD001058.
National Rural Health Mission. Ministry of Health & Family Welfare GoI. Skilled Birth Attendance (SBA) Trainer's Guide for conducting Training of Auxillary Nurse Midwives, Lady Health Visitors & Staff Nurses. Available at: http://tripuranrhm.gov.in/Guidlines/Staff_Nurses2.pdf. Accessed on 22 Jan 2023.
Rural Health Statistics 2020–21. Ministry of Health and Family Welfare. GOI. Available at: https://main.mohfw.gov.in/newshighlights-90. Accessed on 29 Apr 2023.
Training Status Report 2019–20. Mission Directorate NHM, Department of Health & Family Welfare, Govt. of Odisha. Available at: http://www.nrhmorissa.gov.in/writereaddata/Upload/Documents/Training%20Status%20Report%20.pdf. Accessed on 20 Mar 2023.
Dalal AR, Purandare AC. The partograph in childbirth: An absolute essentiality or a mere exercise? J Obstet Gynaecol India. 2018;68:3–14.
Palo SK, Patel K, Singh S, Priyadarshini S, Pati S. Intrapartum monitoring using partograph at secondary level public health facilities-A cross-sectional study in Odisha. India J Fam Med Prim Care. 2019;8:2685–90.
Sharma B, Lahariya C, Majella MG, et al. Burden, differentials and causes of stillbirths in India: A systematic review & meta analysis. Indian J Pediatr. 2023;in press.
Agarwal N, Lahariya C, Sharma B, et al. Stillbirth in India: Current status, challenges, and the way forward. Indian J Pediatr. 2023;in press.
Sharma B, Raina A, Kumar V, Mohanty P, Sharma M, Gupta A. Counting stillbirth in a community - To understand the burden. Clin Epidemiol Glob Health. 2022;14:100977.
Darmstadt GL, Bhutta ZA, Cousens S, Adam T, Walker N, de Bernis L. Evidence-based, cost-effective interventions: how many newborn babies can we save? Lancet. 2005;365:977–88.
Ministry of Health and Family Welfare. Annual Report 2020–21. Available at: https://main.mohfw.gov.in/sites/default/files/Annual%20Report%202020-21%20English.pdf. Accessed on 29 Apr 2023.
Jasani B, Torgalkar R, Ye XY, Syed S, Shah PS. Association of umbilical cord management strategies with outcomes of preterm infants: A systematic review and network meta-analysis. JAMA Pediatr. 2021;175:e210102.
American College of Obstetricians and Gynecologists' Committee on Obstetric Practice. Delayed umbilical cord clamping after birth: ACOG Committee Opinion, Number 814. Obstet Gynecol. 2020;136:e100–6.
Chowdhury A, Neogi SB, Prakash V, et al. Implementation of delayed cord clamping in public health facilities: A case study from India. BMC Pregnancy Childbirth. 2022;22:457.
Lunze K, Bloom DE, Jamison DT, Hamer DH. The global burden of neonatal hypothermia: Systematic review of a major challenge for newborn survival. BMC Med. 2013;11:24.
Muhe LM, McClure EM, Nigussie AK, et al. Major causes of death in preterm infants in selected hospitals in Ethiopia (SIP): A prospective, cross-sectional, observational study. Lancet Glob Health. 2019;7:e1130–8.
Abiramalatha T, Ramaswamy VV, Bandyopadhyay T, et al. Delivery room interventions for hypothermia in preterm neonates: A systematic review and network meta-analysis. JAMA Pediatr. 2021;175:e210775.
WHO Immediate KMC Study Group, Arya S, Naburi H, Kawaza K, et al. Immediate "Kangaroo Mother Care" and survival of infants with low birth weight. N Engl J Med. 2021;384:2028–38.
Victora CG, Bahl R, Barros AJD, et al. Breastfeeding in the 21st century: Epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387:475–90.
Rollins NC, Bhandari N, Hajeebhoy N, et al. Why invest, and what it will take to improve breastfeeding practices? Lancet. 2016;387:491–504.
Dandona R, Kumar GA, Bhattacharya D, et al. Distinct mortality patterns at 0–2 days versus the remaining neonatal period: Results from population-based assessment in the Indian state of Bihar. BMC Med. 2019;17:140.
Mundargi K, Hiregoudar V. Awareness about government maternal benefit schemes among pregnant women attending Anganawadi centres in North Karnataka. Int J Commun Med Public Health. 2021;8:4801–5.
Lahariya C, Roy B, Shukla A, et al. Community action for health in India: Evolution, lessons learnt and ways forward to achieve universal health coverage. WHO South East Asia J Public Health. 2020;9:82–91.
Lahariya C. “Ayushman Bharat” program and universal health coverage in India. Indian Pediatr. 2018;55:495–506.
Lahariya C, Khanna R, Nandan D, et al. Primary health care and child survival in India. Indian J Pediatr. 2010;77:283–90.
Lahariya C. Health & wellness centers to strengthen primary health care in India: Concept, progress and ways forward. Indian J Pediatr. 2020;87:916–29.
Acknowledgements
The authors would like to thank Dr. Chandrakant Lahariya, Dr. Rodney P Vaz, and other technical staff at the Integrated Department of Health Policy, Epidemiology, Pediatrics and Preventive Medicine at the Foundation for People-centric Health Systems for reviewing and providing input on the earlier version of this manuscript.
Author information
Authors and Affiliations
Contributions
PK conceived the idea and outline, and critically reviewed, revised and finalized the manuscript; JK and SSS wrote parts of the initial draft and revised as per feedback. PK will act as the guarantor for this manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kumar, J., Saini, S.S. & Kumar, P. Care During Labour, Childbirth, and Immediate Newborn Care in India: A Review. Indian J Pediatr 90 (Suppl 1), 20–28 (2023). https://doi.org/10.1007/s12098-023-04721-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-023-04721-7