Abstract
Objective
To compare hypoglycemia and the other early neonatal morbidities (from birth till hospital discharge) of late preterm babies born small for gestational age (LP SGA) with their appropriate for age (LP AGA) counterparts.
Methods
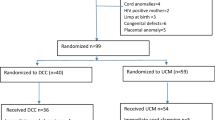
LP SGA and LP AGA, as defined by Fenton charts, were prospectively followed-up to assess development of predefined morbidities, mortality and readmission rates at one month. All live inborn late preterm babies (340/7 to 366/7 weeks, n = 238) were included.
Results
LP SGA babies (n = 72) as compared to LP AGA babies (n = 166) were at higher risk for developing at least one predefined neonatal morbidity before hospital discharge [RR 1.93 (1.6–2.3; p < 0.001)]. These included hypoglycemia, hypothermia, respiratory morbidity needing support, jaundice needing treatment, feeding difficulties, birth asphyxia, and sepsis; besides, significant rates of readmissions and duration of hospital stay.
Conclusions
Being born small for gestation age acts an additional jeopardizing factor in late preterm babies.


Similar content being viewed by others
References
Katz J, Lee AC, Kozuki N, et al; the CHERG Small-for-Gestational-Age-Preterm Birth Working Group. Mortality risk in preterm and small-for-gestational-age babies in low-income and middle-income countries: a pooled country analysis. Lancet. 2013;382:417–25.
Lee ACC, Katz J, Blencowe H, et al. National and regional estimates of term and preterm babies born small for gestational age in 138 low-income and middle-income countries in 2010. Lancet Glob Health. 2013;1:e26–36.
Natarajan G, Shankaran S. Short- and long-term outcomes of moderate and late preterm babies. Am J Perinatol. 2016;33:305–17.
Pulver LS, Guest-Warnick G, Stoddard GJ, Byington CL, Young PC. Weight for gestational age affects the mortality of late preterm babies. Pediatrics. 2009;123:e1072–7.
Rocha CO, Bittar RE, Zugaib M. Neonatal outcomes of late-preterm birth associated or not with intrauterine growth restriction. Obstet Gynecol Int. 2010;article ID 231842, 5 pages, https://doi.org/10.1155/2010/231842.
Boyle EM, Johnson S, Manktelow B, et al. Neonatal outcomes and delivery of care for babies born late preterm or moderately preterm: a prospective population-based study. Arch Dis Child Fetal Neonatal Ed. 2015;100:F479–85.
Tomashek KM, Shapiro-Mendoza CK, Weiss J, et al. Early discharge among late preterm and term newborns and risk of neonatal morbidity. Semin Perinatol. 2006;30:61–8.
Venkatnarayan K, Sankar J, Krishnan A, Deorari AK, Paul VK. A micro-costing model of neonatal intensive care from a tertiary Indian unit: feasibility and implications for insurance. Indian Pediatr. 2014;51:215–7.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm babies. BMC Pediatr. 2013;13:59.
Agarwal R, Deorari A, Paul VK. AIIMS protocol in neonatology. New Delhi: CBS Publishers; 2014.
National Neonatology Forum, India (NNFI). Evidence Based Clinical Practice Guidelines. October 2010. Available at: www.nnfi.org/index.php?option=com_content&view=article&id=6&Itemid. Accessed 25 Jan 2019.
Bertino E, Occhi L, Di Nicola P. The late preterm IUGR and/or SGA. Ital J Pediatr. 2014;40:A3.
Thureen PJ, Anderson MS, Hay WW. The small-for-gestational-age infant. NeoRev. 2001;2:e139–49.
Regev RH, Reichman B. Prematurity and intrauterine growth retardation—double jeopardy? Clin Perinatol. 2004;31:453–73.
Grisaru-Granovsky S, Reichman B, Lerner-Geva L, et al. Mortality and morbidity in preterm small-for-gestational-age babies: a population-based study. Am J Obstet Gynecol. 2012;206:150–e1–7.
Jaiswal A, Murki S, Gaddam P, Reddy A. Early neonatal morbidities in late preterm babies. Indian Pediatr. 2011;48:607–11.
Bhutta ZA, Das JK. Bahl R, et al; Lancet Newborn Interventions Review Group; Lancet Every Newborn Study Group. Can available interventions end preventable deaths in mothers, newborn babies, and stillbirths, and at what cost? Lancet. 2014;384:347–70.
Gupta P, Mital R, Kumar B, Yadav A, Jain M, Upadhyay A. Physical growth, morbidity profile and mortality among healthy late preterm neonates. Indian Pediatr. 2017;54:629–34.
Acknowledgements
The authors acknowledge support of the patients and their parents who consented to the study and agreed for follow up. They also acknowledge help of the NICU and postnatal ward staffs for helping in patient care and giving inputs, their fellow residents for their continuous support and motivation, the hospital IT dept. for statistical help and tracking patient details, their family for their unconditional support and Mr. Ranganadham Srinadh for statistical analysis of logistic regression.
Author information
Authors and Affiliations
Contributions
KV designed the study, made protocol and drafted the final manuscript. AKM collected the data and did the preliminary analysis. RKT, VVT and SCS analyzed the data and contributed in the finalization of the manuscript. KV is the guarantor for this article.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(DOCX 22 kb)
Rights and permissions
About this article
Cite this article
Mallick, A.K., Venkatnarayan, K., Thapar, R.K. et al. Morbidity Patterns of Late Preterm Babies Born Small for Gestation. Indian J Pediatr 86, 578–583 (2019). https://doi.org/10.1007/s12098-019-02925-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-019-02925-4