Abstract
Objective
To study the clinical profile of dengue fever and its outcome in children with application of revised WHO classification and to identify risk factors for severe dengue.
Methods
This study was a prospective observational study of children diagnosed with dengue from July 2012 through February 2013 at a tertiary care hospital in Bangalore, Karnataka (South India).
Results
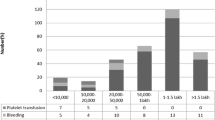
Eighty one children including 55(67.9 %) boys and 26(32.1 %) girls were diagnosed with dengue. Mean age of presentation was 8 y. Vomiting (60.5 %), pain abdomen (32 %), headache (30.9 %), myalgia (23.5 %) and bleeding manifestations (16 %) were the common presenting complaints. Facial puffiness (63 %), hepatomegaly (51.9 %), ascites (48.1 %), pleural effusion (39.5 %) and petechiae (14.8 %) were noted during examination. Dengue NS1 antigen, IgM, IgG were positive in 66.7 %, 29.6 % and 18.5 % of cases respectively.
Investigations showed hemoconcentration in 72.8 %, leucopenia (34.5 %), thrombocytopenia (82.7 %), abnormal liver function test (LFT) (33.3 %). USG abdomen was suggestive of dengue in 66.7 % and gall bladder edema was noted in 53.1 %. Two patients died out of the total 81 patients with mortality rate of 2.5 %. Number of cases classified as Dengue without warning signs (D), Dengue with warning signs (DW) and Severe Dengue (SD) were 48.1 %, 27.2 % and 24.7 % respectively.
Conclusions
Children between 5 and 15 y were most affected by dengue fever. Pain abdomen and vomiting were most common presenting symptoms. Ascites, plerural effusion, hepatomegaly, gall bladder wall thickening and abnormal LFT were found significantly high in severe dengue cases.

Similar content being viewed by others
References
Dengue: Guidelines for diagnosis, treatment, prevention and control. World Health Organization. Geneva, Switzerland: WHO; 2009.
Division of Vector Borne Infectious Disease. Dengue fever. Atlanta, Ga: Centers for Disease Control and Prevention; 2008.
Mittal H, Faridi MM, Arora SK, Patil R. Clinicohematological profile and platelet trends in children with dengue during 2010 epidemic in north India. Indian J Pediatr. 2012;79:467–71.
Kulkarni MJ, Sarathi V, Bhalla V, Shivpuri D, Acharya U. Clinico-epidemiological profile of children hospitalized with dengue. Indian J Pediatr. 2010;77:1103–7.
Anders KL, Nguyet NM, Chau NVV, Hung NT, Thuy TT, Lien le B, et al. Epidemiological factors associated with dengue shock syndrome and mortality in hospitalized dengue patients in Ho Chi Minh city, Vietnam. Am J Trop Med Hyg. 2011;84:127–34.
Wang CC, Lee IK, Su MC, Lin HI, Huang YC, Liu SF, et al. Differences in clinical and laboratory characterstics and disease severity between children and adults with dengue viral infection in Taiwan, 2002. Trans R Soc Trop Med Hyg. 2009;103:871–7.
Ahmed S, Arif F, Yahya Y, Rehman A, Abbas K, Ashraf S, et al. Dengue fever outbreak in Karachi 2006-a study of profile and outcome of children under 15 years of age. J Pak Med Assoc. 2008;58:4–8.
Soares CN, Cabral-Castro MJ, Peralta JM, de Freitus MR, Zalis M, Puccioni-Sohler M. Review of etiologies of viral meningitis and encephalitis in a dengue endemic region. J Neurol Sci. 2011;303:75–9.
Jackson ST, Mullings A, Bennett F, Khan C, Gordon-Strachan G, Rhoden T. Dengue infection in patients presenting with neurological manifestations in a dengue endemic population. West Indian Med J. 2008;57:373–6.
Gupta V, Yadav TP, Pandey RM, Singh A, Gupta M, Kanaujiya P, et al. Risk factors of dengue shock syndrome in children. J Trop Pediatr. 2011;57:451–6.
Chacko B, Subramanian G. Clinical, laboratory and radiological parameters in children with dengue fever and predictive factors for dengue shock syndrome. J Trop Pediatr. 2008;54:137–40.
Joshi R, Baid V. Profile of dengue patients admitted to a teritiary care hospital in Mumbai. Turk J Pediatr. 2011;53:626–31.
Jagdishkumar K, Jain P, Manjunath VG, Umesh L. Hepatic involvement in dengue fever in children. Iran J Pediatr. 2012;22:231–6.
Colbert JA, Gordon A, Roxelin R, Silva S, Silva J, Rocha C, et al. Ultrasound measurement of gall bladder thickening as a diagnostic and prognostic indicator for severe dengue in pediatric patients. Pediatr Infect Dis J. 2007;26:850–2.
Chatterjee R, Mysore A, Ahya K, Shrikande D, Shedabale D. Utility of sonography in clinically suspected dengue. Pediatr Infect Dis. 2012;4:107–11.
Guzman MG, Jaenisch T, Gaczkowski R, Ty Hang VT, Sekaran SD, Kroeger A, et al. Multi-country evaluation of the festivity and specificity of 2 commercially available NS1 ELISA assays for dengue diagnosis. PLoS Negl Trop Dis. 2010;4:e811.
Arya SC, Agarwal N, Parikh SC, Agarwal S. Simultaneous detection of dengue NS1 antigen, IgM plus IgG and platelet enumeration during an outbreak. Sultan Qaboos Univ Med J. 2011;11:470–6.
Hadinegoro SR. The revised WHO dengue case classification: does the system need to be modified? Paediatr Int Child Health. 2012;32:33–8.
Prasad D, Kumar C, Jain A, Kumar R. Accuracy and applicability of revised WHO classification (2009) of dengue in children seen at a teritiary healthcare facility in northern India. Infection. 2013;41:775–82.
Narvez F, Gutierrez G, Perez MA, Elizendo D, Nuñez A, Balmaseda A, et al. Evaluation of the traditional and revised WHO classification of dengue disease severity. PLoS Negl Trop Dis. 2011;5:e1397.
Acknowledgments
The authors would like to thank Mr. Narasimha Murthy, Statistician, Sapthagiri Institute of Medical Sciences, Bangalore for his immense help in preparing the statistics of the study.
Contributions
KSS: Conceived the idea, designed the study, collected the data, entered data, did analysis, wrote first draft, approved the final manuscript and shall act as guarantor of the study; RS: Reviewed and edited the manuscript.
Conflict of Interest
None.
Source of Funding
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sahana, K.S., Sujatha, R. Clinical Profile of Dengue Among Children According to Revised WHO Classification: Analysis of a 2012 Outbreak from Southern India. Indian J Pediatr 82, 109–113 (2015). https://doi.org/10.1007/s12098-014-1523-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-014-1523-3