Abstract
Background
The classification and nomenclature of non-alcoholic fatty liver disease (NAFLD) has been the subject of ongoing debate in the medical community. Through the introduction of metabolic dysfunction-associated fatty liver disease (MAFLD) and the later release of metabolic dysfunction-associated steatotic liver disease (MASLD), the limitations associated with NAFLD are intended to be addressed. Both terminologies incorporate the metabolic component of the disease by providing diagnostic criteria that relies on the presence of underlying metabolic risk factors.
Materials and Methods
An epidemiologic cross-sectional study of individuals who had undergone abdominal ultrasound and vibration-controlled transient elastography (VCTE) as part of a routine check was performed. We evaluated clinical, anthropometric, and biochemical variables to determine the metabolic profile of each subject.
Results
The study included a total of 500 participants, 56.8% (n = 284) males and 43.2% (n = 216) females, with a mean age of 49 ± 10 years. 59.4% (n = 297) were diagnosed with MAFLD and MASLD, 10.2% (n = 51) were diagnosed only with MASLD and 30.4% (n = 152) were not diagnosed with either MAFLD or MASLD. The differences in prevalence were mainly based on the detection of individuals with a BMI < 25 kg/m2, where MASLD captures the largest number (p < 0.001).
Conclusions
Although MASLD has a higher capture of lean patients compared to MAFLD, patients with MAFLD and MASLD have a worse metabolic profile than those with only MASLD. Our results provide evidence that MAFLD better identifies patients likely to have a higher risk of liver fibrosis and of disease progression.
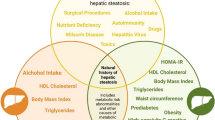
Graphical abstract



Similar content being viewed by others
Data availability
All data supporting the findings of this study are available within the paper.
References
Ramírez-Mejía MM, Qi X, Abenavoli L, Romero-Gómez M, Eslam M, Méndez-Sánchez N. Metabolic dysfunction: the silenced connection with fatty liver disease. Ann Hepatol. 2023;28(6):101138. https://doi.org/10.1016/j.aohep.2023.101138. (Epub 20230717; PubMed PMID: 37468095)
Chan KE, Koh TJL, Tang ASP, Quek J, Yong JN, Tay P, et al. Global prevalence and clinical characteristics of metabolic-associated fatty liver disease: a meta-analysis and systematic review of 10 739 607 individuals. J Clin Endocrinol Metab. 2022;107(9):2691–2700. https://doi.org/10.1210/clinem/dgac321. (PubMed PMID: 35587339)
Eslam M, Alkhouri N, Vajro P, Baumann U, Weiss R, Socha P, et al. Defining paediatric metabolic (dysfunction)-associated fatty liver disease: an international expert consensus statement. Lancet Gastroenterol Hepatol. 2021;6(10):864–873. https://doi.org/10.1016/s2468-1253(21)00183-7. (Epub 20210806 PubMed PMID: 34364544)
Eslam M, Newsome PN, Sarin SK, Anstee QM, Targher G, Romero-Gomez M, et al. A new definition for metabolic dysfunction-associated fatty liver disease: an international expert consensus statement. J Hepatol. 2020;73(1):202–209. https://doi.org/10.1016/j.jhep.2020.03.039. (Epub 20200408 PubMed PMID: 32278004)
Lim GEH, Tang A, Ng CH, Chin YH, Lim WH, Tan DJH, et al. An observational data meta-analysis on the differences in prevalence and risk factors between MAFLD vs NAFLD. Clin Gastroenterol Hepatol. 2023;21(3):619–29.e7. https://doi.org/10.1016/j.cgh.2021.11.038. (Epub 20211204 PubMed PMID: 34871813)
Yamamura S, Eslam M, Kawaguchi T, Tsutsumi T, Nakano D, Yoshinaga S, et al. MAFLD identifies patients with significant hepatic fibrosis better than NAFLD. Liver Int. 2020;40(12):3018–3030. https://doi.org/10.1111/liv.14675. (PubMed PMID: 32997882)
Méndez-Sánchez N, Bugianesi E, Gish RG, Lammert F, Tilg H, Nguyen MH, et al. Global multi-stakeholder endorsement of the MAFLD definition. Lancet Gastroenterol Hepatol. 2022;7(5):388–390. https://doi.org/10.1016/s2468-1253(22)00062-0. (Epub 20220303 PubMed PMID: 35248211)
Méndez-Sánchez N, Díaz-Orozco LE. Editorial: International consensus recommendations to replace the terminology of non-alcoholic fatty liver disease (NAFLD) with metabolic-associated fatty liver disease (MAFLD). Med Sci Monit. 2021;27:e933860. https://doi.org/10.12659/msm.933860. (Epub 20210712, PubMed PMID: 34248137; PubMed Central PMCID: PMC8284081)
Fouad Y, Elwakil R, Elsahhar M, Said E, Bazeed S, Ali Gomaa A, et al. The NAFLD-MAFLD debate: eminence vs evidence. Liver Int. 2021;41(2):255–260. https://doi.org/10.1111/liv.14739. (Epub 20201202 PubMed PMID: 33220154)
Younossi ZM, Rinella ME, Sanyal AJ, Harrison SA, Brunt EM, Goodman Z, et al. From NAFLD to MAFLD: implications of a premature change in terminology. Hepatology. 2021;73(3):1194–1198. https://doi.org/10.1002/hep.31420. (Epub 20210206 PubMed PMID: 32544255)
Rinella ME, Lazarus JV, Ratziu V, Francque SM, Sanyal AJ, Kanwal F, et al. A multi-society Delphi consensus statement on new fatty liver disease nomenclature. J Hepatol. 2023. https://doi.org/10.1016/j.jhep.2023.06.003. (Epub 20230620. PubMed PMID: 37364790)
Pipitone RM, Ciccioli C, Infantino G, La Mantia C, Parisi S, Tulone A, et al. MAFLD: a multisystem disease. Ther Adv Endocrinol Metab. 2023;14:20420188221145548. https://doi.org/10.1177/20420188221145549. (Epub 20230128. PubMed PMID: 36726391; PubMed Central PMCID: PMC9885036)
Wen W, Li H, Wang C, Chen C, Tang J, Zhou M, et al. Metabolic dysfunction-associated fatty liver disease and cardiovascular disease: a meta-analysis. Front Endocrinol (Lausanne). 2022;13:934225. https://doi.org/10.3389/fendo.2022.934225. (Epub 20220916. PubMed PMID: 36187109; PubMed Central PMCID: PMC9523252)
Targher G. Concordance between MAFLD and NAFLD diagnostic criteria in ‘real-world’ data. Liver Int. 2020;40(11):2879–2880. https://doi.org/10.1111/liv.14623. (PubMed PMID: 32738082)
Gutiérrez-Cuevas J, Santos A, Armendariz-Borunda J. Pathophysiological molecular mechanisms of obesity: a link between MAFLD and NASH with cardiovascular diseases. Int J Mol Sci. 2021. https://doi.org/10.3390/ijms222111629. (Epub 20211027. PubMed PMID: 34769060; PubMed Central PMCID: PMC8583943)
Hill MA, Yang Y, Zhang L, Sun Z, Jia G, Parrish AR, et al. Insulin resistance, cardiovascular stiffening and cardiovascular disease. Metabolism. 2021;119:154766. https://doi.org/10.1016/j.metabol.2021.154766. (Epub 20210322 PubMed PMID: 33766485)
Targher G, Corey KE, Byrne CD. NAFLD, and cardiovascular and cardiac diseases: Factors influencing risk, prediction and treatment. Diabetes Metab. 2021;47(2):101215. https://doi.org/10.1016/j.diabet.2020.101215. (Epub 20201206. PubMed PMID: 33296704)
Eslam M, Sanyal AJ, George J. MAFLD: a consensus-driven proposed nomenclature for metabolic associated fatty liver disease. Gastroenterology. 2020;158(7):1999-2014.e1. https://doi.org/10.1053/j.gastro.2019.11.312. (Epub 20200208 PubMed PMID: 32044314)
Lin S, Huang J, Wang M, Kumar R, Liu Y, Liu S, et al. Comparison of MAFLD and NAFLD diagnostic criteria in real world. Liver Int. 2020;40(9):2082–2089. https://doi.org/10.1111/liv.14548. (Epub 20200726 PubMed PMID: 32478487)
Nguyen VH, Le MH, Cheung RC, Nguyen MH. Differential clinical characteristics and mortality outcomes in persons with NAFLD and/or MAFLD. Clin Gastroenterol Hepatol. 2021;19(10):2172–81.e6. https://doi.org/10.1016/j.cgh.2021.05.029. (Epub 20210523 PubMed PMID: 34033923)
Chan KE, Ng CH, Fu CE, Quek J, Kong G, Goh YJ, et al. The spectrum and impact of metabolic dysfunction in MAFLD: a longitudinal cohort analysis of 32,683 overweight and obese individuals. Clin Gastroenterol Hepatol. 2023;21(10):2560–9.e15. https://doi.org/10.1016/j.cgh.2022.09.028. (Epub 20221003 PubMed PMID: 36202348)
Vaz K, Clayton-Chubb D, Majeed A, Lubel J, Simmons D, Kemp W, et al. Current understanding and future perspectives on the impact of changing NAFLD to MAFLD on global epidemiology and clinical outcomes. Hepatol Int. 2023. https://doi.org/10.1007/s12072-023-10568-z. (Epub 20230809. PubMed PMID: 37556065)
Kawaguchi T, Tsutsumi T, Nakano D, Torimura T. MAFLD: Renovation of clinical practice and disease awareness of fatty liver. Hepatol Res. 2022;52(5):422–432. https://doi.org/10.1111/hepr.13706. (Epub 20210917 PubMed PMID: 34472683)
Lim S, Kim JW, Targher G. Links between metabolic syndrome and metabolic dysfunction-associated fatty liver disease. Trends Endocrinol Metab. 2021;32(7):500–514. https://doi.org/10.1016/j.tem.2021.04.008. (Epub 20210508 PubMed PMID: 33975804)
Ballestri S, Zona S, Targher G, Romagnoli D, Baldelli E, Nascimbeni F, et al. Nonalcoholic fatty liver disease is associated with an almost twofold increased risk of incident type 2 diabetes and metabolic syndrome. Evidence from a systematic review and meta-analysis. J Gastroenterol Hepatol. 2016;31(5):936–944. https://doi.org/10.1111/jgh.13264. (PubMed PMID: 26667191)
Cariou B, Byrne CD, Loomba R, Sanyal AJ. Nonalcoholic fatty liver disease as a metabolic disease in humans: a literature review. Diabetes Obes Metab. 2021;23(5):1069–1083. https://doi.org/10.1111/dom.14322. (Epub 20210210. PubMed PMID: 33464677; PubMed Central PMCID: PMC8248154)
Huang Q, Zou X, Wen X, Zhou X, Ji L. NAFLD or MAFLD: which has closer association with all-cause and cause-specific mortality?-results from NHANES III. Front Med (Lausanne). 2021;8:693507. https://doi.org/10.3389/fmed.2021.693507. (Epub 20210701. PubMed PMID: 34277667; PubMed Central PMCID: PMC8280321)
Liang Y, Chen H, Liu Y, Hou X, Wei L, Bao Y, et al. Association of MAFLD with diabetes, chronic kidney disease, and cardiovascular disease: a 4.6-year cohort study in China. J Clin Endocrinol Metab. 2022;107(1):88–97. https://doi.org/10.1210/clinem/dgab641. (PubMed PMID: 34508601; PubMed Central PMCID: PMC8684479)
Song SJ, Lai JC-T, Wong GL-H, Wong VW-S, Yip TC-F. Can we use old NAFLD data under the new MASLD definition? J Hepatol. 2023. https://doi.org/10.1016/j.jhep.2023.07.021
Funding
This study was partially supported by Medica Sur Clinic & Foundation. JG is supported by the Robert W. Storr Bequest to the Sydney Medical Foundation, University of Sydney; a National Health and Medical Research Council of Australia (NHMRC) Program Grant (APP1053206), Project, Ideas and Investigator Grants (APP2001692, APP1107178, APP1108422, APP1196492) and a Cancer Institute, NSW grant (2021/ATRG2028).
Author information
Authors and Affiliations
Contributions
Conception and design: NM-S. Material preparation, data collection and analysis were performed by MMR-M, NM-S and CJ-G. The first draft of the manuscript was written by MMR-M and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Ethics Committee of Medica Sur Clinic & Foundation (protocol code 2021-EXT-552 and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ramírez-Mejía, M.M., Jiménez-Gutiérrez, C., Eslam, M. et al. Breaking new ground: MASLD vs. MAFLD—which holds the key for risk stratification?. Hepatol Int 18, 168–178 (2024). https://doi.org/10.1007/s12072-023-10620-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-023-10620-y