Abstract
Background
Tobacco is consumed mainly as smoking or smokeless tobacco [SLT]. “Smokeless tobacco” (SLT) term is used for the consumption of tobacco mixed with other constituents in form of chewing, spitting and dipping. Consumers of smokeless tobacco chew the products and spit out the juice that builds up in oral cavity which leads to various malignant and pre malignant lesions of oral cavity.
Methods
Descriptive observational study was conducted in the city of Jodhpur through department of ENT, Head & Neck Surgery, Dr. SN medical college, Jodhpur.
Results
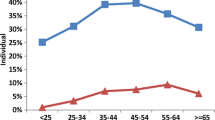
Male to female ratio of smokeless tobacco usage was almost same. Increasing age was associated with occurrence of oral lesions and 43% patients developed oral lesions in the group > 64 yrs of age. Duration was another associating factor and 66% developed symptoms within < 10 years of usage. Oral submucous fibrosis is the most common lesion. Malignant lesions were seen in 0.3% cases. Around 78% cases developed dependency. Diabetic patients were seen more prone to development of oral lesions.
Conclusions
Development of lesions in the oral cavity by smokeless tobacco depends on various factors such as quantity of tobacco usage per day, place of putting tobacco and duration. Awareness regarding its fatal effects and timely diagnosis and management can save many lives.


Similar content being viewed by others
Data Availability
The datasets used in this study are available from corresponding author on reasonable request.
References
Warnakulasuriya S, Muthukrishnan A (2018) Oral health consequences of smokeless tobacco use. Indian J Med Res. 148(1):35. https://doi.org/10.4103/ijmr.ijmr_1793_17
Niaz K, Maqbool F, Khan F, Bahadar H, Ismail Hassan F, Abdollahi M (2017) Smokeless tobacco (paan and gutkha) consumption, prevalence, and contribution to oral cancer. Epidemiol Health 39:e2017009. https://doi.org/10.4178/epih.e2017009
US NCI and WHO. The economics of tobacco and tobacco control. National Cancer Institute (Tobacco Control Monograph 21, NIH Publication No.16-CA-8029). Bethesda, MD; 2016. http://cancercontrol.cancer.gov/brp/tcrb/monographs/21/index.html.
GATS. Global Adult Tobacco Survey: fact sheet, India 2016–17; 2017. http://www.who.int/tobacco/surveillance/survey/gats/GATS_India_2016-17_FactSheet.pdf.
GATS.Global Adult Tobacco Survey: factsheet, India 2016–17; 2017. https://www.who.int/india/heath-topics/tobacco/gats2-state-fact-sheet/rajasthan-gats2-2016-17.pdf
WHO;Oral health assessment form for adults;2013 https://www.who.int/oral_health/publications/pepannex1formadulttooth.pdf
Desai V, Kaur Gill R, Sharma R (2012) Prevalence of habit of tobacco and its deleterious effects in general population of Jaipur district, Rajasthan. J Indian Acad Oral Med Radiol. 24:113–116. https://doi.org/10.5005/jp-journals-10011-1273
Pahwa V, Nair S, Shetty RS, Kamath A (2018) Prevalence of oral premalignant lesions and its risk factors among the adult population in Udupi taluk of coastal Karnataka, India. Asian Pac J Cancer Prev. 19(8):2165–2170. https://doi.org/10.22034/APJCP.2018.19.8.2165
Kawatra A, Lathi A, Kamble SV, Sharma P, Parhar G (2012) Oral Premalignant Lesions associated with areca nut and tobacco chewing among the tobacco industry workers in area of rural Maharastra. Natl J Commun Med 3(2):333
Hallikeri K, Naikmasur V, Guttal K, Shodan M, Chennappa NK (2018) Prevalence of oral mucosal lesions among smokeless tobacco usage: a cross-sectional study. Indian J Cancer 55(4):404–409. https://doi.org/10.4103/ijc.IJC_178_18
Kumar S, Debnath N, Ismail MB, Kumar A, Kumar A, Badiyani BK et al (2015) Prevalence and risk factors for oral potentially malignant disorders in Indian population. Adv Prev Med. 2015:1–7. https://doi.org/10.1155/2015/208519
Narasannavar DA, Head Department of Community Medicine, USM KLE International Medical program, Wantamutte DAS (2014) Prevalence of oral precancerous lesions and conditions among tobacco consumers in rural population around Belgaum. A community based cross sectional study. IOSR J Dent Med Sci. 13(4):31–34. https://doi.org/10.9790/0853-13433134
Ambekar DM, Chaudhary BJ, Kulkarni VV (2014) A study of prevalence of oral precancerous lesions in relation to tobacco habituation. Int J Med Clin Res 5(1):282–285
Srivastava R, Sharma L, Pradhan D, Jyoti B, Singh O (2020) Prevalence of oral premalignant lesions and conditions among the population of Kanpur City, India: a cross-sectional study. J Family Med Prim Care. 9(2):1080–1085. https://doi.org/10.4103/jfmpc.jfmpc_912_19
Mishra GA, Kulkarni SV, Gupta SD, Shastri SS (2015) Smokeless tobacco use in Urban Indian women: prevalence and predictors. Indian J Med Paediatr Oncol 36(3):176–82. https://doi.org/10.4103/0971-5851.166739
Awan KH, Hussain QA, Patil S, Maralingannavar M (2016) Assessing the risk of oral cancer associated with gutka and other smokeless tobacco products: a case-control study. J Contemp Dent Pract 17(9):740–744
Henningfield JE, Fant RV, Tomar SL (1997) Smokeless tobacco: an addicting drug. Adv Dent Res 11(3):330–335. https://doi.org/10.1177/08959374970110030401
Thawal VP, Tzelepis F, Ahmadi S, Palazzi K, Paul C (2022) Addiction perceptions among users of smokeless or combustible tobacco attending a tertiary care hospital in India. Drug Alcohol Rev 41(5):1184–1194. https://doi.org/10.1111/dar.13440
Nair S, Schensul JJ, Begum S, Pednekar MS, Oncken C, Bilgi SM, Pasi AR, Donta B (2015) Use of smokeless tobacco by Indian women aged 18–40 years during pregnancy and reproductive years. PLoS ONE 10(3):e0119814. https://doi.org/10.1371/journal.pone.0119814
Author information
Authors and Affiliations
Contributions
The study was done under complete guidance of NA. The data collection and patient evaluation was done by MS and AB. Statistical analysis and manuscript writing was done by PA. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical Approval
Certificate reference number: SNMC/IEC/2021/plan/482 dated 27/10/2021 by Institutional Ethics Committee, Dr. Sampurnanand Medical College, Jodhpur.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Agarwal, N., Shaikh, M.N., Banu, A. et al. Repercussions of Smokeless Tobacco on Buccal Mucosa: A Community Based Observational Study at a Tertiary Care Centre in Western Rajasthan. Indian J Otolaryngol Head Neck Surg 76, 1891–1897 (2024). https://doi.org/10.1007/s12070-023-04440-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-023-04440-7