Abstract
Objective
This research assessed the relationship between hearing aid usage and quality of life in individuals with hearing impairment, exploring associated demographic and clinical factors.
Methodology
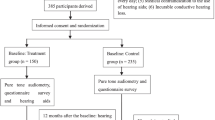
Data from 500 individuals at a tertiary care facility were collected over a year through medical records and an online questionnaire. Quality of life was gauged using WHOQOL-BREF and HHIE. Multiple linear regression analysed the correlation between hearing aid usage and quality of life, adjusting for age, gender, hearing loss severity, and socioeconomic factors.
Results
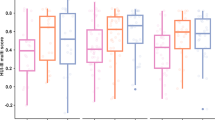
Descriptive statistics showed varying degrees of hearing impairment, socioeconomic status, hearing aid usage, and quality-of-life scores. Bivariate analyses found significant correlations between hearing impairment level, socioeconomic status, hearing aid usage, and quality of life. Linear regression highlighted a positive relationship between daily hearing aid usage duration and quality-of-life scores, even after adjusting for covariates. Variations in quality-of-life ratings were observed between hearing aid users and non-users, spanning different hearing loss levels and socioeconomic statuses. Subgroup analysis showed a positive correlation between hearing aid use and quality of life across age groups.
Conclusion
The study confirms the positive influence of hearing aids on the quality of life in hearing-impaired individuals, emphasizing the benefits of consistent use. Further studies should probe the specific domains and long-term adherence impacts.
Similar content being viewed by others
Data Statement
Data supporting the findings of this study are available from the corresponding author upon reasonable request. Due to the sensitive nature of the data and to maintain participant confidentiality, the data is not publicly available. Any requests for data access will be subject to ethical considerations and participant consent.
References
World Health Organization (2023) Global estimates on prevalence of hearing loss. WHO, Geneva, Switzerland
Contrera KJ, Betz J, Genther DJ et al (2017) Associations of social isolation with anxiety and depression during the early COVID-19 pandemic: a survey of older adults in London, UK. Front Psychiatry 8:591120
Mulrow CD, Aguilar C, Endicott JE et al (1990) Quality-of-life changes and hearing impairment: a randomized trial. Ann Intern Med 113(3):188–194
Dawes P, Emsley R, Cruickshanks KJ et al (2015) Hearing loss and cognition: the role of hearing Aids, social isolation and depression. PLoS ONE 10(3), e0119616
Lin FR, Metter EJ, O’Brien RJ et al (2011) Hearing loss and incident Dementia. Arch Neurol 68(2):214–220
Contrera KJ, Wallhagen MI, Mamo SK et al (2016) Hearing loss health care for older adults. J Am Board Fam Med 29(3):394–403
Kateifidis N, Sarafis P, Malliarou M et al (2016) Quality of life and satisfaction among patients who use hearing Aids. Glob J Health Sci Dec 9(6):177
Perez-Mora R, Lassaletta L, Castro A et al (2012) Quality of life in hearing-impaired children with bilateral hearing devices. B-ENT 8(4):251
Fitzpatrick EM, Olds J, Gaboury I et al (2012) Comparison of outcomes in children with hearing Aids and cochlear implants. Cochlear Implants Int Feb 13(1):5–15
Dawes P, Cruickshanks KJ, Fischer ME et al (2015) Hearing-aid use and long-term health outcomes: hearing handicap, mental health, social engagement, cognitive function, physical health, and mortality. Int J Audiol Nov 54(11):838–844
Mulrow CD, Aguilar C, Endicott JE et al (1990) Quality-of-life changes and hearing impairment: a randomized trial. Ann Intern Med Aug 113(3):188–194
Cohen-Mansfield J, Taylor JW (2004) Hearing aid use in nursing homes, part 2: barriers to effective utilization of hearing Aids. J Am Med Dir Assoc Sep 5(5):289–296
Pasmatzi E, Koulierakis G, Giaglis G (2016) Self-stigma, self-esteem and self-efficacy of mentally ill. Psychiatriki. Oct
Hornsby BW (2013) The effects of hearing aid use on listening effort and mental fatigue associated with sustained speech processing demands. Ear Hear Sep 34(5):523–534
Acknowledgements
Author extends gratitude to Dr. Kashi Birader for designing the study model and questionnaire, Dr. Sudhir for his efforts in data collection & Dr Angshuman Dutta for reviewing revision manuscript & providing suggestion. Our thanks also go to the hospital staff and the participating patients for their invaluable contributions to this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
• No conflicts of interest.
• No research involving human participants or animals was conducted.
• The patient provided informed consent for publication of the case study.
• This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
• There are no material financial or non-financial interests to disclose for the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kumar, S., Biradar, K., Marlapudi, S. et al. Hearing Aids and Quality of Life: A Psychological Perspective. Indian J Otolaryngol Head Neck Surg 76, 852–857 (2024). https://doi.org/10.1007/s12070-023-04297-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-023-04297-w