Abstract
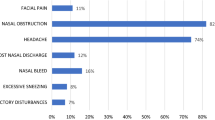
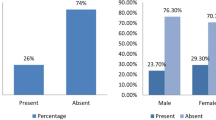
Chronic rhinosinusitis (CRS) is widely prevalent globally. Fungal rhinosinusitis is a subtype which requires early detection by using appropriate tests and to make an accurate decision regarding the treatment modality. This study aims at determining the clinicomycological profile of fungal rhinosinusitis (FRS). A total of 105 patients with CRS were included in the study which was prospectively done during a time period of 18 months in a tertiary care hospital. All patients were subjected to CT scans and diagnostic nasal examinations (DNE) preoperatively. The sinonasal specimens were subjected to KOH mount, fungal culture and histopathological examination following functional endoscopic sinus surgery (FESS). 53% of the patients with fungal sinusitis belonged to the age group 41–60 years. The prevalence of FRS was found to be 38% with aspergillus species accounting for about 85% cases. FRS is a disease which can have a wide spectrum of clinical presentations requiring early detection and appropriate treatment which is essential to avoid both short term and long term sequalae.




Similar content being viewed by others
References
International Rhinosinusitis Advisory Board (1997) Infectious rhinosinusitis in adults: classification, etiology and management. Ear Nose Throat J 76:5–22
Mark S, Schubert (2009) ; 47 (Supplement 1) : 324 – 30
Benninger M, Ferguson B, Hadley J et al (2003) Adult chronic rhinosinusitis: definitions, diagnosis, epidemiology, and pathophysiology. Otolaryngol Head Neck Surg 129(Suppl):1–32
Meltzer EO, Hamilos DL, Hadley JA et al (2004) Rhinosinusitis: establishing definitions for clinical research and patient care. J Allergy Clin Immunol 114(Suppl):155–212
Hamilos DL (2000) Chronic sinusitis. J Allergy Clin Immunol 106:213–227
Hamilos DL (2001) Noninfectious sinusitis. ACI Int 13:27–32
Schubert MS (2006) Allergic fungal sinusitis. Clin Rev Allergy Immunol 30:205–216
Pannathat Soontrapa N, Larbcharoensub T, Luxameechanporn et al (2010) Fungal rhinosinusitis: a retrospective analysis of clinicopathologic features and treatment outcomes at ramathibodi hospital. Southeast asian J trop med public health 42:442–449
Das A, Bal A, Chakrabarti A et al (2009) Spectrum of fungal rhinosinusitis; histopathologist’s perspective. Histopathology 54:854–859
De Shazo RD, Chapin K, Swain R (1997a) Fungal sinusitis. N Engl J Med 337:254–259
Granville L, Chirala M, Cernoch P et al (2004) Fungal sinusitis: histologic spectrum and correlation with culture. Hum Pathol 35:474–481
Sandeep Suresh D, Arumugam G, Zacharias et al (2016) Prevalence and clinical profile of fungal rhinosinusitis. Allergy Rhinol 7:115–120
Rajiv C, Michael, Joy S, Michael1, Ruth H, Ashbee1 et al (2008) Mycological profile of fungal sinusitis: an audit of specimens over a 7-year period in a tertiary care hospital in Tamil Nadu. Indian J Pathol Microbiol 51(4):493–496
Dall’Igna C, Palombini BC, Anselmi F et al (2005) Fungal rhinosinusitis in patients with chronic sinusal disease. Braz J Otorhinolaryngol 71(6):712–720
Dr HS, Satish Dr. Jolene Alokkan, ‘Clinical study of Fungal Rhinosinusitis’,IOSR Journal of Dental and Medical Sciences. ; 5(4) :37–40
Singh AK, Gupta P (2017) Fungal rhinosinusitis: microbiological and histopathological perspective. J Clin Diagn Res 11(7):10–12
Navya N, Vivek T, Sudhir et al (2015) Role of histopathology in the diagnosis of Paranasal Fungal Sinusitis. IOSR J Dent Med Sci 14(1):97–101
Karthikeyan P, Nirmal Coumare V (2010) Incidence and presentation of fungal sinusitis in patient diagnosed with chronic Rhinosinusitis. Indian J Otolaryngol Head Neck Surg 62(4):381–385
Funding
No source of funding for the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study is conducted abiding the ethical standards of the institution.
Conflict of Interest
There is no conflict of interest amongst the authors of the study.
Informed consent
A written and informed consent was taken for the procedure from all the participants of the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Menon, N.N., B, B.M. & S, S. Clinicomycological Profile of Fungal Rhinosinusitis in South India. Indian J Otolaryngol Head Neck Surg 75, 2142–2148 (2023). https://doi.org/10.1007/s12070-023-03826-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-023-03826-x