Abstract
Amyotrophic lateral sclerosis (ALS) is a neurodegenerative disease pathologically characterized by selective degeneration of motor neurons resulting in a catastrophic loss of motor function. The present study aimed to investigate the effect of copper (Cu) exposure on progression of ALS and explore the therapeutic effect and mechanism of Urolithin A (UA) on ALS. 0.13 PPM copper chloride drinking water was administrated in SOD1G93A transgenic mice at 6 weeks, UA at a dosage of 50 mg/kg/day was given for 6 weeks after a 7-week Cu exposure. Motor ability was assessed before terminal anesthesia. Muscle atrophy and fibrosis, motor neurons, astrocytes and microglia in the spinal cord were evaluated by H&E, Masson, Sirius Red, Nissl and Immunohistochemistry Staining. Proteomics analysis, Western blotting and ELISA were conducted to detect protein expression. Mitochondrial adenosine triphosphate (ATP) and malondialdehyde (MDA) levels were measured using an assay kit. Cu-exposure worsened motor function, promoted muscle fibrosis, loss of motor neurons, and astrocyte and microglial activation. It also induced abnormal changes in mitochondria-related biological processes, leading to a significant reduction in ATP levels and an increase in MDA levels. Upregulation of P62 and downregulation of Parkin, PINK1, and LAMP1 were revealed in SOD1G93A mice with Cu exposure. Administration of UA activated mitophagy, modulated mitochondria dysfunction, reduced neuroinflammation, and improved gastrocnemius muscle atrophy and motor dysfunction in SOD1G93A mice with Cu exposure. Mitophagy plays critical role in ALS exacerbated by Cu exposure. UA administration may be a promising treatment strategy for ALS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Amyotrophic lateral sclerosis (ALS) is a neurodegenerative disease characterized by the selective loss of upper and lower motor neurons in the cerebral cortex, brainstem, and spinal cord [1]. Approximately 10% of ALS cases are familial, while the remaining 90% are sporadic [2]. Clinical features of ALS include progressive muscle atrophy and weakness, dysphagia, and eventually respiratory failure [3, 4]. Currently, only riluzole and edaravone have been approved for ALS treatment, but their effectiveness is limited [5]. Due to the lack of effective treatments, ALS typically leads to death within 3–5 years after the onset of the disease [6].
Copper (Cu) is involved in various important functions such as respiration, energy production, myelination of neurons, synthesis of neurotransmitters, immune system response, collagen formation, synthetic dyestuff, and tissue repair after trauma [7,8,9]. Two studies from northern Italy and Michigan revealed the significance of copper exposure in ALS risk and progression [10, 11]. Cu levels were elevated in the spinal cord of transgenic mouse models carrying different SOD1 mutations [12, 13]. In the SOD1G93A mouse model, Cu accumulation preceded the appearance of clinical symptoms, suggesting that high Cu is a characteristic pathology [13]. Excessive copper ion accumulation may disrupt mitochondrial respiratory function by inhibiting the synthesis of iron-sulfur cluster proteins, thereby inducing proteotoxic stress and precipitating a novel form of cell death known as copper-induced cell death [14]. However, Hilton JBW and his colleagues found decreased copper levels in the ventral grey matter, the primary anatomical site of neuronal loss in sporadic ALS [15].
SOD1 transgenic mice showed increased CTR1 levels, decreased ATP7A levels and high levels of metallothionein (MT) in spinal cord in SOD1G93A mice, which has a high affinity for Cu [16].The hypothesis posits that ALS pathogenesis is influenced by dysregulation of copper homeostasis, not by copper ions per se. Validation of the role of low-dose copper exposure in inducing copper-induced cell death versus rectifying copper metabolic dyshomeostasis is necessary to elucidate its impact on ALS etiology.
Mitochondrial dysfunction is a prevalent feature observed in various neurodegenerative diseases, including ALS [17]. It leads to bioenergetic failure, oxidative stress, apoptosis, and potential cell death [18]. Urolithin A (UA), known as a mitophagy activator, has been investigated for its potential to improve mitochondrial function and reduce inflammation, that captures the attention of scientists [19, 20].
In this study, we aimed to investigate the effects of low-dose Cu exposure on the progression of SOD1G93A mice, a transgenic model of ALS, and to explore the therapeutic effect and mechanism of UA on SOD1G93A mice with Cu exposure.
Materials and Methods
Reagents and Antibodies
Copper chloride (II) (CuCl2) was purchased from Sigma-Aldrich (MO, USA) for this study, while UA (specified purity ≥ 98%) was obtained from Macklin-Lab Company (U884401 Urolithin A, CAS no. 1143–70-0). Antibody dilution ratios and product information can be found in Supplementary Table 1.
Animal Breeding and Rearing
The ALS model mouse, transgenic for human SOD1G93A (B6Cg-Tg (SOD1*G93A)1Gur/J, stock number 004435), which expresses a G93A mutant form of human SOD-1, was purchased from Jackson Laboratory (Maine, USA) along with six-week-old mice. All mice were housed in a 12-h light–dark cycle chamber with a stable temperature (20–22℃) and humidity (55%) at the Laboratory Animal Center, Shenzhen Center for Disease Control and Prevention, China. Starting at six weeks of age, female SOD1G93A transgenic mice and WT mice were given 0.13PPM Cu chloride drinking water and normal drinking water treatment [21]. After 7 weeks of Cu exposure, SOD1G93A transgenic mice with Cu exposure were given 50 mg/kg/day UA or saline for 6 weeks (Fig. S1). During the animal experimentation, we followed the ARRIVE guidelines and conducted the study in accordance with the UK Animals (Scientific Procedures) Act 1986 and relevant guidance, as well as the National Research Council Guide for the Care and Use of Laboratory Animals.
Behavioral Tests
Climbing-Pole Test
The climbing-pole test was conducted to evaluate the movement and coordination of the limbs in mice [22]. Mice were placed on rough wooden balls with a rough surface and cross-section, and lower rods were placed in the cage. The mice were positioned upside down to climb from the wooden balls below. The time for the mouse to climb the entire stick was recorded by starting the stopwatch when the mouse started climbing (A) and stopping it when the mouse reached the bottom (B). The total climbing time (C) was calculated as C = A—B. The mice underwent three days of training before the test, twice a day, with a 15-s cut-off value. Each mouse was tested three times, and the average climbing time from the three tests was used as a statistical index.
Rotarod Test
The rotarod test was performed to assess the coordination of movements in mice [23]. Mice were placed on a rotating rod with a diameter of 3 cm, and the rotation speed was set at 30r/min. Five mice were measured simultaneously, with one mouse in each compartment. The measurement time was 3 min, and the time from the start of the rotating rod to the point of dropping off was recorded. The mice underwent training twice a day for three days, with a 300-s threshold. The experiment was repeated three times, and the longest time among the three results was used for evaluation.
Hanging Endurance Test
The hanging endurance test was used to assess the grasping strength of mouse limbs. The mouse was placed in the center of a 21 cm × 21 cm grid (with a line width of approximately 0.1 cm and a spacing of 0.5 cm) and then the grid was inverted to record the time the mouse remained suspended (grasping time). Training was conducted for three consecutive days, twice a day, with a 180-s cut-off value. Any recordings beyond 180 s were capped at 180 s. The experiment was repeated three times, and the longest time among the three results was used for evaluation.
Grip Strength Test
The grip strength test was performed to directly evaluate the muscle strength of mouse limbs [24]. The mouse was placed in the middle of the grip plate on the gripper, and its tail was gently tugged to help it grasp the grip plate. The mouse would release its paw once it had a solid grip, and the force exerted was measured to assess grip strength. The experiment was conducted three times, and the evaluation value was the average of the results.
Gait Test
The gait test is conducted to evaluate the coordination of limb movement in mice [25]. At different time points, we first observe the mice's autonomous motion and then collect gait information during their walking process.
H&E, Masson, Sirius Red, and Nissl Staining, Immunohistochemistry
Spinal cord specimens were isolated from 4 to 5 lumbar spine segments, fixed in 4% paraformaldehyde for 48 h, gradually dehydrated using sucrose gradients, and embedded in paraffin. Sections of the spinal cord (5 µm) were stained with specific staining solutions. For immunohistochemistry, the sections were boiled in sodium citrate for 10 min to repair the antigenic damage, then peroxidase was removed, and the sections were incubated with a protease blocking solution at room temperature for 1 h, and the primary antibodies (GFAP, Iba1, and ChAT) were diluted at 4 degrees Celsius overnight according to the instructions on the website. After the primary antibody was washed, the slices were treated with secondary and tertiary antibodies at room temperature, and then stained with DAB for 2–5 min. All tissue samples were examined using an optical microscope and analyzed using Image-J software.
Proteomics
Extraction and Digestion of Proteins
Each spinal cord tissue was treated with an 8 M urea lysis buffer for protein extraction, followed by sonication. The concentration of extracted proteins was determined using the BCA Protein Assay Kit (Thermo Fisher, NJ, USA). Five individual samples were pooled together in equal amounts (1: 1: 1: 1: 1) to obtain a total of 100 µg protein in each group for enzymatic digestion and protein labeling. The samples were reduced and alkylated using dithiothreitol (DTT) and iodoacetamide (IAA), respectively, and then incubated with proteases at 37℃. After digestion, formic acid was added to adjust the pH of the sample to 1–2. The peptide mixture was desalted using a reversed-phase column (Oasis HLB, Waters, USA) and dried in a vacuum centrifuge before being labeled with tandem mass tags (TMT).
Analysis using LC–MS/MS and TMT Labeling
The peptides from the spinal cord samples were reconstituted, and 50 µL of 200 mM triethyl ammonium bicarbonate (TEAB) was added to each sample. Peptides were labeled according to the instructions provided with the TMT kit and incubated at room temperature for 1 h. To stop the reaction, 8 µL of 5% hydroxylamine was added and incubated for 15 min. The labeled peptides were then desalted, dried, and reconstituted in 100 µL of 0.1% formic acid (FA). High-performance liquid chromatography (HPLC) was used to separate the TMT-labeled peptides based on their components [26]. The labeled peptide samples were loaded onto an Xbridge BEH300 C18 column (Waters, USA). The peptide sample was isolated using Thermo Fisher Scientific's UltiMate 3000 UHPLC and separated into 15 fractions. The fractions were subsequently dried, reconstituted in 20 µL of 0.1% FA, and subjected to liquid chromatography-LC–MS/MS analysis. All proteomic data were deposited in the PRIDE partner repository under the dataset identifier PXD039728.
Bioinformatics Analysis
Differentially expressed proteins were assessed for their abundance in each group using a heat map technique. Protein cluster analysis was performed using Hiplot software (http://www.chiplot.online). The biological mechanisms and pathways associated with the differentially expressed proteins were identified using Metascape software. WebGestalt searches and gene ontology analysis can be conducted using DAVID Bioinformatics Resources 6.8. Pictures were visualized using Cytoscape software after MCODE analysis was used to identify dense protein–protein interaction (PPI) regions.
Western Blot
Spinal cord histamins were cleaved using RIPA lysis buffer (Thermo Scientific, NJ, USA) containing 1 × protease and phosphatase inhibitors, and the supernatant of spinal cord tissue proteins was collected after ultrasound centrifuge. BCA kit (Thermo, USA) was used for protein concentration quantification, a small part of the extracted protein solution was extracted, and then diluted 40 times with ultra-pure water, followed by the preparation of a standard solution, drawing a standard curve according to the measured OD value, so that the protein concentration of the sample was determined by the OD value of each sample (the sample size was determined according to the protein concentration). Protein samples were separated on 10% SDS-PAGE gels and transferred to PVDF membranes. The membranes were then blocked with 5% skim milk for 1–2 h. Primary antibodies were incubated with the membranes overnight at 4℃. After washing with TBST buffer, the membranes were incubated with corresponding diluted secondary antibodies at room temperature. Chemiluminescence was used to visualize the protein bands using an ECL kit (Thermo Scientific, NJ, USA).
Mitochondrial Functional Analysis
Mitochondrial function in mouse tissues was assessed by measuring lipid peroxidation and ATP levels, following previously published methods [27]. The spinal cord tissue was completely lysed with RIPA strong lysate and the spinal cord tissue supernatant was extracted. The concentration of protein in freshly extracted spinal cord tissue was determined with BCA kit. A protein sample or standard (100 µL) was mixed with an MDA detection solution (200 µL) and reacted at 100° C for 15 min. Then let the mixture cool to room temperature, centrifuge at 1000 g for 10 min, and remove the supernatant. Finally, 200 μL supernatant was added to the 96-well plate and the absorbance was measured at 532 nm using an enzymogram [28]. Lipid peroxidation levels are expressed in mol/g protein. The spinal cord tissue was completely lysed with ATP lysate. The protein concentration of spinal cord supernatant was determined by BCA method. The standard ATP solution is diluted with the ATP-detected lysate to the appropriate concentration gradient to make the standard curve. Mix 20 μL of protein or standard with 20 μL of ATP working liquid and leave it at room temperature for 3 min [29]. The concentration of ATP in the sample is quickly measured using an enzyme-labeled instrument with luminometer function. ATP levels are expressed in moles per g of protein.
Statistical Analysis
All statistical analyses were performed using GraphPad Prism 9.0 statistical software (La Jolla, CA, USA). The data were presented as Mean with 95% CI, all data were tested by Shapiro–Wilk or Kolmogorov–Smirnov normality test. Data followed a normal distribution and were analyzed using two-tailed Student's t-test, one-way ANOVA with Tukey's post hoc test. Otherwise, data were analyzed using the Mann–Whitney test. A p-value of less than 0.05 was considered statistically significant.
Results
Cu Exposure Exacerbated Motor Dysfunction in SOD1G93A Mice
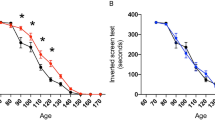
Compared to WT mice, the body weight of 19-week-old SOD1G93A mice was significantly decreased, and further significant weight loss was observed in Cu-treated SOD1G93A mice compared to controls (P < 0.05) (Fig. 1A). SOD1G93A mice showed a significant decrease in motor function in pole-climbing, rotarod, hanging, and grip tests. The Cu-treated group SOD1G93A mice exhibited even greater motor function decline in the rotarod, and grip tests compared to SOD1G93A mice (P < 0.05), but no significant difference was observed in the pole-climbing and hanging tests (Fig. 1B-E). Gait analysis revealed walking impairments in SOD1G93A mice, with significantly reduced stride length and base of support compared to WT mice. Cu treatment further exacerbated these walking abnormalities (P < 0.05, P < 0.001) (Fig. 1F-H).
Cu exposure exacerbates motor performance deficits in SOD1G93A mice (A) Percentage weight gain at 19 weeks, n = 7–8. *, P < 0.05, one-way ANOVA. (B) Time on the pole in the pole-climbing test, n = 7–8. ***, P < 0.001, one-way ANOVA. (C) Retention time on the rotarod in the rotarod test, n = 7–8. *, P < 0.05, one-way ANOVA. (D) Hanging endurance time in the hanging test, n = 7–8. ***, P < 0.001, one-way ANOVA. (E) Grip force in the grip force test, n = 7–8. *, P < 0.05, **, P < 0.01, one-way ANOVA. (F) Representative image of gait analysis at 19 weeks, with arrows indicating stride length. (G-H) Statistical analysis of stride length and base of support in gait analysis n = 7–8. *, P < 0.05, ***, P < 0.001, one-way ANOVA. Data were expressed as Mean with 95% CI
Cu Exposure Exacerbated Muscle Atrophy and Fibrosis in SOD1G93A Mice
At 19 weeks, the weight of the gastrocnemius muscle in SOD1G93A mice was significantly lower than in WT mice, and this reduction was further pronounced in the Cu-treated SOD1G93A mice group. Histological staining with H&E, Masson, and Sirius Red revealed significant muscle atrophy and reduced cross-sectional area in the gastrocnemius muscle of the SOD1G93A group compared to the WT group. These changes were more prominent after Cu treatment (P < 0.05) (Fig. 2).
Cu treatment exacerbates muscle atrophy and fibrosis in SOD1G93A mice (A) Representative images of the gastrocnemius muscle. (B) Statistics of gastrocnemius weight relative to body weight, n = 7. *, P < 0.05, one-way ANOVA. (C) Representative images of H&E staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. (D) Representative images of Masson staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. (E) Representative images of Sirius Red staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. Data were expressed as Mean with 95% CI
Cu Exposure Exacerbated Motor Neuron Loss and Neuroinflammation in SOD1G93A Mice
Immunostaining of the spinal cord revealed a significant increase in the number of GFAP + and Iba-1 + cells in the Cu-treated SOD1G93A mice group compared to the control group. Additionally, there was a significant decrease in motor neurons observed through Nissl staining and ChAT immunostaining in the spinal cord of Cu-treated SOD1G93A mice (P < 0.05, P < 0.01, P < 0.001) (Fig. 3).
Cu treatment increases the number of astrocytes and microglia in the spinal cord of SOD1G93A mice and decreases the number of spinal motor neurons (A) Representative images and quantitative analysis of Nissl staining. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 100 scale bars: 20 μm (bottom panels), n = 3. *, P < 0.05, one-way ANOVA. (B) Representative images and quantitative analysis of ChAT immunostaining (Original magnification × 20, scale bars: 100 μm), n = 3. *, P < 0.05, one-way ANOVA. (C) Representative images and quantitative analysis of GFAP (astrocytes) immunostaining in the spinal cord. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. *, P < 0.05, ***, P < 0.001, one-way ANOVA. (D) Representative images and quantitative analysis of Iba1 (microglia) immunostaining in the spinal cord. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. *, P < 0.05, **, P < 0.01, one-way ANOVA. Data were expressed as Mean with 95% CI
Cu Exposure Disrupted Protein Networks and Impaired Mitochondrial Function
Proteins were collected from the spinal cord to investigate abnormal protein networks following Cu exposure, and LC–MS/MS analysis was performed. Hiplot software was used for cluster analysis, and the differentially expressed proteins (DEPs) from WT, SOD1G93A mice, and Cu-treated SOD1G93A mice groups were divided into six clusters. Cluster 1 showed an upward trend in DEPs, while cluster 6 showed a downward trend (Fig. 4A-B) (Fig. S2). GO analysis identified essential biological processes within these six clusters.
Cluster analysis reveals expression profiles and enriched biological processes in WT, SOD1G93A, and Cu-exposed SOD1G93A group (A) Clusters 1 of expression profiles from cluster analysis and corresponding enriched biological processes. (B) Clusters 6 of expression profiles from cluster analysis and corresponding enriched biological processes. (C) Core modules and enriched pathways for clusters 1 and 6 in proteomic results. Blue represents low abundance, and red represents high abundance. n = 6 for each group. (D-E) ATP levels and lipid peroxidation levels were measured, n = 7. *, P < 0.05, **, P < 0.01, one-way ANOVA. Data were expressed as Mean with 95% CI
Metascape analysis revealed that spinal cord proteins in SOD1G93A mice, after exposure to Cu, displayed abnormal expression in mitochondria-related biological processes, such as inflammatory immune response and mitochondrial electron respiratory transport chain (Fig. 4C). Compared to the SOD1G93A mice group, ATP levels significantly decreased, and MDA levels significantly increased in the Cu-treated SOD1G93A mice group (P < 0.05, P < 0.01) (Fig. 4D, 4E). Heat map analysis demonstrated a decrease in the expression of mitochondria-related proteins following Cu exposure (Fig. S3).
Cu Exposure Inhibited Mitophagy in SOD1G93A Mice
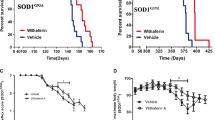
Mitophagy is a process that removes excessive or damaged mitochondria. The impact of low-dose Cu exposure on mitophagy was assessed using western blot analysis. Compared to the WT mice group, upregulation of P62 and downregulation of LC3II/LC3I, Parkin, PINK1, TOM40, P-AMPKα/AMPKα, LAMP1, and CTSD were observed in SOD1G93A mice. Furthermore, there was further upregulation of P62 and downregulation of Parkin, PINK1, and LAMP1 in SOD1G93A mice exposed to Cu (P < 0.05, P < 0.01) (Fig. 5A-B), indicating inhibition of autophagy and mitophagy after Cu exposure. Expression levels of electron transport chain proteins, such as NDUFA10, SDHB, UQCRFS1, and ATP5a, were significantly decreased in the SOD1G93A mice group compared to the WT mice group. Additionally, NDUFA10 and ATP5a were significantly decreased in SOD1G93A mice exposed to Cu (P < 0.05, P < 0.01) (Fig. 5C, 5D).
Cu treatment inhibits mitophagy in the spinal cord of SOD1G93A mice and impairs mitochondrial function by altering mitochondrial dynamics in the spinal cord (A-B) Quantification of AMPKα kinase activity status and expression levels of P62, PINK1, Parkin, LAMP1, and other mitophagy and autophagy-lysosomal related proteins, n = 3. *, P < 0.05, **, P < 0.01 vs. WT group; #, P < 0.05 vs. SOD1G93A vehicle group, one-way ANOVA. (C-D) Western blot and quantitative analysis of electron transport chain proteins NDUFA10, SDHB, UQCRFS1, and ATP5a, n = 3. *, P < 0.05, one-way ANOVA. Data were expressed as Mean with 95% CI
UA Improved Motor Function in Cu-Exposed SOD1G93A Mice by Activating Mitophagy
UA, a mitophagy activator [30], was administered to Cu-exposed SOD1G93A mice for 6 weeks starting at 13 weeks. Compared to Cu-exposed SOD1G93A mice, UA administration significantly improved body weight gain, performance on the rotarod, hang test, and grip strength (P < 0.05, P < 0.01, P < 0.001) (Fig. 6A-E). Gait analysis demonstrated that UA treatment improved walking impairments in Cu-exposed SOD1G93A mice, with significant increases in stride length and base of support observed in SOD1G93A mice with UA administration (P < 0.05, P < 0.001) (Fig. 6F-H).
UA improves motor performance in Cu-exposed SOD1G93A mice (A) Percentage weight gain at 19 weeks, n = 7. *, P < 0.05, Student's t-test. (B) Time on the pole in the pole-climbing test, n = 7. (C) Retention time on the rotarod in the rotarod test, n = 7. *, P < 0.05, Student's t-test. (D) Hanging endurance time in the hanging test, n = 7. **, P < 0.01, Student's t-test. (E) Grip force in the grip force test, n = 7. **, P < 0.01, Student's t-test. (F) Representative image of gait analysis at 19 weeks, with arrows indicating stride length. (G-H) Statistical analysis of stride length and base of support in gait analysis, n = 7. *, P < 0.05, ***, P < 0.001, Student's t-test. Data were expressed as Mean with 95% CI
At 19 weeks, compared to the Cu-exposed SOD1G93A mice group, the muscle weight/body weight ratio significantly increased with UA administration (P < 0.05) (Fig. 7A). Histological staining with H&E, Masson, and Sirius Red revealed that gastrocnemius muscle atrophy improved with UA administration (Fig. 7B-D).
UA improves muscle atrophy and fibrosis in Cu-exposed SOD1G93A mice (A) Statistics of gastrocnemius weight relative to body weight, n = 7. *, P < 0.05, Student's t-test. (B) Representative images of H&E staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. (C) Representative images of Masson staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. (D) Representative images of Sirius Red staining of the gastrocnemius muscle. Original magnification × 10, scale bars: 200 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. Data were expressed as Mean with 95% CI
Furthermore, compared to the Cu-exposed SOD1G93A mice group, the number of GFAP + and Iba1 + cells in the spinal cord, as measured by immunostaining, significantly decreased with UA administration. Additionally, there was a significant increase in motor neuron count observed through Nissl staining and ChAT immunostaining in the spinal cord with UA administration (P < 0.05, P < 0.01) (Fig. 8).
UA decreases the number of astrocytes and microglia in the spinal cord of Cu-exposed SOD1G93A mice and increases the number of spinal motor neurons (A) Representative images and quantitative analysis of Nissl staining. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 100 scale bars: 20 μm (bottom panels), n = 3. **, P < 0.01, Student's t-test. (B) Representative images and quantitative analysis of ChAT immunostaining (Original magnification × 20, scale bars: 100 μm), n = 3. *, P < 0.05, Student's t-test. (C) Representative images and quantitative analysis of GFAP positive immunostaining in the spinal cord. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. **, P < 0.01, Student's t-test. (D) Representative images and quantitative analysis of Iba1 positive immunostaining in the spinal cord. Dashed boxes on top panels indicate region shown at higher magnification in bottom panels. Magnification = × 20, scale bars: 100 μm (top panels), × 40 scale bars: 50 μm (bottom panels), n = 3. **, P < 0.01, Student's t-test. Data were expressed as Mean with 95% CI
Proteomic analysis indicated that UA intervention upregulated biological processes related to muscle contraction and mitochondrial function (Fig. 9A). Mitochondrial functional analysis demonstrated that UA increased ATP levels and significantly decreased lipid peroxidation levels in Cu-exposed SOD1G93A mice (P < 0.01) (Fig. 9D, 9E). Additionally, UA activated autophagy and mitophagy, as evidenced by the significant increase in expression of PINK1, Parkin, and LAMP1 in the spinal cord, and the increased level of NDUFA10 (an electron transport chain protein) in Cu-exposed SOD1G93A mice (P < 0.05) (Fig. 9B, 9C).
UA activates mitophagy in the spinal cord of Cu-exposed SOD1G93A mice and improves mitochondrial function by altering mitochondrial dynamics in the spinal cord (A) Core modules and enriched pathways in proteomic results. Blue represents low abundance, and red represents high abundance. (B, C) Quantification of AMPKα kinase activity state and the expression levels of mitophagy and autophagy-lysosome-related proteins such as PINK1, Parkin, and LAMP1, as well as electron transport chain-related proteins, n = 4. *, P < 0.05, Student's t-test. (D, E) ATP levels and lipid peroxidation levels were measured, n = 7. **, P < 0.01, Student's t-test. Data were expressed as Mean with 95% CI
Discussion
Motor neuron degeneration in the cortex, brain stem, and spinal cord is a prominent feature of ALS, a fatal neurodegenerative disease characterized by progressive muscle paralysis [31]. In the present study, low-dose Cu exposure exacerbated motor dysfunction in SOD1G93A mice, accelerated motor neuron degeneration in the spinal cord, and increased muscle atrophy and fibrosis. The underlying mechanism involved the impairment of mitochondrial function, particularly inhibition of mitophagy. Administration of UA improved motor function in SOD1G93A mice exposed to Cu by activating mitophagy, highlighting the crucial role of mitophagy in Cu-mediated aggravation of ALS and exploring a promising treatment strategy for ALS.
In ALS, alterations in Cu homeostasis may contribute to the disease's development. Spinal cord tissue from sporadic ALS patients has shown a notable increase in Cu concentration [32]. Elevated blood Cu levels have also been identified as potential risk factors for ALS [33]. Disruptions in Cu balance can compromise the functionality of enzymes, receptors, and transporter structures, leading to oxidative stress, alpha-synuclein aggregation, fiber formation, and activation of microglia cells [34, 35]. In 2022, scientist showed copper-induced cell death dependent on mitochondrial respiration in human cells, it explained the need for ancient copper homeostatic mechanisms [14]. In this study, low-dose Cu exposure exacerbated motor decline and associated pathological changes in SOD1G93A mice, a model of ALS. Furthermore, metascope analysis in Cu-exposed SOD1G93A mice revealed abnormal expression of proteins related to mitochondrial processes, such as inflammatory immune response and mitochondrial electron respiratory transport chain. Decreased activity of citrate synthase and respiratory chain complexes I + III, II + III, and IV in the spinal cord tissue of ALS patients post-mortem has been illuminated [36,37,38]. This may be attributed to selective loss of mitochondria or increased mitochondrial DNA damage in the ALS spinal cord [39].
Maintenance of healthy mitochondria through the process of mitophagy is pivotal in various neurodegenerative diseases such as Alzheimer's, Parkinson's, ALS, frontotemporal dementia, and Huntington's disease. Insufficient mitophagy leads to the accumulation of damaged mitochondria, resulting in increased oxidative stress and reduced ATP levels, leading to cellular damage and apoptosis [40,41,42]. Excessive accumulation of Cu induces tissue damage by promoting apoptosis and inhibiting mitophagy, along with the down-regulation of autophagy-related proteins, such as Atg5, Beclin1, Pink1, Parkin, P62, and LC3B [43]. In the present study, this disruption was observed in SOD1G93A mice exposed to Cu, where a decrease in crucial proteins involved in mitophagy was noted, further exacerbated ATP reduction and oxidative stress. Evidence suggests that Cu exposure disrupts the autophagy-lysosomal pathway in ATP7B-deficient hepatocytes [44], and chronic Cu exposure may induce pathological damage by interfering with the mitophagy and subsequent apoptosis [45]. Notably, the activation of mitophagy may serve as an initial response to stress, the subsequent oxidative stress due to mitochondrial dysfunction is a common factor in ALS and other neurodegenerative diseases. During the ALS process, energy metabolism disturbances contribute to activation of astrocyte and microglia, triggering damage in motor neurons mediated by pathways like NF-κB or TGFB through [46,47,48]. In the context of ALS, exposure to Cu induced mitochondrial dysfunction by hindering mitophagy, resulting in neuron loss in SOD1G93A mice.
In order to determine whether mitophagy plays a decisive role in ALS exacerbated by Cu exposure, UA, a mitophagy activator was administrated and showed beneficial effects by improving the motor function, alleviating muscle atrophy and fibrosis, reducing motor neuron loss, and mitigating neuroinflammation. The therapeutic effect of UA was mediated by activation of autophagy and mitophagy which manifested with increasing the expression of PINK1, Parkin, and LAMP1 in the spinal cord. UA modulates the PINK1/Parkin-mediated mitophagy pathway by augmenting the stability of the PINK1 kinase. This stabilization eventuates in the translocation of Parkin to the mitochondria, culminating in the ubiquitination of mitochondrial proteins. The ubiquitin chains are subsequently phosphorylated by PINK1, precipitating the accumulation of phospho-ubiquitinated mitochondrial proteins that function as anchorage sites for adapter proteins, including optineurin and p62. These adapters then interact with microtubule-associated protein 1 light chain 3 (LC3), facilitating the autophagic process. Additionally, UA is shown to activate a mitophagy pathway that is independent of the PINK1/Parkin axis, as denoted by the elevated levels of mitochondrial BNIP3 [49].
Previous studies have indicated that UA enhances ATP and NAD + levels by up-regulating Sirtuin 1 and peroxisome proliferator-activated receptor gamma coactivator 1-α, thereby improving skeletal muscle and mitochondrial function [19]. Additionally, in LPS-stimulated J774.1 mice macrophages, UA has been found to inhibit pro-inflammatory M1 macrophage polarization and the subsequent release of pro-inflammatory cytokines by increasing autophagy flux which prevents nuclear translocation and activation of the AKT/mTOR signaling pathway [20]. This study marks the first to demonstrate that UA enhances mitochondrial function through mitophagy activation, suppresses inflammation, and delays functional deterioration in Cu-exposed SOD1G93A mice. These findings offer crucial insights into ALS mechanisms and pave the way for novel ALS treatment approaches.
Conclusion
Cu exposure in SOD1G93A mice led to impaired motor function, increased muscle atrophy, and motor neuron loss, primarily mediated by disrupted mitophagy. The detrimental effects were mitigated by UA, a mitophagy activator. This suggests that UA administration holds promise as a potential treatment strategy for ALS (Fig. S4).
Data Availability
The mass spectrometry proteomics data have been deposited to the ProteomeXchange Consortium (http://proteomecentral.proteomexchange.org) via the iProX partner repository with the dataset identifier PXD039728.
Abbreviations
- ALS:
-
Amyotrophic lateral sclerosis
- Cu:
-
Copper
- UA:
-
Urolithin A
- ATP:
-
Adenosine triphosphate
- MDA:
-
Malondialdehyde
- MT:
-
Metallothionein
- DTT:
-
Dithiothreitol
- IAA:
-
Iodoacetamide
- TMT:
-
Tandem Mass Tags
- TEAB:
-
Triethyl Ammonium Bicarbonate
- FA:
-
Formic Acid
- HPLC:
-
High-performance liquid chromatography
- PPI:
-
Protein-protein interaction
References
Perera ND, Sheean RK, Lau CL et al (2018) Rilmenidine promotes MTOR-independent autophagy in the mutant SOD1 mouse model of amyotrophic lateral sclerosis without slowing disease progression. Autophagy 14:534–551
Talbott EO, Malek AM, Lacomis D (2016) The epidemiology of amyotrophic lateral sclerosis. Handb Clin Neurol 138:225–238
Pasinelli P, Brown RH (2006) Molecular biology of amyotrophic lateral sclerosis: insights from genetics. Nat Rev Neurosci 7:710–723
Anastasiou E, Lorentz KO, Stein GJ et al (2014) Prehistoric schistosomiasis parasite found in the Middle East. Lancet Infect Dis 14:553–554
Savelieff MG, Nam G, Kang J et al (2019) Development of Multifunctional Molecules as Potential Therapeutic Candidates for Alzheimer’s Disease, Parkinson’s Disease, and Amyotrophic Lateral Sclerosis in the Last Decade. Chem Rev 119:1221–1322
Tak YJ, Park JH, Rhim H et al (2020) ALS-Related Mutant SOD1 Aggregates Interfere with Mitophagy by Sequestering the Autophagy Receptor Optineurin. Int J Mol Sci 21(20):7525
Coelho FC, Squitti R, Ventriglia M et al (2020) Agricultural Use of Copper and Its Link to Alzheimer’s Disease. Biomolecules 10(6):897
Barceloux DG (1999) Copper. J Toxicol Clin Toxicol 37:217–230
Collins JF (2021) Copper nutrition and biochemistry and human (patho)physiology. Adv Food Nutr Res 96:311–364
Antonioni A, Govoni V, Brancaleoni L et al (2023) Amyotrophic Lateral Sclerosis and Air Pollutants in the Province of Ferrara. An Ecological Study. Int J Environ Res Public Health, Northern Italy, p 20
Jang DG; Dou J; Koubek EJ, et al (2024) Metal mixtures associate with higher amyotrophic lateral sclerosis risk and mortality independent of genetic risk and correlate to self-reported exposures: a case-control study. medRxiv
Tokuda E, Okawa E, Ono S (2009) Dysregulation of intracellular copper trafficking pathway in a mouse model of mutant copper/zinc superoxide dismutase-linked familial amyotrophic lateral sclerosis. J Neurochem 111:181–191
Tokuda E, Okawa E, Watanabe S et al (2013) Dysregulation of intracellular copper homeostasis is common to transgenic mice expressing human mutant superoxide dismutase-1s regardless of their copper-binding abilities. Neurobiol Dis 54:308–319
Tsvetkov P, Coy S, Petrova B et al (2022) Copper induces cell death by targeting lipoylated TCA cycle proteins. Science 375:1254–1261
Hilton JBW, Kysenius K, Liddell JR et al (2024) Evidence for disrupted copper availability in human spinal cord supports Cu(II)(atsm) as a treatment option for sporadic cases of ALS. Sci Rep 14:5929
Gong YH, Elliott JL (2000) Metallothionein expression is altered in a transgenic murine model of familial amyotrophic lateral sclerosis. Exp Neurol 162:27–36
Johnson J, Mercado-Ayon E, Mercado-Ayon Y et al (2021) Mitochondrial dysfunction in the development and progression of neurodegenerative diseases. Arch Biochem Biophys 702:108698
Chan DC (2006) Mitochondria: dynamic organelles in disease, aging, and development. Cell 125:1241–1252
Ghosh N, Das A, Biswas N et al (2020) Urolithin A augments angiogenic pathways in skeletal muscle by bolstering NAD(+) and SIRT1. Sci Rep 10:20184
Boakye YD, Groyer L, Heiss EH (2018) An increased autophagic flux contributes to the anti-inflammatory potential of urolithin A in macrophages. Biochim Biophys Acta Gen Subj 1862:61–70
Singh I, Sagare AP, Coma M et al (2013) Low levels of copper disrupt brain amyloid-β homeostasis by altering its production and clearance. Proc Natl Acad Sci U S A 110:14771–14776
Ferrazzo S, Gunduz-Cinar O, Stefanova N et al (2019) Increased anxiety-like behavior following circuit-specific catecholamine denervation in mice. Neurobiol Dis 125:55–66
Shiotsuki H, Yoshimi K, Shimo Y et al (2010) A rotarod test for evaluation of motor skill learning. J Neurosci Methods 189:180–185
Takeshita H, Yamamoto K, Nozato S et al (2017) Modified forelimb grip strength test detects aging-associated physiological decline in skeletal muscle function in male mice. Sci Rep 7:42323
Hampton TG, Amende I (2010) Treadmill gait analysis characterizes gait alterations in Parkinson’s disease and amyotrophic lateral sclerosis mouse models. J Mot Behav 42:1–4
Xu B, Zheng C, Chen X et al (2019) Dysregulation of Myosin Complex and Striated Muscle Contraction Pathway in the Brains of ALS-SOD1 Model Mice. ACS Chem Neurosci 10:2408–2417
Chen C, Jiang X, Li Y et al (2019) Low-dose oral copper treatment changes the hippocampal phosphoproteomic profile and perturbs mitochondrial function in a mouse model of Alzheimer’s disease. Free Radic Biol Med 135:144–156
Chen K, Zhang Q, Wang J et al (2009) Taurine protects transformed rat retinal ganglion cells from hypoxia-induced apoptosis by preventing mitochondrial dysfunction. Brain Res 1279:131–138
Scaricamazza S, Salvatori I, Ferri A et al (2021) Skeletal muscle in ALS: an unappreciated therapeutic opportunity? Cells 10(3):525
Ryu D, Mouchiroud L, Andreux PA et al (2016) Urolithin A induces mitophagy and prolongs lifespan in C. elegans and increases muscle function in rodents. Nat Med 22:879–88
Kiernan MC, Vucic S, Cheah BC et al (2011) Amyotrophic lateral sclerosis. Lancet 377:942–955
Tarnacka B, Jopowicz A, Maślińska M (2021) Copper, Iron, and Manganese Toxicity in Neuropsychiatric Conditions. Int J Mol Sci 22(15):7820
Pereira TC, Campos MM, Bogo MR (2016) Copper toxicology, oxidative stress and inflammation using zebrafish as experimental model. J Appl Toxicol 36:876–885
Caga J, Hsieh S, Lillo P et al (2019) The Impact of Cognitive and Behavioral Symptoms on ALS Patients and Their Caregivers. Front Neurol 10:192
Qin X, Wu P, Wen T et al (2022) Comparative assessment of blood Metal/metalloid levels, clinical heterogeneity, and disease severity in amyotrophic lateral sclerosis patients. Neurotoxicology 89:12–19
Borthwick GM, Johnson MA, Ince PG et al (1999) Mitochondrial enzyme activity in amyotrophic lateral sclerosis: implications for the role of mitochondria in neuronal cell death. Ann Neurol 46:787–790
Fujita K, Yamauchi M, Shibayama K et al (1996) Decreased cytochrome c oxidase activity but unchanged superoxide dismutase and glutathione peroxidase activities in the spinal cords of patients with amyotrophic lateral sclerosis. J Neurosci Res 45:276–281
Wiedemann FR, Manfredi G, Mawrin C et al (2002) Mitochondrial DNA and respiratory chain function in spinal cords of ALS patients. J Neurochem 80:616–625
Swerdlow RH, Parks JK, Cassarino DS et al (1998) Mitochondria in sporadic amyotrophic lateral sclerosis. Exp Neurol 153:135–142
Sandoval H, Thiagarajan P, Dasgupta SK et al (2008) Essential role for Nix in autophagic maturation of erythroid cells. Nature 454:232–235
Lou G, Palikaras K, Lautrup S et al (2020) Mitophagy and Neuroprotection. Trends Mol Med 26:8–20
Li A, Gao M, Liu B et al (2022) Mitochondrial autophagy: molecular mechanisms and implications for cardiovascular disease. Cell Death Dis 13:444
Kang Z, Qiao N, Liu G et al (2019) Copper-induced apoptosis and autophagy through oxidative stress-mediated mitochondrial dysfunction in male germ cells. Toxicol In Vitro 61:104639
Pantoom S, Pomorski A, Huth K et al (2021) Direct Interaction of ATP7B and LC3B Proteins Suggests a Cooperative Role of Copper Transportation and Autophagy. Cells 10(11):3118
Yu W, Liao J, Yang F et al (2021) Chronic tribasic copper chloride exposure induces rat liver damage by disrupting the mitophagy and apoptosis pathways. Ecotoxicol Environ Saf 212:111968
Prinz M, Priller J (2017) The role of peripheral immune cells in the CNS in steady state and disease. Nat Neurosci 20:136–144
Ziff OJ, Clarke BE, Taha DM et al (2022) Meta-analysis of human and mouse ALS astrocytes reveals multi-omic signatures of inflammatory reactive states. Genome Res 32:71–84
Frakes AE, Ferraiuolo L, Haidet-Phillips AM et al (2014) Microglia induce motor neuron death via the classical NF-κB pathway in amyotrophic lateral sclerosis. Neuron 81:1009–1023
D’Amico D, Andreux PA, Valdés P et al (2021) Impact of the Natural Compound Urolithin A on Health, Disease, and Aging. Trends Mol Med 27:687–699
Ma J, Chen T, Wu S et al (2019) iProX: an integrated proteome resource. Nucleic Acids Res 47:D1211-d1217
Chen T, Ma J, Liu Y et al (2022) iProX in 2021: connecting proteomics data sharing with big data. Nucleic Acids Res 50:D1522-d1527
Funding
This study was supported in parts by grants from NSFC (82171583); The Key Basic Research Program of Shenzhen Science and Technology Innovation Commission (JCYJ20200109150717745; JCYJ20200109144418639); Shenzhen Key Medical Discipline Construction Fund (SZXK069), Sanming Project of Medicine in Shenzhen (SZSM201611090); Study on Photothermal tumor Vaccine, Shenzhen Science and Technology Innovation Commission (JCYJ20200109120205924).
Author information
Authors and Affiliations
Contributions
L.Z., X.Y. and Z.Z. designed the experiments. H.Z. and C.G. conducted the study. H.Z. and D.Y. wrote the manuscript. L.N. and K.H. revised the manuscript. C.C., S.L. and G.H. contributed to the animal experiment. L.Z., X.H., D.W., J.L., Z.H. and W.L. contributed to literature search, data collection, analysis, and interpretation. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
All animal experiments comply with the ARRIVE guidelines and should be carried out in accordance with the U.K. Animals (Scientific Procedures) Act, 1986 and associated guidelines, EU Directive 2010/63/EU for animal experiments, or the National Institutes of Health guide for the care and use of Laboratory animals (NIH Publications No. 8023, revised 1978). All efforts were made to minimize animal suffering, to reduce the number of animals used, and to utilize alternatives to in vivo techniques, if available. Moreover, Institutional Animal Care and Use/Ethics Committee, Shenzhen Center for Disease Control and Prevention approved the animal experiments (Approval NO: 2023007, Approval date: Mar.16.2023).
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Consent to Publish
The content of the manuscript is confirmed to have obtained the publication consent of all participants.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhang, H., Gao, C., Yang, D. et al. Urolithin a Improves Motor Dysfunction Induced by Copper Exposure in SOD1G93A Transgenic Mice Via Activation of Mitophagy. Mol Neurobiol (2024). https://doi.org/10.1007/s12035-024-04473-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12035-024-04473-1