Abstract
Neurological diseases can be broadly divided according to causal factors into circulatory system disorders leading to ischemic stroke; degeneration of the nerve cells leading to neurodegenerative diseases, such as Alzheimer’s (AD) and Parkinson’s (PD) diseases, and immune system disorders; bioelectric activity (epileptic) problems; and genetically determined conditions as well as viral and bacterial infections developing inflammation. Regardless of the cause of neurological diseases, they are usually accompanied by disturbances of the central energy in a completely unexplained mechanism. The brain makes up only 2% of the human body’s weight; however, while working, it uses as much as 20% of the energy obtained by the body. The energy requirements of the brain are very high, and regulatory mechanisms in the brain operate to ensure adequate neuronal activity. Therefore, an understanding of neuroenergetics is rapidly evolving from a “neurocentric” view to a more integrated picture involving cooperativity between structural and molecular factors in the central nervous system. This article reviewed selected molecular biomarkers of oxidative stress and energy metabolism disorders such as homocysteine, DNA damage such as 8-oxo2dG, genetic variants, and antioxidants such as glutathione in selected neurological diseases including ischemic stroke, AD, PD, and epilepsy. This review summarizes our and others’ recent research on oxidative stress in neurological disorders. In the future, the diagnosis and treatment of neurological diseases may be substantially improved by identifying specific early markers of metabolic and energy disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
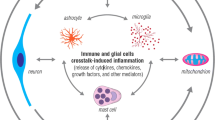
The brain makes up 2% of the average person’s weight. Nevertheless, while working, it uses as much as 20% of the energy obtained by the body [1]. The brain is responsible for a large proportion of the brain’s oxygen consumption [2, 3]. It is estimated that neural signaling accounts for about 75% of cortical energy consumption, while the remaining 25% is used to maintain other functions. Out of the 75%, 44% is used for synaptic transmission and 16% for action potentials [3]. The source of energy for the work of the brain is mostly exclusively glucose [4]; Lundgaard et al. [5] have shown that neurons, and not astrocytes, during rest as well as neural activity, are the primary consumers of glucose (Fig. 1, Table 1).
Mitochondria are essential sources of energy for the brain [6]. These organelles convert energy to adenosine triphosphate (ATP), which neurons need to regulate, among other neurotransmissions [1]. Moreover, ATP plays a crucial role in processes related to maintaining neuronal plasticity [7, 8]. Mitochondria are not only the main energy producers in cells but also the main source of reactive oxygen species (ROS). They generate ROS in oxidative phosphorylation, which is also their major source. ROS leads to damage to macromolecular compounds and metabolic disturbance. Free lipid radicals (lipid peroxides) are formed during lipid oxidation and trigger a destructive chain reaction. They are included in the body due to metabolic reactions, especially in burning polyunsaturated fatty acids, leading to damage to the cell membrane. As a result of damage to the cell membrane, the cell cannot perform its proper metabolic functions, leading to the development of functional disorders in the brain and other organs [9,10,11].
Excitotoxicity and disrupted energy metabolism are significant events leading to nerve cell death in neurodegenerative disorders. These cooperative pathways share one common aspect: triggering oxidative stress by ROS formation. The following oxidative stress markers (8-oxo-2-deoxyguanine, 8-oxo2dG; homocysteine, Hcy; sirtuin 1, SIRT1; short-chain fatty acids, SCFA; others described in the review) could be of interest while studying central nervous system (CNS) diseases.
Oxidative damage is assessed by analyzing lipid peroxidation, mitochondrial dysfunction, and DNA damage. The biomarkers of DNA oxidative damage include 8-oxo2dG [12,13,14,15]. 8-Oxo2dG is the product of the oxidation of guanine in DNA. This oxidative change results in G-C transversion to T-A [16,17,18]. The presence of 8-oxo2dG in nucleic acid during replication may lead to somatic and gene function loss in up to 14% of events, followed by the production of non-functional proteins, including abnormal DNA repair enzymes [19].
Elevated levels of 8-oxo2dG have been demonstrated in the brain and lymphocytes of Alzheimer’s disease (AD) [13, 14] and Parkinson’s disease (PD) [12] patients. At the same time, it has been shown that an increased level of this marker may indicate a gradual increase in damage to nucleic acids and the development of neurodegeneration. Studies by Dorszewska et al. [15] and Dezor et al. [13] have shown that the elevated level of 8-oxo2dG indicates not only the severity of AD dementia (on the Mini–Mental State Examination; MMSE scale) but also the effectiveness of DNA damage repair. Moreover, Dorszewska et al. [14] showed that the repair process of 8-oxo2dG involves three OGG1 isoforms, 1a, 1b, and 1c, and that OGG1-1c most likely plays the role of a compensatory system in the initial phase of the ongoing degenerative process in AD. On the other hand, the polymorphism of the OGG1 Ser326Cys gene is related to the pathogenesis of this dementia through the control of DNA oxidative modification.
Another biomarker involved in regulating mitochondrial functions, stabilizing the chromatin structure, and promoting the DNA repair process, is SIRT1. It is a deacetylase responsible for mitochondrial biogenesis, glucose metabolism, inflammation, and gene transcription. SIRT1 is encoded by the SIRT1 gene, whose polymorphisms are related to physiological aging and neurodegenerative diseases. The role of the rs7895833 polymorphism in increased life expectancy has also been proposed since the AG genotype is associated with higher levels of SIRT1 and lower body weight obesity index [20, 21].
Microbiota is also involved in energy regulation in the brain; it suggests that microbial metabolites influence its functioning. These include SCFA with butyric acid. Butyrate is considered the regulator of microbe levels in the body and is involved in energy metabolism and the control of immune function. Butyrate affects multiple host physiological processes via specific transporters and receptors and as a histone deacetylases (HDAC) inhibitor. It promotes histone acetylation and stimulation of gene expression. Receptors such as GPR43/FFAR2, GPR41/FFAR3, and GPR109a/HCAR2 and transporters including MCT1/SLC16A1 and SMCT1/SLC5A8 are important for its operations [22, 23].
Butyric acid may be involved with other SCFAs such as acetate, propionate, acetoacetate, and d-β-hydroxybutyrate in the pathogenesis of many diseases, including those of a neurological type (e.g., AD) and diabetes, arrhythmogenic cardiomyopathy. Butyrate as an experimental drug has been used in experimental models of neurological disorders, from depression to neurodegenerative diseases of old age [23].
Disruption of bioenergetics may correlate with physiological aging [9,10,11] and age-related diseases, including AD (see the section entitled “Energy Changes in Alzheimer’s Disease”), PD (see the section entitled “Energy Disorders in Parkinson’s Disease”), stroke, and epilepsy [12, 24, 25].
Moreover, the interaction between oxidative stress and neuro-inflammation leads to β-amyloid (Aβ) generation in the brain of AD patients, while PD is the accumulation of degradation of dopaminergic neurons in the substantia nigra, due to the greater susceptibility of the nigrostriatal circuit to mitochondrial dysfunction and oxidative stress. Additionally, mitochondrial complex I activity, which is reduced in PD and is critical to dopaminergic neuron survival, is compromised when glutathione (GSH) levels are reduced in combination with the generation of peroxynitrite radicals. Administration of levodopa (L-dopa) to PD patients, especially long-time therapy, may cause side effects in the form of increased neurotoxicity. The augmented oxidative stress in patients treated with L-dopa may result from lowered levels of GSH and excessive oxidation of dopamine (DA) [12].
GSH in mitochondria (MtGSH) is an alternative pool for cytoplasmic GSH, and its disturbance may lead to the overproduction of ROS, mitochondrial failure, release of caspases, inducers of apoptosis, and the development of dementia. Moreover, during several neurodegenerative diseases, including AD, the level of GSH decreases. GSH has been proposed as a biomarker for diagnosing neurodegenerative diseases and a promising target for future therapies.
Another biothiol involved in the pathogenesis of AD and PD is excessive levels of Hcy [15, 26]. Hcy, a sulfur amino acid, is an intermediate metabolite of methionine. Elevated plasma Hcy level (hyperhomocysteinemia) may cause atherosclerotic vascular and neurodegenerative diseases such as AD and PD. Mild hyperhomocysteinemia is quite prevalent in the general population. It can be caused by genetic defects in the enzymes involved in Hcy metabolism, nutritional deficiencies in vitamin cofactors, certain medications, or renal disease. In the body, Hcy undergoes transsulfuration and transmethylation. Under physiological conditions, about 50% of Hcy is catabolized by transsulfuration to cysteine (Cys), and the remaining 50% of this biomarker is methylated to methionine (Met) [15] (see the chapter entitled “Stroke and energy disorders”).
Another neurological disorder in which biothiols are disturbed is ischemic stroke. In the brain, ischemic stroke is caused by the blockage or rupture of blood vessels. It leads to a disturbance of cerebral blood flow and reduced energy supply to neurons and other brain cells, ultimately resulting in the loss of neurons [27]. Other markers important for the pathogenesis of ischemic stroke are changes in the level of neurotransmitters stimulating, e.g., glutamate and aspartate, and the accompanying release of calcium ions and generation of oxidative stress [28]. Oxidative stress after experimental ischemia violates the integrity of the genome, causes DNA damage and death of neurons and glial and vascular cells, and may lead to the development of neurodegenerative diseases [29, 30]. Moreover, the effects of ischemic changes may have a long-term impact on central structures involving inflammatory factors and be associated with the formation of amyloid plaques and Alzheimer’s-type dementia [31, 32]. More information indicates that disorders in the microbiota-gut-brain axis, manifesting with age and the onset of ischemic stroke, may be associated with the development of risk factors for stroke [33]. Approximately 3% of patients with stroke develop epilepsy [34].
Seizures are the result of a sudden and temporary synchronization of neural activity. It is believed that astrocytes are involved in neurotransmitter storage as well as neurotransmission activity and are responsible for providing neurons with a high energy level to maintain regular and pathological activity, e.g., during an epileptic episode. Moreover, glial cells, especially astrocytes, are involved in neurotransmission through their effects on the transmission of neurons and synapses. The cause of the seizures results from an imbalance between the activity of excitatory and inhibitory neurons, especially between the glutamatergic and gamma-aminobutyric acid (GABAergic) systems. The imbalance between them may be the cause of abnormal bioelectric brain activity. Restoring the balance between excitatory and inhibitory neurons, including relevant pharmacotherapy, may lead to correct neurotransmission in the brain [25].
Emerging energy disorders in neurological diseases, due to the structural and functional complexity of the nervous system, make it necessary to monitor external and internal factors such as energy failure in mitochondria and cytosol, antioxidant status, and response to DNA damage [35, 36].
Energy disturbances in the brain can also be related to genetic or environmental factors such as stress, inappropriate diet, and exposure to toxins [4, 37].
Understanding the brain’s precise and complex energy mechanisms is crucial to discriminate between physiological and pathological processes and will allow indicating more precise disease biomarkers of neurological diseases.
Methodology
The articles selected for the following review have been chosen based on multiple searches through public databases (PubMed, Scopus, Google Scholar, Embase) with the following criteria: “oxidative stress” + “molecular factors” + “ischemic stroke” (242 articles found and 49 results at Embase) and “oxidative stress” + “molecular factors” + “Alzheimer’s” (1134 articles found and 30 results at Embase) and “oxidative stress” + “molecular factors” + “Parkinson’s” (827 articles found and 28 results at Embase) and “oxidative stress” + “molecular factors” + “epilepsy” (101 articles found and 15 results at Embase). Additional papers have been selected based on a search through the references of eligible articles. The last search was performed in August 2022.
The authors’ own research on the subject was also used.
The Role of Homocysteine and Its Metabolism in Stroke
According to the World Health Organization, stroke is the “incoming epidemic of the twenty-first century” [38]. In the past decade, the definition of stroke has been revised and is now defined as an episode of acute neurological dysfunction presumed to be caused by ischemia or hemorrhage, persisting for more than 24 h or leading to earlier death with no apparent cause other than vascular origin [39]. Stroke is the second leading cause of death and disability worldwide, accounting 2017 for 11% of women and 10% of men, while metabolic syndrome (Met/Syn) increases the risk of ischemic stroke [40]. Reaven and co-workers [41] systematically described and defined Met/Syn, which included hyperglycemia, abdominal obesity, hypertriglyceridemia, low high-density lipoprotein cholesterol concentration, hypertension, and interactions between genetic factors, sedentary lifestyle, and diet. Met/Syn is a result of risk factors of metabolic origin that are accompanied by increased risk for cardiovascular disease (consisting of atherogenic dyslipidemia, a prothrombotic state, a pro-inflammatory state, elevated blood pressure, and high-fasting glucose levels of either pre-diabetes or diabetes [42,43,44], obesity, and insulin resistance).
Studies into the traditional risk factors such as metabolic syndrome, smoking, and diets have found that Hcy is an independent risk factor for cerebrovascular diseases (Fig. 2). Hcy is a sulfhydryl-containing amino acid and is an important intermediate product of methionine and Cys metabolism. The concentration of Hcy blood (reference values 5–15 mol/l) should not exceed 14 mol/l on an empty stomach and 30 to 38 mol/l after 6 h from methionine loading. Genetic and nutritional factors, estrogen levels, and age affect the Hcy plasma level [45,46,47]. Subsequently, the predominant metabolism of Hcy occurs via three pathways as a remethylation cycle back to Met by methionine synthase (MS). Tetrahydrofolate metabolism provides a methyl group, and Hcy is remethylated to Met with the assistance of vitamin B12 (VitB12) [48] under the action of methionine adenosyltransferase (MAT). Met is metabolized to S-adenosine methionine (SAM), and SAM is one of the major methyl donors that can be converted to S-adenosine homocysteine (SAH), a methyl removed in this process, which is involved in epigenetic modifications under the action of methyltransferase [49]. SAH removes adenosine by S-adenosine homocysteine hydrolase (SAHH) to form Hcy [50], and these substances are well-associated with the Met cycle and energy metabolism. The second one is known as the transsulfuration pathway or transsulfuration to Cys with vitamin B6 (VitB6) as a coenzyme, whereby Hcy and serine are condensed into cystathionine under the catalysis of cystathionine β-synthase (CBS), followed by cystathionine catalyzed by γ-cystathionine lyase to produce Cys, that is oxidized to sulfate after a series of enzyme catalyzes, and excreted through the urine in the form of inorganic salts [47]. The third one is immediate release into the extracellular fluid; excessive Hcy is thought to be released from the intracellular to the extracellular fluid through the difference in internal and external concentrations and then exported to the systemic circulation to prevent its intracellular accumulation [48, 51]. VitB6, VitB12, and folic acid are involved in the metabolic pathways of Hcy in the methylation and transsulfuration cycle, the lack of which leads to the production of Hcy. Hence, the production and metabolic balance of Hcy are essential for maintaining the body’s homeostasis. Hcy causes platelet adhesion [52] and aggregation, injures tissue endothelial cells, and affects thrombin regulatory protein activity by inhibiting the binding of endothelial cells and tissue-type plasminogen activator [53, 54]. Studies suggest that Hcy induces hypertension by promoting toll-like receptor 4 (TLR-4-driven) chronic vascular inflammation and mitochondria-mediated cell death [55]. Hcy can activate the apoptosis program in nerve cells, inhibit cell membrane sodium/potassium enzyme, induce neuronal metabolic dysfunction [56, 57], and promote the occurrence of acute ischemic stroke [58]. Hcy aggravates atherosclerosis with elevated oxidative stress and reduces S-nitrosylation levels of redox-sensitive protein residues in the vasculature [59]. High levels of Hcy in the blood have a toxic effect on the endothelium of blood vessels and are associated with an increased risk of neurodegenerative processes [60]. Hyperhomocysteinemia activates the enzyme asymmetric dimethylarginine (ADMA). ADMA is an inhibitor of the endothelial isoform of nitric oxide synthase (eNOS), and a reduction in eNOS activity results in a decrease in nitric oxide (NO) concentration (decreasing NO concentration leads to disturbance of the balance between vasodilating abilities in favor of vasoconstriction capacity), which impairs the vasodilating capacity of vascular endothelial cells [61,62,63]. Hyperhomocysteinemia leads to impaired hemostasis resulting in the formation of blood clots in the blood vessel walls [64]. Methylenetetrahydrofolate reductase (MTHFR), CBS, and MS are the key enzymes in Hcy metabolism. MTHFR is an enzyme responsible for the remethylation of Hcy to Met, lowering the Hcy concentration. Studies have revealed that polymorphisms affecting the activity of this enzyme may occur within the MTHFR gene [65, 66]. Missense mutations change the amino acid structure of MTHFR and cause the enzyme N5-N10-methyltetrahydrofolate to be formed, characterized by reduced activity that promotes the development of hyperhomocysteinemia [67,68,69]. Hcy cannot be converted into methionine normally, causing a significant increase in the Hcy content in the blood, which—on the other hand—increases stroke susceptibility [70]. Studies reveal that the heterozygous mutation frequency of MTHFR C677T is higher than that reported in the Chinese population [71, 72], while the homozygous mutation frequency of MTHFR C677T in the Chinese population [73, 74] is the same as reported in non-Chinese. In Caucasian and African populations, Kumar et al. [75] conducted a meta-analysis that indicated that genotyping of the MTHFR gene A1298C polymorphism may be used as a predictor for the occurrence of ischemic stroke; it also resolved the correlation between MTHFR A1298C polymorphism and stroke susceptibility. It was discovered that MTHFR A1298C polymorphism was correlated with stroke in adults. However, the correlation between MTHFR A1298C polymorphism and stroke in children lacked corresponding evidence [76]. A study by Dong et al. [77] indicated that the MTHFR gene could encode the MTHFR enzyme, which plays a crucial role in regulating cellular Hcy and folate metabolism by catalyzing the conversion of 5,10-methylpentylenetetrahydrofolate to 5-methyltetrahydrofolate, and an elevated Hcy level in blood circulation is considered an independent risk factor for cerebral, coronary, and peripheral atherosclerosis [78]. The mutation frequency of CBS 844ins68 and MS A2756G plays an important role in the synthesis and metabolism of Hcy; in Chinese people, the mutation frequency of MS A2756G in the Chinese population was significantly lower than that in Caucasians [71]. A domestic meta-analysis [79] provided evidence that CBS T833C genetic polymorphism was associated with the risk of stroke. Nevertheless, the results from subgroups of the Chinese and Caucasian populations are different; in the Chinese subgroup, the results showed that CBS T833C polymorphism leads to increased incidences of stroke. The findings of several other studies suggest that a 3 mmol/L lower total Hcy level could be associated with a 10% lower risk of recurrent strokes [80,81,82]. Accordingly, clarifying the correlation between Hcy and ischemic stroke and reducing Hcy levels in at-risk patients may play a role in preventing ischemia. Many studies have shown that Hcy is closely correlated with ischemic stroke, especially in the small-vessel occlusion (SVO) and large-artery atherosclerosis (LAA) subtypes [83, 84]. However, some studies have indicated that Hcy is only related to LAA [85].
The precise mechanism of Hcy on the susceptibility of ischemic stroke remains unclear. Most studies of high Hcy levels as a cause of ischemic stroke have found that Hcy generates oxidative stress, damages endothelial cells, and increases fibrinogen production [86, 87]. Moreover, oxidative stress plays an essential role in acute ischemic stroke pathogenesis. Ozkul et al. [88] measured serum levels of NO, malondialdehyde (MDA), and GSH within the first 48 h of stroke in 70 patients and found them significantly higher in acute stroke patients. On the other hand, they did not find a statistically significant correlation between GSH levels and the malfunction of the CNS.
There is possibly a deleterious effect of oxidative stress on clinical outcomes in acute ischemic stroke, and the elevation of GSH levels may be an adaptive mechanism during these occurrences.
Energy Changes in Alzheimer's Disease
The elongation of human survival accompanied significant progress in medicine and technique in the second half of the twentieth century. The elderly population in most modern economics implicates an array of factors contributing to age-related diseases, the most notable of which are epigenetic changes, inflammation, telomere shortening, and mitochondrial abnormalities [89,90,91]. Therefore, the problem of neurodegenerative disorders is becoming considerably more pressing. One of the most common neurodegenerative disorders is AD, the main cause of the severe decline of cognitive functions. Approximately once every minute, a US citizen is diagnosed with AD [92]. Statistical analysis shows that we might see substantial growth in diagnosed AD patients in the upcoming years, reaching as many as 1 million patients yearly [93,94,95,96]. Moreover, AD-induced cognitive impairment results in a significant decrease in quality of life [97].
Some of the most notable pathological changes ongoing in AD are Aβ plaques and hyperphosphorylated tau protein neurofibrillary tangles [98]. In AD development, oxidative stress plays a substantial role (Fig. 2). Researchers currently perceive protein oxidation, DNA oxidation, and lipid peroxidation as signs of energy disorders taking part in AD pathology [99]. ROS results from the O2 transformation intracellular that occurs in every human body cell [100]. Additionally, a certain balance between ROS production and elimination can be severely disrupted in energy disorders. ROS overproduction in such diseases is more likely to occur, leading to cell metabolism destabilization and oxidative damage to DNA and organelles [101]. Therefore, ROS levels could be one of the potential biomarkers of energy disorders in AD and Perez et al. [102] study showed that it is possible to assess the higher level of ROS in fibroblast samples taken from AD patients. The same cells may be the source of another biomarker, 8-oxoguanine. Its presence could indicate oxidative DNA damage in AD patients [102, 103]. Energy disorders might also stimulate the aggregation of advanced glycation products (AGE). Recent research has pointed to AGE as one of the factors playing a role in AD pathology [104]. Moreover, AGE has been identified in Aβ plaques; thus, AGE might be a future biomarker of AD; however, further research into the pathophysiological influence of AGE on AD is needed [104, 105].
Another emerging biomarker is Hcy. Numerous pathological processes occur in the hyperhomocysteinemic state, especially in the central nervous system. Furthermore, Hcy induces ROS production, mitochondrial imbalance, and lipid peroxidation, contributing to energy disorders [106]. Elevated Hcy concentration in the brain stimulates neurotoxicity and promotes cognitive decline [107]. Moreover, an elevated Hcy level has been associated with increased AD risk and can be correlated with the disease’s severity [107, 108]. All these points favor Hcy being an important AD biomarker; nevertheless, more research is needed [107,108,109,110].
Energy disorders contributing to AD might also originate from disruption in nuclear-encoded oxidative phosphorylation subunits (OXPHOS); as a result, mitochondrial activity is disturbed severely; especially, complex IV seems to be the most affected. This results in a chain of mitochondrial reactions ending in increased production of ROS. Lunnon et al.’s [113] study demonstrated that specific genes are more likely to invoke such a reaction, namely MT-ND1, MT-ND2, MT-ATP6, MT-CO1, MT-CO2, MT-CO3, and MT-ND6. Determining the overexpression of said OXPHOS genes might give some insight into energy disorder-driven AD pathology. Furthermore, OXPHOS genes may be a viable option for an AD biomarker in the future [111,112,113,114,115,116].
Another representative of mitochondria-oriented pathology is cytochrome c oxidase (CO) dysregulation. Among AD patients, the activity of CO is severely impaired [117]. In addition, impaired CO functionality might increase ROS production, leading to a higher chance of oxidative damage. Determining the specific mutations in patients might mean these changes can be another biomarker of energy disorders in AD. Therefore, the energetic disturbance in AD caused by pathological changes in the course of the disease may be the starting point for new therapies in the future.
Energy Disorders in Parkinson’s Disease
PD is the second most prevalent neurodegenerative disorder after AD. Approximately 2% of the population over the age of 65 suffers from PD. Moreover, men are affected 1.5 times more than women [118]. The main symptoms of PD are resting tremor, rigidity, bradykinesia, and postural instability; however, the precise etiology is yet to be defined, although it should be considered a multifactored disease with environmental, genetic, and epigenetic risks. With increasing age, the risk of PD is greater. Pathologically, the disease is characterized by the loss of dopaminergic neurons in the substantia nigra, which leads to decreased DA levels in the basal ganglia and the formation of Lewy bodies (LB). These intracellular formations consist of α-synuclein conglomerates [119]. It is believed that the occurrence of motor symptoms is correlated with dysregulation of the basal ganglia circuitries [120]. Additionally, during PD, there is a tendency toward non-motor symptoms such as sleep disturbances, depression, cognitive deficits, and autonomic and sensory dysfunction [121]. Mostly, PD is sporadic and, as a cause of the occurrence, indicates a correlation between genetic and environmental factors. In 15% of cases, the cause of PD is rare familial genetic mutations. In both forms of PD, mitochondrial dysfunction has been observed [122].
The first case of PD was described over 200 years ago, but even currently, there are no specific diagnostic markers [123]. To recognize PD, the patient must represent the clinical symptoms, including motor and non-motor disorders [124]. Oxidative stress is indicated as one of the main factors responsible for neurodegeneration in PD [125]. ROS are produced in the mitochondrial respiratory chain (Fig. 2). They result from metabolic processes occurring in cells and play an important role in cell defense [126, 127]. The antioxidative mechanisms control the levels of ROS in dopaminergic neurons by including GSH, superoxide dismutase (SOD), and protein deglycase 1 (DJ-1). In patients with PD, more mutations have been described [125]. This statement may confirm that the nigral neurons are harmed by oxidative damage [128]. During aerobic respiration, electrons may escape from complex I (nicotinamide adenine dinucleotide, NADH) and complex III (cytochrome bc1) to generate ROS [129]. This resulting ROS may be converted further into hydrogen peroxide by SOD2 and detoxified by catalase [130]. If these mechanisms are inefficient, the reactive molecules oxidize mitochondrial DNA (mtDNA) [12]. Neuronal damage leading to the presence and progression of PD may be the result of these neuronal abnormalities [128].
Mitochondria need a constant rejuvenation. Maintaining a healthy mitochondrial population requires the clearance of damaged proteins and organelles [131]. The mitochondrial clearance process is provided by mitochondrial quality control (MQC) complexes, including AAA proteases, the ubiquitin–proteasome system, mitochondrial-derived vesicles, and mitophagy [131, 132]. A dual interaction between Parkin and PTEN-induced kinase 1 (PINK1) plays the primary role in activating MQC.
MQC activation disorders increase ROS levels and decrease ATP levels [132]. Translocase of the outer membrane 20 (TOM20) is the main protein involved in the degradation of PINK1, which may further induce mitophagy signals [133]. In the situation of mitochondrial complex insufficiency, proteotoxicity, or membrane depolarization impairment, there is PINK1 aggregation, which causes homodimerization and subsequent autophosphorylation promoting activation of kinase—all of which leads to the bonding of Parkin and ubiquitin. This complex is phosphorylated by PINK1 at Ser65, promoting E3 ligase activity [133, 134]. As a result, more Parkin is connected with ubiquitin conglomerates resulting in a higher rate of mitophagy [133, 135]. The latest studies focus on the autophagy process in neurodegenerative disease, especially in PD, where autophagy is impaired, leading to LB accumulation which cannot be removed by proteasomes [136, 137]. Additionally, the increased ROS level distorts the function of proteasomes and consequently causes the collection of an increased amount of damaged protein in the cells [138]. In dopaminergic neurons, there is a tendency toward higher levels of ROS, resulting in more sensitivity to various stress factors than other neurons.
DA may be metabolized by monoamineoxidase (MAO) [129]. The other pathway involves spontaneous DA oxidation in the presence of iron, generating 6-hydroxydopamine (6-OHDA) quinone. In the presence of oxygen, 6-OHDA is subsequently transformed into a reactive electrophilic molecule, p-quinone. There is also the possibility of oxidizing DA to DA-quinone (DAQ) [127, 139]. DAQ is described as a molecule that affects the cell’s ability to sequester ROS by reacting with Cys-106 of the neuroprotective protein DJ-1 [140, 141]. In dopaminergic neuronal cells, DJ-1 is mostly located in the cytoplasm. During a higher exposure to ROS, it is oxidized to cysteine-sulfinic (Cys-SO2H) and then translocated to the nucleus and the mitochondria [142]. However, DJ-1 has a lower efficiency in removing ROS than other enzymes, which allows us to assume that it may be an oxidative stress sensor by modulating signaling pathways and the expression of specific genes [143]. It has been indicated that the high level of DJ-1 promotes GSH synthesis and, in this way, protects DA neurons from the negative effects of H2O2 [142].
As a result, the change level of ROS causes the binding of DJ-1 to mitochondrial complex I and change the activity of NADH: ubiquinone oxidoreductase and, ultimately, the entire respiratory chain [144]. The disturbances in handling iron, especially in DA neurons, may result in the greatest ROS generation. The most recent studies indicate a correlation between metal ions and α-synuclein, resulting in decreased GSH levels and increased lipid peroxidation, which favors the higher production of H2O2 and hydroxyl radicals [145, 146]. All these abnormalities cause decreased ATP levels and nucleic acid damage. The main product of hydroxyl radicals is 8-oxo2dG [147]. In PD patients, the level of 8-oxo2dG compared to controls was increased in cerebrospinal fluid, serum, and urine [16]. In patients treated with L-dopa during therapy, the levels of 8-oxo2dG and corresponding DNA alterations may fluctuate depending on its duration [148].
Epilepsy and Energy Damage
Epilepsy is one of the most common neurological diseases in the world and affects approximately 1–1.5% of the population; according to data from the World Health Organization, more than 50 million people suffer from it [149]. The prevalence of epilepsy is highest in the age group up to 10 years, especially in the first months of life and after 65 years. It is also more often diagnosed in males and developing countries [150]. However, recent epidemiological studies show that the number of patients with childhood epilepsy is decreasing while the incidence of senile epilepsy is increasing, especially after the age of 75 [151]. In 2017, the International League Against Epilepsy task force published a new, practical definition of epilepsy, thus formulating a slightly different perspective on its diagnosis [152]. According to the latest thinking, epilepsy is a brain disease that can be diagnosed in one of the following three clinical situations: when there are at least two unprovoked (or reflex) seizures that occur at least 24 h apart or when there is one unprovoked (or reflex) seizure and the likelihood of further recurrence is comparable to the overall risk of recurrence (at least 60%), such as after two unprovoked attacks that may occur in the next 10 years, and when an epileptic syndrome can be diagnosed [153].
Epilepsy is a group of symptoms that many factors can cause. According to the latest etiological classification, epilepsy is divided into genetically determined epilepsy (formerly called idiopathic), when the disease is clinically manifested mainly by epileptic seizures and is a direct result of a known or suspected genetic defect (or several mutations), e.g., the SCN1A gene [154]. Another type of epilepsy of structural/metabolic etiology (formerly symptomatic) is a genetically determined or acquired pathological condition that increases the risk of seizures and epilepsy of unknown cause (formerly called cryptogenic) resulting from an unexplained pathological state [153].
At the cellular level, epilepsy is the result of an imbalance between excitatory and inhibitory mechanisms, leading to paroxysmal excitation of cortical neurons. There is no one generally accepted theory of this phenomenon, i.e., epileptogenesis. This term is understood as a process that, after the action of a damaging stimulus, leads to cellular and molecular changes in the brain, resulting in the appearance of spontaneously recurring seizures. Seizures may result from structural or functional brain damage or changes in cellular metabolic pathways [155].
It is believed that metabolic and energy disorders play a crucial role in the pathogenesis of epilepsy (Fig. 2). Excessive neuronal discharges may result from the delivery of an altered energy level. In contrast, energy depletion during a seizure is an endogenous mechanism for ending a seizure. In the control of neural energy homeostasis, astrocytes play an important role via a neurometabolic linkage. Moreover, astrocyte dysfunction in epilepsy changes fundamental metabolic mechanisms. Among the disturbed metabolism associated with the astrocytes, there is, e.g., glutamate turnover, which in these central cells may directly contribute to neuronal hyperactivity. A consequence of astrocyte dysfunction is also a disturbance in the movement of energy metabolites and a disorder in removing ions (potassium) and neurotransmitters (glutamate). Astrocyte dysfunction also increases the metabolism of adenosine, the metabolic degradation product of ATP responsible for inhibiting energy-intensive processes and glucose consumption. The phenomenon of astroglial energy homeostasis in controlling neuronal excitability, related to the prevention of glucose utilization, may serve as a target for the pharmacotherapy of epilepsy [25, 156,157,158].
An essential role in the development of epilepsy attacks is played by disorders of neurotransmitters, especially GABA and glutamate, classified as primary messengers, which play a crucial role in the processes of stimulating and inhibiting neurons [159]. GABA is produced by the decarboxylation of glutamic acid and functions as an inhibitory neurotransmitter in the brain. Glutamate, in turn, responds to stimulation, and it is estimated that it is released in more than half of the synapses of the central nervous system [160]. The hyperactivity of the neuron is believed to result from the imbalance between glutamate stimulation and GABA inhibition [161, 162].
The reasons for the initiation and progression of epilepsy may include an increase in extracellular glutamate concentration, structural changes in the receptors for this substance (e.g., lack of the N-methyl-D-aspartic acid, NMDA NR1 subunit), impaired transport through the membrane (e.g., a reduction in the number of GLAST transporters, glutamate aspartate transporter, and GLT-1, glutamate transporter), and autoimmune mechanisms. Recent studies have shown that the concentration of pro-inflammatory cytokines—interleukins (IL) IL-1β, IL-6, and tumor necrosis factor alpha (TNF-α)—significantly increases in brain regions where epileptogenesis and signal spreading occur [163,164,165].
The treatment strategy for epilepsy patients is based on the long-term administration of antiepileptic drugs (AEDs) [166]. Many studies have shown that AEDs, depending on their type, can modulate the process of apoptosis and increase the concentration of Hcy. A study by Sniezawska et al. [167] showed that patients with epilepsy treated with AEDs changed not only their level of Hcy but also another risk factor for vascular diseases, ADMA, with the participation of genetic variants of genes regulating the level of Hcy, such as MTHFR, MTR, and MTHFD1. It has also been shown that pharmacotherapy of AEDs in patients with epilepsy increases Hcy concentration, especially in patients treated with polytherapy and long-term treatment. In addition, it has been shown that people with the MTHFR CT (C677T) and MTHFD1 GG (G1958A) genotypes seem more susceptible to increased Hcy levels during AED treatment. Moreover, genetic conditions may lead to a disturbance of the ratio between Hcy and Met, arginine and ADMA, and impaired Hcy control over ADMA levels.
On the other hand, Łagan-Jędrzejczyk et al. [168] showed that in epilepsy patients with hyperhomocysteinemia treated with AEDs, the level of factors responsible for the introduction of cells to apoptosis (the ratio of Bax:Bcl-2 proteins) and cells in apoptosis increased, as measured by an increase in the level of cells with active caspase-3 using flow cytometry.
A study by Loi et al. [169] also indicated changes in apoptotic proteins in epilepsy. It showed that cells deficient in cyclin-dependent kinase-like 5 (CDKL5) increased the proapoptotic Bax protein and biomarkers associated with DNA damage (γH2AX, RAD50, and PARP1). Moreover, CDKL5-deficient cells were hypersensitive to stress associated with DNA damage, accumulated more DNA damage foci, and were more susceptible to cell death than the controls [169].
The limitations of the review are as follows:
-
Common neurological diseases are only described in the review.
-
Neurological diseases with neurodegenerative changes were selected.
-
Diseases in which ROS generation is involved in the pathogenesis have been selected.
-
Selected biomarkers of energy disorders are described.
-
Non-selective biomarkers present in various pathologies of the central nervous system have been described.
Conclusion
Although degenerative changes in neurological diseases such as stroke, AD, PD, and epilepsy have different mechanisms of central damage, affect other areas of the brain, and develop different clinical features in patients, they generally lead to an increase in oxidative stress and energy disturbances and the appearance of altered biomarker levels. The levels of factors related to energy disorders are of particular interest, including Hcy, DNA damage in the form of 8-oxo2dG, genetic variants, and antioxidants such as GSH (Table 1). Specific biomarkers are currently sought for neurological diseases related to disease manifestation, progression, and responses to available drug pharmacotherapy.
We believe that by finding specific early markers of metabolic and energy disorders, the diagnosis and treatment of neurological diseases could improve in the near future.
Data Availability
Not applicable.
Abbreviations
- Aβ:
-
β-Amyloid
- AD:
-
Alzheimer’s disease
- ADMA:
-
Asymmetric dimethylarginine
- AEDs:
-
Antiepileptic drugs
- AGE:
-
Glycation products
- ATP:
-
Adenosine triphosphate
- C:
-
Cytosine
- CBS:
-
Cystathionine β-synthase
- CDKL-5:
-
Cyclin-dependent kinase-like 5
- CNS:
-
Central nervous system
- CO:
-
Cytochrome c oxidase
- Cys:
-
Cysteine
- Cys-SO2H:
-
Cysteine-sulfinic
- DA:
-
Dopamine
- DAQ:
-
DA-quinone
- DJ-1:
-
Protein deglycase 1
- DNA:
-
Deoxyribonucleic acid
- eNOS:
-
Endothelial isoform of nitric oxide synthase
- ET-1:
-
Endothelin 1
- GABA:
-
Gamma-aminobutyric acid
- GLAST:
-
Glutamate aspartate transporter
- GLT-1:
-
Glutamate transporter
- GSH:
-
Glutathione
- Hcy:
-
Homocysteine
- HDAC:
-
Histone deacetylases
- IL-1β:
-
Interleukin-1β
- IL-6:
-
Interleukin-IL-6
- LAA:
-
Large-artery atherosclerosis
- LB:
-
Lewy body
- L-CAR:
-
Levocarnitine
- L-dopa:
-
Levodopa
- MAO:
-
Monoamineoxidase
- MAT:
-
Methionine adenosyltransferase
- MDA:
-
Malondialdehyde
- Met:
-
Methionine
- Met/Syn:
-
Metabolic syndrome
- MQC:
-
Mitochondrial quality control
- mtDNA:
-
Mitochondrial DNA
- mtGSH:
-
GSH in mitochondria
- MMSE:
-
Mini–Mental State Examination
- MS:
-
Methionine synthase
- MTHFR:
-
Methylenetetrahydrofolate reductase
- NADH:
-
Nicotinamide adenine dinucleotide
- NMDA:
-
N-Methyl-D-aspartic acid
- NO:
-
Nitric oxide
- 3-NP:
-
3-Nitropropionic acid
- 6-OHDA:
-
6-Hydroxydopamine
- 8-oxo2dG:
-
8-Oxo-2-deoxyguanine
- OXPHOS:
-
Oxidative phosphorylation subunits
- PD:
-
Parkinson’s disease
- PGI2:
-
Prostaglandin G2
- PINK1:
-
PTEN-induced kinase 1
- QUIN:
-
Quinolinic acid (2,3-pyridine dicarboxylic acid)
- ROS:
-
Reactive oxygen species
- SAH:
-
S-Adenosine homocysteine
- SAHH:
-
S-Adenosine homocysteine hydrolase
- SAM:
-
S-Adenosine methionine
- SCFA:
-
Short-chain fatty acids
- SIRT1:
-
Sirtuin 1
- SOD:
-
Superoxide dismutase
- SVO:
-
Small-vessel occlusion
- T:
-
Thymine
- TLR-4:
-
Toll-like receptor 4
- TNF-α:
-
Tumor necrosis factor alpha
- TOM20:
-
Translocase of the outer membrane 20
- TXA2:
-
Thromboxane A2
- VitB6:
-
Vitamin B6
- VitB12:
-
Vitamin B12
References
Joshi AU, Mochly-Rosen D (2018) Mortal engines: mitochondrial bioenergetics and dysfunction in neurodegenerative diseases. Pharmacol Res 138:2–15
Wong-Riley MTT (1989) Cytochrome oxidase: an endogenous metabolic marker for neuronal activity. Trends Neurosci 12(3):94–101
Howarth C, Gleeson P, Attwell D (2012) Updated energy budgets for neural computation in the neocortex and cerebellum. J Cereb Blood Flow Metab 32(7):1222–1232
Gerozissis K (2008) Brain insulin, energy and glucose homeostasis; genes, environment and metabolic pathologies. Eur J Pharmacol 585(1):38–49
Lundgaard I, Li B, Xie L et al (2015) Direct neuronal glucose uptake heralds activity-dependent increases in cerebral metabolism. Nat Commun 6:6807
Grimm A, Eckert A (2017) Brain aging and neurodegeneration: from a mitochondrial point of view. J Neurochem 143(4):418–431
Dorszewska J, Kozubski W, Waleszczyk W, Zabel M, Ong K (2020) Neuroplasticity in the pathology of neurodegenerative diseases. Neural Plast 2020:4245821
Kozubski W, Ong K, Waleszczyk W, Zabel M, Dorszewska J (2021) Molecular factors mediating neural cell plasticity changes in dementia brain diseases. Neural Plast 2021:8834645
Dorszewska J, Adamczewska-Goncerzewicz Z (2004) Oxidative damage to DNA, p53 gene expression and p53 protein level in the process of aging in rat brain. Respir Physiol Neurobiol 139(3):227–236
Dorszewska J, Adamczewska-Goncerzewicz Z, Szczech J (2004) Apoptotic proteins in the course of aging of central nervous system in the rat. Respir Physiol Neurobiol 139(2):145–155
Dorszewska J (2013) Cell biology of normal brain aging: synaptic plasticity-cell death. Aging Clin Exp Res 25(1):25–34
Kowalska M, Piekut T, Prendecki M, Sodel A, Kozubski W, Dorszewska J (2020) Mitochondrial and nuclear DNA oxidative damage in physiological and pathological aging. DNA Cell Biol 39(8):1410–1420
Dezor M, Dorszewska J, Florczak J et al (2011) Expression of 8-oxoguanine DNA glycosylase 1 (OGG1) and the level of p53 and TNF-αlpha proteins in peripheral lymphocytes of patients with Alzheimer’s disease. Folia Neuropathol 49(2):123–131
Dorszewska J, Kempisty B, Jaroszewska-Kolecka J et al (2009) Expression and polymorphisms of gene 8-oxoguanine glycosylase 1 and the level of oxidative DNA damage in peripheral blood lymphocytes of patients with Alzheimer’s disease. DNA Cell Biol 28(11):579–588
Dorszewska J, Florczak J, Rozycka A et al (2007) Oxidative DNA damage and level of thiols as related to polymorphisms of MTHFR, MTR, MTHFD1 in Alzheimer’s and Parkinson’s diseases. Acta Neurobiol Exp (Warsz) 67(2):113–129
Isobe C, Abe T, Terayama Y (2010) Levels of reduced and oxidized coenzymeQ-10 and 8-hydroxy-2′-deoxyguanosine in the cerebrospinal fluid of patients with living Parkinson’s disease demonstrate that mitochondrial oxidative damage and/or oxidative DNA damage contributes to the neurodegenerative process. Neurosci Lett 469(1):159–163
Gmitterová K, Gawinecka J, Heinemann U, Valkovič P, Zerr I (2018) DNA versus RNA oxidation in Parkinson’s disease: which is more important? Neurosci Lett 662:22–28
Popov AV, Yudkina AV, Vorobjev YN, Zharkov DO (2020) Catalytically Competent Conformation of the active site of human 8-oxoguanine-DNA glycosylase. Biochemistry (Mosc) 85(2):192–204
Yasui M, Kanemaru Y, Kamoshita N, Suzuki T, Arakawa T, Honma M (2014) Tracing the fates of site-specifically introduced DNA adducts in the human genome. DNA Repair 15:11–20
Zillikens MC, van Meurs JBJ, Rivadeneira F et al (2009) SIRT1 genetic variation is related to BMI and risk of obesity. Diabetes 58(12):2828–2834
Kilic U, Gok O, Erenberk U et al (2015) A Remarkable age-related increase in SIRT1 protein expression against oxidative stress in elderly: SIRT1 gene variants and longevity in human. PLOS ONE 10:e0117954
Piekut T, Hurła M, Banaszek N, Szejn P, Dorszewska J, Kozubski W (2022) Infectious agents and Alzheimer’s disease. J Integr Neurosci 21(2):73
Stilling RM, van de Wouw M, Clarke G, Stanton C, Dinan TG, Cryan JF (2016) The neuropharmacology of butyrate: the bread and butter of the microbiota-gut-brain axis? Neurochem Int 99:110–132
Chen Y (2022) Disturbed cerebral circulation and metabolism matters: a preface to the special issue “Stroke and Energy Metabolism”: a preface to the special issue “Stroke and Energy Metabolism.” J Neurochem 160(1):10–12
Cloix JF, Hévor T (2009) Epilepsy, regulation of brain energy metabolism and neurotransmission. Curr Med Chem 16(7):841–853
Prendecki M, Kowalska M, Łagan-Jędrzejczyk U et al (2020) Genetic factors related to the immune system in subjects at risk of developing Alzheimer’s disease. J Integr Neurosci 19(2):359–371
Bon LI, Maksimovich NY (2021) Histological disorders of neurons of phylogenetically different parts of the cerebral cortex in partial, subtotal, stepwise subtotal, and total cerebral ischemia. J Med Sci 90(1):108–115
Pluta R, Salínska E, Puka M, Stafiej A, Lazarewicz (1988) Early changes in extracellular amino acids and calcium concentrations in rabbit hippocampus following complete 15-min cerebral ischemia. Resuscitation 16(3):193–210
Pluta R, Kiś J, Januszewski S, Jabłoński M, Czuczwar SJ (2022) Cross-talk between amyloid, Tau protein and free radicals in post-ischemic brain neurodegeneration in the form of Alzheimer’s disease proteinopathy. Antioxidants (Basel) 11(1):146
Pluta R (2022) Brain ischemia as a bridge to Alzheimer’s disease. Neural Regen Res 17(4):791–792
Radenovic L, Nenadic M, Ułamek-Kozioł M et al (2020) Heterogeneity in brain distribution of activated microglia and astrocytes in a rat ischemic model of Alzheimer’s disease after 2 years of survival. Aging (Albany NY) 12(12):12251–12267
Sekeljic V, Bataveljic D, Stamenkovic S et al (2012) Cellular markers of neuroinflammation and neurogenesis after ischemic brain injury in the long-term survival rat model. Brain Struct Funct 217(2):411–420
Pluta R, Jabłoński M, Januszewski S, Czuczwar SJ (2022) Crosstalk between the aging intestinal microflora and the brain in ischemic stroke. Front Aging Neurosci 14:998049
Vercueil L (2007) Seizure and epilepsy after stroke. Presse Med 36(1 Pt 2):176–181
Silva-Adaya D, Pérez-De La Cruz V, Herrera-Mundo MN et al (2008) Excitotoxic damage, disrupted energy metabolism, and oxidative stress in the rat brain: antioxidant and neuroprotective effects of L-carnitine. J Neurochem 105(3):677–689
Niziński J, Kamieniarz L, Filberek P, Sibrecht G, Guzik P (2020) Monitoring the skin NADH changes during ischaemia and reperfusion in humans. J Med Sci 89(1):60–70
Prendecki M, Florczak-Wyspianska J, Kowalska M et al (2018) Biothiols and oxidative stress markers and polymorphisms of TOMM40 and APOC1 genes in Alzheimer’s disease patients. Oncotarget 9(81):35207–35225
Sarikaya H, Ferro J, Arnold M (2015) Stroke prevention–medical and lifestyle measures. Eur Neurol 73(3–4):150–157
Sacco RL, Kasner SE, Broderick JP et al (2013) An updated definition of stroke for the 21st century a statement for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke 44(7):2064–2089
Reaven GM (1988) Banting lecture 1988. Role of insulin resistance in human disease. Diabetes 37(12):1595–1607
No authors listed (1993) Summary of the second report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel II). JAMA 269(23):3015–3023
National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) (2002) Third report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation 106(25):3143–3421
Alberti KGMM, Zimmet P, Shaw J, IDF Epidemiology Task Force Consensus Group (2005) The metabolic syndrome—a new worldwide definition. Lancet 366(9491):1059–1062
Velazquez R, Ferreira E, Winslow W et al (2020) Maternal choline supplementation meliorates Alzheimer’s disease pathology by reducing brain homocysteine levels across multiplegenerations. Mol Psychiatry 25(10):2620–2629
Kalani A, Kamat PK, Givvimani S et al (2014) Nutri-epigenetics ameliorates blood-brain barrier damage and neurodegeneration in hyperhomocysteinemia: role of folic acid. J Mol Neurosci 52(2):202–215
Škovierová H, Vidomanová E, Mahmood S et al (2016) The molecular and cellular effect of homocysteine metabolism imbalance on human health. Int J Mol Sci 17(10):1733
Schalinske KL, Smazal AL (2012) Homocysteine imbalance: a pathological metabolic marker. Adv Nutr 3(6):755–762
Friso S, Choi SW, Girelli D et al (2002) A common mutation in the 5,10 methylenetetrahydrofolate reductase gene affects genomic DNA methylation through an interaction with folate status. Proc Natl Acad Sci USA 99(8):5606–5611
Mentch SJ, Locasale JW (2016) One-carbon metabolism and epigenetics: understanding the specificity. Ann N Y Acad Sci 1363(1):91–98
Hannibal L, Blom HJ (2017) Homocysteine and disease: causal associations or piphenomenons? Mol Aspects Med 53:36–42
Malinowska J, Tomczynska M, Olas B (2012) Changes of blood platelet adhesion to collagen and fibrinogen induced by homocysteine and its thiolactone. Clin Biochem 45(15):1225–1228
McCully KS (2015) Homocysteine metabolism, atherosclerosis, and diseases of aging. Compr Physiol 6(1):471–505
Smith AD, Refsum H (2016) Homocysteine, B vitamins, and cognitive impairment. Annu Rev Nutr 36:211–239
Familtseva A, Chaturvedi P, Kalani A et al (2016) Toll-like receptor 4 mutation suppresses hyperhomocysteinemia induced hypertension. Am J Physiol Cell Physiol 311(4):C596–C606
Mattson MP, Shea TB (2003) Folate and homocysteine metabolism in neural plasticity and neurodegenerative disorders. Trends Neurosci 26(3):137–146
Folstein M, Liu T, Peter I et al (2007) The homocysteine hypothesis of depression. Am J Psychiatry 164(6):861–867
Chen Y, Zou H, Peng M, Chen Y (2022) Association between homocysteine levels in acute stroke and poststroke depression: a systematic review and meta-analysis. Brain Behav 12(6):e2626
Li J, Zhang Y, Zhang Y et al (2018) GSNOR modulates hyperhomocysteinemia-induced T cell activation and atherosclerosis by switching Akt S-nitrosylation to phosphorylation. Redox Biol 17:386–399
Montecinos-Oliva C, Arrázola MS, Jara C, Tapia-Rojas C, Inestrosa NC (2020) Hormetic-like effects of L-homocysteine on synaptic structure, function, and Aβ aggregation. Pharmaceuticals 13(2):24
Do Carmo S, Hanzel CE, Jacobs MJ et al (2016) Rescue of early bace-1 and global DNA demethylation by S adenosylmethionine reduces amyloid pathology and improves cognition in an Alzheimer’s model. Sci Rep 6:34051
Wassef M, Baxter BT, Chisholm RL et al (2001) Pathogenesis of abdom¬inal aortic aneurysms: a multidisciplinary research program sup¬ported by the National Heart, Lung, and Blood Institute. J Vasc Surg 34(4):730–738
Kraczkowska S, Suchocka Z, Pachecki J (2005) Podwyższone stężenie homocysteiny we krwi jako wskaźnik zagrożenia zdrowia. Biul Wydz Farm AMW 3:4–13 (in Polish)
Ukachukwu V, Idris S, McIlwee A (2012) Acute myocardial infarction in a young patient with hyperhomocysteinaemia. BMJ Case Rep 2012:bcr2012007489
Ferrara F, Novo S, Grimaudo S et al (2006) Methylenetetrahydrofolate reductase mutation in subjects with abdominal aortic aneurysm subdivided for age. Clin Hemorheol Microcirc 34(3):421–426
Jakobsche-Policht U, Bednarska-Chabowska D, Sadakierska-Chudy A, Adamiec-Mroczek J (2014) Expression of the PAR-1 protein on the surface of platelets in patients with chronic peripheral arterial insufficiency - preliminary report. Adv Clin Exp Med 23(2):159–167
Pramukarso DT, Faradz SM, Sari S, Hadisaputro S (2015) Association between methylenetetrahydrofolate reductase (MTHFR) polymorphism and carotid intima medial thickness progression in post ischaemic stroke patient. Ann Transl Med 3(21):324
Song Y, Li B, Wang C, Wang P, Gao X, Liu G (2016) Association between 5,10-methylenetetrahydrofolate reductase C677T gene polymorphism and risk of ischemic stroke: a meta-analysis. J Stroke Cerebrovasc Dis 25(3):679–687
Toffoli G, De Mattia E (2008) Pharmacogenetic relevance of MTHFR polymorphisms. Pharmacogenomics 9(9):1195–1206
Zhao M, Wang X, He M et al (2017) Homocysteine and stroke risk: modifying effect of Methylenetetrahydrofolate Reductase C677T polymorphism and folic acid intervention. Stroke 48(5):1183–1190
Zhang T, Jiang Y, Zhang S et al (2020) The association between homocysteine and ischemic stroke subtypes in Chinese. A meta-analysis. Medicine (Baltimore) 99(12):e19467
Cattaneo M (1999) Hyperhomocysteinemia, atherosclerosis and thrombosis. Thromb Haemost 81(2):165–176
Fu S, Luo L, Ye P, Xiao W (2015) Multimarker analysis for new biomarkers in relation to central arterial stiffness and hemodynamics in a Chinese community-dwelling population. Angiology 66(10):950–956
Zhang MJ, Hu ZC, Yin YW et al (2014) A meta-analysis of the relationship between MTHFR gene A1298C polymorphism and the risk of adult stroke. Cerebrovasc Dis 38(6):425–432
Kumar A, Sharma R, Misra S, Nath M, Kumar P (2020) Relationship between methylenetetrahydrofolate reductase (MTHFR) gene (A1298C) polymorphism with the risk of stroke: a systematic review and metaanalysis. Neurol Res 42(11):913–922
Coen Herak DC, Krleza JL, Antolic MR et al (2017) Association of polymorphisms in coagulation factor genes and enzymes of homocysteine metabolism with arterial ischemic stroke in children. Clin Appl Thromb Hemost 8:1042–1051
Dong X, Wang J, Wang G, Wang J, Wang L, Du Y (2021) MTHFR A1298C gene polymorphism on stroke risk: an updated meta-analysis. Genes Environ 43(1):40
Toyoda K, Uwatoko T, Shimada T et al (2004) Recurrent small-artery disease in hyperhomocysteinemia: widowers’ stroke syndrome? Intern Med 43(9):869–872
Ding R, Lin S, Chen D (2012) The association of cystathionine b synthase (CBS) T833C polymorphism and the risk of stroke: a meta-analysis. J Neurol Sci 312(1–2):26–30
Toole JF, Malinow MR, Chambless LE et al (2004) Lowering homocysteine in patients with ischemic stroke to prevent recurrent stroke, myocardial infarction, and death: the vitamin intervention for stroke prevention (VISP) randomized controlled trial. JAMA 291(5):565–575
Wang Q, Zhao J, Chang H, Liu X, Zhu R (2021) Homocysteine and folic acid: risk factors for Alzheimer’s disease—an updated meta-Analysis. Front Aging Neurosci 13:665114
Huang X, Li Y, Li P et al (2017) Association between percent decline in serum total homocysteine and risk of first stroke. Neurology 89(20):2101–2107
Gungor L, Polat M, Ozberk MB, Avci B, Abur U (2018) Which ischemic stroke subtype is associated with hyperhomocysteinemia? J Stroke Cerebrovasc Dis 27(7):1921–1929
Huang S, Cai J, Tian Y (2021) The prognostic value of homocysteine in acute ischemic stroke patients: a systematic review and meta-analysis. Front Syst Neurosci 12(14):600582
Zhang W, Zhang X (2015) Correlation between the youth cerebral infarction in different TOAST classifications and high homocysteine. Cell Biochem Biophys 71(1):39–42
Spencer ChGC, Martin SC, Felmeden DC, Blann AD, Beevers GD, Lip GYH (2004) Relationship of homocysteine to markers of platelet and endothelial activation in “high risk” hypertensives: a substudy of the Anglo-Scandinavian Cardiac Outcomes Trial. Int J Cardiol 94(2–3):293–300
Kaźmierski J, Sobów T (2011) Hiperhomocysteinemia jako czynnik ryzyka i cel terapeutyczny w leczeniu i profilaktyce wtórnej udaru niedokrwiennego. In: Kozubski W, Dorszewska J (eds) Homocysteina a farmakoterapia w neurologii. Poznan University of Medical Sciences, Poznan, Poland, pp 99–114 (in Polish)
Ozkul A, Akyol A, Yenisey C, Arpaci E, Kiylioglu N, Tataroglu C (2007) Oxidative stress in acute ischemic storke. J Clin Neurosci 14:1062–1066
Xu Y, Sun Z (2015) Molecular basis of Klotho: from gene to function in aging. Endocr Rev 36(2):174–193
Shiels PG, Stenvinkel P, Kooman JP, McGuinness D (2017) Circulating markers of ageing and allostatic load: a slow train coming. Pract Lab Med 7:49–54
Salvioli S, Monti D, Lanzarini C et al (2013) Immune system, cell senescence, aging and longevity–inflamm-aging reappraised. Curr Pharm Des 19(9):1675–1679
Alzheimer’s Association (2016) 2016 Alzheimer’s disease facts and figures. Alzheimers Dement 12(4):459–509
Baumgart M, Snyder HM, Carrillo MC, Fazio S, Kim H, Johns H (2015) Summary of the evidence on modifiable risk factors for cognitive decline and dementia: a population-based perspective. Alzheimers Dement 11(6):718–726
Campisi J (2013) Aging, cellular senescence, and cancer. Annu Rev Physiol 75:685–705
Campisi J, d’Adda di Fagagna F (2007) Cellular senescence: when bad things happen to good cells. Nat Rev Mol Cell Biol 8(9):729–740
Alzheimer’s Association (2016) Alzheimer’s disease facts and figures. Alzheimers Dement 12(4):459–509
Prince M, Bryce R, Albanese E, Wimo A, Ribeiro W, Ferri CP (2013) The global prevalence of dementia: a systematic review and metaanalysis. Alzheimers Dement 9(1):63–75
Ballard C, Gauthier S, Corbett A, Brayne C, Aarsland D, Jones E (2011) Alzheimer’s disease. Lancet 377(9770):1019–1031
Wang X, Wang W, Li L, Perry G, Lee H, Zhu X (1842) Oxidative stress and mitochondrial dysfunction in Alzheimer’s disease. Biochim Biophys Acta 8:1240–1247
Hayyan M, Hashim MA, AlNashef IM (2016) Superoxide ion: generation and chemical implications. Chem Rev 116(5):3029–3085
Edreva A (2005) Generation and scavenging of reactive oxygen species in chloroplasts: a submolecular approach. Agric Ecosyst Environ 106(2):119–133
Pérez MJ, Ponce DP, Osorio-Fuentealba C, Behrens MI, Quintanilla RA (2017) Mitochondrial bioenergetics is altered in fibroblasts from patients with sporadic Alzheimer’s disease. Front Neurosci 11:553
Ramamoorthy M, Sykora P, Scheibye-Knudsen M et al (2012) Sporadic Alzheimer disease fibroblasts display an oxidative stress phenotype. Free Radic Biol Med 53(6):1371–1380
Ott C, Jacobs K, Haucke E, Navarrete Santos A, Grune T, Simm A (2014) Role of advanced glycation end products in cellular signaling. Redox Biol 2:411–429
Sasaki N, Fukatsu R, Tsuzuki K et al (1998) Advanced glycation end products in Alzheimer’s disease and other neurodegenerative diseases. Am J Pathol 153(4):1149–1155
Kowalska M, Wize K, Prendecki M, Lianeri M, Kozubski W, Dorszewska J (2020) Genetic variants and oxidative stress in Alzheimer’s disease. Curr Alzheimer Res 17(3):208–223
Ho PI, Ortiz D, Rogers E, Shea TB (2002) Multiple aspects of homocysteine neurotoxicity: glutamate excitotoxicity, kinase hyperactivation and DNA damage. J Neurosci Res 70(5):694–702
Setién-Suero E, Suárez-Pinilla M, Suárez-Pinilla P, Crespo-Facorro B, Ayesa-Arriola R (2016) Homocysteine and cognition: a systematic review of 111 studies. Neurosci Biobehav Rev 69:280–298
Morrison LD, Smith DD, Kish SJ (1996) Brain S-Adenosylmethionine levels are severely decreased in Alzheimer’s disease. J Neurochem 67(3):1328–1331
Fuso A, Seminara L, Cavallaro RA, D’Anselmi F, Scarpa S (2005) S-adenosylmethionine/homocysteine cycle alterations modify DNA methylation status with consequent deregulation of PS1 and BACE and beta-amyloid production. Mol Cell Neurosci 28(1):195–204
Bosetti F (2002) Cytochrome c oxidase and mitochondrial F1F0-ATPase (ATP synthase) activities in platelets and brain from patients with Alzheimer’s disease. Neurobiol Aging 23(3):371–376
Kish SJ, Bergeron C, Rajput A et al (1992) Brain cytochrome oxidase in Alzheimer’s disease. J Neurochem 59:776–779
Lunnon K, Keohane A, Pidsley R et al (2017) Mitochondrial genes are altered in blood early in Alzheimer’s disease. Neurobiol Aging 53:36–47
Maurer I (2000) A selective defect of cytochrome c oxidase is present in brain of Alzheimer disease patients. Neurobiol Aging 21(3):455–462
Mutisya EM, Bowling AC, Beal MF (1994) Cortical cytochrome oxidase activity is reduced in Alzheimer’s disease. J Neurochem 63(6):2179–2184
Valla J, Berndt JD, Gonzalez-Lima F (2001) Energy hypometabolism in posterior cingulate cortex of Alzheimer’s patients: superficial laminar cytochrome oxidase associated with disease duration. J Neurosci 21(13):4923–4930
Davis RE, Miller S, Herrnstadt C et al (1997) Mutations in mitochondrial cytochrome c oxidase genes segregate with late-onset Alzheimer disease. Proc Natl Acad Sci USA 94(9):4526–4531
Dorsey ER, Constantinescu R, Thompson JP et al (2006) Projected number of people with Parkinson disease in the most populous nations, 2005 through 2030. Neurology 68(5):384–386
Spillantini MG, Goedert M (2006) The α-Synucleinopathies: Parkinson’s disease, dementia with Lewy bodies, and multiple system atrophy. Ann N Y Acad Sci 920:16–27
Kravitz AV, Freeze BS, Parker PR et al (2010) Regulation of parkinsonian motor behaviours by optogenetic control of basal ganglia circuitry. Nature 466(7306):622–626
Perez FA, Palmiter RD (2005) Parkin-deficient mice are not a robust model of parkinsonism. Proc Natl Acad Sci USA 102(6):2174–2179
Banerjee R, Starkov AA, Beal MF, Thomas B (2009) Mitochondrial dysfunction in the limelight of Parkinson’s disease pathogenesis. Biochim Biophys Acta 1792(7):651–663
Parnetti L, Gaetani L, Eusebi P (2019) CSF and blood biomarkers for Parkinson’s disease. Lancet Neurol 18(6):573–586
Braak H, Ghebremedhin E, Rüb U, Bratzke H, Del Tredici K (2004) Stages in the development of Parkinson’s disease-related pathology. Cell Tissue Res 318(1):121–134
Dorszewska J, Kowalska M, Prendecki M, Piekut T, Kozłowska J, Kozubski W (2021) Oxidative stress factors in Parkinson’s disease. Neural Regen Res 16(7):1383–1391
Puspita L, Chung SY, Shim J (2017) Oxidative stress and cellular pathologies in Parkinson’s disease. Mol Brain 10(1):53
Saito Y (2017) DJ-1 as a biomarker of Parkinson’s disease. Adv Exp Med Biol 1037:149–171
Bender A, Krishnan KJ, Morris CM et al (2006) High levels of mitochondrial DNA deletions in substantia nigra neurons in aging and Parkinson disease. Nat Genet 38(5):515–517
Dröse S, Brandt U (2008) The Mechanism of Mitochondrial Superoxide Production by the Cytochrome bc1 Complex. J Biol Chem 283(31):21649–21654
Subramaniam SR, Chesselet M-F (2013) Mitochondrial dysfunction and oxidative stress in Parkinson’s disease. Prog Neurobiol 106–107:17–32
Misgeld T, Schwarz TL (2017) Mitostasis in neurons: maintaining mitochondria in an extended cellular architecture. Neuron 96(3):651–666
Amadoro G, Corsetti V, Florenzano F et al (2014) Morphological and bioenergetic demands underlying the mitophagy in post-mitotic neurons: the pink–parkin pathway. Front Aging Neurosci 6:18
Harper JW, Ordureau A, Heo J-M (2018) Building and decoding ubiquitin chains for mitophagy. Nat Rev Mol Cell Biol 19(2):93–108
van der Merwe C, Jalali Sefid Dashti Z, Christoffels A, Loos B, Bardien S (2015) Evidence for a common biological pathway linking three Parkinson’s disease-causing genes:parkin, PINK1and DJ-1. Eur J Neurosci 41(9):1113–1125
Kalinderi K, Bostantjopoulou S, Fidani L (2016) The genetic background of Parkinson’s disease: current progress and future prospects. Acta Neurol Scand 134(5):314–326
Banerjee R, Beal MF, Thomas B (2010) Autophagy in neurodegenerative disorders: pathogenic roles and therapeutic implications. Trends Neurosci 33(12):541–549
Lynch-Day MA, Mao K, Wang K, Zhao M, Klionsky DJ (2012) The role of autophagy in Parkinson’s disease. Cold Spring Harb Perspect Med 2(4):a009357–a009357
Shamoto-Nagai M, Maruyama W, Kato Y et al (2003) An inhibitor of mitochondrial complex I, rotenone, inactivates proteasome by oxidative modification and induces aggregation of oxidized proteins in SH-SY5Y cells. J Neurosci Res 74(4):589–597
LaVoie MJ, Hastings TG (1999) Dopamine quinone formation and protein modification associated with the striatal neurotoxicity of methamphetamine: evidence against a role for extracellular dopamine. J Neurosci 19(4):1484–1491
Van Laar VS, Mishizen AJ, Cascio M, Hastings TG (2009) Proteomic identification of dopamine-conjugated proteins from isolated rat brain mitochondria and SH-SY5Y cells. Neurobiol Dis 34(3):487–500
Girotto S, Sturlese M, Bellanda M et al (2012) Dopamine-derived Quinones Affect the Structure of the Redox Sensor DJ-1 through Modifications at Cys-106 and Cys-53. J Biol Chem 287(22):18738–18749
Kim S-J, Park Y-J, Hwang I-Y, Youdim MBH, Park K-S, Oh YJ (2012) Nuclear translocation of DJ-1 during oxidative stress-induced neuronal cell death. Free Radic Biol Med 53(4):936–950
Kahle PJ, Waak J, Gasser T (2009) DJ-1 and prevention of oxidative stress in Parkinson’s disease and other age-related disorders. Free Radic Biol Med 47(10):1354–1361
Hayashi T, Ishimori C, Takahashi-Niki K et al (2009) DJ-1 binds to mitochondrial complex I and maintains its activity. Biochem Biophys Res Commun 390(3):667–672
Lotharius J, Brundin P (2002) Pathogenesis of Parkinson’s disease: dopamine, vesicles and α-synuclein. Nat Rev Neurosci 3(12):932–942
Deas E, Cremades N, Angelova PR et al (2016) Alpha-synuclein oligomers interact with metal ions to induce oxidative stress and neuronal death in Parkinson’s disease. Antioxid Redox Signal 24(7):376–391
He R, Yan X, Guo J, Xu Q, Tang B, Sun Q (2018) Recent advances in biomarkers for Parkinson’s disease. Front Aging Neurosci 10:305
Dorszewska J, Prendecki M, Lianeri M, Kozubski W (2014) Molecular effects of L-dopa therapy in Parkinson’s disease. Curr Genomics 15(1):11–17
https://www.who.int/news-room/fact-sheets/detail/epilepsy, 9 February 2023
Ngugi AK, Kariuki SM, Bottomley C, Kleinschmidt I, Sander JW, Newton CR (2011) Incidence of epilepsy: a systematic review and meta-analysis. Neurology 77(10):1005–1012
Vu LC, Piccenna L, Kwan P, O’Brien TJ (2018) New-onset epilepsy in the elderly. Br J Clin Pharmacol 84(10):2208–2217
Scheffer IE, Berkovic S, Capovilla G et al (2017) ILAE classification of the epilepsies: position paper of the ILAE Commission for Classification and Terminology. Epilepsia 58(4):512–521
Berg AT, Berkovic SF, Brodie MJ et al (2010) Revised terminology and concepts for organization of seizures and epilepsies: report of the ILAE Commission on Classification and Terminology 2005–2009. Epilepsia 51(4):676–685
Scheffer IE, Nabbout R (2019) SCN1A-related phenotypes: epilepsy and beyond. Epilepsia 60(Suppl 3):S17–S24
Yow HY, Ahmad N, Makmor-Bakry M (2013) Pathogenesis of epilepsy: challenges in animal models. Iran J Basic Med Sci 16(11):1119–1132
Boison D, Steinhäuser C (2018) Epilepsy and astrocyte energy metabolism. Glia 66(6):1235–1243
Beamer E, Kuchukulla M, Boison D, Engel T (2021) ATP and adenosine-Two players in the control of seizures and epilepsy development. Prog Neurobiol 204:102105
Chan F, Liu J (2021) Molecular regulation of brain metabolism underlying circadian epilepsy. Epilepsia 62 Suppl 1(Suppl 1):S32–S48
Aroniadou-Anderjaska V, Fristch B, Qashu F, Braga MF (2008) Pathology and pathophysiology of the amygdala in epileptogenesis and epilepsy. Epilepsy Res 78(2–3):102–116
Reiner A, Levitz J (2018) Glutamatergic signaling in the central nervous system: ionotropic and metabotropic receptors in concert. Neuron 98(6):1080–1098
Treiman DM (2001) GABAergic mechanisms in epilepsy. Epilepsia 42(Suppl 3):8–12
Kai K, Ruusuvuori E, Seja P, Voipio J, Puskarjov M (2014) GABA actions and ionic plasticity in epilepsy. Curr Opin Neurobiol 26:34–41
Voglis G, Tavernarakis N (2006) The role of synaptic ion channels in synaptic plasticity. EMBO Rep 7(11):1104–1110
Chapman AG (2000) Glutamate and epilepsy. J Nutr 130(4S Suppl):1043S-1045S
Yi JH, Hazell AS (2006) Excitotoxic mechanisms and the role of astrocytic glutamate transporters in traumatic brain injury. Neurochem Int 48(5):394–403
Boon P, Santos SF, Jansen AC, Lagae L, Legros B, Weckhuysen S (2021) Recommendations for the treatment of epilepsy in adult and pediatric patients in Belgium: 2020 update. Acta Neurol Belg 121(1):241–257
Sniezawska A, Dorszewska J, Rozycka A et al (2011) MTHFR, MTR, and MTHFD1 gene polymorphisms compared to homocysteine and asymmetric dimethylarginine concentrations and their metabolites in epileptic patients treated with antiepileptic drugs. Seizure 20(7):533–540
Lagan-Jedrzejczyk U, Lianeri M, Kozubski W, Dorszewska J (2014) Homocysteine and apoptotic factors in epileptic patients treated with antiepileptic drugs. In: McCully K (ed) Homocysteine: structure, biosynthesis and health implications. NOVA Sciences Publishers Inc, NY, USA, pp 83–111
Loi M, Trazzi S, Fuchs C et al (2020) Increased DNA Damage and Apoptosis in CDKL5-Deficient Neurons. Mol Neurobiol 57(5):2244–2262
Matz K, Tuomilehto J, Teuschl Y, Dachenhausen A, Brainin M (2022) Comparison of oral glucose tolerance test and HbA1c in detection of disorders of glucose metabolism in patients with acute stroke. Cardiovasc Diabetol 19(1):204
Yamagata K (2022) Lactate supply from astrocytes to neurons and its role in ischemic stroke-induced neurodegeneration. Neuroscience 481:219–231
Rana AK, Singh D (2018) Targeting glycogen synthase kinase-3 for oxidative stress and neuroinflammation: opportunities, challenges and future directions for cerebral stroke management. Neuropharmacology 139:124–136
Yu ZF, Mattson MP (1999) Dietary restriction and 2-deoxyglucose administration reduce focal ischemic brain damage and improve behavioral outcome: evidence for a preconditioning mechanism. J Neurosci Res 57(6):830–839
Lioutas VA, Alfaro-Martinez F, Bedoya F, Chung CC, Pimentel DA, Novak V (2015) Intranasal insulin and insulin-like growth factor 1 as neuroprotectants in acute ischemic stroke. Transl Stroke Res 6(4):264–275
Chen Z, Zhong Ch (2013) Decoding Alzheimer’s disease from perturbed cerebral glucose metabolism: implications for diagnostic and therapeutic strategies. Prog Neurobiol 108:21–43
Carter SF, Herholz K, Rosa-Neto P, Pellerin L, Nordberg A, Zimmer ER (2019) Astrocyte biomarkers in Alzheimer’s disease. Trends Mol Med 25(2):77–95
Duarte AI, Santos MS, Oliveira CR, Moreira PI (2018) Brain insulin signalling, glucose metabolism and females’ reproductive aging: a dangerous triad in Alzheimer’s disease. Neuropharmacology 136(Pt B):223–242
Nadebaum DP, Krishnadas N, Poon AMT et al (2021) Head-to-head comparison of cerebral blood flow single-photon emission computed tomography and 18 F-fluoro-2-deoxyglucose positron emission tomography in the diagnosis of Alzheimer disease. Intern Med J 51(8):1243–1250
Kellar D, Craft S (2020) Brain insulin resistance in Alzheimer’s disease and related disorders: mechanisms and therapeutic approaches. Lancet Neurol 19(9):758–766
Marques A, Dutheil F, Durand E et al (2018) Glucose dysregulation in Parkinson’s disease: too much glucose or not enough insulin? Parkinsonism Relat Disord 55:122–127
Nagao M, Hayashi H (2009) Glycogen synthase kinase-3beta is associated with Parkinson’s disease. Neurosci Lett 449(2):103–107
Walker Z, Gandolfo F, Orini S et al (2018) Clinical utility of FDG PET in Parkinson’s disease and atypical parkinsonism associated with dementia. Eur J Nucl Med Mol Imaging 45(9):1534–1545
Kwon HS, Koh SH (2020) Neuroinflammation in neurodegenerative disorders: the roles of microglia and astrocytes. Transl Neurodegener 9(1):42
Fauser S, Tumani H (2017) Epilepsy. Handb Clin Neurol 146:259–266
McDonald TS, Carrasco-Pozo C, Hodson MP, Borges K (2017) Alterations in cytosolic and mitochondrial [U- 13 C]glucose metabolism in a chronic epilepsy mouse model. eNeuro 4(1):ENEURO.0341-16.2017
Hamed SA (2007) Leptin and insulin homeostasis in epilepsy: relation to weight adverse conditions. Epilepsy Res 75(1):1–9
Liu HG, Yang BW, Zhao BT et al (2021) The electroclinical features and surgical outcomes of inferior perisylvian epilepsy. Epilepsy Behav 121(Pt A):108028
Andrabi SS, Parvez S, Tabassum H (2020) Ischemic stroke and mitochondria: mechanisms and targets. Protoplasma 257(2):335–343
Kann O, Kovács R (2007) Mitochondria and neuronal activity. Am J Physiol Cell Physiol 292(2):C641-657
Wu Y, Chen M, Jiang J (2019) Mitochondrial dysfunction in neurodegenerative diseases and drug targets via apoptotic signaling. Mitochondrion 49:35–45
Li P, Stetler RA, Leak RK et al (2018) Oxidative stress and DNA damage after cerebral ischemia: potential therapeutic targets to repair the genome and improve stroke recovery. Neuropharmacology 134(Pt B):208–217
Olowe R, Sandouka S, Saadi A, Shekh-Ahmad T (2020) Approaches for reactive oxygen species and oxidative stress quantification in epilepsy. Antioxidants (Basel) 9(10):990
Arlt S, Schwedhelm E, Kölsch H et al (2012) Dimethylarginines, homocysteine metabolism, and cerebrospinal fluid markers for Alzheimer’s disease. J Alzheimers Dis 31(4):751–758
Smeyne M, Smeyne RJ (2013) Glutathione metabolism and Parkinson’s disease. Free Radic Biol Med 62:13–25
Fan X, Zhang L, Li H et al (2020) Role of homocysteine in the development and progression of Parkinson’s disease. Ann Clin Transl Neurol 7(11):2332–2338
Kirbas S, Kirbas A, Tufekci A et al (2016) Serum levels of homocysteine, asymmetric dimethylarginine and nitric oxide in patients with Parkinson’s disease. Acta Clin Belg 71(2):71–75
Ansari R, Mahta A, Mallack E, Luo JJ (2014) Hyperhomocysteinemia and neurologic disorders: a review. J Clin Neurol 10(4):281–288
Nikolic D, Jankovic M, Petrovic B, Novakovic I (2020) Genetic aspects of inflammation and immune response in stroke. Int J Mol Sci 21(19):7409
Nikolac Perkovic M, Videtic Paska A, Konjevod M et al (2021) Epigenetics of Alzheimer’s disease. Biomolecules 11(2):195
Pavlou MAS, Outeiro TF (2017) Epigenetics in Parkinson’s disease. Adv Exp Med Biol 978:363–390
Henshall DC, Kobow K (2015) Epigenetics and epilepsy. Cold Spring Harb Perspect Med 5(12):a022731
Wang Y, Lu S, Chen Y et al (2021) Smoothened is a therapeutic target for reducing glutamate toxicity in ischemic stroke. Sci Transl Med 13(610):eaba3444
Czapski GA, Strosznajder JB (2021) Glutamate and GABA in microglia-neuron cross-talk in Alzheimer’s disease. Int J Mol Sci 22(21):11677
Iovino L, Tremblay ME, Civiero L (2020) Glutamate-induced excitotoxicity in Parkinson’s disease: the role of glial cells. J Pharmacol Sci 144(3):151–164
Beghi E, Beghi M (2020) Epilepsy, antiepileptic drugs and dementia. Curr Opin Neurol 33(2):191–197
Zaremba PD, Białek M, Błaszczyk B, Cioczek P, Czuczwar SJ (2006) Non-epilepsy uses of antiepilepsy drugs. Pharmacol Rep 58(1):1–12
Funding
This work was co-supported by the Polish National Centre for Research and Development (NCBiR) (co-funded by the European Union), grant no. POWR.03.01.00–00-T006/18–00.
Author information
Authors and Affiliations
Contributions
Izabela Korczowska-Łącka—section preparation “The Role of Homocysteine and Its Metabolism in Stroke”.
Mikołaj Hurła—section preparation “Energy Changes in Alzheimer’s Disease”.
Natalia Banaszek—section preparation “Energy Disorders in Parkinson’s Disease”.
Dominik Kobylarek—section preparation “Epilepsy and Energy Damage”.
Oliwia Szymanowicz—substantive and editorial, linguistic improvement.
Wojciech Kozubski—substantial contributions to the conception or design of the work.
Jolanta Dorszewska—drafting the work or revising it critically for important intellectual content and final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Research Involving Human Participants and/or Animals
Not applicable.
Informed Consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Korczowska-Łącka, I., Hurła, M., Banaszek, N. et al. Selected Biomarkers of Oxidative Stress and Energy Metabolism Disorders in Neurological Diseases. Mol Neurobiol 60, 4132–4149 (2023). https://doi.org/10.1007/s12035-023-03329-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-023-03329-4