Abstract
Background
Intracerebral hemorrhage (ICH) is one of the most lethal stroke types and lacks effective therapeutic regimens. Recently, evidence has suggested the involvement of the ferroptosis inhibitor ferrostatin-1 (Fer-1) in the pathophysiological process of ICH. In this study, we examined the underlying mechanism.
Methods
We induced an in vitro apoptosis model in organotypic hippocampal slice (OHS) using hemoglobin (Hb) and an in vivo ICH model using collagenase. OHSs were treated with MK-801, Fer-1, glutamate, and Hb to assess the impacts of Fer-1 on neuron apoptosis, glutathione peroxidase-4 activity, reactive oxygen species production, inflammation-related factors, expression of M1 markers and M2 markers, and the phagocytic function of microglial cells in vitro. Then, ICH mice were treated with Fer-1 and ruxolitinib to evaluate the effects of Fer-1-orchestrating janus kinase 1/signal transducer and activator of transcription 6 pathway on neurological function, brain water content, hematoma volume, the anti-inflammatory factor, M1 and M2 markers, and the phagocytic function of microglial cells in vivo.
Results
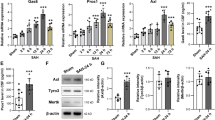
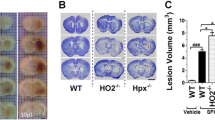
Hb or glutamate facilitated glutathione peroxidase dysfunction, reactive oxygen species production, and neuronal apoptosis in OHSs, which was nullified by Fer-1. Fer-1 polarized microglial cells to the M2 phenotype, enhanced their phagocytic function, and prevented inflammation in Hb-induced OHSs. In the ICH mouse model, Fer-1 was found to improve neurological function and promote hematoma absorption. In addition, Fer-1 activated the Fer-1-orchestrating janus kinase 1/signal transducer and activator of transcription 6 pathway, which accelerated microglial M2 polarization, enhanced the phagocytic function of microglial cells, and restrained inflammation in ICH mice.
Conclusions
Overall, our findings suggest that Fer-1 may be a novel mechanism underlying microglial M2 polarization and inflammation after ICH.







Similar content being viewed by others
References
Ikram MA, Wieberdink RG, Koudstaal PJ. International epidemiology of intracerebral hemorrhage. Curr Atheroscler Rep. 2012;14(4):300–6. https://doi.org/10.1007/s11883-012-0252-1.
Charidimou A, Morotti A, Valenti R, et al. Journal Club: time trends in incidence, case fatality, and mortality of intracerebral hemorrhage. Neurology. 2016;86(20):e206–9. https://doi.org/10.1212/WNL.0000000000002678.
Jolink WMT, Wiegertjes K, Rinkel GJE, Algra A, de Leeuw FE, Klijn CJM. Location-specific risk factors for intracerebral hemorrhage: systematic review and meta-analysis. Neurology. 2020;95(13):e1807–18. https://doi.org/10.1212/WNL.0000000000010418.
Cordonnier C, Demchuk A, Ziai W, Anderson CS. Intracerebral haemorrhage: current approaches to acute management. Lancet. 2018;392(10154):1257–68. https://doi.org/10.1016/S0140-6736(18)31878-6.
Wolf SA, Boddeke HW, Kettenmann H. Microglia in physiology and disease. Annu Rev Physiol. 2017;79:619–43. https://doi.org/10.1146/annurev-physiol-022516-034406.
Li Q, Lan X, Han X, Wang J. Expression of Tmem119/Sall1 and Ccr2/CD69 in FACS-sorted microglia- and monocyte/macrophage-enriched cell populations after intracerebral hemorrhage. Front Cell Neurosci. 2018;12:520. https://doi.org/10.3389/fncel.2018.00520.
Chang CF, Wan J, Li Q, Renfroe SC, Heller NM, Wang J. Alternative activation-skewed microglia/macrophages promote hematoma resolution in experimental intracerebral hemorrhage. Neurobiol Dis. 2017;103:54–69. https://doi.org/10.1016/j.nbd.2017.03.016.
Horwath MC, Bell-Horwath TR, Lescano V, Krishnan K, Merino EJ, Deepe GS Jr. Antifungal activity of the lipophilic antioxidant ferrostatin-1. ChemBioChem. 2017;18(20):2069–78. https://doi.org/10.1002/cbic.201700105.
Zhang Z, Wu Y, Yuan S, et al. Glutathione peroxidase 4 participates in secondary brain injury through mediating ferroptosis in a rat model of intracerebral hemorrhage. Brain Res. 2018;1701:112–25. https://doi.org/10.1016/j.brainres.2018.09.012.
Li Q, Han X, Lan X, et al. Inhibition of neuronal ferroptosis protects hemorrhagic brain. JCI Insight. 2017;2(7): e90777. https://doi.org/10.1172/jci.insight.90777.
He Y, Gao Y, Zhang Q, Zhou G, Cao F, Yao S. IL-4 switches microglia/macrophage M1/M2 polarization and alleviates neurological damage by modulating the JAK1/STAT6 pathway following ICH. Neuroscience. 2020;437:161–71. https://doi.org/10.1016/j.neuroscience.2020.03.008.
Cai W, Dai X, Chen J, et al. STAT6/Arg1 promotes microglia/macrophage efferocytosis and inflammation resolution in stroke mice. JCI Insight. 2019;4(20): e131355. https://doi.org/10.1172/jci.insight.131355.
Wang JB, Erickson JW, Fuji R, et al. Targeting mitochondrial glutaminase activity inhibits oncogenic transformation. Cancer Cell. 2010;18(3):207–19. https://doi.org/10.1016/j.ccr.2010.08.009.
Kim H, Kim E, Park M, Lee E, Namkoong K. Organotypic hippocampal slice culture from the adult mouse brain: a versatile tool for translational neuropsychopharmacology. Prog Neuropsychopharmacol Biol Psychiatry. 2013;41:36–43. https://doi.org/10.1016/j.pnpbp.2012.11.004.
Hu F, Huang Y, Semtner M, et al. Down-regulation of Aquaporin-1 mediates a microglial phenotype switch affecting glioma growth. Exp Cell Res. 2020;396(2):112323. https://doi.org/10.1016/j.yexcr.2020.112323.
Wang Q, Zou MH. Measurement of reactive oxygen species (ROS) and mitochondrial ROS in AMPK knockout mice blood vessels. Methods Mol Biol. 2018;1732:507–17. https://doi.org/10.1007/978-1-4939-7598-3_32.
Kernstock RM, Girotti AW. New strategies for the isolation and activity determination of naturally occurring type-4 glutathione peroxidase. Protein Expr Purif. 2008;62(2):216–22. https://doi.org/10.1016/j.pep.2008.07.014.
Riccardi C, Nicoletti I. Analysis of apoptosis by propidium iodide staining and flow cytometry. Nat Protoc. 2006;1(3):1458–61. https://doi.org/10.1038/nprot.2006.238.
Hosny NM, Atia NN, El-Gizawy SM, Badary DM, Hareedy MS. Innovative HPTLC method with fluorescence detection for assessment of febuxostat-montelukast combination and study of their protective effects against gouty arthritis. Analyst. 2018;143(18):4366–78. https://doi.org/10.1039/c8an00772a.
Tamakoshi K, Ishida A, Takamatsu Y, et al. Motor skills training promotes motor functional recovery and induces synaptogenesis in the motor cortex and striatum after intracerebral hemorrhage in rats. Behav Brain Res. 2014;260:34–43. https://doi.org/10.1016/j.bbr.2013.11.034.
Masuda T, Maki M, Hara K, et al. Peri-hemorrhagic degeneration accompanies stereotaxic collagenase-mediated cortical hemorrhage in mouse. Brain Res. 2010;1355:228–39. https://doi.org/10.1016/j.brainres.2010.07.101.
Heine A, Held SA, Daecke SN, et al. The JAK-inhibitor ruxolitinib impairs dendritic cell function in vitro and in vivo. Blood. 2013;122(7):1192–202. https://doi.org/10.1182/blood-2013-03-484642.
Takamatsu Y, Ishida A, Hamakawa M, Tamakoshi K, Jung CG, Ishida K. Treadmill running improves motor function and alters dendritic morphology in the striatum after collagenase-induced intracerebral hemorrhage in rats. Brain Res. 2010;1355:165–73. https://doi.org/10.1016/j.brainres.2010.07.070.
Clark WM, Lessov NS, Dixon MP, Eckenstein F. Monofilament intraluminal middle cerebral artery occlusion in the mouse. Neurol Res. 1997;19(6):641–8. https://doi.org/10.1080/01616412.1997.11740874.
MacLellan CL, Auriat AM, McGie SC, et al. Gauging recovery after hemorrhagic stroke in rats: implications for cytoprotection studies. J Cereb Blood Flow Metab. 2006;26(8):1031–42. https://doi.org/10.1038/sj.jcbfm.9600255.
Qu X, Wang N, Cheng W, Xue Y, Chen W, Qi M. MicroRNA-146a protects against intracerebral hemorrhage by inhibiting inflammation and oxidative stress. Exp Ther Med. 2019;18(5):3920–8. https://doi.org/10.3892/etm.2019.8060.
Wu H, Wu T, Li M, Wang J. Efficacy of the lipid-soluble iron chelator 2,2’-dipyridyl against hemorrhagic brain injury. Neurobiol Dis. 2012;45(1):388–94. https://doi.org/10.1016/j.nbd.2011.08.028.
Zeng J, Chen Y, Ding R, et al. Isoliquiritigenin alleviates early brain injury after experimental intracerebral hemorrhage via suppressing ROS- and/or NF-kappaB-mediated NLRP3 inflammasome activation by promoting Nrf2 antioxidant pathway. J Neuroinflammation. 2017;14(1):119. https://doi.org/10.1186/s12974-017-0895-5.
Chen S, Zhao L, Sherchan P, et al. Activation of melanocortin receptor 4 with RO27-3225 attenuates neuroinflammation through AMPK/JNK/p38 MAPK pathway after intracerebral hemorrhage in mice. J Neuroinflammation. 2018;15(1):106. https://doi.org/10.1186/s12974-018-1140-6.
Zhou Y, Wang S, Li Y, Yu S, Zhao Y. SIRT1/PGC-1alpha signaling promotes mitochondrial functional recovery and reduces apoptosis after intracerebral hemorrhage in rats. Front Mol Neurosci. 2017;10:443. https://doi.org/10.3389/fnmol.2017.00443.
Chang CF, Goods BA, Askenase MH, et al. Erythrocyte efferocytosis modulates macrophages towards recovery after intracerebral hemorrhage. J Clin Invest. 2018;128(2):607–24. https://doi.org/10.1172/JCI95612.
Byun YG, Chung WS. A novel in vitro live-imaging assay of astrocyte-mediated phagocytosis using pH indicator-conjugated synaptosomes. J Vis Exp. 2018;132:56647. https://doi.org/10.3791/56647.
Lan X, Han X, Li Q, et al. Pinocembrin protects hemorrhagic brain primarily by inhibiting toll-like receptor 4 and reducing M1 phenotype microglia. Brain Behav Immun. 2017;61:326–39. https://doi.org/10.1016/j.bbi.2016.12.012.
Gadermaier E, Tesarz M, Suciu AA, Wallwitz J, Berg G, Himmler G. Characterization of a sandwich ELISA for the quantification of all human periostin isoforms. J Clin Lab Anal. 2018;32(2): e22252. https://doi.org/10.1002/jcla.22252.
Yao ST, Cao F, Chen JL, et al. NLRP3 is required for complement-mediated caspase-1 and IL-1beta activation in ICH. J Mol Neurosci. 2017;61(3):385–95. https://doi.org/10.1007/s12031-016-0874-9.
Wu T, Liang X, Liu X, et al. Induction of ferroptosis in response to graphene quantum dots through mitochondrial oxidative stress in microglia. Part Fibre Toxicol. 2020;17(1):30. https://doi.org/10.1186/s12989-020-00363-1.
Gong Y, Wang N, Liu N, Dong H. Lipid peroxidation and GPX4 inhibition are common causes for myofibroblast differentiation and ferroptosis. DNA Cell Biol. 2019;38(7):725–33. https://doi.org/10.1089/dna.2018.4541.
Wang S, Cao M, Xu S, et al. Luteolin alters macrophage polarization to inhibit inflammation. Inflammation. 2020;43(1):95–108. https://doi.org/10.1007/s10753-019-01099-7.
Wang L, Zhao H, Wang L, et al. Effects of selected resveratrol analogues on activation and polarization of lipopolysaccharide-stimulated BV-2 microglial cells. J Agric Food Chem. 2020;68(12):3750–7. https://doi.org/10.1021/acs.jafc.0c00498.
Yamada N, Karasawa T, Wakiya T, et al. Iron overload as a risk factor for hepatic ischemia-reperfusion injury in liver transplantation: potential role of ferroptosis. Am J Transplant. 2020;20(6):1606–18. https://doi.org/10.1111/ajt.15773.
Lan X, Han X, Liu X, Wang J. Inflammatory responses after intracerebral hemorrhage: from cellular function to therapeutic targets. J Cereb Blood Flow Metab. 2019;39(1):184–6. https://doi.org/10.1177/0271678X18805675.
Jung JE, Sun G, Bautista Garrido J, et al. The mitochondria-derived peptide humanin improves recovery from intracerebral hemorrhage: implication of mitochondria transfer and microglia phenotype change. J Neurosci. 2020;40(10):2154–65. https://doi.org/10.1523/JNEUROSCI.2212-19.2020.
Zhao X, Sun G, Zhang J, Ting SM, Gonzales N, Aronowski J. Dimethyl fumarate protects brain from damage produced by intracerebral hemorrhage by mechanism involving Nrf2. Stroke. 2015;46(7):1923–8. https://doi.org/10.1161/STROKEAHA.115.009398.
Chen B, Chen Z, Liu M, et al. Inhibition of neuronal ferroptosis in the acute phase of intracerebral hemorrhage shows long-term cerebroprotective effects. Brain Res Bull. 2019;153:122–32. https://doi.org/10.1016/j.brainresbull.2019.08.013.
Li P, Zhao G, Ding Y, et al. Rh-IFN-alpha attenuates neuroinflammation and improves neurological function by inhibiting NF-kappaB through JAK1-STAT1/TRAF3 pathway in an experimental GMH rat model. Brain Behav Immun. 2019;79:174–85. https://doi.org/10.1016/j.bbi.2019.01.028.
Li S, Yang S, Sun B, Hang C. Melatonin attenuates early brain injury after subarachnoid hemorrhage by the JAK-STAT signaling pathway. Int J Clin Exp Pathol. 2019;12(3):909–15.
Im JH, Yeo IJ, Park PH, et al. Deletion of Chitinase-3-like 1 accelerates stroke development through enhancement of neuroinflammation by STAT6-dependent M2 microglial inactivation in Chitinase-3-like 1 knockout mice. Exp Neurol. 2020;323: 113082. https://doi.org/10.1016/j.expneurol.2019.113082.
Acknowledgements
We acknowledge and appreciate our colleagues for their valuable efforts and comments regarding this article.
Funding
This study was supported by Qiqihar science and Technology Bureau (SFGG-201952).
Author information
Authors and Affiliations
Contributions
Lijuan Huang and Yanjiao Zhang participated in the conception and design of the study. Liang Zhao and Qingyou Chen performed the analysis and interpretation of data. Li Li contributed to drafting the article. Lijuan Huang and Yanjiao Zhang revised it critically for important intellectual content. Liang Zhao is the guarantor for the article who accepts full responsibility for the work and/or the conduct of the study, had access to the data, and oversaw the decision to publish. The final manuscript was approved by all authors.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical Approval/Human and Animal Rights
We confirm that this manuscript adheres to ethical guidelines and indicate ethical approvals (institutional review board) and use of informed consent, as appropriate. Retrospective studies require a statement regarding institutional review board approval. The current study was performed with the approval of the Ethics Committee of The Third Affiliated Hospital of Qiqihar Medical University, Qiqihar Cancer Hospital. The animal experiments were strictly designed and performed according to the Guide for the Care and Use of Laboratory animals published by the US National Institutes of Health. Extensive efforts were made to ensure minimal suffering of the animals included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Huang, L., Zhang, Y., Zhao, L. et al. Ferrostatin-1 Polarizes Microglial Cells Toward M2 Phenotype to Alleviate Inflammation After Intracerebral Hemorrhage. Neurocrit Care 36, 942–954 (2022). https://doi.org/10.1007/s12028-021-01401-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-021-01401-2