Abstract
Background
Survivors of aneurysmal subarachnoid hemorrhage (SAH) face a protracted intensive care unit (ICU) course and are at risk for developing refractory hydrocephalus with the need for a permanent ventriculoperitoneal shunt (VPS). Management of the external ventricular drain (EVD) used to provide temporary cerebrospinal fluid diversion may influence the need for a VPS, ICU length of stay (LOS), and drain complications, but the optimal EVD management approach is unknown. Therefore, we sought to determine the effect of EVD discontinuation strategy on VPS rate.
Methods
This was a prospective multicenter observational study at six neurocritical care units in the United States. The target population included adults with suspected aneurysmal SAH who required an EVD. Patients were preassigned to rapid or gradual EVD weans based on their treating center. The primary outcome was the rate of VPS placement. Secondary outcomes were EVD duration, ICU LOS, hospital LOS, and drain complications.
Results
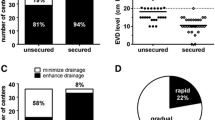
A rapid EVD wean protocol was associated with a lower rate of VPS placement, including a delayed posthospitalization shunt, in an adjusted Cox proportional analysis (hazard ratio 0.52 [p = 0.041]) and adjusted logistic regression model (odds ratio 0.43 [95% confidence interval 0.18–1.03], p = 0.057). A rapid wean was also associated with 2.1 fewer EVD days (p = 0.007) and saved an estimated 2.5 ICU days (p = 0.049), as compared with a gradual wean protocol. There were fewer nonfunctioning EVDs in the rapid group (odds ratio 0.32 [95% confidence interval 0.11–0.92]). Furthermore, we found that the time to first wean and the number of weaning attempts were important independent covariates that affected the likelihood of receiving a VPS and the duration of ICU admission.
Conclusions
A rapid EVD wean was associated with decreased rates of VPS placement, decreased ICU LOS, and decreased drain complications in survivors of aneurysmal SAH. These findings suggest that a randomized multicentered controlled study comparing rapid vs. gradual EVD weaning protocols is justified.




Similar content being viewed by others
References
Connolly ES Jr, Rabinstein AA, Carhuapoma JR, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/american Stroke Association. Stroke. 2012;43(6):1711–37.
Maher M, Schweizer TA, Macdonald RL. Treatment of spontaneous subarachnoid hemorrhage: guidelines and gaps. Stroke. 2020;51(4):1326–32.
Chung DY, Olson DM, John S, et al. Evidence-based management of external ventricular drains. Curr Neurol Neurosci Rep. 2019;19(12):94.
Chung DY, Abdalkader M, Nguyen TN. Aneurysmal subarachnoid hemorrhage. Neurol Clin. 2021;39(2):419–42.
Gigante P, Hwang BY, Appelboom G, et al. External ventricular drainage following aneurysmal subarachnoid haemorrhage. Br J Neurosurg. 2010;24(6):625–32.
Fried HI, Nathan BR, Rowe AS, et al. The insertion and management of external ventricular drains: an evidence-based consensus statement : a statement for healthcare professionals from the Neurocritical Care Society. Neurocrit Care. 2016;24(1):61–81.
Capion T, Lilja-Cyron A, Juhler M, Mathiesen TI, Wetterslev J. Prompt closure versus gradual weaning of extraventricular drainage for hydrocephalus in adult patients with aneurysmal subarachnoid haemorrhage: a systematic review protocol with meta-analysis and trial sequential analysis. BMJ Open. 2019;9(10):e029719.
Chung DY, Mayer SA, Rordorf GA. External Ventricular drains after subarachnoid hemorrhage: is less more? Neurocrit Care. 2018;28(2):157–61.
Merkler AE, Ch’ang J, Parker WE, Murthy SB, Kamel H. The rate of complications after ventriculoperitoneal shunt surgery. World Neurosurg. 2017;98:654–8.
Chung DY, Leslie-Mazwi TM, Patel AB, Rordorf GA. Management of external ventricular drains after subarachnoid hemorrhage: a multi-institutional survey. Neurocrit Care. 2017;26(3):356–61.
von Elm E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. PLoS Med. 2007;4(10):e296.
Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–81.
Harris PA, Taylor R, Minor BL, et al. The REDCap consortium: building an international community of software platform partners. J Biomed Inform. 2019;95:103208.
Rao SS, Chung DY, Wolcott Z, et al. Intermittent CSF drainage and rapid EVD weaning approach after subarachnoid hemorrhage: association with fewer VP shunts and shorter length of stay. J Neurosurg. 2019; pp. 1–6.
Ascanio LC, Gupta R, Adeeb N, et al. Relationship between external ventricular drain clamp trials and ventriculoperitoneal shunt insertion following nontraumatic subarachnoid hemorrhage: a single-center study. J Neurosurg. 2018;130(3):956–62.
Perry A, Graffeo CS, Kleinstern G, et al. Quantitative modeling of external ventricular drain output to predict shunt dependency in aneurysmal subarachnoid hemorrhage: cohort study. Neurocrit Care. 2020;33(1):218–29.
Graeb DA, Robertson WD, Lapointe JS, Nugent RA, Harrison PB. Computed tomographic diagnosis of intraventricular hemorrhage. Etiology and prognosis Radiology. 1982;143(1):91–6.
Czorlich P, Ricklefs F, Reitz M, et al. Impact of intraventricular hemorrhage measured by Graeb and LeRoux score on case fatality risk and chronic hydrocephalus in aneurysmal subarachnoid hemorrhage. Acta Neurochir (Wien). 2015;157(3):409–15.
Morgan TC, Dawson J, Spengler D, et al. The modified Graeb score: an enhanced tool for intraventricular hemorrhage measurement and prediction of functional outcome. Stroke. 2013;44(3):635–41.
Klopfenstein JD, Kim LJ, Feiz-Erfan I, et al. Comparison of rapid and gradual weaning from external ventricular drainage in patients with aneurysmal subarachnoid hemorrhage: a prospective randomized trial. J Neurosurg. 2004;100(2):225–9.
Jabbarli R, Pierscianek D, Rolz R, et al. Gradual external ventricular drainage weaning reduces the risk of shunt dependency after aneurysmal subarachnoid hemorrhage: a pooled analysis. Oper Neurosurg (Hagerstown). 2018;15(5):498–504.
Allan D. Intracranial pressure monitoring: a study of nursing practice. J Adv Nurs. 1989;14(2):127–31.
Olson DM, Lewis LS, Bader MK, et al. Significant practice pattern variations associated with intracranial pressure monitoring. J Neurosci Nurs. 2013;45(4):186–93.
Olson DM, Batjer HH, Abdulkadir K, Hall CE. Measuring and monitoring ICP in neurocritical care: results from a national practice survey. Neurocrit Care. 2014;20(1):15–20.
Olson DM, Zomorodi M, Britz GW, et al. Continuous cerebral spinal fluid drainage associated with complications in patients admitted with subarachnoid hemorrhage. J Neurosurg. 2013;119(4):974–80.
Amrhein V, Greenland S, McShane B. Scientists rise up against statistical significance. Nature. 2019;567(7748):305–7.
Schupper AJ, Eagles ME, Neifert SN, Mocco J, Macdonald RL. Lessons from the CONSCIOUS-1 study. J Clin Med. 2020;9(9):2970.
Acknowledgements
The authors thank Alexa Collins and Sara Gray (UTSW) for assistance with data collection and Matthew Cobler-Lichter, Joanna Yang, and Mabel Chung for helpful comments. Special thanks to Marek Mirski for helpful comments on the manuscript.
Funding
Dr. Chung and Dr. Locascio have received support from the National Institutes of Health (R25NS065743, KL2TR002542, and K08NS112601 to DYC and UL1TR001102 to JJL). This work was conducted with support from Harvard Catalyst | The Harvard Clinical and Translational Science Center (National Center for Advancing Translational Sciences, National Institutes of Health Award UL1TR002541) and financial contributions from Harvard University and its affiliated academic health care centers. The content is solely the responsibility of the authors and does not necessarily represent the official views of Harvard Catalyst, Harvard University and its affiliated academic healthcare centers, or the National Institutes of Health. Dr. Chung has also received support from the American Heart Association and American Stroke Association (18POST34030369), the Andrew David Heitman Foundation, the Aneurysm and AVM Foundation, and the Brain Aneurysm Foundation’s Timothy P. Susco and Andrew David Heitman Foundation Chairs of Research.
Author information
Authors and Affiliations
Contributions
DYC, BBT, MAK, AM, SSR, JJL, ABP, WM, DMO, SJ, and GAR conceptualized and designed the study. DYC, BBT, MAK, AM, SSR, AT, KK, WM, DMO, SJ, and GAR collected the data. DYC, AM, JHL, and JJL performed statistical analysis. DYC and JHL made the figures. DYC prepared the first draft of the article. All authors revised the article and gave approval of the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflicts of interest.
Ethical approval/informed consent
We adhered to ethical guidelines. Ethical approvals (institutional review board) were obtained. Use of informed consent was not applicable. Prospective observational studies require a statement regarding institutional review board approval, which we have obtained, as stated in the article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chung, D.Y., Thompson, B.B., Kumar, M.A. et al. Association of External Ventricular Drain Wean Strategy with Shunt Placement and Length of Stay in Subarachnoid Hemorrhage: A Prospective Multicenter Study. Neurocrit Care 36, 536–545 (2022). https://doi.org/10.1007/s12028-021-01343-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-021-01343-9