Abstract
Background
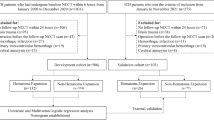
Identification of intracerebral hemorrhage (ICH) patients at risk of substantial hematoma expansion (SHE) could facilitate the selection of candidates likely to benefit from therapies aiming to minimize ICH growth. We aimed to develop a grading tool that can be quickly used during the hyperacute phase to predict the risk of SHE.
Methods
We reviewed data from 237 spontaneous ICH patients who had baseline head CT scan within 12 h of symptom onset and follow-up CT during the following 72 h. We performed logistic regression analyses to determine the predictors of SHE (defined as an absolute increase in ICH volume >6 ml or an increase >33 % on follow-up CT). We identified 6 predictors; each was assigned a point in the graphic interface of a nomogram which was used to construct a scoring system—The Hematoma Expansion Prediction (HEP) Score, varying from 0 to 18 points. We evaluated the ability of the model to predict the probability of SHE using c-statistics.
Results
SHE occurred in 74 patients (31.2 %). The final model to predict SHE included 6 variables: time from onset to baseline CT (<3 vs. 3–12 h), history of dementia, current smoking, antiplatelet use, Glasgow Comma Scale score, and the presence of subarachnoid hemorrhage on baseline scan. The model had satisfactory discrimination ability with a bootstrap corrected c-index of 0.76 (95 % CI 0.69–0.83) and good calibration. Patients with a total HEP score >3 were at greatest risk for SHE.
Conclusions
We developed and internally validated a novel nomogram and an easy to use score which accurately predict the probability of SHE based on six easily obtainable parameters. This could be useful for treatment decision and stratification. External prospective validation of the HEP score is warranted before its application to other populations.


Similar content being viewed by others
References
Delcourt C, Huang Y, Arima H, INTERACT1 Investigators, et al. Hematoma growth and outcomes in intracerebral hemorrhage: the INTERACT1 study. Neurology. 2012;79:314–9.
Vermeer SE, Algra A, Franke CL, Koudstaal PJ, Rinkel GJ. Long-term prognosis after recovery from primary intracerebral hemorrhage. Neurology. 2002;59:205–9.
Brott T, Broderick J, Kothari R, et al. Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke. 1997;28:1–5.
Leira R, Dávalos A, Silva Y, et al. Stroke Project, Cerebrovascular Diseases Group of the Spanish Neurological Society. Early neurologic deterioration in intracerebral hemorrhage: predictors and associated factors. Neurology. 2004;63:461–7.
Mayer SA, Brun NC, Begtrup K, Recombinant Activated Factor VII Intracerebral Hemorrhage Trial Investigators, et al. Recombinant activated factor VII for acute intracerebral hemorrhage. N Engl J Med. 2005;352:777–85.
Mayer SA, Brun NC, Begtrup K, FAST Trial Investigators, et al. Efficacy and safety of recombinant activated factor VII for acute intracerebral hemorrhage. N Engl J Med. 2008;358:2127–37.
Goldstein JN, Fazen LE, Snider R, et al. Contrast extravasation on CT angiography predicts hematoma expansion in intracerebral hemorrhage. Neurology. 2007;68:889–94.
Demchuk AM, Dowlatshahi D, Rodriguez-Luna D, et al. PREDICT/Sunnybrook ICH CTA study group. Prediction of haematoma growth and outcome in patients with intracerebral haemorrhage using the CT-angiography spot sign (PREDICT): a prospective observational study. Lancet Neurol. 2012;11:307–14.
Brouwers HB, Chang Y, Falcone GJ, et al. Predicting hematoma expansion after primary intracerebral hemorrhage. JAMA Neurol. 2014;71:158–64.
Iasonos A, Schrag D, Raj GV, Panageas KS. How to build and interpret a nomogram for cancer prognosis. J Clin Oncol. 2008;26:1364–70.
Kattan MW. Nomograms are superior to staging and risk grouping systems for identifying high-risk patients: preoperative application in prostate cancer. Curr Opin Urol. 2003;13:111–6.
Shariat SF, Karakiewicz PI, Suardi N, Kattan MW. Comparison of nomograms with other methods for predicting outcomes in prostate cancer: a critical analysis of the literature. Clin Cancer Res. 2008;14:4400–7.
Toyoda K, Okada Y, Minematsu K, et al. Antiplatelet therapy contributes to acute deterioration of intracerebral hemorrhage. Neurology. 2005;65:1000–4.
Kazui S, Naritomi H, Yamamoto H, Sawada T, Yamaguchi T. Enlargement of spontaneous intracerebral hemorrhage. Incidence and time course. Stroke. 1996;27:1783–7.
Hussein HM, Tariq NA, Palesch YY, Qureshi AI, ATACH Investigators. Reliability of hematoma volume measurement at local sites in a multicenter acute intracerebral hemorrhage clinical trial. Stroke. 2013;44:237–9.
Romero JM, Brouwers HB, Lu J, et al. Prospective validation of the computed tomographic angiography spot sign score for intracerebral hemorrhage. Stroke. 2013;44:3097–102.
Brouwers HB, Biffi A, Ayres AM, et al. Apolipoprotein E genotype predicts hematoma expansion in lobar intracerebral hemorrhage. Stroke. 2012;43:1490–5.
Barras CD, Tress BM, Christensen S, Recombinant Activated Factor VII Intracerebral Hemorrhage Trial Investigators, et al. Density and shape as CT predictors of intracerebral hemorrhage growth. Stroke. 2009;40:1325–31.
Dowlatshahi D, Smith EE, Flaherty ML, Ali M, Lyden P, Demchuk AM, VISTA Collaborators. Small intracerebral haemorrhages are associated with less haematoma expansion and better outcomes. Int J Stroke. 2011;6:201–6.
Cucchiara B, Messe S, Sansing L, Kasner S, Lyden P, CHANT Investigators. Hematoma growth in oral anticoagulant related intracerebral hemorrhage. Stroke. 2008;39:2993–6.
Broderick JP, Diringer MN, Hill MD, Recombinant Activated Factor VII Intracerebral Hemorrhage Trial Investigators, et al. Determinants of intracerebral hemorrhage growth: an exploratory analysis. Stroke. 2007;38:1072–5.
Maruishi M, Shima T, Okada Y, Nishida M, Yamane K. Involvement of fluctuating high blood pressure in the enlargement of spontaneous intracerebral hematoma. Neurol Med Chir (Tokyo). 2001;41:300–4.
Fujii Y, Takeuchi S, Sasaki O, Minakawa T, Tanaka R. Multivariate analysis of predictors of hematoma enlargement in spontaneous intracerebral hemorrhage. Stroke. 1998;29:1160–6.
Rodriguez-Luna D, Piñeiro S, Rubiera M, et al. Impact of blood pressure changes and course on hematoma growth in acute intracerebral hemorrhage. Eur J Neurol. 2013;20:1277–83.
Takeda R, Ogura T, Ooigawa H, et al. A practical prediction model for early hematoma expansion in spontaneous deep ganglionic intracerebral hemorrhage. Clin Neurol Neurosurg. 2013;115:1028–31.
Brouwers HB, Falcone GJ, McNamara KA, et al. CTA spot sign predicts hematoma expansion in patients with delayed presentation after intracerebral hemorrhage. Neurocrit Care. 2012;17:421–8.
Rodriguez-Luna D, Rubiera M, Ribo M, et al. Serum low-density lipoprotein cholesterol level predicts hematoma growth and clinical outcome after acute intracerebral hemorrhage. Stroke. 2011;42:2447–52.
Kuramatsu JB, Mauer C, Kiphuth IC, et al. Reported antiplatelet use influences long-term outcome independently in deep intracerebral hemorrhage. Neurosurgery. 2012;70:342–50.
Silva Y, Leira R, Tejada J, Lainez JM, Castillo J, Dávalos A, Stroke Project, Cerebrovascular Diseases Group of the Spanish Neurological Society. Molecular signatures of vascular injury are associated with early growth of intracerebral hemorrhage. Stroke. 2005;36:86–91.
Rincon F, Lyden P, Mayer SA. Relationship between temperature, hematoma growth, and functional outcome after intracerebral hemorrhage. Neurocrit Care. 2013;18:45–53.
Yildiz OK, Arsava EM, Akpinar E, Topcuoglu MA. Previous antiplatelet use is associated with hematoma expansion in patients with spontaneous intracerebral hemorrhage. J Stroke Cerebrovasc Dis. 2012;21:760–6.
Kazui S, Minematsu K, Yamamoto H, Sawada T, Yamaguchi T. Predisposing factors to enlargement of spontaneous intracerebral hematoma. Stroke. 1997;28:2370–5.
Becker KJ, Baxter AB, Bybee HM, Tirschwell DL, Abouelsaad T, Cohen WA. Extravasation of radiographic contrast is an independent predictor of death in primary intracerebral hemorrhage. Stroke. 1999;30:2025–32.
Lim JK, Hwang HS, Cho BM, et al. Multivariate analysis of risk factors of hematoma expansion in spontaneous intracerebral hemorrhage. Surg Neurol. 2008;69:40–5.
Huynh TJ, Demchuk AM, Dowlatshahi D, et al. PREDICT/Sunnybrook ICH CTA Study Group. Spot sign number is the most important spot sign characteristic for predicting hematoma expansion using first-pass computed tomography angiography: analysis from the PREDICT study. Stroke. 2013;44:972–7.
Sullivan L, Massaro J, D’Agostino R. Presentation of multivariate data for clinical use: the Framingham Study risk score functions. Stat Med. 2004;23:1631–60.
Lou M, Al-Hazzani A, Goddeau RP Jr, Novak V, Selim M. Relationship between white-matter hyperintensities and hematoma volume and growth in patients with intracerebral hemorrhage. Stroke. 2010;41:34–40.
Martí-Fàbregas J, Delgado-Mederos R, Granell E, RENEVAS group (Stroke Research Network, RETICS, Instituto de Salud Carlos III), et al. Microbleed burden and hematoma expansion in acute intracerebral hemorrhage. Eur Neurol. 2013;70:175–8.
Feigin VL, Rinkel GJ, Lawes CM, et al. Risk factors for subarachnoid hemorrhage: an updated systematic review of epidemiological studies. Stroke. 2005;36:2773–80.
Kurth T, Kase CS, Berger K, Schaeffner ES, Buring JE, Gaziano JM. Smoking and the risk of hemorrhagic stroke in men. Stroke. 2003;34:1151–5.
Finelli PF. Cerebral amyloid angiopathy as cause of convexity SAH in elderly. Neurologist. 2010;16:37–40.
Viswanathan A, Greenberg SM. Cerebral amyloid angiopathy in the elderly. Ann Neurol. 2011;70:871–80.
Acknowledgments
Dr. Yao is supported by a grant from a scholarship from Renji Hospital in Shanghai, China; Dr. Selim is partly supported by the NIH/NINDS (U01 NS074425).
Disclosures
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yao, X., Xu, Y., Siwila-Sackman, E. et al. The HEP Score: A Nomogram-Derived Hematoma Expansion Prediction Scale. Neurocrit Care 23, 179–187 (2015). https://doi.org/10.1007/s12028-015-0147-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-015-0147-4