Abstract
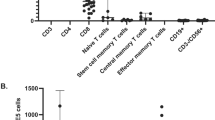
Sickle cell disease (SCD) is associated with alterations in immune phenotypes. CD4+CD28null T lymphocytes have pro-inflammatory functions and are linked to vascular diseases. To assess the percentage of CD4+CD28null T lymphocytes, natural killer cells (NK), and IFN-gamma levels, we compared 40 children and adolescents with SCD with 40 healthy controls and evaluated their relation to disease severity and response to therapy. Patients with SCD steady state were studied, focusing on history of frequent vaso-occlusive crisis, hydroxyurea therapy, and IFN-gamma levels. Analysis of CD4+CD28null T lymphocytes and NK cells was done by flow cytometry. Liver and cardiac iron overload were assessed. CD4+CD28null T lymphocytes, NK cells, and IFN-gamma levels were significantly higher in patients than controls. Patients with history of frequent vaso-occlusive crisis and those with vascular complications had higher percentage of CD4+CD28null T lymphocytes and IFN-gamma while levels were significantly lower among hydroxyurea-treated patients. CD4+CD28null T lymphocytes were positively correlated to transfusional iron input while these cells and IFN-gamma were negatively correlated to cardiac T2* and duration of hydroxyurea therapy. NK cells were correlated to HbS and indirect bilirubin. Increased expression of CD4+CD28null T lymphocytes highlights their role in immune dysfunction and pathophysiology of SCD complications.





Similar content being viewed by others
References
Belcher JD, Chunsheng Chen C, Nguyen J, Milbauer L, Abdulla F, Alayash AI. Heme triggers TLR4 signaling leading to endothelial cell activation and vaso-occlusion in murine sickle cell disease. Blood. 2014;123:377–90.
Holtzclaw JD, Jack D, Aguayo SM, Eckman JR, Roman J, Hsu LL. Enhanced pulmonary and systemic response to endotoxin in transgenic sickle mice. Am J Respir Crit Care Med. 2004;169:687–95.
Nickel RS, Osunkwo I, Garrett A, Robertson J, Archer DR, Promislow DE, et al. Immune parameter analysis of children with sickle cell disease on hydroxycarbamide or chronic transfusion therapy. Br J Haematol. 2015;169:574–83.
Luckheeram RV, Zhou R, Verma AD, Xia B. CD4+T cells: differentiation and functions. Clin Dev Immunol. 2012;2012:925135.
Ojo OT, Shokunbi WA. CD4+ T lymphocytes count in sickle cell anaemia patients attending a tertiary hospital. Niger Med J. 2014;55:242–5.
Vallejo AN, Weyand CM, Goronzy JJ. T-cell senescence: a culprit of immune abnormalities in chronic inflammation and persistent infection. Trends Mol Med. 2004;10:119–24.
Ingrid ED, Ernesto TA, Christina B, Juan CK. CD4+CD28null T cells in coronary artery disease: when helpers become killers. Cardiovasc Res. 2009;81:11–9.
Dumitriu IE. The life (and death) of CD4+ CD28(null) T cells in inflammatory diseases. Immunology. 2015;146:185–93.
Dumitriu IE, Baruah P, Finlayson CJ, Loftus IM, Antunes RF, Lim P, et al. High levels of costimulatory receptors OX40 and 4-1BB characterize CD4+CD28null T cells in patients with acute coronary syndrome. Circ Res. 2012;110:857–69.
Vivier E, Raulet DH, Moretta A, Caligiuri MA, Zitvogel L, Lanier LL, et al. Innate or adaptive immunity? The example of natural killer cells. Science. 2011;331:44–9.
Borrego F, Masilamani M, Marusina AI, Tang X, Coligan JE. The CD94/NKG2 family of receptors: from molecules and cells to clinical relevance. Immunol Res. 2006;35:263–78.
Kirwan SE, Burshtyn DN. Regulation of natural killer cell activity. Curr Opin Immunol. 2007;19:46–54.
Segal BM. The role of natural killer cells in curbing neuroinflammation. J Neuroimmunol. 2007;191:2–7.
Damodar T, Kuruvilla TS, Kithan L. Natural killer cells: now and future. Experiment. 2014;25:1717–25.
Giubilato S, Liuzzo G, Brugaletta S, Pitocco D, Graziani F, Smaldone C, et al. Expansion of CD4+CD28null T-lymphocytes in diabetic patients: exploring new pathogenetic mechanisms of increased cardiovascular risk in diabetes mellitus. Eur Heart J. 2011;32:1214–26.
El-Samahy MH, Tantawy AA, Adly AA, Habeeb NM, Ismail EA, Hamed GM, et al. Expression of CD4+ CD28null T lymphocytes in children and adolescents with type 1 diabetes mellitus: relation to microvascular complications, aortic elastic properties, and carotid intima media thickness. Pediatr Diabetes. 2017;18:785–93.
Wethers DL. Sickle cell disease in childhood: part I. Laboratory diagnosis, pathophysiology and health maintenance. Am Fam Physician. 2000;62:1013–20.
Kwiatkowski JL. Hemoglobinopathies. In: Lanzkowsky P, editor. Manual of pediatric hematology and oncology. 5th ed. London: Elsevier; 2011. p. 221.
van Beers EJ, Schaap MCL, Berkmans RJ, Nieuwland R, Sturk A, van Doormaal FF, et al. CURAMA study group. Circulating erythrocyte-derived microparticles are associated with coagulation activation in sickle cell disease. Haematologica. 2009;94:1513–9.
Darbari DS, Onyekwere O, Nouraie M, Minniti CP, Luchtman-Jones L, Rana S, et al. Markers of severe vaso-occlusive painful episode frequency in children and adolescents with sickle cell anemia. J Pediatr. 2012;160:286–90.
Bernini JC, Rogers ZR, Sandler ES, Reisch JS, Quinn CT, Buchanan GR. Beneficial effect of intravenous dexamethasone in children with mild to moderately severe acute chest syndrome complicating sickle cell disease. Blood. 1998;92:3082–9.
Pashankar FD, Carbonella J, Bazzy-Asaad A, Friedman A. Prevalence and risk factors of elevated pulmonary artery pressures in children with sickle cell disease. Pediatrics. 2008;121:777–82.
Cappellini MD, Cohen A, Eleftheriou A, Eleftheriou A, Piga Aorter J, Taher A. Guidelines for the clinical management of Thalassaemia [Internet]. 2nd revised edition. Nicosia (CY): Thalassaemia International Federation; 2008. Chapter 2, Blood transfusion therapy in β-Thalassaemia major. Available from: https://www.ncbi.nlm.nih.gov/books/NBK173967/.
Vermylen C. What is new in iron overload? Eur J Pediatr. 2008;167:377–81.
Silvilairat S, Sittiwangkul R, Pongprot Y, Charoenkwan P, Phornphutkul C. Tissue doppler echocardiography reliably reflects severity of iron overload in pediatric patients with beta thalassemia. Eur J Echocardiogr. 2008;9:368–72.
Morice WG. The immunophenotypic attributes of NK cells and NK-cell lineage lymphoproliferative disorders. Am J Clin Pathol. 2007;127:881–6.
El-Rashedy FH, El-Hawy MA, Helwa MA, Abd-Allah SS. Study of CD4+, CD8+, and natural killer cells (CD16+, CD56+) in children with immune thrombocytopenic purpura. Hematol Oncol Stem Cell Ther. 2017;10:8–14.
Hankins JS, McCarville MB, Loeffler RB, Smeltzer MP, Onciu M, Hoffer FA, et al. R2* magnetic resonance imaging of the liver in patients with iron overload. Blood. 2009;113:4853–5.
Olivieri NF. Progression of iron overload in sickle cell disease. Semin Hematol. 2001;38:57–62.
Musallam KM, Cappellini MD, Wood JC, Motta I, Graziadei G, Tamim H, et al. Elevated liver iron concentration is a marker of increased morbidity in patients with β thalassemia intermedia. Haematologica. 2011;96:1605–12.
Carpenter JP, He T, Kirk P, Roughton M, Anderson LJ, de Noronha SV, et al. On T2* magnetic resonance and cardiac iron. Circulation. 2011;123:1519–28.
Anderson LJ, Holden S, Davis B, Prescott E, Charrier CC, Bunce NH, et al. Cardiovascular T2-star (T2*) magnetic resonance for the early diagnosis of myocardial iron overload. Eur Heart J. 2001;22:2171–9.
Merchant R, Joshi A, Ahmed J, Krishnan P, Jankharia B. Evaluation of cardiac iron load by cardiac magnetic resonance in thalassemia. Indian Pediatr. 2011;48:697–701.
Platt O. Sickle cell anemia as an inflammatory disease. J Clin Invest. 2000;106:337–8.
Maly K, Schirmer M. The story of CD4+CD28− T cells revisited: solved or still ongoing? J Immunol Res. 2015;2015:348746.
Mandal A, Viswanathan C. Natural killer cells: in health and disease. Hematol. 2015;8:47–55.
West M, Wethers D, Smith J, Steinberg M. Laboratory profile of sickle cell disease: a cross-sectional analysis. J Clin Epidemiol. 1992;45:893–909.
Lard LR, Mul FP, de Haas M, Roos D, Duits AJ. Neutrophil activation in sickle cell disease. J Leukoc Biol. 1999;66:411–5.
Wallace KL, Marshall MA, Ramos SI, Lannigan JA, Field JJ, Strieter RM, et al. NKT cells mediate pulmonary inflammation and dysfunction in murine sickle cell disease through production of IFN-gamma and CXCR3 chemokines. Blood. 2009;114:667–76.
Polanowska-Grabowska R, Wallace K, Field JJ, Chen L, Marshall MA, Figler R, et al. P-Selectin-mediated platelet-neutrophil aggregate formation activates neutrophils in mouse and human sickle cell disease. Arterioscler Thromb Vasc Biol. 2010;30:2392–9.
Omoti CE. Haematological values in sickle cell anaemia in steady state and during vaso-occlusive crises in Benin City. Niger Ann Afr Med. 2005;4:62–7.
Akinbami A, Dosunmu A, Adediran A, Oshinaike O, Adebola P, Arogundade O. Haematological values in homozygous sickle cell disease in steady state and haemoglobin phenotypes AA controls in Lagos, Nigeria. BMC Res Notes. 2012;5:396–402.
Koffi KG, Sawadogo D, Meite M, Nanho DC, Tanoh ES, Attia AK, et al. Reduced levels of T-cell subsets CD4+ and CD8+ in homozygous sickle cell anaemia patients with splenic defects. Hematol J. 2003;4:363–5.
Serjeant GR. The natural history of sickle cell disease. Cold Spring Harb Perspect Med. 2013;3:a011783.
Musa BO, Onyemelukwe GC, Hambolu JO, Mamman AI, Isa AH. Pattern of serum cytokine expression and T-cell subsets in sickle cell disease patients in vaso-occlusive crisis. Clin Vaccine Immunol. 2010;17(4):602–8.
Frenette PS. Sickle cell vaso-occlusion: multistep and multicellular paradigm. Curr Opin Hematol. 2002;9:101–6.
Pitanga T, Vilas-Boas W, Cerqueira B, Seixas M, Barbosa C, Adorno E, et al. Cytokine profiles in sickle cell anemia: pathways to be unraveled. Adv Biosci Biotechnol. 2013;4:6–12.
Brennan PJ, Tatituri RV, Brigl M, Kim EY, Tuli A, Sanderson JP, et al. Invariant natural killer T cells recognize lipid self antigen induced by microbial danger signals. Nat Immunol. 2011;12:1202–11.
Stetson DB, Mohrs M, Reinhardt RL, Baron JL, Wang ZE, Gapin L, et al. Constitutive cytokine mRNAs mark natural killer (NK) and NK T cells poised for rapid effector function. J Exp Med. 2003;198:1069–76.
Field JJ, Lin G, Okam MM, Majerus E, Keefer J, Onyekwere O, et al. Sickle cell vaso-occlusion causes activation of iNKT cells that is decreased by the adenosine A2A receptor agonist regadenoson. Blood. 2013;121:3329–34.
Kaaba SA, Al Fazaa L. F cells, fetal hemoglobin levels, lymphocyte subsets, and frequency of crises in sickle-cell disease in Kuwait. Ann Hematol. 2000;79:291–5.
Mosmann TR. Cytokine secretion patterns and the cross regulation of T cell subsets. Immunol Res. 1991;10:183–8.
Van Parijs L, Abbas AK. Homeostasis and self tolerance in the immune system: turning lymphocytes off. Science. 1998;280:243–8.
Charache S, Terrin ML, Moore RD, Dover GJ, Barton FB, Eckert SV, et al. Effect of hydroxyurea on frequency of painful crises in sickle cell anemia. N Engl J Med. 1995;332:1317–22.
Wang WC, Ware RE, Miller ST, Iyer RV, Casella JF, Minniti CP, et al. Hydroxycarbamide in very young children with sickle-cell anaemia: a multicentre, randomised, controlled trial (BABY HUG). Lancet. 2011;377:1663–72.
Goncalves MS, Queiroz IL, Cardoso SA, Zanetti A, Strapazoni AC, Adorno E, et al. Interleukin 8 as a vaso-occlusive marker in Brazilian patients with sickle cell disease. Braz J Med Biol Res. 2001;34:1309–13.
Wun T. The role of inflammation and leukocytes in the pathogenesis of sickle cell disease; haemoglobinopathy. Hematology. 2001;5:403–12.
Wallace KL, Linden J. Adenosine A2A receptors induced on iNKT and NK cells reduce pulmonary inflammation and injury in mice with sickle cell disease. Blood. 2010;116:5010–20.
Acknowledgements
The manuscript has not been submitted elsewhere nor previously published.
Author information
Authors and Affiliations
Contributions
The corresponding author, on behalf of all authors, hereby states that all authors have contributed to the manuscript in significant ways and have reviewed and agreed upon the manuscript content.
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
ElAlfy, M.S., Adly, A.A.M., Ebeid, F.S.E. et al. Immunological role of CD4+CD28null T lymphocytes, natural killer cells, and interferon-gamma in pediatric patients with sickle cell disease: relation to disease severity and response to therapy. Immunol Res 66, 480–490 (2018). https://doi.org/10.1007/s12026-018-9010-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-018-9010-y