Abstract
Purpose
The management of primary hyperparathyroidism (PHPT) during pregnancy may be surgical or conservative. This study compared adverse outcomes between surgical and non-surgical treatments. Additionally, the study investigated the correlation between serum calcium values and complication rates.
Methods
A systematic review of retrospective studies, case series, and case reports. Biochemical parameters, interventions, and outcomes of each pregnancy were recorded. The study population comprised two groups: the non-surgical and surgical groups. Adverse outcomes were categorized as maternal, obstetric, or neonatal.
Results
The surgical and non-surgical groups consisted of 163 and 185 patients, respectively. A positive correlation was observed between the mean maternal gestational calcium value and both maternal and obstetric complication. Neonatal complications were more prevalent in patients treated conservatively across all maternal calcium values (p < 0.001). No significant differences were observed in maternal outcomes and overall obstetric outcomes between the study groups, albeit a higher mean serum calcium value in the surgical group (12.3 mg/dL) compared with the non-surgical group (11.1 mg/dL).
Conclusions
Given the significantly lower neonatal adverse outcomes in the non-surgical group compared to the surgical group, along with non-inferior maternal and obstetric outcomes in the surgical group, the overall data of this study suggest that parathyroidectomy is favorable to non-surgical management even in cases of mild hypercalcemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary hyperparathyroidism (PHPT) is a relatively rare condition to encounter in women of reproductive age, with an estimated rate of 7.7–50 cases per 100,000 women of this population [1, 2].
Pregnancy is characterized by physiological changes in calcium metabolism which must be considered: calcium absorption increases twofold by third trimester, driven by vitamin D and parathyroid hormone-related protein (PTHrP). The latter is synthesized during pregnancy from the amnion, as well as breasts to lesser extent, and other reproductive tissues [3]. PTHrP acts similarly to parathyroid hormone (PTH), promoting epithelial growth and tissue differentiation in the fetus and acting as the primary stimulus for the active placental calcium pump [3]. Total serum calcium values decrease during pregnancy due to the increased intravascular volume, calcium placental efflux, and increased urinary output. Finally, ionized calcium levels remain unchanged, and PTH falls to the low-normal range [4,5,6,7].
The etiology of gestational PHPT is most often a parathyroid adenoma, and less commonly parathyroid hyperplasia (5–10%) or parathyroid carcinoma (<1%) [8, 9]. PHPT may also occur as part of an inherited syndrome, and genetic counseling has been recommended for patients younger than 40 carrying the disease [10, 11].
PHPT may be managed conservatively or surgically. Conservative treatment is typically recommended for asymptomatic patients, or those with mild hypercalcemia, or as a bridge to surgery. It includes close follow-up, electrolyte, and hormonal monitoring, along with hydration alone in mild to moderate patients or additional pharmacological therapy in cases of refractory hypercalcemia [7, 12, 13]. The definitive treatment for this condition is parathyroidectomy, which can be performed via cervical exploration or minimally invasive parathyroidectomy (MIP). [9, 14] Reports of successful ablation of the gland are also documented [15,16,17].
Data regarding pregnancy complication rates from gestational PHPT are variable. Norman et al. reported a significant difference in pregnancy loss in gestational PHPT [18], and citations across the literature claim complications of PHPT during pregnancy may reach as high as 67% of mothers and 80% of offspring [19,20,21]. However, more recent large cohorts have reported no increased risk of obstetric complications [22, 23]. Although several studies have shown increased risk of complications in non-surgical treatment compared to surgical treatment, current guidelines suggest surgery only when the patient is either symptomatic or with hypercalcemia exceeding 1 mg/dL above the normal limits [7, 24]. Similarly, surgical safety is controversial. While some studies conclude that surgery during pregnancy causes more adverse events than surgery on non-pregnant patients [25, 26], others conclude that the risks of parathyroidectomy are minimal, hence surgery should not be delayed when necessary [27,28,29,30]. A recent Chinese expert consensus concluded surgery should be considered regardless of the stage of pregnancy when hypercalcemia appears hazardous to the patient or fetus [7]. In mind of the above controversies, the current study compared the complication rates between surgical and non-surgical managements, utilizing all the relevant published data available.
Methods
Study design
A literature search on PubMed, ScienceDirect (Elsevier), and Google Scholar was performed using the terms: “pregnancy” or “gestation”, “hyperparathyroidism”, “PHPT”, and “parathyroidectomy”. Database included published studies between 1980 and 2023. The study population comprised of women who experienced primary hyperparathyroidism (PHPT) during pregnancy and either underwent parathyroidectomy during pregnancy (surgical group) or were managed conservatively (non-surgical group). Recorded data included the patient’s age, biochemical values, obstetric and medical history, time of diagnosis, etiology, presenting symptoms, management, and complications, which were subsequently classified as maternal, obstetric, or neonatal. We excluded reports involving significant comorbidities, such as metastatic non-parathyroid cancer or any condition unrelated to PHPT severe enough to require management in the intensive care unit (ICU) during pregnancy, reports with missing data, and patients treated with alternative management not addressed in this article’s scope. We excluded cases with calcium values exceeding 15 mg/dl as these were deemed rare and complex, leading to higher complication rates and outcome bias. Additionally, we excluded records involving ectopic parathyroid adenomas, parathyroid carcinomas, and patients positive for multiple endocrine neoplasia type 1 (MEN1) as these rare cases were correlated with extended hospital stays, alternative management strategies, and complicated outcomes.
Data collection
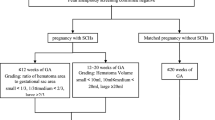
The initial search yielded 777 articles, manually filtered to identify 259 relevant articles for screening. Following the screening process for duplications and exclusion criteria, 168 publications were selected, comprising 348 cases for data analysis (as depicted in the PRISMA flow diagram in Fig. 1). Each pregnancy was analyzed as a single case. Maternal, obstetric, and neonatal complications were considered as adverse outcomes that occurred solely during pregnancy or shortly after delivery. Hypercalcemia was defined as total serum calcium exceeding 10.5 mg/dL. Normal range for PTH were defined as 10–65 pg/mL. Calcium values utilized for analysis represented the average of total serum calcium values measured during pregnancy, as ionized calcium was not consistently reported in a significant number of articles. In cases where albumin levels were provided or corrected calcium values were available, the corrected values were utilized for analysis.
Statistical analysis
Analysis was performed by the Beer-Sheva Faculty of Health Sciences in Israel using Windows GraphPad Prism version 10.2.2. Demographic data is expressed as either raw values or medians and interquartile ranges (IQR) when data did not follow a normal distribution. Statistical significance was assumed as p < 0.05. Differences in complication rates were calculated using the t-test was for quantitative data, and chi-square test for categorical data. Correlation between calcium rates and complication rates was calculated using Pearson’s correlation.
Results
Out of the 348 cases analyzed, 163 (47%) underwent parathyroidectomy (the surgical group), while 185 (53%) were managed conservatively (the non-surgical group). The mean ages were 31 ± 3 and 31.5 ± 3.5 years, respectively. Average total calcium levels for the surgical group were higher, with a median of 12.3 mg/dL (range:11.5–13.3), compared to 11.1 mg/dL (range: 10.7–11.6) in the non-surgical group. Median PTH levels were 137 pg/mL (range: 94–237) and 123 pg/mL (range:71–224) for the respective groups. 61% of the surgical group underwent surgery during the second trimester, 25% during the third trimester, and 7% during the first trimester. (see Table 1)
In the non-surgical group, most patients were treated using IV fluids. Data regarding specific therapeutic agents and their outcomes were missing for most cases; 18 patients received furosemide, an additional 18 received calcitonin and 15 patients received cinacalcet. Positive results to treatment were described in only 17 patients. Thus, statistically significant results regarding the efficacy of different pharmacological regimens could not be achieved.
Maternal, obstetric, and neonatal complication rates comparing the study arms are presented in Table 2 with the following results: Maternal complications occurred in 19.5% of the entire study population. No significant differences in maternal complication rates were observed between the study arms. The overall obstetric complications were not significantly different between study groups as well, however, subcategory analysis revealed higher rates of preeclampsia/eclampsia and preterm labor in the non-surgical group and higher rates of hyperemesis gravidarum in the surgical group. Rates of pregnancy loss were higher in the non-surgical group, with 15.3% compared to 1.3% in the surgical group. From a total of 22 cases of pregnancy loss, 10 cases described 1st-trimester miscarriage, and the rest did not specify further details. Numbers of neonatal complications were significantly higher in the non-surgical group compared to the surgical group. This difference was evident in transient neonatal hypocalcemia (24.4% vs. 2.7%), hypocalcemic tetany (10.7% vs. none), hypocalcemic convulsions (6.9% vs. none), and ICU admissions (9.9% vs. 3.3%), but not neonatal demise.
A statistically significant positive correlation was observed between serum calcium values and both maternal and obstetric complication rates (p < 0.05), but not neonatal complications (Table 3). Nevertheless, complication rates in the non-surgical group were significantly higher across all calcium levels compared with the surgical group (with p < 0.001, as illustrated in Fig. 2).
Discussion
Maternal complications
Maternal complications affected 19.5% of the study population in the current study, with no significant difference in complication rates between the surgical and non-surgical groups. Interestingly, maternal complications in the surgical group were not elevated despite the higher mean serum calcium levels. This outcome could potentially be attributed to parathyroidectomy. The variations in calcium levels between the study groups most likely stem from the selection of patients in the higher spectrum of mean serum calcium towards surgical intervention, rather than non-surgical management. Schnatz et al. hypothesized that adverse outcomes in patients selected for surgical intervention could stem from underlying long-term untreated disease rather than from surgery itself [31, 32]. The risk of surgery has been reported to be minimal [28, 33,34,35], with curative results in 95–98% of cases [9, 14, 36, 37]. In the present study, the operation was curative in 98% of cases, with postoperative complications occurring in 4.9%. Specifically, three patients experienced hungry bone syndrome, three suffered from hypocalcemic tetany, one patient had permanent hypoparathyroidism, and one patient experienced transient vocal cord palsy.
Obstetric complications
Obstetric complications resulted in significant differences on a few parameters, namely, preterm delivery, preeclampsia, and pregnancy loss, which occurred at higher rates in the non-surgical group. Additionally, hyperemesis gravidarum occurred at higher rates in the surgical group, most likely due to the early diagnosis of their symptomatic disease and subsequent selection for surgical intervention (Table 2). Analysis of the data presented in this article suggests that the increase in pregnancy loss arises from losses that occurred in the first trimester and early second trimester before potential surgical intervention. Consequently, these instances were categorized under the non-surgical group. The pregnancy loss rate for the entire study population was 7.8%, lower than the documented 15% rate for women in the general population aged 30–34 [38, 39]. Overall, the current study findings suggest that parathyroidectomy did not significantly alter the overall rates of obstetric complications when compared to non-surgical management, aligning with the conclusions reported previously by Hirsch et al. [23] and Abood and Vestergaard [22], however, it may potentially be associated to a reduced risk of preterm delivery and preeclampsia.
Neonatal complications
Neonatal adverse outcomes were significantly more prevalent in the non-surgical group than in the surgical group. The significant difference was evident across all maternal mean calcium values (Fig. 2). These results are supported by previously reported data [30, 40, 41]. Sandler et al. that revealed that even in asymptomatic PHPT, infant complications were less prevalent in the surgical group [41]. The variation in adverse outcomes between the groups primarily consisted of transient postpartum hypocalcemia, hypocalcemic tetany, convulsions, and subsequently, a higher number of ICU admissions. Neonatal hypocalcemia can be severe and prolonged, often necessitating long-term calcium supplementation [42], with median onset of clinical manifestations at the 11th day postpartum [7]. Although a significant correlation was observed between calcium values and maternal and obstetric adverse outcomes, no correlation was seen between neonatal complications and mean maternal gestational calcium values, indicating that neonatal adverse outcomes result from complex interactions beyond mean calcium values alone. Neonatal hypocalcemia is attributed to the suppression of parathyroid glands in utero. After birth, the neonate relies on kidney reabsorption and intestinal absorption, facilitated by an active PTH and calcitriol-dependent mechanism [3]. However, the suppressed parathyroid glands are unable to meet the increased demand, leading to hypocalcemia within the first days to weeks after delivery. During gestation, most calcium is actively transported through the placenta, regulated by PTHrP. 80% of mineral requirements reaches the fetus during the third trimester of pregnancy [7, 43]. Notably, PTH itself does not cross the placenta, and it remains uncertain whether the hormone affects the transfer of calcium through the placenta based on animal models [3]. In this study, most patients in the surgical group underwent parathyroidectomy during the second trimester, indicating their mean gestational calcium during the third trimester remained within normal values. This observation could potentially account for the reduced risk of postpartum neonatal hypocalcemia and its sequelae in the surgical group. However, the limited number of cases specifying post-operative and subsequent gestational serum calcium values made it challenging to draw statistically significant conclusions. Similarly, due to data unavailability, it was impossible to compare the efficacy and outcomes between different non-surgical treatment regimens. Future prospective studies may investigate whether reduced third-trimester calcium values correlate with lower rates of neonatal complications, preferably utilizing ionized calcium, as this marker is more reliable during pregnancy, and compare it with the outcomes of non-surgical management.
Conclusions
Adverse neonatal outcomes were significantly fewer in the surgical group than in the non-surgical group. This difference was evident across all mean maternal gestational calcium values, suggesting that surgical intervention may yield superior neonatal outcomes, regardless of maternal calcium values. Maternal and overall obstetric complication rates did not significantly differ between the study groups. Additionally, the present study identified a positive correlation between maternal and obstetric outcomes and mean maternal gestational calcium levels, consistent with previously published findings. Given the superior neonatal outcomes alongside non-inferior maternal and obstetric outcomes, the overall data presented in this study suggest that parathyroidectomy is favorable over conservative treatment, even in cases of mild primary hyperparathyroidism.
Limitations
The primary limitation of this study was the compilation of a patient database from published sources comprising retrospective studies, case series, and case reports. This method introduced a selection bias toward more severe cases, typically reported in the literature. However, this bias is partially mitigated by including 249 cases identified through retrospective reviews. Nevertheless, it cannot be ruled out that asymptomatic patients and those with PHPT within the normocalcemic range may exhibit lower complication rates than those documented in this study.
Data availability
This article has utilized data from widely available, previously published data. All data supporting the findings of this study are available within the paper and its supplementary information which is available in an online repository (https://doi.org/10.17632/6vjfskyvzc.2). The Search algorithm is depicted in Table 1, and anonymous case data is in Table 2 of the online repository.
References
M.W. Yeh, P.H.G. Ituarte, H.C. Zhou, S. Nishimoto, I.-L. Amy Liu, A. Harari et al. Incidence and prevalence of primary hyperparathyroidism in a racially mixed population. J. Clin. Endocrinol. Metab. 98, 1122–1129 (2013). https://doi.org/10.1210/jc.2012-4022
S.H. Golden, K.A. Robinson, I. Saldanha, B. Anton, P.W. Ladenson, Prevalence and incidence of endocrine and metabolic disorders in the United States: a comprehensive review. J. Clin. Endocrinol. Metab. 94, 1853–1878 (2009). https://doi.org/10.1210/jc.2008-2291
C.S. Kovacs, The role of PTHrP in regulating mineral metabolism during pregnancy, lactation, and fetal/neonatal development. Clin. Rev. Bone Miner. Metab. 12, 142–164 (2014). https://doi.org/10.1007/s12018-014-9157-6
J. Bollerslev, L. Rejnmark, A. Zahn, A. Heck, N.M. Appelman-Dijkstra, L. Cardoso et al. European expert consensus on practical management of specific aspects of parathyroid disorders in adults and in pregnancy: recommendations of the ESE Educational Program of Parathyroid Disorders (PARAT 2021). Eur. J. Endocrinol. 186, R33–R63 (2021). https://doi.org/10.1530/EJE-21-1044
H.L. Barrett, A. McElduff, Vitamin D and pregnancy: an old problem revisited. Best Pract. Res. Clin. Endocrinol. Metab. 24, 527–539 (2010). https://doi.org/10.1016/j.beem.2010.05.010
C.S. Kovacs, H.M. Kronenberg, Maternal-fetal calcium and bone metabolism during pregnancy, puerperium, and lactation. Endocr. Rev. 18, 832–872 (1997). https://doi.org/10.1210/edrv.18.6.0319
H. Zhong, Q. Liao, J. Liu, X. Chen, Y. Hu, S. Jian et al. Expert consensus on multidisciplinary approach to the diagnosis and treatment of primary hyperparathyroidism in pregnancy in China. Endocrine 82, 282–295 (2023). https://doi.org/10.1007/s12020-023-03392-w
J.P. Bilezikian, M.L. Brandi, R. Eastell, S.J. Silverberg, R. Udelsman, C. Marcocci et al. Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the Fourth International Workshop. J. Clin. Endocrinol. Metab. 99, 3561–3569 (2014). https://doi.org/10.1210/jc.2014-1413
R. Udelsman, G. Åkerström, C. Biagini, Q.-Y. Duh, P. Miccoli, B. Niederle et al. The surgical management of asymptomatic primary hyperparathyroidism: proceedings of the Fourth International Workshop. J. Clin. Endocrinol. Metab. 99, 3595–3606 (2014). https://doi.org/10.1210/jc.2014-2000
S.M. Wilhelm, T.S. Wang, D.T. Ruan, J.A. Lee, S.L. Asa, Q.-Y. Duh et al. The American Association of Endocrine Surgeons guidelines for definitive management of primary hyperparathyroidism. JAMA Surg 151, 959–968 (2016). https://doi.org/10.1001/jamasurg.2016.2310
A. McCarthy, S. Howarth, S. Khoo, J. Hale, S. Oddy, D. Halsall et al. Management of primary hyperparathyroidism in pregnancy: a case series. Endocrinol. Diabetes Metab. Case Rep. 2019, 19–0039 (2019). https://doi.org/10.1530/EDM-19-0039
A.N. DiMarco, K. Meeran, I. Christakis, V. Sodhi, C. Nelson-Piercy, N.S. Tolley et al. Seventeen cases of primary hyperparathyroidism in pregnancy: a call for management guidelines. J. Endocr. Soc. 3, 1009–1021 (2019). https://doi.org/10.1210/js.2018-00340
F. Cetani, F. Saponaro, C. Marcocci, Non-surgical management of primary hyperparathyroidism. Best Pract. Res. Clin. Endocrinol. Metab. 32, 821–835 (2018). https://doi.org/10.1016/j.beem.2018.09.006
C. Nastos, A. Paspala, I. Mavroeidi, F. Stavratis, V. Lampadiari, S. Kalantaridou et al. Surgical management of primary hyperparathyroidism during pregnancy: a systematic review of the literature. Gynecol. Endocrinol. 37, 1086–1095 (2021). https://doi.org/10.1080/09513590.2021.1932801
S. Bansal, R.M. Kaushik, R. Kaushik, S. Modi, S. Raghuvanshi, A. Kusum, Primary hyperparathyroidism presenting as severe hypercalcemia with acute pancreatitis in pregnancy. Gynecol. Endocrinol. 36, 469–472 (2020). https://doi.org/10.1080/09513590.2019.1698028
R. Pal, S.K. Bhadada, N. Gupta, A. Behera, N. Aggarwal, A. Aggarwal et al. Primary hyperparathyroidism in pregnancy: observations from the Indian PHPT registry. J. Endocrinol. Invest 44, 1425–1435 (2021). https://doi.org/10.1007/s40618-020-01441-z
L. Zhang, Y.R. Luo, Y. Hu, Y. Zhai, H. Gao, Z. Cao, Primary hyperparathyroidism in pregnancy: insights from a case of a 28-year-old woman with miscarriages and hyperemesis gravidarum. Ann. Lab. Med. 41, 336–338 (2021). https://doi.org/10.3343/alm.2021.41.3.336
J. Norman, D. Politz, L. Politz, Hyperparathyroidism during pregnancy and the effect of rising calcium on pregnancy loss: a call for earlier intervention. Clin. Endocrinol. 71, 104–109 (2009). https://doi.org/10.1111/j.1365-2265.2008.03495.x
L. Kohlmeier, R. Marcus, Calcium disorders of pregnancy. Endocrinol. Metab. Clin. North Am. 24, 15–39 (1995). https://doi.org/10.1016/S0889-8529(18)30052-5
M. Som, J.S. Stroup, Primary hyperparathyroidism and pregnancy. Bayl Univ. Med. Cent. Proc. 24, 220–223 (2011). https://doi.org/10.1080/08998280.2011.11928719
F.L. Delmonico, R.M. Neer, A.B. Cosimi, A.B. Barnes, P.S. Russell, Hyperparathyroidism during pregnancy. Am. J. Surg. 131, 328–337 (1976). https://doi.org/10.1016/0002-9610(76)90127-6
A. Abood, P. Vestergaard, Pregnancy outcomes in women with primary hyperparathyroidism. Eur. J. Endocrinol. 171, 69–76 (2014). https://doi.org/10.1530/EJE-13-0966
D. Hirsch, V. Kopel, V. Nadler, S. Levy, Y. Toledano, G. Tsvetov, Pregnancy outcomes in women with primary hyperparathyroidism. J. Clin. Endocrinol. Metab. 100, 2115–2122 (2015). https://doi.org/10.1210/jc.2015-1110
A.A. Khan, D.A. Hanley, R. Rizzoli, J. Bollerslev, J.E.M. Young, L. Rejnmark et al. Primary hyperparathyroidism: review and recommendations on evaluation, diagnosis, and management. A Canadian and international consensus. Osteoporos. Int. 28, 1–19 (2016). https://doi.org/10.1007/s00198-016-3716-2
S.Y. Huang, P.-H. Lo, W.-M. Liu, Y.-G. Cherng, C.-C. Yeh, T.-L. Chen et al. Outcomes after nonobstetric surgery in pregnant patients: a nationwide study. Mayo Clin. Proc. 91, 1166–1172 (2016). https://doi.org/10.1016/j.mayocp.2016.06.021
S. Kuy, Outcomes following thyroid and parathyroid surgery in pregnant women. Arch. Surg. 144, 399–406 (2009). https://doi.org/10.1001/archsurg.2009.48
M.C. Tolcher, W.E. Fisher, S.L. Clark, Nonobstetric surgery during pregnancy. Obstet. Gynecol. 132, 395–403 (2018). https://doi.org/10.1097/AOG.0000000000002748
R. Cohen-Kerem, C. Railton, D. Oren, M. Lishner, G. Koren, Pregnancy outcome following non-obstetric surgical intervention. Am. J. Surg. 190, 467–473 (2005). https://doi.org/10.1016/j.amjsurg.2005.03.033
V. Balinskaite, A. Bottle, V. Sodhi, A. Rivers, P.R. Bennett, S.J. Brett et al. The risk of adverse pregnancy outcomes following nonobstetric surgery during pregnancy: estimates from a retrospective cohort study of 6.5 million pregnancies. Ann. Surg. 266, 260–266 (2017). https://doi.org/10.1097/SLA.0000000000001976
H. Jiao, L. Sun, Y. Liu, J. Zhou, X. Chen, J. Liu et al. Multidisciplinary team efforts to improve the pregnancy outcome of pregnancy complicated with primary hyperparathyroidism: case series from a single hospital. BMC Pregnancy Childbirth 21, 576 (2021). https://doi.org/10.1186/s12884-021-04042-7
P.F. Schnatz, S.L. Curry, Primary hyperparathyroidism in pregnancy: evidence-based management. Obstet. Gynecol. Surv. 57, 365–376 (2002). https://doi.org/10.1097/00006254-200206000-00022
P.F. Schnatz, S. Thaxton, Parathyroidectomy in the third trimester of pregnancy. Obstet. Gynecol. Surv. 60, 672–682 (2005). https://doi.org/10.1097/01.ogx.0000180889.23678.fb
K.C. Kort, H.J. Schiller, P.J. Numann, Hyperparathyroidism and pregnancy. Am. J. Surg. 177, 66–68 (1999). https://doi.org/10.1016/S0002-9610(98)00302-X
M. Nejdlova, T. Johnson, Anaesthesia for non-obstetric procedures during pregnancy. Contin. Educ. Anaesth. Crit. Care Pain 12, 203–206 (2012). https://doi.org/10.1093/bjaceaccp/mks022
B.C. Visser, R.E. Glasgow, K.K. Mulvihill, S.J. Mulvihill, Safety and timing of nonobstetric abdominal surgery in pregnancy. Dig. Surg. 18, 409–417 (2001). https://doi.org/10.1159/000050183
R. Udelsman, Z. Lin, P. Donovan, The superiority of minimally invasive parathyroidectomy based on 1650 consecutive patients with primary hyperparathyroidism. Ann. Surg. 253, 585–591 (2011). https://doi.org/10.1097/SLA.0b013e318208fed9
J.M. Ruda, C.S. Hollenbeak, B.C. Stack, A systematic review of the diagnosis and treatment of primary hyperparathyroidism from 1995 to 2003. Otolaryngol. Neck Surg. 132, 359–372 (2005). https://doi.org/10.1016/j.otohns.2004.10.005
R. Rai, L. Regan, Recurrent miscarriage. The Lancet 368, 601–611 (2006). https://doi.org/10.1016/S0140-6736(06)69204-0
R.M. Silver, Fetal death. Obstet Gynecol 109, 153–167 (2007). https://doi.org/10.1097/01.AOG.0000248537.89739.96
V. Dochez, G. Ducarme, Primary hyperparathyroidism during pregnancy. Arch. Gynecol. Obstet. 291, 259–263 (2015). https://doi.org/10.1007/s00404-014-3526-8
M.L. Sandler, R. Ho, M.H. Xing, S. Gidumal, H. Spitzer, J.C. Levy et al. Primary hyperparathyroidism during pregnancy treated with parathyroidectomy: a systematic review. The Laryngoscope 131, 1–7 (2021). https://doi.org/10.1002/lary.29489
H.A. Korkmaz, B. Özkan, D. Terek, C. Dizdarer, S. Arslanoğlu, Neonatal seizure as a manifestation of unrecognized maternal hyperparathyroidism. J. Clin. Res. Pediatr. Endocrinol. 5, 206–208 (2013). https://doi.org/10.4274/Jcrpe.1037
P. Pothiwala, S.N. Levine, Parathyroid surgery in pregnancy: review of the literature and localization by aspiration for parathyroid hormone levels. J. Perinatol. 29, 779–784 (2009). https://doi.org/10.1038/jp.2009.84
Funding
Open access funding provided by Bar-Ilan University.
Author information
Authors and Affiliations
Contributions
The authors E.S. and A.Z. formulated the study conception and design. The author E.S. screened and collected the data for analysis. The author S.G.G. performed the statistical analysis and prepared the tables and figures. All authors reviewed the results and formulated the conclusions for the draft manuscript. The author E.S. wrote the manuscripts. The author A.Z. commented on previous versions and reviewed the final manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Eli, S., Gal, S.G. & Adnan, Z. Comparison between surgical and non-surgical management of primary hyperparathyroidism during pregnancy: a systematic review. Endocrine (2024). https://doi.org/10.1007/s12020-024-03930-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12020-024-03930-0