Abstract
Introduction
Natriuretic peptide receptor-A (NPR-A) signaling system is considered as an intrinsic productive mechanism of the heart that opposes abnormal cardiac remodeling and hypertrophic growth. NPR-A is coded by Npr1 gene, and its expression is downregulated in the hypertrophied heart.
Aim
We sought to examine the levels of Npr1 gene transcription in triiodo-L-thyronine (T3) treated hypertrophied cardiomyocyte (H9c2) cells, in vitro, and also the involvement of β-adrenergic receptor (β-AR) - Reactive oxygen species (ROS) signaling system in the down-regulation of Npr1 transcription also studied.
Main methods
Anti-hypertrophic Npr1 gene transcription was monitored in control and T3-treated (dose and time dependent) H9c2 cells, using a real time PCR method. Further, cell size, intracellular cGMP, ROS, hypertrophy markers (ANP, BNP, α-sk, α-MHC and β-MHC), β-AR, and protein kinase cGMP-dependent 1 (PKG-I) genes expression were also determined. The intracellular cGMP and ROS levels were determined by ELISA and DCF dye method, respectively. In addition, to neutralize T3 mediated ROS generation, H9c2 cells were treated with T3 in the presence and absence of antioxidants [curcumin (CU) or N-acetyl-L-cysteine (NAC)].
Results
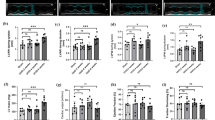
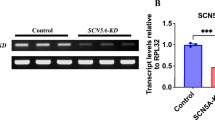
A dose dependent (10 pM, 100 pM, 1 nM and 10 nM) and time dependent (12 h, 24 h and 48 h) down-regulation of Npr1 gene transcription (20, 39, 60, and 74% respectively; 18, 55, and 85%, respectively) were observed in T3-treated H9c2 cells as compared with control cells. Immunofluorescence analysis also revealed that a marked down regulation of NPR- A protein in T3-treated cells as compared with control cells. Further, a parallel downregulation of cGMP and PKG-I (2.4 fold) were noticed in the T3-treated cells. In contrast, a time dependent increased expression of β-AR (60, 72, and 80% respectively) and ROS (26, 48, and 74%, respectively) levels were noticed in T3-treated H9c2 cells as compared with control cells. Interestingly, antioxidants, CU or NAC co-treated T3 cells displayed a significant reduction in ROS (69 and 81%, respectively) generation and to increased Npr1 gene transcription (81 and 88%, respectively) as compared with T3 alone treated cells.
Conclusion
Our result suggest that down regulation of Npr1 gene transcription is critically involved in T3- induced hypertrophic growth in H9c2 cells, and identifies the cross-talk between T3-β-AR-ROS and NPR-A signaling.








Similar content being viewed by others
References
Y. Takahashi, T. Nakayama, M. Soma, Y. Izumi, K. Kanmatsuse, Organization of the Human Natriuretic Peptide Receptor A Gene. Biochem. Biophys. Res. Commun. 246(3), 736–739 (1998). https://doi.org/10.1006/bbrc.1998.8693
D.G. Lowe, M.S. Chang, R. Hellmiss, E. Chen, S. Singh, D.L. Garbers, D.V. Goeddel, Human atrial natriuretic peptide receptor defines a new paradigm for second messenger signal transduction. EMBO J. 8(5), 1377–1384 (1989). https://doi.org/10.1002/j.1460-2075.1989.tb03518.x
D.L. Garbers, Guanylyl cyclase receptors and their endocrine, paracrine, and autocrine ligands. Cell 71(1), 1–4 (1992). https://doi.org/10.1016/0092-8674(92)90258-e
K.N. Pandey, Biology of natriuretic peptides and their receptors. Peptides 26(6), 901–932 (2005). https://doi.org/10.1016/j.peptides.2004.09.024
L.R. Potter, T. Hunter, Phosphorylation of the Kinase Homology Domain Is Essential for Activation of the A-Type Natriuretic Peptide Receptor. Mol. Cell. Biol. 18(4), 2164–2172 (1998). https://doi.org/10.1128/mcb.18.4.2164
I. Mani, K.N. Pandey, Emerging concepts of receptor endocytosis and concurrent intracellular signaling: Mechanisms of guanylyl cyclase/natriuretic peptide receptor-A activation and trafficking. Cell Signal 60, 17–30 (2019). https://doi.org/10.1016/j.cellsig.2019.03.022
V. Cannone, A. Cabassi, R. Volpi, J.C. Burnett, Atrial natriuretic peptide: a molecular target of novel therapeutic approaches to cardio-metabolic disease. Int. J. Mol. Sci. 20(13), 3265 (2019). https://doi.org/10.3390/ijms20133265
I. Kishimoto, T. Tokudome, K. Nakao, K. Kangawa, Natriuretic peptide system: an overview of studies using genetically engineered animal models. FEBS J. 278(11), 1830–1841 (2011). https://doi.org/10.1111/j.1742-4658.2011.08116.x
E. Vellaichamy, M.L. Khurana, J. Fink, K.N. Pandey, Involvement of the NF-kappa B/matrix metalloproteinase pathway in cardiac fibrosis of mice lacking guanylyl cyclase/natriuretic peptide receptor A. J. Biol. Chem. 280(19), 19230–19242 (2005). https://doi.org/10.1074/jbc.m411373200
P.M. Oliver, J.E. Fox, R. Kim, H.A. Rockman, H.S. Kim, R.L. Reddick, K.N. Pandey, S.L. Milgram, O. Smithies, N. Maeda, Hypertension, cardiac hypertrophy, and sudden death in mice lacking natriuretic peptide receptor A. Proc. Natl Acad. Sci. USA 94(26), 14730–5 (1997). https://doi.org/10.1073/pnas.94.26.14730
L.J. Ellmers, J.W. Knowles, H.S. Kim, O. Smithies, N. Maeda, V.A. Cameron, Ventricular expression of natriuretic peptides in Npr1(-/-) mice with cardiac hypertrophy and fibrosis. Am. J. Physiol. Heart Circ. Physiol. 283(2), H707–14 (2002). https://doi.org/10.1152/ajpheart.00677.2001
E. Vellaichamy, D. Zhao, N. Somanna, K.N. Pandey, Genetic disruption of guanylyl cyclase/natriuretic peptide receptor-A up-regulates ACE and AT1 receptor gene expression and signaling: role in cardiac hypertrophy. Physiol. Genomics 31(12), 193–202 (2007). https://doi.org/10.1152/physiolgenomics.00079.2007
D. Zhao, E. Vellaichamy, N. Somanna, K.N. Pandey, Guanylyl cyclase/natriuretic peptide receptor-A gene disruption causes increased adrenal angiotensin II and aldosterone levels. Am. J. Physiol. Renal Physiol. 293(1), F121–F127 (2007). https://doi.org/10.1152/ajprenal.00478.2006
S. Rubattu, G. Bigatti, A. Evangelista, C. Lanzani, R. Stanzione, L. Zagato, P. Manunta, S. Marchitti, V. Venturelli, G. Bianchi, M. Volpe, P. Stella, Association of atrial natriuretic peptide and type a natriuretic peptide receptor gene polymorphisms with left ventricular mass in human essential hypertension. J. Am. Coll. Cardiol. 48(3), 499–505 (2006). https://doi.org/10.1016/j.jacc.2005.12.081
J. Wang, Z. Wang, C. Yu, Association of Polymorphisms in the Atrial Natriuretic Factor Gene with the Risk of Essential Hypertension: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health. 13(5), 458 (2016). https://doi.org/10.3390/ijerph13050458
V. Gopi, V. Subramanian, S. Manivasagam, E. Vellaichamy, Angiotensin II down- regulates natriuretic peptide receptor-A expression and guanylyl cyclase activity in H9c2 (2-1) cardiac myoblast cells: role of ROS and NF-kB. Mol. Cell Biochem. 409(1-2), 67–79 (2015). https://doi.org/10.1007/s11010-015-2513-0
W. Song, H. Wang, Q. Wu, Atrial natriuretic peptide in cardiovascular biology and disease (NPPA). Gene 569(1), 1–6 (2015). https://doi.org/10.1016/j.gene.2015.06.029
S. Manivasagam, E. Vellaichamy, Suppression of Npr1, not Npr2 gene function induces hypertrophic growth in H9c2 cells in vitro. Biochem. Biophys. Res. Commun. 491(2), 250–256 (2017). https://doi.org/10.1016/j.bbrc.2017.07.123
S. Manivasagam, V. Subramanian, A. Tumala, E. Vellaichamy, Differential expression and regulation of anti-hypertrophic genes Npr1 and Npr2 during β-adrenergic receptor activation-induced hypertrophic growth in rats. Mol. Cell Endocrinol. 433, 117–29 (2016). https://doi.org/10.1016/j.mce.2016.06.010
P. Kumar, R. Garg, G. Bolden, K.N. Pandey, Interactive roles of Ets-1, Sp1, and acetylated histones in the retinoic acid-dependent activation of guanylyl cyclase/atrial natriuretic peptide receptor-A gene transcription. J. Biol. Chem. 285(48), 37521–30 (2010). https://doi.org/10.1074/jbc.M110.132795
U. Subramanian, P. Kumar, I. Mani, D. Chen, I. Kessler, R. Periyasamy, G. Raghavaraju, K. Pandey, Retinoic acid and sodium butyrate suppress the cardiac expression of hypertrophic markers and proinflammatory mediators in Npr1 gene-disrupted haplotype mice. Physiol. Genomics 48(7), 477–490 (2016). https://doi.org/10.1152/physiolgenomics.00073.2015
S. Manivasagam, T. Velusamy, B. Sowndharajan, N. Chandrasekar, S. Dhanusu, E. Vellaichamy, Valporic acid enhances the Atrial Natriuretic Peptide (ANP) mediated anti-hypertrophic activity by modulating the Npr1 gene transcription in H9c2 cells in vitro. Eur. J. Pharmacol. 813, 94–104 (2017). https://doi.org/10.1016/j.ejphar.2017.07.042
I. Klein, S. Danzi, Thyroid disease and the heart. Circulation 116(15), 1725–1735 (2007). https://doi.org/10.1161/CIRCULATIONAHA.106.678326
S. Danzi, I. Klein, Thyroid disease and the cardiovascular system. Endocrinol. Metab. Clin. N. Am. 43(2), 517–528 (2014). https://doi.org/10.1016/j.ecl.2014.02.005
A. Jabbar, A. Pingitore, S.H. Pearce, A. Zaman, G. Iervasi, S. Razvi, Thyroid hormones and cardiovascular disease. Nat. Rev. Cardiol. 14(1), 39–55 (2017). https://doi.org/10.1038/nrcardio.2016.174
C.W. Siu, C.Y. Yeung, C.P. Lau, A.W.C. Kung, H.F. Tse, Incidence, clinical characteristics and outcome of congestive heart failure as the initial presentation in patients with primary hyperthyroidism. Heart 93(4), 483–487 (2010). https://doi.org/10.1136/hrt.2006.100628
B. Biondi, Mechanisms in endocrinology. Heart failure and thyroid dysfunction. Eur. J. Endocrinol. 167(5), 609–18 (2012). https://doi.org/10.1530/EJE-12-0627
J.E. Mitchell, A.S. Hellkamp, D.B. Mark, J. Anderson, G.W. Johnson, J.E. Poole, K.L. Lee, G.H. Bardy, Thyroid function in heart failure and impact on mortality. JACC Heart Fail 1(1), 48–55 (2013). https://doi.org/10.1016/j.jchf.2012.10.004
J.P. Bilezikian, J.N. Loeb, The influence of hyperthyroidism and hypothyroidism on α- and β-adrenergic receptor systems and adrenergic responsiveness. Endocr. Rev. 41(4), 378–387 (1983). https://doi.org/10.1210/edrv-4-4-378
L.W. Hu, L.A. Benvenuti, E.A. Liberti, M.S. Carneiro‐Ramos, M.L.M. Barreto‐Chaves, Thyroxine‐induced cardiac hypertrophy:Influence of adrenergic nervous system versus renin‐angiotensin system on myocyte remodeling. Am. J. Physiol. Regul. Integr. Comp. Physiol. 285(6), 1473–1480 (2003). https://doi.org/10.1152/ajpregu.00269.2003
W. Dillmann, Cardiac hypertrophy and thyroid hormone signaling. Heart Fail. Rev. 15(2), 125–132 (2010). https://doi.org/10.1007/s10741-008-9125-7
A.P.C. Takano, N. Senger, C.D. Munhoz, M.L.M. Barreto‐Chaves, AT1 blockage impairs NF‐kB activation mediated by thyroid hormone in cardiomyocytes. Pflugers Archiv 470(3), 549–558 (2018). https://doi.org/10.1007/s00424-017-2088-6
M.S. Carneiro‐Ramos, G.P. Diniz, A.P. Nadu, J. Almeida, R.L.P. Vieira, R.A.S. Santos, M.L.M. Barreto‐Chaves, Blockage of angiotensin II type 2 receptor prevents thyroxine‐mediated cardiac hypertrophy by blocking Akt activation. Basic Res. Cardiol. 105(3), 325–335 (2010). https://doi.org/10.1007/s00395-010-0089-0
A. Parthasarathy, V. Gopi, S. Umadevi, A. Simna, M.J.U. Sheik, H. Divya, E. Vellaichamy, Suppression of atrial natriuretic peptide/natriuretic peptide receptor-A- mediated signaling up-regulates angiotensin-II-induced collagen synthesis in adult cardiac fibroblasts. Mol. Cell Biochem. 378(1-2), 217–228 (2013). https://doi.org/10.1007/s11010-013-1612-z
G. Sacripanti, M. Nguyen, L. Lorenzini, S. Frascarelli, A. Saba, R. Zucchi, S. Ghelardoni, 3,5-Diiodo-l-Thyronine Increases Glucose Consumption in Cardiomyoblasts Without Affecting the Contractile Performance in Rat Heart. Front. Endocrinol. 30(9), 282 (2018). https://doi.org/10.3389/fendo.2018.00282
A. Rozanski, A.P.C. Takano, P.N. Kato, A.G. Soares, C. Lellis-Santos, J.C. Campos, J.C.B. Ferreira, M.L.M. Barreto-Chaves, A.S. Moriscot, M-protein is down-regulated in cardiac hypertrophy driven by thyroid hormone in rats. Mol. Endocrinol. 27(12), 2055–65 (2013). https://doi.org/10.1210/me.2013-1018
S.M. Chacko, K.G. Nevin, R. Dhanyakrishnan, B.P. Kumar, Protective effect of p-coumaric acid against doxorubicin induced toxicity in H9c2 cardiomyoblast cell lines. Toxicol. Rep. 2, 1213–1221 (2015). https://doi.org/10.1016/j.toxrep.2015.08.002
J.H. Lee, D.H. Kim, M.A. Kim, K.H. Jung, K.H. Lee, Mitochondrial ROS-Mediated Metabolic and Cytotoxic Effects of Isoproterenol on Cardiomyocytes Are p53-Dependent and Reversed by Curcumin. Molecules 27(4), 1346 (2022). https://doi.org/10.3390/molecules27041346
M.M. Bradford, A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal. Biochem. 7(72), 248–54 (1976). https://doi.org/10.1006/abio.1976.9999
J.W. Knowles, G. Esposito, L. Mao, J.R. Hagaman, J.E. Fox, O. Smithies, H.A. Rockman, N. Maeda, Pressure-independent enhancement of cardiac hypertrophy in natriuretic peptide receptor A-deficient. mice. J. Clin. Invest. 107(8), 975–984 (2001). https://doi.org/10.1172/jci11273
I. Kishimoto, K. Rossi, D.L. Garbers, A genetic model provides evidence that the receptor for atrial natriuretic peptide (guanylyl cyclase-A) inhibits cardiac ventricular myocyte hypertrophy. Proc. Natl Acad. Sci. USA 98(5), 2703–2706 (2001). https://doi.org/10.1073/pnas.051625598
M.L. Barreto-Chaves, N. Senger, M. Fevereiro, A.C. Parletta, A. Takano, Impact of hyperthyroidism on cardiac hypertrophy. Endocr. Connect. 9(3), R59–69 (2020). https://doi.org/10.1530/EC-19-0543
S. Ventrella, I. Klein, Beta-adrenergic receptor blocking drugs in the management of hyperthyroidism. Endocrinologist 4(5), 391–399 (1994). https://doi.org/10.1097/00019616-199409000-00010
R.D. Utiger, β-Adrenergic-antagonist therapy for hyperthyroid Graves’ disease. N. Engl. J. Med 310(24), 1597–1598 (1984). https://doi.org/10.1056/NEJM198406143102410
I. Klein, K. Ojamaa, Thyroid hormone and the cardiovascular system. N. Engl. J. Med. 344(7), 501–509 (2001). https://doi.org/10.1056/NEJM200102153440707
H.A. Rockman, W.J. Koch, R.J. Lefkowitz, Seven-transmembrane-spanning receptors and heart function. Nature 415(68), 206–12 (2002). https://doi.org/10.1038/415206a
A.S.R. Araujo, G.P. Diniz, F.E.R. Seibel, G. Branchini, M.F.M. Ribeiro, I.S. Brum, N. Khaper, M.L.M. Barreto-Chaves, A.B. Bello-Klein, Reactive oxygen and nitrogen species balance in the determination of thyroid hormones-induced cardiac hypertrophy mediated by renin- angiotensin system. Mol. Cell Endocrinol. 333(1), 78–84 (2011). https://doi.org/10.1016/j.mce.2010.12.018
H. Yaomeng, L. Tongxin, G. Shichao, L. Shuyu, Z. Xiaoran, L. Ying, L. Dangyang, L. Weimin, L. Yang, L. Kunshen, Z. Zheng, L. Chao, Investigating the Role of NPR1 in Dilated Cardiomyopathy and its Potential as a Therapeutic Target for Glucocorticoid Therapy. Front. Pharmacol. 14, 1290253 (2023). https://doi.org/10.3389/fphar.2023.1290253
C. Nunn, M.X. Zou, A.J. Sobiesiak, A.A. Roy, L. Kirshenbaum, P. Chidiac, RGS2 inhibits β-adrenergic receptor-induced cardiomyocyte hypertrophy. Cell Signal 22(8), 1231–1239 (2010). https://doi.org/10.1016/j.cellsig.2010.03.015
G.X. Zhang, S. Kimura, A. Nishiyama, T. Shokoji, M. Rahman, L. Yao, Y. Abe, Cardiac oxidative stress in acute and chronic isoproterenol-infused rats. Cardiovasc. Res. 65(1), 230e238 (2005). https://doi.org/10.1016/j.cardiores.2004.08.013
P. Venditti, S. Di. Meo, Thyroid hormone-induced oxidative stress. Cell. Mol. Life Sci 63(4), 414–434 (2006). https://doi.org/10.1007/s00018-005-5457-9
G.P. Diniz, M.S. Carneiro-Ramos, M.L.M. Barreto-Chaves, Angiotensin type 1 receptor mediates thyroid hormone-induced cardiomyocyte hypertrophy through the Akt/GSK- 3beta/mTOR signaling pathway. Basic Res. Cardiol. 104(6), 653–67 (2009). https://doi.org/10.1007/s00395-009-0043-1
C.H. Huang, F.T. Wang, Y.D. Hsuuw, F.J. Huang, W.H. Chan, Non-embryotoxic dosage of alternariol aggravates ochratoxin A-triggered deleterious effects on embryonic development through ROS-dependent apoptotic processes. Toxicol. Res. 10(6), 1211–1222 (2021). https://doi.org/10.1093/toxres/tfab112
Y. Zhang, S. Su, W. Li, Y. Ma, J. Shen, Y. Wang, Y. Shen, J. Chen, Y. Ji, Y. Xie, H. Ma, M. Xiang, Piezo1-Mediated Mechanotransduction Promotes Cardiac Hypertrophy by Impairing Calcium Homeostasis to Activate Calpain/Calcineurin Signaling. Hypertension 78(3), 647–660 (2021). https://doi.org/10.1161/HYPERTENSIONAHA.121.17177
A. Kaumann, S. Bartel, P. Molenaar, L. Sanders, K. Burrell, D. Vetter, P. Hempel, P. Karczewski, E. Krause, Activation of β2-adrenergic receptors hastens relaxation and mediates phosphorylation of phospholamban, troponin I, and C protein in ventricular myocardium from patients with terminal heart failure. Circulation 99(1), 65–72 (1999). https://doi.org/10.1161/01.cir.99.1.65
W. Dillmann, Cellular action of thyroid hormone on the heart. Thyroid 12(6), 447–52 (2002). https://doi.org/10.1089/105072502760143809
F. Vargas, J. Moreno, I. Rodriguez-Gomez, R. Wangensteen, A. Osuna, M. Alvarez-Guerra, J. Garcia-Estan, Vascular and renal function in experimental thyroid disorders. Eur. J. Endocrinol. 154(2), 197–212 (2006). https://doi.org/10.1530/eje.1.02093
F. Cioffi, R. Senese, A. Lanni, F. Goglia, Thyroid hormones and mitochondria: with a brief look at derivatives and analogues. Mol. Cell Endocrinol. 379(1), 51–61 (2013). https://doi.org/10.1016/j.mce.2013.06.006
T. Ines, G. Benjamin, J. Angelo, B. Doruntina, R. Rene, O. Barbara, F. Wolfgang, T. Corina, T3-induced enhancement of mitochondrial Ca2+ uptake as a boost for mitochondrial metabolism. Free Radical Biol. Med 181, 197–208 (2022). https://doi.org/10.1016/j.freeradbiomed.2022.01.024
T. Ide, H. Tsutsui, S. Hayashidani, D. Kang, N. Suematsu, K. Nakamura, A. Takeshita, Mitochondrial DNA Damage and Dysfunction Associated With Oxidative Stress in Failing Hearts After Myocardial Infarction. Circ. Res. 88(5), 529–535 (2001). https://doi.org/10.1161/01.res.88.5.529
D.M. Deborah, L.R. Lincoln, Dendroaspis natriuretic peptide and the designer natriuretic peptide, CD-NP, are resistant to proteolytic inactivation. J. Mol. Cell. Cardiol. 51(1), 0–71 (2011). https://doi.org/10.1016/j.yjmcc.2011.03.013
E.J. Tsai, D.A. Kass, Cyclic GMP signaling in cardiovascular pathophysiology and therapeutics. Pharmacol. Ther. 122(3), 216–38 (2009). https://doi.org/10.1016/j.pharmthera.2009.02.009
N. Senger, M. Melo, G. Diniz, M. Campagnole-Santos, R. Santos, M. Barreto-Chaves, Angiotensin-(1-7) reduces cardiac effects of thyroid hormone by GSK3Β/NFATc3 signaling pathway. Clin. Sci. 132(11), 1117–1133 (2018). https://doi.org/10.1042/CS20171606
Acknowledgements
We are grateful to Dr. N. Dhatchanamoorthy for the support during this study. This study was supported by RUSA 2.0 - University of Madras (T1 PF6).
Author information
Authors and Affiliations
Contributions
Study design: E.V. Collection of data: G.N. interpretation of data: E.V. Authors participate in drafting the article: G.N. and E.V. Revising it critically for important intellectual content: E.V. Final approval of the version to be published: All authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nagaraj, G., Vellaichamy, E. Triiodo-L-thyronine (T3) downregulates Npr1 gene (coding for natriuretic peptide receptor-A) transcription in H9c2 cells: involvement of β-AR-ROS signaling. Endocrine (2024). https://doi.org/10.1007/s12020-024-03849-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12020-024-03849-6