Abstract
Aim
Triple-A Syndrome (TAS) is a rare autosomal recessive disorder characterized by adrenal insufficiency, achalasia, and alacrimia. This disorder is caused by mutations in the AAAS gene. The aim of this study is to discuss the clinical, laboratory and molecular genetic analysis results of 12 patients with TAS.
Method
We evaluated 12 patients from 8 families. Clinical and laboratory data were retrospectively collected from the medical records of the patients in the database for the period 2015–2020. All exons and exon-intron junctions of the AAAS gene were evaluated by next-generation sequencing method. Detected variants were classified according to American Collage of Medical Genetics criteria.
Results
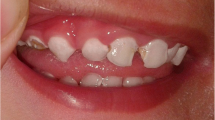
Alacrimia was found in all patients (100%); achalasia was found in 10 patients (83.3%) and adrenal insufficiency was found in 10 patients (83.3%). In addition, hyperreflexia(6/12), learning disability(5/12), hypernasal speech(5/12), muscle weakness(8/12), delayed walking(7/12), delayed speech(6/12), excessive sweating(7/12), optic atrophy(1/12), epilepsy(1/12), palmoplantar hyperkeratosis(5/12), multiple dental caries(9/12), atrophy of the thenar/hypothenar muscles(4/12) and short stature(4/12) were detected. The DHEA-S levels were measured in 10 patients and were found to be low in 8 of them. In all patients, the sodium and potassium levels were found to be normal. AAAS gene sequencing revealed four previously reported c.1066_1067del (p.Leu356fs*8), c.1432 C > T (p.Arg478*), c.688 C > T (p.Arg230*), and c.1368_1372del (p.Gln456fs*38) variants and two novel homozygous c.1250-1 G > A and c.398_399 + 2del variants in the AAAS gene.
Conclusion
We detected two novel variants in the AAAS gene. While the classic triad is present in 66.7% of the cases, neurological dysfunction, skin and dental pathologies also occur quite frequently. The earliest and most common finding of TAS is alacrimia. Therefore, adrenal insufficiency should be investigated in all patients with alacrimia and if necessary, genetic analysis should be performed for TAS. In addition, TAS should be followed up with a multidisciplinary approach since it involves many systems.
Similar content being viewed by others
References
D.C. Sadowski, F. Ackah, B. Jiang, L.W. Svenson, Achalasia: incidence, prevalence and survival. A population-based study. Neurogastroenterol. Motil. 22, 256–261 (2010). https://doi.org/10.1111/j.1365-2982.2010.01511.x. Epub 2010 May 11
J. Allgrove, G.S. Clayden, J.C. Macaulay, Familial glucocorticoid deficiency with achalasia of the cardia and deficient tear production. Lancet 311, 1284–1286 (1978). https://doi.org/10.1016/S0140-6736(78)91268-0
K. Handschug, S. Sperling, S.J. Yoon, S. Hennig, A.J. Clark, A. Huebner, Triple A syndrome is caused by mutations in AAAS, a new WD-repeat protein gene. Hum. Mol. Genet 10, 283–290 (2001). https://doi.org/10.1093/hmg/10.3.283
J.M. Cronshaw, A.N. Krutchinsky, W. Zhang, B.T. Chait, M.J. Matunis, Proteomic analysis of the mammalian nuclear pore complex. J. Cell Biol. 158, 915–927 (2002). https://doi.org/10.1083/jcb.200206106
R. Prasad, L.A. Metherell, A.J. Clark, H.L. Storr, Deficiency of ALADIN impairs redox homeostasis in human adrenal cells and inhibits steroidogenesis. Endocrinology 154, 3209–3218 (2013). https://doi.org/10.1210/en.2013-1241
R. Jühlen, J. Idkowiak, A.E. Taylor, et al. Role of ALADIN in human adrenocortical cells for oxidative stress response and steroidogenesis. PLoS ONE 10, e0124582 (2015). https://doi.org/10.1371/journal.pone.0124582
F. Roucher-Boulez, A. Brac de la Perriere, A. Jacquez et al. Triple-A syndrome: a wide spectrum of adrenal dysfunction. Eur. J. Endocrinol. 178, 199–207 (2018)
F. Kilicli, F. Acibucu, S. Senel et al. Allgrove syndrome. Singap. Med. J. 53, e92–4 (2012)
M. Ventura, J. Serra-Caetano, R. Cardoso, I. Dinis, M. Melo, F. Carrilho, A. Mirante, The spectrum of pediatric adrenal insufficiency: insights from 34 years of experience. J. Pediatr. Endocrinol. Metab. 32, 721–726 (2019)
C.E. Flück, Mechanısms In Endocrınology: Update on pathogenesis of primary adrenal insufficiency: beyond steroid enzyme deficiency and autoimmune adrenal destruction. Eur. J. Endocrinol. 177, 99–111 (2017). Epub 2017 Apr 27
R. Perry, O. Kecha, J. Paquette, C. Huot, G. Van Vliet, C. Deal, Primary adrenal insufficiency in children: twenty years experience at the Sainte-ustine Hospital, Montreal. J. Clin. Endocrinol. Metab. 90, 3243–3250 (2005). Epub 2005 Apr 5
M. Wijaya, M. Huamei, Z. Jun, M. Du, Y. Li, Q. Chen, H. Chen, G. Song, Etiology of primary adrenal insufficiency in children: a 29-year singlecenter experience. J. Pediatr. Endocrinol. Metab. 32, 615–622 (2019)
T. Kirkgoz, T. Guran, Primary adrenal insufficiency in children: diagnosis and management. Best. Pr. Res Clin. Endocrinol. Metab. 32, 397–424 (2018). https://doi.org/10.1016/j.beem.2018.05.010
E. Kurnaz, P. Duminuco, Z. Aycan, Ş. Savaş-Erdeve, N. Muratoğlu Şahin, M. Keskin, E. Bayramoğlu, M. Bonomi, S. Çetinkaya, Clinical and genetic characterisation of a series of patients with triple A syndrome. Eur. J. Pediatr. 177(3 Mar), 363–369 (2018). https://doi.org/10.1007/s00431-017-3068-8. Epub 2017 Dec 19
R. Polat, A. Ustyol, E. Tuncez, T. Guran, A broad range of symptoms in allgrove syndrome: single center experience in Southeast Anatolia. J. Endocrinol. Investig. 43(2 Feb), 185–196 (2020). https://doi.org/10.1007/s40618-019-01099-2. Epub 2019 Aug 21
T. Milenkovic, D. Zdravkovic, N. Savic, S. Todorovic, K. Mitrovic, K. Koehler, A. Huebner, Triple A syndrome: 32 years experience of a single centre (1977-2008). Eur. J. Pediatr. 169(11), 1323–8 (2010). https://doi.org/10.1007/s00431-010-1222-7. Epub 2010 May 25
F. Gaiani, P. Gismondi, R. Minelli, G. Casadio, N. de’Angelis, F. Fornaroli, G.L. de’Angelis, M. Manfredi, Case report of a familial triple: a syndrome and review of the literature. Med. (Baltim.) 29(22), e20474 (2020). https://doi.org/10.1097/MD.0000000000020474. 99
F. Kallabi, N. Belghuith, H. Aloulou et al. Clinical and genetic characterization of 26 Tunisian patients with Allgrove syndrome. Arch. Med. Res. 47, 105–110 (2016). https://doi.org/10.1016/j.arcmed.2016.04.004
L.M. Walter, E.F. Christa. Adrenal cortex and its disorders. Pediatric Endocrinology. In: ed A. Sperling Mark (Elsevier Saunders: Philadelphia, 2014), p. 471–532.
H. Patt, K. Koehler, S. Lodha et al. Phenotype–genotype spectrum of AAA syndrome from Western India and systematic review of literature. Endocr. Connect. 6, 901–913 (2017). https://doi.org/10.1530/EC-17-0255
H.L. Storr, B. Kind, D.A. Parfitt et al. Deficiency of ferritin heavy-chain nuclear import in triple a syndrome implies nuclear oxidative damage as the primary disease mechanism. Mol. Endocrinol. 23, 2086–2094 (2009). https://doi.org/10.1210/me.2009-0056
M. Hirano, Y. Furiya, H. Asai, A. Yasui, S. Ueno, ALADINI482S causes selective failure of nuclear protein import and hypersensitivity to oxidative stress in triple A syndrome. Proc. Natl Acad. Sci. 103, 2298–2303 (2006). https://doi.org/10.1073/pnas.0505598103
E. Çamtosun, İ. Dündar, A. Akıncı, L. Kayaş, N. Çiftci, Pediatric Primary Adrenal Insufficiency: A 21-year Single Center Experience. J. Clin. Res Pediatr. Endocrinol. 13(1 Feb), 88–99 (2021). https://doi.org/10.4274/jcrpe.galenos.2020.2020.0132. Epub 2020 Sep 17
R. Lanes, L.P. Plotnick, T.E. Bynum et al. Glucocorticoid and partial mineralocorticoid deficiency associated with achalasia. J. Clin. Endocrinol. Metab. 50, 268–270 (1980). https://doi.org/10.1210/jcem-50-2-268
C.V. Collares, J. Antunes-Rodrigues, A.C. Moreira, S.N. Franca, L.A. Pereira, M.M. Soares, J. Elias Junior, A.J. Clark, M. de Castro, L.L. Elias, Heterogeneity in the molecular basis of ACTH resistance syndrome. Eur. J. Endocrinol. 159, 61–68 (2008). https://doi.org/10.1530/EJE-08-0079
M. Dumic, N. Barišic, V. Kusec, K. Stingl, M. Skegro, A. Stanimirovic, K. Koehler, A. Huebner, Long-term clinical follow-up and molecular genetic findings in eight patients with triple A syndrome. Eur. J. Pediatr. 171(10), 1453–9 (2012). https://doi.org/10.1007/s00431-012-1745-1. Epub 2012 Apr 28
A. Tebaibia, M.A. Boudjella, D. Boutarene, F. Benmediouni, H. Brahimi, N. Oumnia, Incidence, clinical features and para-clinical findings of achalasia in Algeria: experience of 25 years. World J. Gastroenterol. 22, 8615–8623 (2016). https://doi.org/10.3748/wjg.v22.i38.8615
C. Hallal, C.O. Kieling, D.L. Nunes, C.T. Ferreira, G. Peterson, S.G. Barros, C.A. Arruda, J.C. Fraga, H.A. Goldani, Diagnosis, misdiagnosis, and associated diseases of achalasia in children and adolescents: a twelve-year single center experience. Pediatr. Surg. Int. 28(12), 1211–1217 (2012). https://doi.org/10.1007/s00383-012-3214-3
A.E. Vallet, A. Verschueren, P. Petiot et al. Neurological features in adult Triple-A (Allgrove) syndrome. J. Neurol. 259, 39–46 (2012). https://doi.org/10.1007/s00415-011-6115-9
C. Goizet, B. Catargi, F. Tison, A. Tullio-Pelet, S. Hadj-Rabia, F. Pujol, A. Lagueny, S. Lyonnet, D. Lacombe, Progressive bulbospinal amyotrophy in triple A syndrome with AAAS gene mutation. Neurology 58(6), 962–965 (2002)
H. Houlden, S. Smith, M. De Carvalho, J. Blake, C. Mathias, N.W. Wood, M.M. Reilly, Clinical and genetic characterization of families with triple A (Allgrove) syndrome. Brain 125(Pt 12 Dec), 2681–90 (2002). https://doi.org/10.1093/brain/awf270
M. Gazarian, C.T. Cowell, M. Bonney, W.G. Grigor, The 4A syndrome: adrenocortical insufficiency associated with achalasia, alacrima, autonomic and other neurological abnormalities. Eur. J. Pediatr. 154, 18–23 (1995)
B. Kind, K. Koehler, M. Krumbholz, D. Landgraf, A. Huebner, Intracellular ROS level is increased in fibroblasts of triple A syndrome patients. J. Mol. Med (Berl.) 88, 1233–1242 (2010). https://doi.org/10.1007/s00109-010-0661-y
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The study was performed in accordance with the rules of Declaration of Helsinki and approved by the Institutional Ethics Committee of Gazi Yaşargil Training and Research Hospital (Document number: 22.07.2022/142).
Informed consent
Since the study was retrospective, informed consent was not available from the parents of the patients.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yıldırım, R., Unal, E., Tekmenuray-Unal, A. et al. The clinical and laboratory features of patients with triple A syndrome: a single-center experience in Turkey. Endocrine 79, 376–383 (2023). https://doi.org/10.1007/s12020-022-03206-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-022-03206-5