Abstract
Purpose
Evidences have shown that elevated lipoprotein(a) [Lp(a)] levels were associated with a lower risk of type 2 diabetes, but a higher risk of cardiovascular events in general populations. We aim to demonstrate the effect of Lp(a) concentrations on type 2 diabetes and cardiovascular events in a Chinese population with very high cardiovascular risk.
Methods
Seven hundred ninety-eight participants who underwent coronary angiography between March and November 2013 with normal glucose metabolism were followed up from July to December 2018.
Results
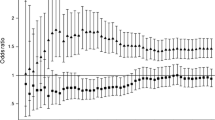
Five hundred thirty-five participants completed follow-up, and 395 of them had blood glucose data. Among 395 participants with blood glucose data, a total of 28 incident type 2 diabetes were identified during a median follow-up period of 4.42 years. Compared with the patients in the lowest tertile of Lp(a), the multifactorial adjusted HR for type 2 diabetes was 0.29 in the highest tertile (95% confidence intervals (CI) 0.10–0.89; P for trend = 0.03). Among 535 patients who completed follow-up, a total of 80 cases of major adverse cardiovascular events (MACE) were identified during a median follow-up period of 5.08 years. Compared with the patients in the lowest tertile of Lp(a), the multifactorial adjusted HR for MACE was 1.95 in the highest tertile (95% CI 1.05–3.65; P for trend = 0.03).
Conclusions
Elevated Lp(a) levels were associated with a lower risk of type 2 diabetes, but a higher risk of cardiovascular events in a Chinese population with very high cardiovascular risk.





Similar content being viewed by others
References
M.P. Stern, Diabetes and cardiovascular disease. The “common soil” hypothesis. Diabetes 44(4), 369–374 (1995). https://doi.org/10.2337/diab.44.4.369
D.L. Eaton, G.M. Fless, W.J. Kohr, J.W. McLean, Q.T. Xu, C.G. Miller, R.M. Lawn, A.M. Scanu, Partial amino acid sequence of apolipoprotein(a) shows that it is homologous to plasminogen. Proc. Natl Acad. Sci. USA 84(10), 3224–3228 (1987)
K. Schmidt, A. Noureen, F. Kronenberg, G. Utermann, Structure, function, and genetics of lipoprotein (a). J. Lipid Res. 57(8), 1339–1359 (2016). https://doi.org/10.1194/jlr.R067314
P.R. Kamstrup, A. Tybjærg-Hansen, R. Steffensen, B.G. Nordestgaard, Genetically elevated lipoprotein(a) and increased risk of myocardial infarction. JAMA 301(22), 2331–2339 (2009). https://doi.org/10.1001/jama.2009.801
D. Saleheen, P.C. Haycock, W. Zhao, A. Rasheed, A. Taleb, A. Imran, S. Abbas, F. Majeed, S. Akhtar, N. Qamar, K.S. Zaman, Z. Yaqoob, T. Saghir, S. Rizvi, A. Memon, N.H. Mallick, M. Ishaq, S.Z. Rasheed, F.U. Memon, K. Mahmood, N. Ahmed, P. Frossard, S. Tsimikas, J.L. Witztum, S. Marcovina, M. Sandhu, D.J. Rader, J. Danesh, Apolipoprotein(a) isoform size, lipoprotein(a) concentration, and coronary artery disease: a mendelian randomisation analysis. Lancet Diabetes Endocrinol. 5(7), 524–533 (2017). https://doi.org/10.1016/S2213-8587(17)30088-8
P.R. Kamstrup, M. Benn, A. Tybjærg-Hansen, B.G. Nordestgaard, Extreme lipoprotein(a) levels and risk of myocardial infarction in the general population. Circulation 117(2), 176–184 (2008). https://doi.org/10.1161/CIRCULATIONAHA.107.715698
S.S. Virani, A. Brautbar, B.C. Davis, V. Nambi, R.C. Hoogeveen, A.R. Sharrett, J. Coresh, T.H. Mosley, J.D. Morrisett, D.J. Catellier, A.R. Folsom, E. Boerwinkle, C.M. Ballantyne, Associations between lipoprotein(a) levels and cardiovascular outcomes in black and white subjects. Circulation 125(2), 241–249 (2012). https://doi.org/10.1161/CIRCULATIONAHA.111.045120
M.L. O’Donoghue, D.A. Morrow, S. Tsimikas, S. Sloan, A.F. Ren, E.B. Hoffman, N.R. Desai, S.D. Solomon, M. Domanski, K. Arai, S.E. Chiuve, C.P. Cannon, F.M. Sacks, M.S. Sabatine, Lipoprotein(a) for risk assessment in patients with established coronary artery disease. J. Am. Coll. Cardiol. 63(6), 520–527 (2014). https://doi.org/10.1016/j.jacc.2013.09.042
W. Dai, J. Long, Y. Cheng, Y. Chen, S. Zhao, Elevated plasma lipoprotein(a) levels were associated with increased risk of cardiovascular events in Chinese patients with stable coronary artery disease. Sci. Rep. 8(1) (2018). https://doi.org/10.1038/s41598-018-25835-5
K.L. Chien, H.C. Hsu, T.C. Su, F.C. Sung, M.F. Chen, Y.T. Lee, Lipoprotein(a) and cardiovascular disease in ethnic Chinese: The Chin-Shan Community Cardiovascular Cohort Study. Clin. Chem. 54(2), 285–291 (2008). https://doi.org/10.1373/clinchem.2007.090969
S. Mora, P.R. Kamstrup, N. Rifai, B.G. Nordestgaard, J.E. Buring, P.M. Ridker, Lipoprotein(a) and risk of type 2 diabetes. Clin. Chem. 56(8), 1252–1260 (2010). https://doi.org/10.1373/clinchem.2010.146779
Z. Ye, P.C. Haycock, D. Gurdasani, C. Pomilla, S.M. Boekholdt, S. Tsimikas, K.T. Khaw, N.J. Wareham, M.S. Sandhu, N.G. Forouhi, The association between circulating lipoprotein(a) and type 2 diabetes: is it causal? Diabetes 63(1), 332–342 (2013). https://doi.org/10.2337/db13-1144
E. Rhee, J.H. Cho, D.Y. Lee, H. Kwon, S.E. Park, C. Park, K. Oh, S. Park, W. Lee, Insulin resistance contributes more to the increased risk for diabetes development in subjects with low lipoprotein(a) level than insulin secretion. PLoS ONE 12(5), e177500 (2017). https://doi.org/10.1371/journal.pone.0177500
E. Paige, K.L. Masconi, S. Tsimikas, F. Kronenberg, P. Santer, S. Weger, J. Willeit, S. Kiechl, P. Willeit, Lipoprotein(a) and incident type-2 diabetes: results from the prospective Bruneck study and a meta-analysis of published literature. Cardiovasc. Diabetol. 16(1) (2017). https://doi.org/10.1186/s12933-017-0520-z
L. Ding, A. Song, M. Dai, M. Xu, W. Sun, B. Xu, J. Sun, T. Wang, Y. Xu, J. Lu, W. Wang, Y. Bi, G. Ning, Serum lipoprotein (a) concentrations are inversely associated with T2D, prediabetes, and insulin resistance in a middle-aged and elderly Chinese population. J. Lipid Res. 56(4), 920–926 (2015). https://doi.org/10.1194/jlr.P049015
D. Mu-Han-Ha-Li, T. Zhai, Y. Ling, X. Gao, LPA kringle IV type 2 is associated with type 2 diabetes in a Chinese population with very high cardiovascular risk. J. Lipid Res. 59(5), 884–891 (2018). https://doi.org/10.1194/jlr.P082792
American Diabetes Association, 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2018. Diabetes Care 41(Suppl. 1), S13–S27 (2018). https://doi.org/10.2337/dc18-S002
D.L. Rainwater, S.M. Haffner, Insulin and 2-hour glucose levels are inversely related to Lp(a) concentrations controlled for LPA genotype. Arterioscler. Thromb. Vasc. Biol. 18(8), 1335–1341 (1998). https://doi.org/10.1161/01.ATV.18.8.1335
A. Kaya, A. Onat, H. Yuksel, G. Can, M. Yuksel, E. Ademoglu, Lipoprotein(a)-activated immunity, insulin resistance and new-onset diabetes. Postgrad. Med. 129(6), 611–618 (2017). https://doi.org/10.1080/00325481.2017.1342508
D.M. Neele, E.C. de Wit, H.M. Princen, Insulin suppresses apolipoprotein(a) synthesis by primary cultures of cynomolgus monkey hepatocytes. Diabetologia 42(1), 41–44 (1999)
M.B. Boffa, M.L. Koschinsky, Lipoprotein (a): truly a direct prothrombotic factor in cardiovascular disease? J. Lipid Res. 57(5), 745–757 (2016). https://doi.org/10.1194/jlr.R060582
F.M. van der Valk, S. Bekkering, J. Kroon, C. Yeang, J. Van den Bossche, J.D. van Buul, A. Ravandi, A.J. Nederveen, H.J. Verberne, C. Scipione, M. Nieuwdorp, L.A. Joosten, M.G. Netea, M.L. Koschinsky, J.L. Witztum, S. Tsimikas, N.P. Riksen, E.S. Stroes, Oxidized phospholipids on lipoprotein(a) elicit arterial wall inflammation and an inflammatory monocyte response in humans. Circulation 134(8), 611–624 (2016). https://doi.org/10.1161/CIRCULATIONAHA.116.020838
H.G. Kraft, H.J. Menzel, F. Hoppichler, W. Vogel, G. Utermann, Changes of genetic apolipoprotein phenotypes caused by liver transplantation. Implications for apolipoprotein synthesis. J. Clin. Investig. 83(1), 137–142 (1989). https://doi.org/10.1172/JCI113849
S. Erqou, A. Thompson, E. Di Angelantonio, D. Saleheen, S. Kaptoge, S. Marcovina, J. Danesh, Apolipoprotein(a) isoforms and the risk of vascular disease. J. Am. Coll. Cardiol. 55(19), 2160–2167 (2010). https://doi.org/10.1016/j.jacc.2009.10.080
A. Tolbus, M.B. Mortensen, S.F. Nielsen, P.R. Kamstrup, S.E. Bojesen, B.G. Nordestgaard, Kringle IV type 2, not low lipoprotein(a), as a cause of diabetes: a novel genetic approach using SNPs associated selectively with lipoprotein(a) concentrations or with kringle IV type 2 repeats. Clin. Chem. 63(12), 1866–1876 (2017). https://doi.org/10.1373/clinchem.2017.277103
P.R. Kamstrup, B.G. Nordestgaard, Lipoprotein(a) concentrations, isoform size, and risk of type 2 diabetes: a Mendelian randomisation study. The lancet. Diabetes Endocrinol. 1(3), 220–227 (2013). https://doi.org/10.1016/S2213-8587(13)70064-0
Author information
Authors and Affiliations
Contributions
Y.L. conceived and designed the study. D.M., T.Z., and Z.C. contributed to the data collection. D.M. contributed to the management and analysis of data. D.M. and Y.L. wrote and revised the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Muhanhali, D., Zhai, T., Cai, Z. et al. Lipoprotein(a) concentration is associated with risk of type 2 diabetes and cardiovascular events in a Chinese population with very high cardiovascular risk. Endocrine 69, 63–72 (2020). https://doi.org/10.1007/s12020-020-02286-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02286-5