Abstract
Purpose
Emerging clinical evidence has implied that alkaline phosphatase (ALP) may contribute to gestational diabetes mellitus (GDM). However, there were no studies to reveal the independent and prospective associations between ALP and GDM. Our aim was to explore the independent and prospective associations between early maternal ALP level and GDM risk and glucose regulation.
Methods
In a prospective cohort study with 2073 singleton mothers at four maternity units in China, maternal serum ALP levels were measured before 20 gestational weeks. Using logistic regression, we analyzed the relationship between maternal ALP level and risk of GDM. We further explored the relationships of ALP level to fasting blood glucose (FBG), 1-h and 2-h post-load blood glucose (1-h, 2-h PBG) with multiple linear regression. Finally, we analyzed the association between maternal ALP level and isolated impaired fasting glucose (i-IFG) and isolated impaired glucose tolerance (i-IGT) risk.
Results
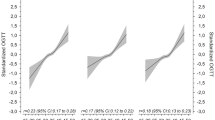
The maximum value of maternal ALP level was 90 U/L, within the normal range. After adjustment for confounding factors, the odds ratio (ORs) of GDM increased linearly with ALP level (p for overall association = 0.002, p for nonlinear association = 0.799), with the OR comparing the highest versus lowest quartile of 2.47 (95% CI 1.47, 4.15). Moreover, each additional of 10 U/L ALP level was associated with a 2% higher FBG (p = 0.043) and a 12% higher 1-h PBG (p = 0.004). Higher ALP level also increased the risk of i-IFG (OR 3.73, 95% CI 1.17–11.86) and i-IGT (OR 2.03, 95% CI 1.07–3.84).
Conclusions
Even within the upper limit of normal, higher early maternal ALP level could increase the risk of GDM. Moreover, both FBG and PBG were increased with early maternal ALP.


Similar content being viewed by others
References
E. Chiefari, B. Arcidiacono, D. Foti, A. Brunetti, Gestational diabetes mellitus: an updated overview. J. Endocrinol. Invest 40(9), 899–909 (2017)
P.M. Catalano, H.D. McIntyre, J.K. Cruickshank, D.R. McCance, A.R. Dyer, B.E. Metzger, L.P. Lowe, E.R. Trimble, D.R. Coustan, D.R. Hadden, B. Persson, M. Hod, J.J. Oats; Group, H.S.C.R., The hyperglycemia and adverse pregnancy outcome study: associations of GDM and obesity with pregnancy outcomes. Diabetes Care 35(4), 780–786 (2012)
N.J. Fernandez, B.A. Kidney, Alkaline phosphatase: beyond the liver. Vet. Clin. Pathol. 36(3), 223–233 (2007)
U. Sharma, D. Pal, R. Prasad, Alkaline phosphatase: an overview. Indian J. Clin. Biochem. 29(3), 269–278 (2014)
E. Epstein, F.L. Kiechle, J.D. Artiss, B. Zak, The clinical use of alkaline phosphatase enzymes. Clin. Lab. Med. 6(3), 491–505 (1986)
F.A. Aleem, Total and heat-stable serum alkaline phosphatase in normal and abnormal pregnancies. Obstet. Gynecol. 40(2), 163–172 (1972)
F. Schiele, J. Henny, J. Hitz, C. Petitclerc, R. Gueguen, G. Siest, Total bone and liver alkaline phosphatases in plasma: biological variations and reference limits. Clin. Chem. 29(4), 634–641 (1983)
G.M. Rao, L.O. Morghom, Correlation between serum alkaline phosphatase activity and blood glucose levels. Enzyme 35(1), 57–59 (1986)
G. Sesti, T.V. Fiorentino, M.L. Hribal, A. Sciacqua, F. Perticone, Association of hepatic insulin resistance indexes to nonalcoholic fatty liver disease and related biomarkers. Nutr. Metab. Cardiovasc. Dis. 23(12), 1182–1187 (2013)
J. Vangipurapu, A. Stancakova, T. Kuulasmaa, J. Paananen, J. Kuusisto, E.-R.S. Group, E. Ferrannini, M. Laakso, A novel surrogate index for hepatic insulin resistance. Diabetologia 54(3), 540–543 (2011)
S.C. Chen, S.P. Tsai, J.Y. Jhao, W.K. Jiang, C.K. Tsao, L.Y. Chang, Liver Fat, hepatic enzymes, alkaline phosphatase and the risk of incident type 2 diabetes: a prospective study of 132,377 adults. Sci. Rep. 7(1), 4649 (2017)
J. Wojcicka-Bentyn, K. Czajkowski, J. Sienko, M. Grymowicz, M. Bros, Extremely elevated activity of serum alkaline phosphatase in gestational diabetes: a case report. Am. J. Obstet. Gynecol. 190(2), 566–567 (2004)
S. Lozo, A. Atabeygi, M. Healey, Extreme elevation of alkaline phosphatase in a pregnancy complicated by gestational diabetes and infant with neonatal alloimmune thrombocytopenia. Case Rep. Obstet. Gynecol. 2016, 4896487 (2016)
S.S. Siddiqi, A.G. Borse, A. Pervez, S. Anjum, A study of bone turnover markers in gestational diabetes mellitus. Indian J. Endocrinol. Metab. 21(1), 38–44 (2017)
H. Zhang, X. Qiu, C. Zhong, K. Zhang, M. Xiao, N. Yi, G. Xiong, J. Wang, J. Yao, L. Hao, S. Wei, N. Yang, X. Yang, Reproducibility and relative validity of a semi-quantitative food frequency questionnaire for Chinese pregnant women. Nutr. J. 14, 56 (2015)
T. Xiong, C. Zhong, X. Zhou, R. Chen, M. Xiao, Y. Wu, X. Hu, W. Wang, X. Li, C. Liu, G. Xiong, X. Yang, L. Hao, N. Yang, Maternal circulating transthyretin level is longitudinally associated with increased risk of gestational diabetes mellitus: it is not just an indicator of nutritional status. Diabetes Care 40(5), e53–e54 (2017)
B.E. Metzger, S.G. Gabbe, B. Persson et al. Consensus Panel International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care 33(3), 676–682 (2010). International Association of Diabetes and Pregnancy Study Groups
M.H. Black, D.A. Sacks, A.H. Xiang, J.M. Lawrence, Clinical outcomes of pregnancies complicated by mild gestational diabetes mellitus differ by combinations of abnormal oral glucose tolerance test values. Diabetes Care 33(12), 2524–2530 (2010)
M. Nannipieri, C. Gonzales, S. Baldi, R. Posadas, K. Williams, S.M. Haffner, M.P. Stern, E. Ferrannini; Mexico City diabetes, s., Liver enzymes, the metabolic syndrome, and incident diabetes: the Mexico City diabetes study. Diabetes Care 28(7), 1757–1762 (2005)
J. Liu, S.L. Au Yeung, S.L. Lin, G.M. Leung, C.M. Schooling, Liver enzymes and risk of ischemic heart disease and type 2 diabetes mellitus: a mendelian randomization study. Sci. Rep. 6, 38813 (2016)
K. Bora, M. Borah, H. Chutia, C.K. Nath, D. Das, A.A. Ruram, Presence of concurrent derangements of liver function tests in type 2 diabetes and their relationship with glycemic status: a retrospective observational study from Meghalaya. J. Lab. Physicians 8(1), 30–35 (2016)
E. Sivan, X. Chen, C.J. Homko, E.A. Reece, G. Boden, Longitudinal study of carbohydrate metabolism in healthy obese pregnant women. Diabetes Care 20(9), 1470–1475 (1997)
P.M. Catalano, E.D. Tyzbir, R.R. Wolfe, J. Calles, N.M. Roman, S.B. Amini, E.A. Sims, Carbohydrate metabolism during pregnancy in control subjects and women with gestational diabetes. Am. J. Physiol. 264(1 Pt 1), E60–E67 (1993)
A.T. Ali, C.B. Penny, J.E. Paiker, G. Psaras, F. Ikram, N.J. Crowther, The relationship between alkaline phosphatase activity and intracellular lipid accumulation in murine 3T3-L1 cells and human preadipocytes. Anal. Biochem. 354(2), 247–254 (2006)
E.J. Boyko, W.Y. Fujimoto, D.L. Leonetti, L. Newell-Morris, Visceral adiposity and risk of type 2 diabetes: a prospective study among Japanese Americans. Diabetes Care 23(4), 465–471 (2000)
T. Hayashi, E.J. Boyko, D.L. Leonetti, M.J. McNeely, L. Newell-Morris, S.E. Kahn, W.Y. Fujimoto, Visceral adiposity and the risk of impaired glucose tolerance: a prospective study among Japanese Americans. Diabetes Care 26(3), 650–655 (2003)
M. Shibata, Y. Kihara, M. Taguchi, M. Tashiro, M. Otsuki, Nonalcoholic fatty liver disease is a risk factor for type 2 diabetes in middle-aged Japanese men. Diabetes Care 30(11), 2940–2944 (2007)
H. Yki-Jarvinen, Non-alcoholic fatty liver disease as a cause and a consequence of metabolic syndrome. Lancet Diabetes Endocrinol. 2(11), 901–910 (2014)
T. Fukuda, M. Hamaguchi, T. Kojima, K. Mitsuhashi, Y. Hashimoto, A. Ohbora, T. Kato, N. Nakamura, M. Fukui, Transient remission of nonalcoholic fatty liver disease decreases the risk of incident type 2 diabetes mellitus in Japanese men. Eur. J. Gastroenterol. Hepatol. 28(12), 1443–1449 (2016)
A. Kerner, O. Avizohar, R. Sella, P. Bartha, O. Zinder, W. Markiewicz, Y. Levy, G.J. Brook, D. Aronson, Association between elevated liver enzymes and C-reactive protein: possible hepatic contribution to systemic inflammation in the metabolic syndrome. Arterioscler Thromb. Vasc. Biol. 25(1), 193–197 (2005)
M. Wolf, L. Sandler, K. Hsu, K. Vossen-Smirnakis, J.L. Ecker, R. Thadhani, First-trimester C-reactive protein and subsequent gestational diabetes. Diabetes Care 26(3), 819–824 (2003)
G.J. Valenzuela, L.A. Munson, N.M. Tarbaux, J.R. Farley, Time-dependent changes in bone, placental, intestinal, and hepatic alkaline phosphatase activities in serum during human pregnancy. Clin. Chem. 33(10), 1801–1806 (1987)
A.B. Okesina, D. Donaldson, P.T. Lascelles, P. Morris, Effect of gestational age on levels of serum alkaline phosphatase isoenzymes in healthy pregnant women. Int J. Gynaecol. Obstet. 48(1), 25–29 (1995)
Acknowledgements
The authors gratefully acknowledge the cooperation of the pregnant women who took part in this study. We also thank the staff at the maternity clinics of Hubei Maternal and Child Health Hospital and The Central Hospital of Wuhan for their considerable assistance with many aspects of this study. We are sincerely grateful to everyone in Tongji Maternal and Child Health Cohort Study Group.
Author contributions
N.Y., X.Y., and L.H. designed the study; T.X., C.Z., G.S., X.Z., R.C., Q.L., Y.W., Q.G., L.H., X.H., and M.X. researched the data; T.X. drafted the paper; L.H. and N.Y. reviewed/edited the paper and contributed to discussion. N.Y. was the guarantor of this work.
Funding
This work was supported by the National Program on Basic Research Project of China (No. 2013FY114200) and China Postdoctoral Science Foundation (No. 2018M632877).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the Ethics Review Committee of Tongji Medical College, Huazhong University of Science and Technology (No. 201302).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
These authors contributed equally: Liping Hao, Nianhong Yang
Supplementary information
Rights and permissions
About this article
Cite this article
Xiong, T., Zhong, C., Sun, G. et al. Early maternal circulating alkaline phosphatase with subsequent gestational diabetes mellitus and glucose regulation: a prospective cohort study in China. Endocrine 65, 295–303 (2019). https://doi.org/10.1007/s12020-019-01954-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-019-01954-5