Abstract
Purpose
Despite the well-known deleterious effects of cortisol on skeletal muscle, whether subtle cortisol excess in subclinical hypercortisolism (SH) affects skeletal muscle mass is unknown. Our objective was to understand the effects of the cortisol level on skeletal muscle mass in patients with SH.
Methods
We compared skeletal muscle mass and fat mass (FM) between 21 patients with SH (12 women and 9 men) and 224 controls (67 women and 157 men) with nonfunctioning adrenal incidentaloma (NFAI). Medical records were reviewed, and we measured body composition parameters using bioelectrical impedance analysis and serum cortisol levels after the overnight 1-mg dexamethasone suppression test (DST).
Results
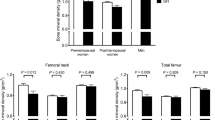
After adjusting for confounding factors, 1-mg DST levels were inversely correlated with appendicular skeletal muscle mass (ASM) (γ = −0.245, P = 0.040), lower limb ASM (γ = −0.244, P = 0.040), and appendicular skeletal muscle index (ASMI; height-adjusted ASM) (γ = −0.229, P = 0.048) in all women, but not men. ASM and ASMI were significantly lower by 6.2% (P = 0.033) and 5.9% (P = 0.046), respectively, in women with SH compared with those with NFAI, but not men. Conversely, FM and percent fat mass were similar between the two groups. Compared with women with NFAI, among those with SH, lower limb, but not upper limb, ASM was lower by 6.8% (P = 0.020).
Conclusions
This study showed that women with SH had lower skeletal muscle mass, especially of the lower limb, and suggested that subtle cortisol excess also has adverse effects on skeletal muscle metabolism.




Similar content being viewed by others
References
L.K. Chen, L.K. Liu, J. Woo, P. Assantachai, T.W. Auyeung, K.S. Bahyah, M.Y. Chou, L.Y. Chen, P.S. Hsu, O. Krairit, J.S. Lee, W.J. Lee, Y. Lee, C.K. Liang, P. Limpawattana, C.S. Lin, L.N. Peng, S. Satake, T. Suzuki, C.W. Won, C.H. Wu, S.N. Wu, T. Zhang, P. Zeng, M. Akishita, H. Arai, Sarcopenia in Asia: consensus report of the Asian Working Group for sarcopenia. J. Am. Med. Dir. Assoc. 15, 95–101 (2014)
L.K. Chen, W.J. Lee, L.N. Peng, L.K. Liu, H. Arai, M. Akishita, Asian Working Group for Sarcopenia Recent advances in sarcopenia research in Asia: 2016 update from the Asian Working Group for sarcopenia. J. Am. Med. Dir. Assoc. 17, 767.e1–767.e7 (2016).
Y.S. Kim, Y. Lee, Y.S. Chung, D.J. Lee, N.S. Joo, D. Hong, G. Song, H.J. Kim, Y.J. Choi, K.M. Kim, Prevalence of sarcopenia and sarcopenic obesity in the Korean population based on the Fourth Korean National Health and Nutritional Examination Surveys. J. Gerontol. A. Biol. Sci. Med. Sci. 67, 1107–1113 (2012)
M. Ryu, J. Jo, Y. Lee, Y.S. Chung, K.M. Kim, W.C. Baek, Association of physical activity with sarcopenia and sarcopenic obesity in community-dwelling older adults: the Fourth Korea National Health and Nutrition Examination Survey. Age. Ageing 42, 734–740 (2013)
M. Fassnacht, W. Arlt, I. Bancos, H. Dralle, J. Newell-Price, A. Sahdev, A. Tabarin, M. Terzolo, S. Tsagarakis, O.M. Dekkers, Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 175, G1–G34 (2016)
G. Di Dalmazi, R. Pasquali, F. Beuschlein, M. Reincke, Subclinical hypercortisolism: a state, a syndrome, or a disease? Eur. J. Endocrinol. 173, M61–M71 (2015)
A.A. Khaleeli, R.H. Edwards, K. Gohil, G. McPhail, M.J. Rennie, J. Round, E.J. Ross, Corticosteroid myopathy: a clinical and pathological study. Clin. Endocrinol. 18, 155–166 (1983)
M.A. Minetto, F. Lanfranco, A. Botter, G. Motta, G. Mengozzi, R. Giordano, A. Picu, E. Ghigo, E. Arvat, Do muscle fiber conduction slowing and decreased levels of circulating muscle proteins represent sensitive markers of steroid myopathy? A pilot study in Cushing’s disease. Eur. J. Endocrinol. 164, 985–993 (2011)
R. Muller, E. Kugelberg, Myopathy in Cushing’s syndrome. J. Neurol. Neurosurg. Psychiatry 22, 314–319 (1959)
E. Olafsson, H.R. Jones Jr., A.T. Guay, C.B. Thomas, Myopathy of endogenous Cushing’s syndrome: a review of the clinical and electromyographic features in 8 patients. Muscle Nerve. 17, 692–693 (1994)
A.C. Ammini, N. Tandon, N. Gupta, A.S. Bhalla, K. Devasenaspathy, G. Kumar, J.P. Sahoo, S. Chittawar, J. Philip, M.P. Baruah, C.S. Dwarakanath, S. Tripathi, Etiology and clinical profile of patients with Cushing’s syndrome: a single center experience. Indian J. Endocrinol. Metab. 18, 99–105 (2014)
M.J. Bolland, I.M. Holdaway, J.E. Berkeley, S. Lim, W.J. Dransfield, J.V. Conaglen, M.S. Croxson, G.D. Gamble, P.J. Hunt, R.J. Toomath, Mortality and morbidity in Cushing’s syndrome in New Zealand. Clin. Endocrinol. 75, 436–442 (2011)
F. Pecori Giraldi, M. Moro, F. Cavagnini, Study Group on the Hypothalamo-Pituitary-Adrenal Axis of the Italian Society of Endocrinology, Gender-related differences in the presentation and course of Cushing’s disease. J. Clin. Endocrinol. Metab. 88, 1554–1558 (2003).
M.A. Minetto, F. Lanfranco, G. Motta, S. Allasia, E. Arvat, G. D’Antona, Steroid myopathy: some unresolved issues. J. Endocrinol. Invest. 34, 370–375 (2011)
F. Ferrau, M. Korbonits, Metabolic comorbidities in Cushing’s syndrome. Eur. J. Endocrinol. 173, M133–M157 (2015)
S.H. Lee, K.H. Song, J. Kim, S. Park, S.H. Ahn, H. Kim, Y.Y. Cho, S. Suh, B.J. Kim, J.H. Kim, J.M. Koh, New diagnostic criteria for subclinical hypercortisolism using postsurgical hypocortisolism: the Co-work of Adrenal Research study. Clin. Endocrinol. 86, 10–18 (2017)
I. Chiodini, Clinical review: diagnosis and treatment of subclinical hypercortisolism. J. Clin. Endocrinol. Metab. 96, 1223–1236 (2011)
D.A. Delivanis, N.M. Iniguez-Ariza, M.H. Zeb, M.R. Moynagh, N. Takahashi, T.J. McKenzie, M.A. Thomas, C. Gogos, W.F. Young, I. Bancos, V. Kyriazopoulou, Impact of hypercortisolism on skeletal muscle mass and adipose tissue mass in patients with adrenal adenomas. Clin. Endocrinol. 88, 209–216 (2018)
E. Van Cauter, R. Leproult, D.J. Kupfer, Effects of gender and age on the levels and circadian rhythmicity of plasma cortisol. J. Clin. Endocrinol. Metab. 81, 2468–2473 (1996)
V. Messier, R. Rabasa-Lhoret, S. Barbat-Artigas, B. Elisha, A.D. Karelis, M. Aubertin-Leheudre, Menopause and sarcopenia: a potential role for sex hormones. Maturitas 68, 331–336 (2011)
I. Janssen, S.B. Heymsfield, R.N. Baumgartner, R. Ross, Estimation of skeletal muscle mass by bioelectrical impedance analysis. J. Appl. Physiol. (1985) 89, 465–471 (2000).
M. Tosato, E. Marzetti, M. Cesari, G. Savera, R.R. Miller, R. Bernabei, F. Landi, R. Calvani, Measurement of muscle mass in sarcopenia: from imaging to biochemical markers. Aging Clin. Exp. Res. 29, 19–27 (2017)
M. Drey, C.M. Berr, M. Reincke, J. Fazel, J. Seissler, J. Schopohl, M. Bidlingmaier, S. Zopp, N. Reisch, F. Beuschlein, A. Osswald, R. Schmidmaier, Cushing’s syndrome: a model for sarcopenic obesity. Endocrine 57, 481–485 (2017)
G. Woodrow, Y. Devine, M. Cullen, E. Lindley, Application of bioelectrical impedance to clinical assessment of body composition in peritoneal dialysis. Perit. Dial. Int.: J. Int. Soc. Perit. Dial. 27, 496–502 (2007)
L. Barzon, N. Sonino, F. Fallo, G. Palu, M. Boscaro, Prevalence and natural history of adrenal incidentalomas. Eur. J. Endocrinol. 149, 273–285 (2003)
F. Mantero, M. Terzolo, G. Arnaldi, G. Osella, A.M. Masini, A. Ali, M. Giovagnetti, G. Opocher, A. Angeli, A survey on adrenal incidentaloma in Italy. Study Group on Adrenal Tumors of the Italian Society of Endocrinology. J. Clin. Endocrinol. Metab. 85, 637–644 (2000)
A.R. Hong, J.H. Kim, K.S. Park, K.Y. Kim, J.H. Lee, S.H. Kong, S.Y. Lee, C.S. Shin, S.W. Kim, S.Y. Kim, Optimal follow-up strategies for adrenal incidentalomas: reappraisal of the 2016 ESE-ENSAT guidelines in real clinical practice. Eur. J. Endocrinol. 177, 475–483 (2017)
I. Chiodini, V. Morelli, B. Masserini, A.S. Salcuni, C. Eller-Vainicher, R. Viti, F. Coletti, G. Guglielmi, C. Battista, V. Carnevale, L. Iorio, P. Beck-Peccoz, M. Arosio, B. Ambrosi, A. Scillitani, Bone mineral density, prevalence of vertebral fractures, and bone quality in patients with adrenal incidentalomas with and without subclinical hypercortisolism: an Italian multicenter study. J. Clin. Endocrinol. Metab. 94, 3207–3214 (2009)
V. Morelli, F. Donadio, C. Eller-Vainicher, V. Cirello, L. Olgiati, C. Savoca, E. Cairoli, A.S. Salcuni, P. Beck-Peccoz, I. Chiodini, Role of glucocorticoid receptor polymorphism in adrenal incidentalomas. Eur. J. Clin. Invest. 40, 803–811 (2010)
H. Siggelkow, M. Etmanski, S. Bozkurt, P. Grobeta, R. Koepp, J. Brockmoller, M.V. Tzvetkov, Genetic polymorphisms in 11beta-hydroxysteroid dehydrogenase type 1 correlate with the postdexamethasone cortisol levels and bone mineral density in patients evaluated for osteoporosis. J. Clin. Endocrinol. Metab. 99, E293–E302 (2014)
A. Szappanos, A. Patocs, P. Gergics, R. Bertalan, A. Kerti, B. Acs, K. Feldmann, K. Racz, M. Toth, The 83,557insA variant of the gene coding 11beta-hydroxysteroid dehydrogenase type 1 enzyme associates with serum osteocalcin in patients with endogenous Cushing’s syndrome. J. Steroid Biochem. Mol. Biol. 123, 79–84 (2011)
Acknowledgements
This study was supported by grants from the Asan Institute for Life Sciences, Seoul, Republic of Korea (Project No.2014-1215).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
These authors are co-first authors: Jae Hyeon Kim and Mi Kyung Kwak.
Rights and permissions
About this article
Cite this article
Kim, J.H., Kwak, M.K., Ahn, S.H. et al. Alteration in skeletal muscle mass in women with subclinical hypercortisolism. Endocrine 61, 134–143 (2018). https://doi.org/10.1007/s12020-018-1598-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-018-1598-0