Abstract
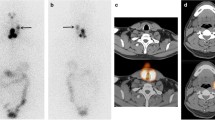
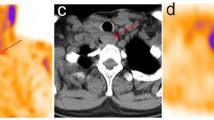
The purpose of this prospective study was to determine the incremental diagnostic value of single photon emission computed tomography/computed tomography with iodine-131 over planar whole body scan in the staging of patients with differentiated thyroid carcinoma. A total of 365 patients (270 female, 95 male) with differentiated thyroid carcinoma were treated with radioiodine therapy for thyroid remnant ablation with radical intent after thyroidectomy between January 2013 and November 2014. In addition to planar whole body scan, single photon emission computed tomography/computed tomography of neck and chest were performed. Each radioactive focus at whole body scan was classified as positive or equivocal with respect of specific territories: thyroid bed, cervical lymph nodes and distant metastases.Whole-body scan detected focal uptake in 353 patients and no uptake in 12. The location was considered equivocal in 100. Single photon emission computed tomography/computed tomography detected focal uptake in 356 patients and no uptake in nine. In three patients with negative wholebody scan, single photon emission computed tomography/computed tomography provided information about residual activity in the thyroid bed. By single photon emission computed tomography/computed tomography the location was equivocal in 18 patients only. Single photon emission computed tomography/computed tomography was helpful in 82 out of 100 patients with equivocal findings by whole body scan allowing a correct identification of the uptake sites. In a great number of equivocal whole body scan, due to high remnant activity, single photon emission computed tomography/computed tomography was able to differentiate between thyroid remnant and lymph nodes uptake. In 22 out of 100 patients with doubtful whole body scan, single photon emission computed tomography/computed tomography correctly identified nodal or distant metastases, and in 2/100 patients, focal uptake classified as metastatic by whole body scan was reclassified as para-physiological by single photon emission computed tomography/computed tomography. The TNM classification changed in 13 out of 22 patients. Single photon emission computed tomography/computed tomography improves detection and localization of the iodine-131 uptake after thyroidectomy in patients with differentiated thyroid carcinoma and it is more accurate than whole body scan to evaluate lymph nodes and to identify and characterize distant metastases. Single photon emission computed tomography/computed tomography aids assessment of lower/upper stage in a significant number of patients with differentiated thyroid carcinoma and it can affect therapy decision-making and patient management.



Similar content being viewed by others
Abbreviations
- SPECT/CT:
-
single photon emission computed tomography/computed tomography
- WBS:
-
planar whole body scan
- DTC:
-
differentiated thyroid carcinoma
- LN:
-
neck lymph node
- rhTSH:
-
recombinant human thyrotropin
- HEGP:
-
high-energy general purpose
- ABC:
-
automatic body contouring
References
L. Davies, H.G. Welch, Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295, 2164–2167 (2006)
S.A. Hundahl, I.D. Fleming, A.M. Fremgen, H.R. Menck, A National Cancer Data Base report on 53,856 cases of thyroid carcinoma treated in the U.S., 1985–1995. Cancer 83, 2638–2648 (1998)
E.P. Simard, E.M. Ward, R. Siegel, A. Jemal, Cancers with increasing incidence trends in the United States: 1999 through 2008. CA Cancer J. Clin. 62(2), 118–128 (2012)
S.F. Dinneen, M.J. Valimaki, E.J. Bergstralh, J.R. Goellner, C.A. Gorman, I.D. Hay, Distant metastases in papillary thyroid carcinoma:100 cases observed at one institution during 5 decades. J. Clin. Endocrinol. Metab. 80(7), 2041–2045 (1995)
F. Pacini et al., Post-surgical use of radioiodine (131I) in patients with papillary and follicular thyroid cancer and the issue of remnant ablation: a consensus report. Eur. J. Endocrinol. 153(5), 651–659 (2005)
M. Luster, S.E. Clarke, M. Dietlein et al., Guidelines for radioiodine therapy of differentiated thyroid cancer. Eur. J. Nucl. Med. Mol. Imaging 35(10), 1941–1959 (2008)
B.R. Haugen, E.K. Alexander, K.C. Bible, G.M. Doherty, S.J. Mandel, Y.E. Nikiforov, F. Pacini, G.W. Randolph, A.M. Sawka, M. Schlumberger, K.G. Schuff, S.I. Sherman, J.A. Sosa, D.L. Steward, R.M. Tuttle, L. Wartofsky, 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid 26(1), 1–133 (2016)
M. Schlumberger, C. Challeton, F. De Vathaire et al., Radioactive iodine treatment and external radiotherapy for lung and bone metastases from thyroid carcinoma. J. Nucl. Med. 37(4), 598–605 (1996)
E.L. Mazzaferri, S.M. Jhiang, Long-term impact of initial surgical and medical therapy on papillary and follicular thyroid cancer. Am. J. Med. 97, 418–428 (1994)
S.I. Sherman, Thyroid carcinoma. Lancet 361, 501–511 (2003)
W.G. Spies, C.H. Wojtowicz, S.M. Spies, A.Y. Shah, A.M. Zimmer, Value of post-therapy whole-body I-131 imaging in the evaluation of patients with thyroid carcinoma having undergone high-dose I- 131 therapy. Clin. Nucl. Med 14, 793–800 (1989)
M. Filesi, A. Signore, G. Ventroni, F.F. Melacrinis, G. Ronga, Role of initial iodine-131 whole-body scan and serum thyroglobulin in differentiated thyroid carcinoma metastases. J. Nucl. Med. 39, 1542–1546 (1998)
K. Tharp, O. Israel, J. Hausmann et al., Impact of 131I-SPECT/CT images obtained with an integrated system in the follow-up of patients with thyroid carcinoma. Eur. J. Nucl. Med. Mol. Imaging 31(10), 1435–1442 (2004)
J. Ruf, L. Lehmkuhl, H. Bertram et al., Impact of SPECT and integrated low-dose CT after radioiodine therapy on the management of patients with thyroid carcinoma. Nucl. Med. Commun. 25(12), 1177–1182 (2004)
L. Chen, Q. Luo, Y. Shen et al., Incremental value of 131I SPECT/CT in the management of patients with differentiated thyroid carcinoma. J. Nucl. Med. 49(12), 1952–1957 (2008)
K.K. Wong, N. Zarzhevsky, J.M. Cahill, K.A. Frey, A.M. Avram, Incremental value of diagnostic 131I SPECT/CT fusion imaging in the evaluation of differentiated thyroid carcinoma. Am. J. Roentgenol. 191(6), 1785–1794 (2008)
Y. Yamamoto, Y. Nishiyama, T. Monden, Y. Matsumura, K. Satoh, M. Ohkawa, Clinical usefulness of fusion of 131I SPECT and CT images in patients with differentiated thyroid carcinoma. J. Nucl. Med. 44, 1905–1910 (2003)
SB Edge, DR Byrd, CC Compton, AG Fritz, FL Greene, A Trotti, (eds.) AJCC Cancer Staging Manual. 7th edn. (New York, NY, Springer, 2010)
National Cancer Institute. Thyroid cancer, http://www.cancer.gov/cancertopics/types/thyroid (2014). Accessed 27 Nov 2015
R.H. Nishiyama, Overview of surgical pathology of the thyroid gland. World J. Surg. 24, 898–906 (2000)
M. Bongiovanni, G. Paone, L. Ceriani, M. Pusztaszer, Cellular and molecular basis for thyroid cancer imaging in nuclear medicine. Clin. Transl. Imaging 1, 149–161 (2013)
B.R. Haugen, E.C. Lin, Isotope imaging for metastatic thyroid cancer. Endocrinol. Metab. Clin. North Am. 30(2), 469–492 (2001)
D.I. Glazer, R.K. Brown, K.K. Wong, H. Savas, M.D. Gross, A.M. Avram, SPECT/CT evaluation of unusual physiologic radioiodine biodistributions: pearls and pitfalls in imaging interpretation. Radiographics 33, 397–418 (2013)
K.K. Wong, D.J. Wale, L.M. Fig, M.D. Gross, SPET–CT in thyroid cancer: a systematic review. Clin. Transl. Imaging 2, 459–475 (2014)
S. Kohlfuerst, I. Igerc, M. Lobnig, H.J. Gallowitsch, I. Gomez-Segovia, S. Matschnig, Z. Mayr, P. Mikosch, M. Beheshti, P. Lind, Posttherapeutic 131I SPECT-CT offers high diagnostic accuracy when the findings on conventional planar imaging are inconclusive and allows a tailored patient treatment regimen. Eur. J. Nucl. Med. Mol. Imaging 36, 886–893 (2009)
D. Schmidt, A. Szikszai, R. Linke, W. Bautz, T. Kuwert, Impact of 131I SPECT/spiral CT on nodal staging of differentiated thyroid carcinoma at the first radioablation. J. Nucl. Med. 50, 18–23 (2009)
N. Aide, N. Heutte, J.P. Rame, E. Rousseau, C. Loiseau, M.H. Amar, S. Bardet, Clinical relevance of single-photon emission computed tomography/computed tomography of the neck and thorax in postablation 131I scintigraphy for thyroid cancer. J. Clin. Endocrinol. Metab. 94, 2075–2084 (2009)
A. Spanu, M.E. Solinas, F. Chessa, D. Sanna, S. Nuvoli, G. Madeddu, 131I SPECT/CT in the follow-up of differentiated thyroid carcinoma: incremental value versus planar imaging. J. Nucl. Med. 50, 184–190 (2009)
H. Wakabayashi, K. Nakajima, M. Fukuoka, A. Inaki, A. Nakamura, D. Kayano, S. Kinuya, Double-phase 131I whole body scan and 131I SPECT-CT images in patients with differentiated thyroid cancer: their effectiveness for accurate identification. Ann. Nucl. Med. 25, 609–615 (2011)
Y.L. Xue, Z.L. Qiu, H.J. Song, Q.Y. Luo, Value of 131I SPECT/CT for the evaluation of differentiated thyroid cancer: a systematic review of the literature. Eur. J. Nucl. Med. Mol. Imaging 40, 768–778 (2013)
Y. Maruoka, K. Abe, S. Baba, T. Isoda et al., Incremental diagnostic value of SPECT/CT with 131I scintigraphy after radioiodine therapy in patients with well-differentiated thyroid carcinoma. Radiology 265, 902–909 (2012)
T. Barwick, I. Murray, H. Megadmi, W.M. Drake, P.N. Plowman, S.A. Akker et al., Single photon emission computed tomography (SPECT)/computed tomography using iodine-123 in patients with differentiated thyroid cancer: additional value over whole body planar imaging and SPECT. Eur. J. Endocrinol. 162, 1131–1139 (2010)
A.M. Avram, Radioiodine scintigraphy with SPECT/CT: an important diagnostic tool for thyroid cancer staging and risk stratification. J. Nucl. Med. 53, 754–764 (2012)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zilioli, V., Peli, A., Panarotto, M.B. et al. Differentiated thyroid carcinoma: Incremental diagnostic value of 131I SPECT/CT over planar whole body scan after radioiodine therapy. Endocrine 56, 551–559 (2017). https://doi.org/10.1007/s12020-016-1086-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-016-1086-3