Abstract
Background/Objectives
Sickle cell disease (SCD) complications mostly result from vascular dysfunction, concerning systemic microvasculature and cerebral large vessels. The aim of this cohort study was to identify potential circulating biomarkers predictive for further vascular event occurrence in pediatric SCD.
Methods
We consecutively enrolled 108 children with SCD at steady state, aged 3–18 years old (median 9.8 years). Hematology, coagulation, hemolysis, endothelial, platelet and vascular activation parameters were recorded at inclusion. Neurovascular and systemic vascular events were prospectively recorded during a mean follow-up period of 27 months.
Results
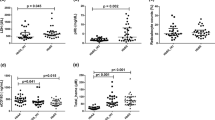
Patients at steady state displayed significantly higher hemolysis and platelet activation markers, higher leukocyte, CD34+ hematopoietic stem cell and microvesicle counts, and a pro-coagulant profile compared to controls matched for age and ethnicity. Circulating endothelial cell or nucleosome level did not differ. During the follow-up period, 36 patients had at least one neurovascular (n = 12) or systemic vascular event (n = 25). In a multivariate model, high CD34+ cell count was the best predictor for the occurrence of a vascular event (OR 1.2 for 1000 cell/mL increase, 95% CI [1.049–1.4], p = 0.013, sensitivity 53%, specificity 84% for a threshold of 8675 cells/mL).
Conclusion
CD34+ cell count at steady state is a promising biomarker of further vascular event in children with SCD.


Similar content being viewed by others
References
Adams, R., McKie, V., Nichols, F., Carl, E., Zhang, D. L., McKie, K., Figueroa, R., Litaker, M., Thompson, W., & Hess, D. (1992). The use of transcranial ultrasonography to predict stroke in sickle cell disease. The New England Journal of Medicine, 326(9), 605–610.
Wang, W. C., Gallagher, D. M., Pegelow, C. H., Wright, E. C., Vichinsky, E. P., Abboud, M. R., Moser, F. G., & Adams, R. J. (2000). Multicenter comparison of magnetic resonance imaging and transcranial Doppler ultrasonography in the evaluation of the central nervous system in children with sickle cell disease. Journal of Pediatric Hematology/Oncology, 22(4), 335–339.
Miller, S. T., Sleeper, L. A., Pegelow, C. H., Enos, L. E., Wang, W. C., Weiner, S. J., Wethers, D. L., Smith, J., & Kinney, T. R. (2000). Prediction of adverse outcomes in children with sickle cell disease. The New England Journal of Medicine, 342(2), 83–89.
Stevens, M. C., Hayes, R. J., Vaidya, S., & Serjeant, G. R. (1981). Fetal hemoglobin and clinical severity of homozygous sickle cell disease in early childhood. The Journal of Pediatrics, 98(1), 37–41.
Lebensburger, J., Johnson, S. M., Askenazi, D. J., Rozario, N. L., Howard, T. H., & Hilliard, L. M. (2011). Protective role of hemoglobin and fetal hemoglobin in early kidney disease for children with sickle cell anemia. American Journal of Hematology, 86(5), 430–432.
Silva, C. M., Giovani, P., & Viana, M. B. (2011). High reticulocyte count is an independent risk factor for cerebrovascular disease in children with sickle cell anemia. Pediatric Blood & Cancer, 56(1), 116–121.
Meier, E. R., Wright, E. C., & Miller, J. L. (2014). Reticulocytosis and anemia are associated with an increased risk of death and stroke in the newborn cohort of the cooperative study of sickle cell disease. American Journal of Hematology, 89(9), 904–906.
DeBaun, M. R., Sarnaik, S. A., Rodeghier, M. J., Minniti, C. P., Howard, T. H., Iyer, R. V., Inusa, B., Telfer, P. T., Kirby-Allen, M., Quinn, C. T., Bernaudin, F., Airewele, G., Woods, G. M., Panepinto, J. A., Fuh, B., Kwiatkowski, J. K., King, A. A., Rhodes, M. M., Thompson, A. A., Heiny, M. E., Redding-Lallinger, R. C., Kirkham, F. J., Sabio, H., Gonzalez, C. E., Saccente, S. L., Kalinyak, K. A., Strouse, J. J., Fixler, J. M., Gordon, M. O., Miller, J. P., Noetzel, M. J., Ichord, R. N., & Casella, J. F. (2012). Associated risk factors for silent cerebral infarcts in sickle cell anemia: Low baseline hemoglobin, sex, and relative high systolic blood pressure. Blood, 119(16), 3684–3690.
Switzer, J. A., Hess, D. C., Nichols, F. T., & Adams, R. J. (2006). Pathophysiology and treatment of stroke in sickle-cell disease: Present and future. The Lancet. Neurology, 5(6), 501–512.
Platt, O. S. (2005). Preventing stroke in sickle cell anemia. The New England Journal of Medicine, 353(26), 2743–2745.
de Montalembert, M., Aggoun, Y., Niakate, A., Szezepanski, I., & Bonnet, D. (2007). Endothelial-dependent vasodilation is impaired in children with sickle cell disease. Haematologica, 92(12), 1709–1710.
Ataga, K. I., Moore, C. G., Jones, S., Olajide, O., Strayhorn, D., Hinderliter, A., & Orringer, E. P. (2006). Pulmonary hypertension in patients with sickle cell disease: A longitudinal study. British Journal of Haematology, 134(1), 109–115.
National Institutes of Health. (2002). The Management of Sickle Cell Disease. http://www.nhlbi.nih.gov/files/docs/guidelines/sc_mngt.pdf
NHS. (2010). Sickle cell disease in childhood, standards and guidelines for clinical care. http://sct.screening.nhs.uk/getdata.php?id=11164
Tounian, P., Aggoun, Y., Dubern, B., Varille, V., Guy-Grand, B., Sidi, D., Girardet, J. P., & Bonnet, D. (2001). Presence of increased stiffness of the common carotid artery and endothelial dysfunction in severely obese children: A prospective study. Lancet, 358(9291), 1400–1404.
Woywodt, A., Kirsch, T., & Haubitz, M. (2006). Immunomagnetic isolation and FACS--competing techniques for the enumeration of circulating endothelial cells. Thrombosis and Haemostasis, 96, 1), 1–1), 2.
Smadja, D. M., Gaussem, P., Mauge, L., Israël-Biet, D., Dignat-George, F., Peyrard, S., et al. (2009). Circulating endothelial cells: A new candidate biomarker of irreversible pulmonary hypertension secondary to congenital heart disease. Circulation, 119(3), 374–381.
Sutherland, D. R., Anderson, L., Keeney, M., Nayar, R., & Chin-Yee, I. (1996). The ISHAGE guidelines for CD34+ cell determination by flow cytometry. International Society of Hematotherapy and Graft Engineering. Journal of Hematotherapy, 5(3), 213–226.
Mauge, L., Sabatier, F., Boutouyrie, P., D’Audigier, C., Peyrard, S., Bozec, E., et al. (2014). Forearm ischemia decreases endothelial colony-forming cell angiogenic potential. Cytotherapy, 16(2), 213–224.
Le Manach, Y., Kahn, D., Bachelot-Loza, C., Le Sache, F., Smadja, D. M., Remones, V., et al. (2014). Impact of aspirin and clopidogrel interruption on platelet function in patients undergoing major vascular surgery. PLoS One, 9(8), e104491.
Robert, S., Lacroix, R., Poncelet, P., Harhouri, K., Bouriche, T., Judicone, C., Wischhusen, J., Arnaud, L., & Dignat-George, F. (2012). High-sensitivity flow cytometry provides access to standardized measurement of small-size microparticles--brief report. Arteriosclerosis, Thrombosis, and Vascular Biology, 32(4), 1054–1058.
Fuchs, T. A., Kremer Hovinga, J. A., Schatzberg, D., Wagner, D. D., & Lämmle, B. (2012). Circulating DNA and myeloperoxidase indicate disease activity in patients with thrombotic microangiopathies. Blood, 120(6), 1157–1164.
Torsten Hothorn, Hornik, K., Van de Wiel, M. A., & Zeileis, A. (2008). Implementation of a class of permutation tests: the coin package., 28(8), 1–23.
Ofori-Acquah, S. F., Buchanan, I. D., Osunkwo, I., Manlove-Simmons, J., Lawal, F., Quarshie, A., et al. (2012). Elevated circulating angiogenic progenitors and white blood cells are associated with hypoxia-inducible angiogenic growth factors in children with sickle cell disease. Anemia, 2012, 156598.
Patel, S. D., Humphries, J., Mattock, K., Wadoodi, A., Modarai, B., Ahmad, A., Burnand, K. G., Waltham, M., & Smith, A. (2012). Hematopoietic progenitor cells and restenosis after carotid endarterectomy. Stroke; a Journal of Cerebral Circulation, 43(6), 1663–1665.
Wierenga, A. T. J., Vellenga, E., & Schuringa, J. J. (2014). Convergence of hypoxia and TGFβ pathways on cell cycle regulation in human hematopoietic stem/progenitor cells. PLoS One, 9(3), e93494.
Lee, P. S. S., & Poh, K. K. (2014). Endothelial progenitor cells in cardiovascular diseases. World Journal of Stem Cells, 6(3), 355–366.
Ratajczak, M. Z., Ratajczak, J., Suszynska, M., Miller, D. M., Kucia, M., & Shin, D.-M. (2017). A novel view of the adult stem cell compartment from the perspective of a quiescent population of very small embryonic-like stem cells. Circulation Research, 120(1), 166–178.
Smadja, D. M. (2017). Bone marrow very small embryonic-like stem cells: New generation of autologous cell therapy soon ready for prime time? Stem Cell Reviews, 13(2), 198–201.
Guerin, C. L., Loyer, X., Vilar, J., Cras, A., Mirault, T., Gaussem, P., Silvestre, J. S., & Smadja, D. M. (2015). Bone-marrow-derived very small embryonic-like stem cells in patients with critical leg ischaemia: Evidence of vasculogenic potential. Thrombosis and Haemostasis, 113(5), 1084–1094.
Guerin, C. L., Rossi, E., Saubamea, B., Cras, A., Mignon, V., Silvestre, J.-S., & Smadja, D. M. (2017). Human very small embryonic-like cells support vascular maturation and therapeutic revascularization induced by endothelial progenitor cells. Stem Cell Reviews, 13(4), 552–560.
Zhang, S., Zhao, L., Wang, J., Chen, N., Yan, J., & Pan, X. (2017). HIF-2α and Oct4 have synergistic effects on survival and myocardial repair of very small embryonic-like mesenchymal stem cells in infarcted hearts. Cell Death & Disease, 8(1), e2548.
Croizat, H., Ponchio, L., Nicolini, F. E., Nagel, R. L., & Eaves, C. J. (2000). Primitive haematopoietic progenitors in the blood of patients with sickle cell disease appear to be endogenously mobilized. British Journal of Haematology, 111(2), 491–497.
Chang, K. H., Nayak, R. C., Roy, S., Perumbeti, A., Wellendorf, A. M., Bezold, K. Y., Pirman M., Hill S. E., Starnes J., Loberg A., Zhou X., Inagami T., Zheng Y., Malik P., Cancelas J. A. (2015). Vasculopathy-associated hyperangiotensinemia mobilizes haematopoietic stem cells/progenitors through endothelial AT2R and cytoskeletal dysregulation. Nature Communications, 6, 5914.
Adams, R. J., Brambilla, D. J., Granger, S., Gallagher, D., Vichinsky, E., Abboud, M. R., Pegelow C.H., Woods G., Rohde E.M., Nichols F.T., Jones A., Luden J.P., Bowman L., Hagner S., Morales K.H., Roach E.S., STOP Study. (2004). Stroke and conversion to high risk in children screened with transcranial Doppler ultrasound during the STOP study. Blood, 103(10), 3689–3694.
Solovey, A., Lin, Y., Browne, P., Choong, S., Wayner, E., & Hebbel, R. P. (1997). Circulating activated endothelial cells in sickle cell anemia. The New England Journal of Medicine, 337(22), 1584–1590.
Smadja, D. M., Mauge, L., Sanchez, O., Silvestre, J.-S., Guerin, C., Godier, A., Henno, P., Gaussem, P., & Israel-Biet, D. (2010). Distinct patterns of circulating endothelial cells in pulmonary hypertension. The European Respiratory Journal, 36(6), 1284–1293.
Levy, M., Bonnet, D., Mauge, L., Celermajer, D. S., Gaussem, P., & Smadja, D. M. (2013). Circulating endothelial cells in refractory pulmonary hypertension in children: Markers of treatment efficacy and clinical worsening. PLoS One, 8(6), e65114.
Manzoni, M., Comolli, G., Torchio, M., Mazzini, G., & Danova, M. (2015). Circulating endothelial cells and their subpopulations: Role as predictive biomarkers in antiangiogenic therapy for colorectal cancer. Clinical Colorectal Cancer, 14(1), 11–17.
Liu, Y., Yuan, D., Ye, W., Lv, T., & Song, Y. (2015). Prognostic value of circulating endothelial cells in non-small cell lung cancer patients: A systematic review and meta-analysis. Translational Lung Cancer Research, 4(5), 610–618.
Zhou, F., Zhou, Y., Dong, J., & Tan, W. (2017). Circulating endothelial cells and their subsets: Novel biomarkers for cancer. Biomarkers in Medicine.
Noubouossie, D. C. F., Lê, P. Q., Rozen, L., Ziereisen, F., Willems, D., Demulder, A., & Ferster, A. (2013). Thrombin generation in children with sickle cell disease: Relationship with age, hemolysis, transcranial Doppler velocity, and hydroxyurea treatment. European Journal of Haematology, 91(1), 46–54.
Bartolucci, P., & Galactéros, F. (2012). Clinical management of adult sickle-cell disease. Current Opinion in Hematology, 19(3), 149–155.
Acknowledgements
The authors would like to thank Florence Desvard, Yann Brunel, Laurent Garcia, Aurélie Dumont, and Peggy Tournoux for their excellent technical assistance. The French Institute for Medical Research INSERM funded Dr. M. Kossorotoff for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest Statement
The authors disclose any conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 95 kb)
Rights and permissions
About this article
Cite this article
Kossorotoff, M., De Montalembert, M., Brousse, V. et al. CD34+ Hematopoietic Stem Cell Count Is Predictive of Vascular Event Occurrence in Children with Sickle Cell Disease. Stem Cell Rev and Rep 14, 694–701 (2018). https://doi.org/10.1007/s12015-018-9835-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-018-9835-8