Abstract
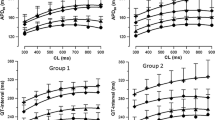
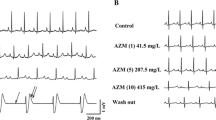
Recent results from data mining analyses and reports of adverse drug events suggest a QT-prolonging drug–drug interaction resulting from the combination of distinct proton pump inhibitors and cephalosporins. Therefore, this study aimed at investigating the effect of the suspected QT-prolonging combinations of lansoprazole + ceftriaxone and esomeprazole + cefazolin, respectively. 26 hearts of New Zealand White rabbits were retrogradely perfused and paced at different cycle lengths. After generating baseline data, the hearts were assigned to two groups: In group 1, hearts were treated with 5 µM lansoprazole. Thereafter, 200 µM ceftriaxone was infused additionally. Group 2 was perfused with 10 µM esomeprazole followed by 250 µM cefazolin. In group 1, lansoprazole did not significantly alter QT intervals and APD90. Additional treatment with ceftriaxone significantly shortened QT interval, APD90 and slightly reduced dispersion of repolarization compared to sole lansoprazole infusion. In group 2, esomeprazole led to a significant shortening of the QT interval without altering APD90 or dispersion. Additional treatment with the antibiotic cefazolin further shortened QT interval, APD90 and reduced the dispersion of repolarization. Incidence of ventricular arrhythmias was not significantly altered in both groups. This is the first experimental whole-heart study that investigated the impact of a concomitant treatment with proton pump inhibitors and cephalosporins. In contrast to previous reports, the combination of both agents did not cause QT prolongation but instead shortened QT interval and action potential duration. As a consequence, no triggered activity occurred in the presence of a stable dispersion of repolarization.




Similar content being viewed by others
Abbreviations
- APD:
-
Action potential duration
- APD90 :
-
Action potential duration at 90%-repolarization
- CFN:
-
Cefazolin
- CFX:
-
Ceftriaxone
- CL:
-
Cycle length
- DDI:
-
Drug–drug interaction
- ECG:
-
Electrocardiogram
- ERP:
-
Effective refractory period
- ESO:
-
Esomeprazole
- LNS:
-
Lansoprazole
- MAP:
-
Monophasic action potential
- PPI:
-
Proton pump inhibitors
- PRR:
-
Post-repolarization refractoriness
- SQTS:
-
Short QT syndrome
- VT:
-
Ventricular tachycardia
References
Frommeyer, G., & Eckardt, L. (2016). Drug-induced proarrhythmia: Risk factors and electrophysiological mechanisms. Nature Reviews Cardiology, 13(1), 36–47.
Lorberbaum, T., Sampson, K. J., Chang, J. B., Iyer, V., Woosley, R. L., Kass, R. S., et al. (2016). Coupling data mining and laboratory experiments to discover drug interactions causing QT prolongation. Journal of the American College of Cardiology, 68(16), 1756–1764.
Shin, J. M., & Kim, N. (2013). Pharmacokinetics and pharmacodynamics of the proton pump inhibitors. Journal of Neurogastroenterology and Motility, 19(1), 25–35.
Strand, D. S., Kim, D., & Peura, D. A. (2017). 25 years of proton pump inhibitors: A comprehensive review. Gut and Liver, 11(1), 27–37.
Patterson Burdsall, D., Flores, H. C., Krueger, J., Garretson, S., Gorbien, M. J., Iacch, A., et al. (2013). Use of proton pump inhibitors with lack of diagnostic indications in 22 Midwestern US skilled nursing facilities. Journal of American Medical Directors Association, 14(6), 429–432.
Scholler, J., Nivoix, Y., Herbrecht, R., Kemmel, V., & Leveque, D. (2011). Ventricular bigeminy associated with voriconazole, methadone and esomeprazole. International Journal of Clinical Pharmacy, 33(6), 905–908.
Poluzzi, E., Raschi, E., Motola, D., Moretti, U., & De Ponti, F. (2010). Antimicrobials and the risk of torsades de pointes: The contribution from data mining of the US FDA Adverse Event Reporting System. Drug Safety, 33(4), 303–314.
Tsubokura, M., Miura, Y., Itokawa, T., Murata, K., Takei, N., Higaki, T., et al. (2011). Fatal dysrhythmia following initiation of lansoprazole during a long-term course of voriconazole. Journal of Clinical Pharmacology, 51(10), 1488–1490.
Lazzerini, P. E., Bertolozzi, I., Rossi, M., Capecchi, P. L., & Laghi-Pasini, F. (2017). Combination therapy with ceftriaxone and lansoprazole, acquired long QT syndrome, and Torsades de Pointes risk. Journal of the American College of Cardiology, 69(14), 1876–1877.
Frommeyer, G., Ellermann, C., Dechering, D. G., Kochhauser, S., Bogeholz, N., Guner, F., et al. (2016). Ranolazine and vernakalant prevent ventricular arrhythmias in an experimental whole-heart model of short QT syndrome. Journal of Cardiovascular Electrophysiology, 27(10), 1214–1219.
Ellermann, C., Sterneberg, M., Kochhauser, S., Dechering, D. G., Fehr, M., Eckardt, L., et al. (2018). Antiarrhythmic effect of antazoline in experimental models of acquired short- and long-QT-syndromes. Europace., 20(10), 1699–1706.
Frommeyer, G., Clauss, C., Ellermann, C., Bogossian, H., Dechering, D. G., Kochhauser, S., et al. (2017). Antiarrhythmic effect of vernakalant in an experimental model of Long-QT-syndrome. Europace., 19(5), 866–873.
Frommeyer, G., Garthmann, J., Ellermann, C., Dechering, D. G., Kochhauser, S., Reinke, F., et al. (2018). Broad antiarrhythmic effect of mexiletine in different arrhythmia models. Europace., 20(8), 1375–1381.
Schleibinger, M., Steinbach, C. L., Topper, C., Kratzer, A., Liebchen, U., Kees, F., et al. (2015). Protein binding characteristics and pharmacokinetics of ceftriaxone in intensive care unit patients. British Journal of Clinical Pharmacology, 80(3), 525–533.
Krupa, L. Z., & Fellows, I. W. (2019). Lansoprazole-induced hypomagnesaemia. BMJ Case Report. https://doi.org/10.1136/bcr-2012-006342.
Seslar, S. P., Berul, C. I., Burklow, T. R., Cecchin, F., & Alexander, M. E. (2006). Transient prolonged corrected QT interval in Lyme disease. Journal of Pediatrics, 148(5), 692–697.
Clauss, S., Bleyer, C., Schuttler, D., Tomsits, P., Renner, S., Klymiuk, N., et al. (2019). Animal models of arrhythmia: Classic electrophysiology to genetically modified large animals. Nature Reviews Cardiology, 16(8), 457–475.
Onda, K., Tong, S., Beard, S., Binder, N., Muto, M., Senadheera, S. N., et al. (2017). Proton pump inhibitors decrease soluble FMS-like tyrosine kinase-1 and soluble endoglin secretion, decrease hypertension, and rescue endothelial dysfunction. Hypertension, 69(3), 457–468.
Valentin, J. P., Hoffmann, P., De Clerck, F., Hammond, T. G., & Hondeghem, L. (2004). Review of the predictive value of the Langendorff heart model (Screenit system) in assessing the proarrhythmic potential of drugs. Journal of Pharmacological and Toxicological Methods, 49(3), 171–181.
Acknowledgements
This study was supported by the Hans-and-Gertie Fischer Foundation (to G.F.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no relationships that could be construed as a conflict of interest.
Ethical Approval & Statement
All applicable international, national and institutional guidelines for the care and use of animals were followed. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution at which the studies were conducted.
Additional information
Handling Editor: Dr. Dakshesh Patel.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wolfes, J., Ellermann, C., Burde, S. et al. Concomitant Treatment with Proton Pump Inhibitors and Cephalosporins Does Not Enhance QT-Associated Proarrhythmia in Isolated Rabbit Hearts. Cardiovasc Toxicol 20, 531–538 (2020). https://doi.org/10.1007/s12012-020-09577-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-020-09577-3