Abstract
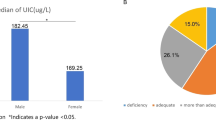
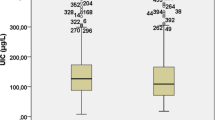
Great changes have taken place in the incidence of thyroid diseases since the implementation of universal salt iodization (USI). However, the high incidence of thyroid diseases caused by the high iodine intake has been contentious. The aim of this study was to investigate the relationship between iodine intake and thyroid diseases through the comparison of urine iodine concentration (UIC) between patients with thyroid diseases and healthy volunteers and to assess the status of iodine intake among the residents. From November 2013 to May 2014, 905 patients who underwent thyroid surgeries and 272 subjects of healthy controls were enrolled and were divided into two groups: the case group and the control group, respectively. Levels of thyroid hormones and thyroid autoantibodies in serum from blood were analyzed among all the patients. UIC and thyroid B ultrasounds were performed on each participant. The median urinary iodine (MUI) concentration was 184.5 and 169.6 μg/L for case group and control group, respectively (P = 0.003). Significant differences of the MUI were found between healthy controls and patients with Hashimoto’s thyroiditis (MUI = 221.3 μg/L), nodular goiter (MUI = 193.5 μg/L), multiple nodules (MUI = 185.9 μg/L), nodule diameter ≥1 cm (MUI = 194.4 μg/L), hyperthyroidism (MUI = 258.7 μg/L), thyroid peroxidase antibody (TPOAb) (+), and thyroglobulin antibody (TGAb) (+) (MUI = 196.4 μg/L), and P values were 0.003, 0.000, 0.002, 0.000, 0.000, and 0.001, respectively. The susceptibility of the thyroid diseases among normal people was significantly associated with female sex (odds ratio (OR) = 3.3), older age (OR = 2.1), and high iodine intake (OR = 1.3). In conclusion, high iodine intake was likely to lead to the occurrence of thyroid diseases, such as Hashimoto thyroiditis, nodular goiter, and hyperthyroidism, through a long-term mechanism. USI should continue to be carried out and individual UIC detection was recommended for the disequilibrium of the iodine nutritional status among normal people.
Similar content being viewed by others
References
WHO/UNICEF/ICCIDD (2001) Assessment of the iodine deficiency disorders and monitoring their elimination. WHO, Geneva
Konig F, Andersson M, Hotz K, Aeberli I, Zimmermann MB (2011) Ten repeat collections for urinary iodine from spot samples or 24-h samples are needed to reliably estimate individual iodine status in women. J Nutr 141:2049–2054
Zhang JY, Li SM, Leng JL, Chen YJ, Pu J, Li JM, Pang FX, Huang YH, Nong J, Cen YZ, He H, Li R, Wei LN, He HY (2013) Changes of the spectrum on thyroid disease after the ten-year implementation of universal salt iodization in Guangxi Zhuang Autonomous Region. Zhonghua Liu Xing Bing Xue Za Zhi 34:970–974
Liu YQ, Zhang SQ, Chen WQ, Chen LL, Zhang SW, Zhang XD, Zheng RS (2012) Trend of incidence and mortality on thyroid cancer in China during 2003–2007. Zhonghua Liu Xing Bing Xue Za Zhi 33:1044–1048
Camargo R, Knobel M, Medeiros-Neto G (2007) Iodine nutrition: more is better? Arq Bras Endocrinol Metabol 51:639–640
Pino S, Fang SL, Braverman LE (1998) Ammonium persulfate: a new and safe method for measuring urinary iodine by ammonium persulfate oxidation. Exp Clin Endocrinol Diabetes 106(Suppl 3):S22–27
Teng W, Shan Z, Teng X, Guan H, Li Y, Teng D, Jin Y, Yu X, Fan C, Chong W, Yang F, Dai H, Yu Y, Li J, Chen Y, Zhao D, Shi X, Hu F, Mao J, Gu X, Yang R, Tong Y, Wang W, Gao T, Li C (2006) Effect of iodine intake on thyroid diseases in China. N Engl J Med 354:2783–2793
Teng X, Shan Z, Chen Y, Lai Y, Yu J, Shan L, Bai X, Li Y, Li N, Li Z, Wang S, Xing Q, Xue H, Zhu L, Hou X, Fan C, Teng W (2011) More than adequate iodine intake may increase subclinical hypothyroidism and autoimmune thyroiditis: a cross-sectional study based on two Chinese communities with different iodine intake levels. Eur J Endocrinol 164:943–950
Hashemipour M, Amini M, Aminorroaya A, Dastjerdi MI, Rezvanian H, Kachoei A, Moaddab MH, Mohammadi M, Kelishadi R, Amini Z, Haghighi S, Shojaee-Moradie F (2007) High prevalence of goiter in an iodine replete area: do thyroid auto-antibodies play a role? Asia Pac J Clin Nutr 16:403–410
Dogan M, Acikgoz E, Acikgoz M, Cesur Y, Ariyuca S, Bektas MS (2011) The frequency of Hashimoto thyroiditis in children and the relationship between urinary iodine level and Hashimoto thyroiditis. J Pediatr Endocrinol Metab 24:75–80
Latrofa F, Fiore E, Rago T, Antonangeli L, Montanelli L, Ricci D, Provenzale MA, Scutari M, Frigeri M, Tonacchera M, Vitti P (2013) Iodine contributes to thyroid autoimmunity in humans by unmasking a cryptic epitope on thyroglobulin. J Clin Endocrinol Metab 98:E1768–1774
Burek CL, Rose NR (2008) Autoimmune thyroiditis and ROS. Autoimmun Rev 7:530–537
Kim JY, Kim KR (2000) Dietary iodine intake and urinary iodine excretion in patients with thyroid diseases. Yonsei Med J 41:22–28
Poljak NK, Kontic M, Colovic Z, Jeroncic I, Luksic B, Mulic R (2011) Iodine intake and epidemiological characteristics of thyroid cancer: comparison between inland and littoral Croatia. Acta Clin Croat 50:329–339
Clero E, Doyon F, Chungue V, Rachedi F, Boissin JL, Sebbag J, Shan L, Bost-Bezeaud F, Petitdidier P, Dewailly E, Rubino C, de Vathaire F (2012) Dietary iodine and thyroid cancer risk in French Polynesia: a case-control study. Thyroid 22:422–429
Sehestedt T, Knudsen N, Perrild H, Johansen C (2006) Iodine intake and incidence of thyroid cancer in Denmark. Clin Endocrinol (Oxf) 65:229–233
Zhu W, Liu X, Hu X, Zhou S, Wang Y, Zhang Y (2012) Investigation on the iodine nutritional status and the prevalence of thyroid carcinoma in Zhoushan Archipelago residents. Wei Sheng Yan Jiu 41:79–82
Siegel R, Naishadham D, Jemal A (2012) Cancer statistics, 2012. CA Cancer J Clin 62:10–29
Pellegriti G, Frasca F, Regalbuto C, Squatrito S, Vigneri R (2013) Worldwide increasing incidence of thyroid cancer: update on epidemiology and risk factors. J Cancer Epidemiol 2013:965212
Davies L, Welch HG (2014) Current thyroid cancer trends in the United States. JAMA Otolaryngol Head Neck Surg 140:317–322
Knobel M, Medeiros-Neto G (2007) Relevance of iodine intake as a reputed predisposing factor for thyroid cancer. Arq Bras Endocrinol Metabol 51:701–712
Gharib H, Papini E, Paschke R, Duick DS, Valcavi R, Hegedus L, Vitti P, Nodules AAETFoT (2010) American Association of Clinical Endocrinologists, Associazione Medici Endocrinologi, and European Thyroid Association Medical guidelines for clinical practice for the diagnosis and management of thyroid nodules. Endocr Pract 16(Suppl 1):1–43
American Thyroid Association Guidelines Taskforce on Thyroid N, Differentiated Thyroid C, DS C, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, Mazzaferri EL, McIver B, Pacini F, Schlumberger M, Sherman SI, Steward DL, Tuttle RM (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Laurberg P, Cerqueira C, Ovesen L, Rasmussen LB, Perrild H, Andersen S, Pedersen IB, Carle A (2010) Iodine intake as a determinant of thyroid disorders in populations. Best Pract Res Clin Endocrinol Metab 24:13–27
Suzuki H, Higuchi T, Sawa K, Ohtaki S, Horiuchi Y (1965) “Endemic coast goiter” in Hokkaido, Japan. Acta Endocrinol (Copenh) 50:161–176
Thomopoulos P (2002) Hyperthyroidism due to excess iodine. Presse Med 31:1664–1669
Mo Z, Lou XM, Zhu WM, Wang XF, Mao GM, Zhou JS, Ding GQ (2013) A cross-sectional study on iodine nutrition in general population from Zhejiang province, China. Zhonghua Liu Xing Bing Xue Za Zhi 34:464–470
Soriguer F, Garcia-Fuentes E, Gutierrez-Repiso C, Rojo-Martinez G, Velasco I, Goday A, Bosch-Comas A, Bordiu E, Calle A, Carmena R, Casamitjana R, Castano L, Castell C, Catala M, Delgado E, Franch J, Gaztambide S, Girbes J, Gomis R, Gutierrez G, Lopez-Alba A, Martinez-Larrad MT, Menendez E, Mora-Peces I, Ortega E, Pascual-Manich G, Serrano-Rios M, Valdes S, Vazquez JA, Vendrell J (2012) Iodine intake in the adult population. Di@bet.es study. Clin Nutr 31:882–888
Amouzegar A, Khazan M, Hedayati M, Azizi F (2014) An assessment of the iodine status and the correlation between iodine nutrition and thyroid function during pregnancy in an iodine sufficient area. Eur J Clin Nutr 68:397–400
Liu P, Liu L, Shen H, Jia Q, Wang J, Zheng H, Ma J, Zhou D, Liu S, Su X (2014) The standard, intervention measures and health risk for high water iodine areas. PLoS One 9:e89608
Xu J, Dong HJ, Lu BL, Li SM, Zheng QS, Zhuang GX (2008) Surveillance on iodized salt in China, in 2006. Zhonghua Liu Xing Bing Xue Za Zhi 29:253–257
Acknowledgments
The authors thank all of the participants in the study and wish to convey our appreciation to all staff involved.
Conflict of interest
No potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, H., Tian, Y., Liu, Z. et al. Correlation Between Iodine Intake and Thyroid Disorders: A Cross-Sectional Study from the South of China. Biol Trace Elem Res 162, 87–94 (2014). https://doi.org/10.1007/s12011-014-0102-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-014-0102-9