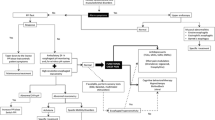
Opinion statement
Functional heartburn and functional chest pain of presumed esophageal origin are characterized by symptoms suggesting an esophageal origin, but negative work-up on routine investigations, including ruling out gastroesophageal reflux disease. Visceral hypersensitivity is a potentially unifying pathophysiological concept, thought to underlie these disorders. In addition, there is important overlap with other functional disorders and psychiatric co-morbidity. This review summarizes current concepts on definition, diagnosis, and treatment options for functional heartburn and functional chest pain of presumed esophageal origin. Antidepressants are frequently used in these conditions, where they are presumed to act as neuromodulators of visceral hypersensitivity. There is a need for high-quality trials evaluating the efficacy of antidepressants and more specific neuromodulators, such as pregabalin, in functional esophageal disorders.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance
Vakil N, van Zanten SV, Kahrilas P, Dent J, Jones R, Global Consensus Group. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900–20.
Poelmans J, Feenstra L, Demedts I, Rutgeerts P, Tack J. The yield of upper gastrointestinal endoscopy in patients with suspected reflux-related chronic ear, nose, and throat symptoms. Am J Gastroenterol. 2004;99(8):1419–26.
Sigterman KE, van Pinxteren B, Bonis PA, Lau J, Numans ME. Short-term treatment with proton pump inhibitors, H2-receptor antagonists and prokinetics for gastro-oesophageal reflux disease-like symptoms and endoscopy negative reflux disease. Cochrane Database Syst Rev. 2013;5:CD002095. doi:10.1002/14651858.CD002095.pub5.
Scarpellini E, Ang D, Pauwels A, De Santis A, Vanuytsel T, Tack J. Management of refractory typical gastro-esophageal reflux disease symptoms, Nature Reviews Gastroenterol Hepatol, 2015, in press.
Ang D, Sifrim D, Tack J. Mechanisms of heartburn. Nat Clin Pract Gastroenterol Hepatol. 2008;5(7):383–92.
Mainie I, Tutuian R, Shay S, Vela M, Zhang X, Sifrim D, et al. Acid and non-acid reflux in patients with persistent symptoms despite acid suppressive therapy: a multicentre study using combined ambulatory impedance-pH monitoring. Gut. 2006;55(10):1398–402.
Herregods TV, Troelstra M, Weijenborg PW, Bredenoord AJ, Smout AJ. Patients with refractory reflux symptoms often do not have GERD. Neurogastroenterol Motil. 2015;27:1267–73. Recent study showing that 30% of patients with PPI refractory reflux symptoms suffer from functional heartburn, based on pH-impedance measurements.
Galmiche JP, Clouse RE, Bálint A, Cook IJ, Kahrilas PJ, Paterson WG, et al. Functional esophageal disorders. Gastroenterology. 2006;130(5):1459–65.
Fass R, Tougas G. Functional heartburn: the stimulus, the pain, and the brain. Gut. 2002;51:885–92.
Yang M, Li ZS, Xu XR, et al. Characterization of cortical potentials evoked by oesophageal balloon distention and acid perfusion in patients with functional heartburn. Neurogastroenterol Motil. 2006;18:292–9.
Vela MF, Craft BM, Sharma N, et al. Refractory heartburn: comparison of intercellular space diameter in documented GERD vs. functional heartburn. Am J Gastroenterol. 2011;106:844–50.
Woodland P, Al-Zinaty M, Yazaki E, et al. In vivo evaluation of acid-induced changes in oesophageal mucosa integrity and sensitivity in non-erosive reflux disease. Gut. 2013;62:1256–61. This study suggests that a lower baseline impedance, as a measure for epithelial integrity, may distinguish NERD from functional heartburn.
Johnston BT, Lewis SA, Collins JS, et al. Acid perception in gastro-oesophageal reflux disease is dependent on psychosocial factors. Scand J Gastroenterol. 1995;30:1–5.
Shapiro M, Green C, Bautista JM, et al. Functional heartburn patients demonstrate traits of functional bowel disorder but lack a uniform increase of chemoreceptor sensitivity to acid. Am J Gastroenterol. 2006;101:1084–91.
Fass R, Sontag SJ, Traxler B, et al. Treatment of patients with persistent heartburn symptoms: a double-blind, randomized trial. Clin Gastroenterol Hepatol. 2006;4:50–6.
Shaheen NJ, Weinberg DS, Denberg TD, et al. Upper endoscopy for gastroesophageal reflux disease: best practice advice from the clinical guidelines committee of the American College of Physicians. Ann Intern Med. 2012;157:808–16.
Poh CH, Gasiorowska A, Navarro-Rodriguez T, Willis MR, Hargadon D, Noelck N, et al. Upper GI tract findings in patients with heartburn in whom proton pump inhibitor treatment failed versus those not receiving antireflux treatment. Gastrointest Endosc. 2010;71(1):28–34.
Kahrilas PJ, Bredenoord AJ, Fox M, Gyawali CP, Roman S, Smout AJ, et al. The Chicago Classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil. 2015;27(2):160–74.
Zerbib F, Roman S, Ropert A, des Varannes SB, Pouderoux P, Chaput U, et al. Esophageal pH-impedance monitoring and symptom analysis in GERD: a study in patients off and on therapy. Am J Gastroenterol. 2006;101(9):1956–63.
Hemmink GJ, Bredenoord AJ, Weusten BL, Monkelbaan JF, Timmer R, Smout AJ. Esophageal pH-impedance monitoring in patients with therapy-resistant reflux symptoms: ‘on’ or ‘off’ proton pump inhibitor? Am J Gastroenterol. 2008;103(10):2446–53.
Kindt S, Tack J. Pathophysiology of noncardiac chest pain: not only acid. Dis Mon. 2008;54(9):615–26.
Wang WH, Huang JQ, Zheng GF, Wong WM, Lam SK, Karlberg J, et al. Is proton pump inhibitor testing an effective approach to diagnose gastroesophageal reflux disease in patients with noncardiac chest pain?: a meta-analysis. Arch Intern Med. 2005;165(11):1222–8.
Richter JE, Dalton CB, Bradley LA, Castell DO. Oral nifedipine in the treatment of noncardiac chest pain in patients with the nutcracker esophagus. Gastroenterology. 1987;93(1):21–8.
Balaban DH, Yamamoto Y, Liu J, et al. Sustained esophageal contraction: a marker of esophageal chest pain identified by intraluminal ultrasonography. Gastroenterology. 1999;116:29–37.
Pehlivanov N, Liu J, Mittal RK. Sustained esophageal contraction: a motor correlate of heartburn symptom. Am J Physiol Gastrointest Liver Physiol. 2001;281:G743–51.
Mittal RK, Buck M, Ledgerwood MM, Jiang Y. Low esophageal wall blood perfusion & hypoxia in esophageal mucosa in patients with nutcracker esophagus. Gastroenterology. 2015;4:S75–6.
Richter JE, Barish CF, Castell DO. Abnormal sensory perception in patients with esophageal chest pain. Gastroenterology. 1986;91:845–52.
Rao SS, Gregersen H, Hayek B, et al. Unexplained chest pain: the hypersensitive, hyperreactive, and poorly compliant esophagus. Ann Intern Med. 1996;124:950–8.
Brock C, Andresen T, Frøkjaer JB, Gale J, Olesen AE, Arendt-Nielsen L, et al. Central pain mechanisms following combined acid and capsaicin perfusion of the human oesophagus. Eur J Pain. 2010;14(3):273–81.
Fagring AJ, Gaston-Johansson F, Kjellgren KI, et al. Unexplained chest pain in relation to psychosocial factors and health-related quality of life in men and women. Eur J Cardiovasc Nurs. 2007;6:329–36.
Stollman NH, Bierman PS, Ribeiro A, et al. CO2 provocation of panic: symptomatic and manometric evaluation in patients with noncardiac chest pain. Am J Gastroenterol. 1997;92:839–42.
Cooke RA, Anggiansah A, Wang J, et al. Hyperventilation and esophageal dysmotility in patients with noncardiac chest pain. Am J Gastroenterol. 1996;91:480–4.
Cremonini F, Wise J, Moayyedi P, Talley NJ. Diagnostic and therapeutic use of proton pump inhibitors in non-cardiac chest pain: a metaanalysis. Am J Gastroenterol. 2005;100(6):1226–32.
Ghillebert G, Janssens J. Provocation tests versus 24-h pH and pressure measurements. Eur J Gastroenterol Hepatol. 1995;7(12):1141–6.
Tack J, Zaninotto G. Therapeutic options in oesophageal dysphagia. Nat Rev Gastroenterol Hepatol. 2015;12(6):332–41.
Vanuytsel T, Bisschops R, Farré R, Pauwels A, Holvoet L, Arts J, et al. Botulinum toxin reduces dysphagia in patients with nonachalasia primary esophageal motility disorders. Clin Gastroenterol Hepatol. 2013;11(9):1115–1121.e2.
Marjoux S, Pioche M, Benet T, Lanne JS, Roman S, Ponchon T, et al. Fatal mediastinitis following botulinum toxin injection for esophageal spasm. Endoscopy. 2013;45(Suppl 2 UCTN):E405–6.
Weijenborg PW, de Schepper HS, Smout AJ, Bredenoord AJ. Effects of antidepressants in patients with functional esophageal disorders or gastroesophageal reflux disease: a systematic review. Clin Gastroenterol Hepatol. 2015;13(2):251–259.e1. Comprehensive review on the effect of antidepressants in functional esophageal disorders.
Peghini PL, Katz PO, Castell DO. Imipramine decreases oesophageal pain perception in human male volunteers. Gut. 1998;42(6):807–13.
Gorelick AB, Koshy SS, Hooper FG, Bennett TC, Chey WD, Hasler WL. Differential effects of amitriptyline on perception of somatic and visceral stimulation in healthy humans. Am J Physiol. 1998;275(3 Pt 1):G460–6.
Cannon 3rd RO, Quyyumi AA, Mincemoyer R, et al. Imipramine in patients with chest pain despite normal coronary angiograms. N Engl J Med. 1994;330:1411–7.
Clouse RE, Lustman PJ, Eckert TC, et al. Low-dose trazodone for symptomatic patients with esophageal contraction abnormalities. a double-blind, placebo-controlled trial. Gastroenterology. 1987;92:1027–36.
Broekaert D, Fischler B, Sifrim D, et al. Influence of citalopram, a selective serotonin reuptake inhibitor, on oesophageal hypersensitivity: a double-blind, placebo-controlled study. Aliment Pharmacol Ther. 2006;23:365–70.
Varia I, Logue E, O’Connor C, et al. Randomized trial of sertraline in patients with unexplained chest pain of noncardiac origin. Am Heart J. 2000;140:367–72.
Doraiswamy PM, Varia I, Hellegers C, et al. A randomized controlled trial of paroxetine for noncardiac chest pain. Psychopharmacol Bull. 2006;39:15–24.
Spinhoven P, Van der Does AJ, Van Dijk E, et al. Heart-focused anxiety as a mediating variable in the treatment of noncardiac chest pain by cognitive-behavioral therapy and paroxetine. J Psychosom Res. 2010;69:227–35.
Lee H, Kim JH, Min BH, et al. Efficacy of venlafaxine for symptomatic relief in young adult patients with functional chest pain: a randomized, double-blind, placebo-controlled, crossover trial. Am J Gastroenterol. 2010;105:1504–12. Well-conducted randomized cross-over study demonstrating efficacy of venlafaxine on non-cardiac chest pain, but at the cost of side effects.
Kisely S, Campbell LA, Skerritt P. Psychological interventions for symptomatic management of non-specific chest pain in patients with normal coronary anatomy. Cochrane Database Syst Rev. 2015;30(6):CD004101.
Shapiro M, Shanani R, Taback H, et al. Functional chest pain responds to biofeedback treatment but functional heartburn does not: what is the difference? Eur J Gastroenterol Hepatol. 2012;24:708–14.
Rodriguez-Stanley S, Zubaidi S, Proskin HM, et al. Effect of tegaserod on esophageal pain threshold, regurgitation, and symptom relief in patients with functional heartburn and mechanical sensitivity. Clin Gastroenterol Hepatol. 2006;4:442–50.
Novartis. Press release: Novartis suspends US marketing and sales of Zelnorm in response to request from FDA. Available from: http://www.zelnorm.com/Zelnrom_PR_US_330_Final_12_1007.pdf.
Khajanchee YS, Hong D, Hansen PD, et al. Outcomes of antireflux surgery in patients with normal preoperative 24-hour pH test results. Am J Surg. 2004;187:599–603.
Campos GM, Peters JH, DeMeester TR, et al. Multivariate analysis of factors predicting outcome after laparoscopic Nissen fundoplication. J Gastrointest Surg. 1999;3:292–300.
Rao SS, Mudipalli RS, Remes-Troche JM, et al. Theophylline improves esophageal chest pain--a randomized, placebo-controlled study. Am J Gastroenterol. 2007;102:930–8.
Remes-Troche JM, Chahal P, Mudipalli R, et al. Adenosine modulates oesophageal sensorimotor function in humans. Gut. 2009;58:1049–55.
Chua YC, Ng KS, Sharma A, et al. Randomised clinical trial: pregabalin attenuates the development of acid-induced oesophageal hypersensitivity in healthy volunteers - a placebo-controlled study. Aliment Pharmacol Ther. 2012;35:319–26.
Krarup AL, Ny L, Astrand M, et al. Randomised clinical trial: the efficacy of a transient receptor potential vanilloid 1 antagonist AZD1386 in human oesophageal pain. Aliment Pharmacol Ther. 2011;33:1113–22.
Krarup AL, Ny L, Gunnarsson J, et al. Randomized clinical trial: inhibition of the TRPV1 system in patients with nonerosive gastroesophageal reflux disease and a partial response to PPI treatment is not associated with analgesia to esophageal experimental pain. Scand J Gastroenterol. 2013;48:274–84.
Sarkar S, Hobson AR, Hughes A, Growcott J, Woolf CJ, Thompson DG, et al. The prostaglandin E2 receptor-1 (EP-1) mediates acid-induced visceral pain hypersensitivity in humans. Gastroenterology. 2003;124(1):18–25.
Willert RP, Woolf CJ, Hobson AR, Delaney C, Thompson DG, Aziz Q. The development and maintenance of human visceral pain hypersensitivity is dependent on the N-methyl-D-aspartate receptor. Gastroenterology. 2004;126(3):683–92.
Bulmer DC, Botha CA, Wheeldon A, Grey K, Mein CA, Lee K, et al. Evidence of a role for GTP cyclohydrolase-1 in visceral pain. Neurogastroenterol Motil. 2015;27(5):656–62.
Kono T, Sei H, Yamasaki T, Tomita T, Oshima T, Fukui H, et al. A novel prostanoid EP1 receptor antagonist ONO-8539 reduces acid-induced heartburn symptoms in healthy volunteers. United European Gastroenterol J. 2015;3(5S):A90. abstract.
www.clinicaltrials.gov. A study of the effect of ONO-8539 on oesophageal pain hypersensitivity in patients with non-erosive reflux disease. ClinicalTrials.gov Identifier NCT01707901.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Tim Vanuytsel and Ans Pauwels declare that they have no conflict of interest.
Jan Tack reports money to institution for advice or lecture from AlfaWassermann, Almirall, AstraZeneca, Danone, Ironwood, Janssen, Menarini, Mylan, Novartis, Nutricia, Rhythm, Shionogi, Shire, SKLife, Takeda, Theravance, Tsumura, Yuhan, and Zeria.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Esophagus
Rights and permissions
About this article
Cite this article
Tack, J., Vanuytsel, T. & Pauwels, A. Established and Emerging Treatment Options for Functional Heartburn and Chest Pain. Curr Treat Options Gastro 14, 19–27 (2016). https://doi.org/10.1007/s11938-016-0081-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11938-016-0081-3