Abstract
Purpose of Review
The purpose of this review is to educate the reader about the evolving classification of axial spondyloarthritis (AxSpA) and describe recent treatment data from clinical trials of medications with mechanisms of action other than TNF inhibition. The review will also address emerging treatment strategies for AxSpA.
Recent Findings
New and more sensitive classification schema for AxSpA find that the prevalence of the disease is more than twice that of the historic definition of ankylosing spondylitis (AS), when patients without radiographically observable damage to the sacroiliac joints are included. TNF inhibitors have shown efficacy in the full spectrum of disease. IL-17 inhibitors, e.g., secukinumab and ixekizumab and janus kinase (JAK) inhibitors, have shown good efficacy and relatively good safety in radiographically defined AxSpA and are being tested in non-radiographic (nr) AxSpA. Several immunomodulatory medicines approved for psoriasis, psoriatic arthritis, and rheumatoid arthritis have not shown efficacy in AxSpA, highlighting the importance of conducting good-quality, placebo-controlled trials in this condition. Treatment strategies such as “treat to target” and tapering therapy are being studied.
Summary
There remains a large unmet need to identify and adequately treat the full spectrum of AxSpA. The use of TNF inhibitors has improved our ability to achieve remission or low disease activity in AxSpA. Newer medicines with different mechanisms of action, e.g., IL-17 or JAK inhibition, are also showing similar ability. Continued research, including identification of new targets of treatment, is critical.
Similar content being viewed by others
Notes
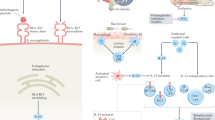
Inflammatory back pain, Arthritis, Enthesitis (heel), Uveitis, Dactylitis, Psoriasis, Crohn‘s disease/ulcerative colitis, Good response to NSAIDs, Family history for SpA, Elevated CRP, HLA-B*27.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
van der Linden S, Valkenburg HA, Cats A. Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum. 1984;27(4):361–8.
•• Reveille JD, Weisman MH. The epidemiology of back pain, axial spondyloarthritis and HLA-B27 in the United States. Am J Med Sci. 2013;345(6):431–6 Landmark paper describing the NHANEs epidemiologic survey in the USA, characterizing the prevalence of AxSpA in up to 1.4% of the population, and radiographic AxSpA or AS in approximately 0.5%, with detailed characterization by ethnicity, age, and gender.
Dougados M, van der Linden S, Juhlin R, et al. The European Spondylarthropathy Study Group preliminary criteria for the classification of spondylarthropathy. Arthritis Rheum. 1991;34:1218–27.
Amor B, Dougados M, Mijiyawa M. Criteria for the classification of spondyloarthropathies. Rev Rheum Mal Osteoaric. 1990;57:85–9.
Rudwaleit M, Landewe R, van der Heijde D, et al. The development of Assessment of Spondylo Arthritis International Society classification criteria for axial spondyloarthritis (part I): classification of paper patients by expert opinion including uncertainty appraisal. Ann Rheum Dis. 2009;68(6):770–6.
• Rudwaleit M, van der Heijde D, Landewe R, et al. The development of Assessment of Spondylo Arthritis International Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis. 2009;68(6):777–83 These two papers describe the axial spondyloarthritis classification criteria—the study design and conduct of the study upon which the criteria is based and the final criteria.
• Rudwaleit M, van der Heijde D, Landewe R, et al. The Assessment of Spondylo Arthritis International Society classification criteria for peripheral spondyloarthritis and for spondyloarthritis in general. Ann Rheum Dis. 2011;70(1):25–31 These two papers describe the axial spondyloarthritis classification criteria—the study design and conduct of the study upon which the criteria is based and the final criteria.
• van der Heijde D, Ramiro S, Landewe R, et al. 2016 update of the ASAS-EULAR management recommendations for axial spondyloarthritis. Ann Rheum Dis. 2017;76(6):978–91 This paper summarizes the most recent ASAS-EULAR treatment recommendations for AxSpA.
• Ward MM, Deodhar A, Akl EA, et al. American College of Rheumatology/Spondylitis Association of America/Spondyloarthritis Research and Treatment Network 2015 recommendations for the treatment of ankylosing spondylitis and nonradiographic Axial spondyloarthritis. Arthritis Rheum. 2016;68(2):282–98 This paper summarizes the ACR-SAA-SPARTAN treatment recommendations for AxSpA.
Dorner T, Strand V, Cornes P, et al. The changing landscape of biosimilars in rheumatology. Ann Rheum Dis. 2016;75(6):974–82.
Miossec P, Korn T, Kuchroo VK. Interleukin-17 and type 17 helper T cells. N Engl J Med. 2009;361(9):888–98.
•• Mease PJ. Inhibition of interleukin-17, interleukin-23 and the TH17 cell pathway in the treatment of psoriatic arthritis and psoriasis. Curr Opin Rheumatol. 2015;27(2):127–33 This paper reviews the IL-17/IL-23/TH17 cell pathway which is of critical importance in the pathophysiology of AxSpA, psoriasis, and psoriatic arthritis.
Appel H, Maier R, Wu P, et al. Analysis of IL-17(+) cells in facet joints of patients with spondyloarthritis suggests that the innate immune pathway might be of greater relevance than the Th17-mediated adaptive immune response. Arthritis Res Ther. 2011;13(3):R95.
Shen H, Goodall JC, Hill Gaston JS. Frequency and phenotype of peripheral blood Th17 cells in ankylosing spondylitis and rheumatoid arthritis. Arthritis Rheum. 2009;60(6):1647–56.
Zhang L, Li YG, Li YH, et al. Increased frequencies of Th22 cells as well as Th17 cells in the peripheral blood of patients with ankylosing spondylitis and rheumatoid arthritis. PLoS One. 2012;7(4):e31000.
Bowness P, Ridley A, Shaw J, et al. Th17 cells expressing KIR3DL2+ and responsive to HLA-B27 homodimers are increased in ankylosing spondylitis. J Immunol. 2011;186(4):2672–80.
•• Sherlock JP, Joyce-Shaikh B, Turner SP, et al. IL-23 induces spondyloarthropathy by acting on ROR-gammat+ CD3 + CD4-CD8- entheseal resident T cells. Nat Med. 2012;18(7):1069–76 Seminal paper, using a murine model, for the hypothesis that a key pathway in the pathogenesis of spondyloarthritides is through the stimulation of resident lymphocytes by IL-23 which in turn produce IL-17, IL-22, and TNF which interact with effector cells in various sites to create the osteolytic and osteoproliferative pathology of these conditions.
Reinhardt A, Yevsa T, Worbs T, et al. Interleukin-23-dependent gamma/delta T cells produce interleukin-17 and accumulate in the enthesis, aortic valve, and ciliary body in mice. Arthritis Rheum. 2016;68(10):2476–86.
• Baeten D, Sieper J, Braun J, et al. Secukinumab, an interleukin-17A inhibitor, in ankylosing spondylitis. N Engl J Med. 2015;373(26):2534–48 Paper describing the pivotal trials leading to the approval of secukinumab, an IL-17i, in ankylosing spondylitis.
• van der Heijde D, Cheng-Chung Wei J, Dougados M, et al. Ixekizumab, an interleukin-17A antagonist in the treatment of ankylosing spondylitis or radiographic axial spondyloarthritis in patients previously untreated with biological disease-modifying anti-rheumatic drugs (COAST-V): 16 week results of a phase 3 randomized, double-blind, active-controlled and placebo-controlled trial. Lancet. 2018;392(10163):2441–51 Paper describing a pivotal trial of ixekizumab, an IL-17i, in AS/radiographic AxSpA (r-AxSpA) patients naïve to biologic therapy.
• Deodhar A, Poddubnyy D, Pacheco-Tena C, et al. Efficacy and safety of ixekizumab in the treatment of radiographic axial spondyloarthritis: 16 week results of a phase 3 randomized, double-blind, placebo controlled trial in patients with prior inadequate response or intolerance to tumor necrosis factor inhibitors. Arthritis Rheum. 2018; Paper describing a pivotal trial of ixekizumab, an IL-17i, in AS/r-AxSpA patients who have previously been treated with TNFi.
•• Lories RJ, McInnes IB. Primed for inflammation: enthesis-resident T cells. Nat Med. 2012;18(7):1018–9 Eloquent editorial on the importance of reference 17, the Sherlock paper.
Mease PJ. Biologic therapy for psoriatic arthritis. Rheum Dis Clin N Am. 2015;41(4):723–38.
Kaushik SB, Lebwohl MG. Review of safety and efficacy of approved systemic psoriasis therapies. Int J Dermatol. 2018.
Poddubnyy D, Hermann KG, Callhoff J, et al. Ustekinumab for the treatment of patients with active ankylosing spondylitis: results of a 28-week, prospective, open-label, proof-of-concept study (TOPAS). Ann Rheum Dis. 2014;73(5):817–23.
Deodhar A, Gensler LS, Sieper J, et al. Three multicenter, randomized, double-blind, placebo-controlled studies evaluating the efficacy and safety of ustekinumab in axial spondyloarthritis. Arthritis Rheum. 2018.
Mease PJ, Kellner H, Morita A, et al. Efficacy and safety of risankizumab, a selective il-23p19 inhibitor, in patients with active psoriatic arthritis over 24 weeks: results from a phase 2 trial. Arthritis Rheum. 2017;69(suppl 10).
Gordon KB, Strober B, Lebwohl M, et al. Efficacy and safety of risankizumab in moderate-to-severe plaque psoriasis (UltIMMa-1 and UltIMMa-2): results from two double-blind, randomised, placebo-controlled and ustekinumab-controlled phase 3 trials. Lancet. 2018;392(10148):650–61.
Baeten D, Ostergaard M, Wei JC, et al. Risankizumab, an IL-23 inhibitor, for ankylosing spondylitis: results of a randomised, double-blind, placebo-controlled, proof-of-concept, dose-finding phase 2 study. Ann Rheum Dis. 2018;77(9):1295–302.
• Mease P. Ustekinumab fails to show efficacy in a phase III axial spondyloarthritis program: the importance of negative results. Arthritis Rheum. 2019;71(2):179–81 Editorial hypothesizing why two medications which inhibit IL-23, ustekinumab and risankizumab, may have failed to show efficacy in the treatment of ankylosing spondylitis.
Pathan E, Abraham S, Van Rossen E, et al. Efficacy and safety of apremilast, an oral phosphodiesterase 4 inhibitor, in ankylosing spondylitis. Ann Rheum Dis. 2013;72(9):1475–80.
• van der Heijde D, Deodhar A, Wei JC, et al. Tofacitinib in patients with ankylosing spondylitis: a phase II, 16-week, randomised, placebo-controlled, dose-ranging study. Ann Rheum Dis. 2017;76(8):1340–7 Pivotal studies demonstrating the effectiveness of two JAK inhibitors, tofacitinib, and filgotinib in the treatment of ankylosing spondylitis.
•• van der Heijde D, Baraliakos X, Gensler LS, et al. Efficacy and safety of filgotinib, a selective Janus kinase 1 inhibitor, in patients with active ankylosing spondylitis (TORTUGA): results from a randomised, placebo-controlled, phase 2 trial. Lancet. 2018;392(10162):2378–87 Pivotal studies demonstrating the effectiveness of two JAK inhibitors, tofacitinib, and filgotinib in the treatment of ankylosing spondylitis.
Smolen J, Breedveld F, Burmester G, et al. Extended report: treating rheumatoid arthritis to target: 2014 update of the recommendations of an international task force. Ann Rheum Dis. 2015.
Smolen JS, Braun J, Dougados M, et al. Treating spondyloarthritis, including ankylosing spondylitis and psoriatic arthritis, to target: recommendations of an international task force. Ann Rheum Dis. 2014;73(1):6–16.
•• Smolen JS, Schols M, Braun J, et al. Treating axial spondyloarthritis and peripheral spondyloarthritis, especially psoriatic arthritis, to target: 2017 update of recommendations by an international task force. Ann Rheum Dis. 2018;77(1):3–17 Synopsis of the systematic literature review and expert discussion on the “treat-to-target” concept in the management of AxSpA and psoriatic arthritis.
Coates LC, Moverley AR, McParland L, et al. Effect of tight control of inflammation in early psoriatic arthritis (TICOPA): a UK multicentre, open-label, randomised controlled trial. Lancet. 2015;386(10012):2489–98.
van den Bosch F, Carron P, Mease P. Biologic treatment of axial spondyloarthritis. Chapter 15. In: Mease P, Khan M, editors. Axial spondyloarthritis: Elsevier Inc; 2019. p. 223–38.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Mease reports grants and personal fees from AbbVie, grants and personal fees from Amgen, grants and personal fees from Bristol Myers Squibb, personal fees from Boehringer Ingelheim, grants and personal fees from Celgene, personal fees from Galapagos, personal fees from Genentech, personal fees from Gilead, grants and personal fees from Janssen, grants and personal fees from Lilly, grants and personal fees from Novartis, grants and personal fees from Pfizer, grants and personal fees from Sun, grants and personal fees from UCB, during the conduct of the study.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Spondyloarthritis
Rights and permissions
About this article
Cite this article
Mease, P. Emerging Immunomodulatory Therapies and New Treatment Paradigms for Axial Spondyloarthritis. Curr Rheumatol Rep 21, 35 (2019). https://doi.org/10.1007/s11926-019-0830-0
Published:
DOI: https://doi.org/10.1007/s11926-019-0830-0