Abstract
Purpose of Review
It is well established that controlled immune activation and balance is critical for women’s reproductive health and successful pregnancy outcomes. Research in recent decades in both clinical and animal studies has demonstrated that aberrant immune activation and inflammation play a role in the development and progression of women’s reproductive health and pregnancy-related disorders. Inflammasomes are multi-protein cytoplasmic complexes that mediate immune activation. In this review, we summarize current knowledge on the role of inflammasome activation in pregnancy-related disorders.
Recent Findings
Increased activation of inflammasome is associated with multiple women’s health reproductive disorders and pregnancy-associated disorders, including preeclampsia (PreE). Inflammasome activation is also associated with the novel coronavirus disease 2019 (COVID-19) disease caused by the SARS-Cov-2 virus. We and others have observed a positive association between increased PreE incidences with the onset of the COVID-19 pandemic. Here, we present our recent data indicating increased inflammasome activation, represented by caspase-1 activity, in women with COVID-19 and PreE compared to normotensive pregnant women COVID-19.
Summary
The role of inflammation in pregnancy-related disorders is an area of intense research interest. With the onset of the COVID-19 pandemic and the associated increase in PreE observed clinically, there is a greater need to identify mechanisms of pathophysiology and targets to treat this maternal disorder. Inflammasome activation is associated with PreE and COVID-19 infection and may hold therapeutic potential to improve outcomes associated with PreE and curb the morbidity attributed to PreE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammation in the female reproductive system contributes to various disorders of pregnancy and reproductive health [1,2,3,4]. Inflammasomes are cytoplasmic, multi-protein complexes that mediate innate and adaptive immune responses and inflammation [5, 6]. As members of the innate immune system, inflammasomes recognize patterns indicative of infection or changes in cellular homeostasis and initiate responses by the immune system to eliminate pathogens and repair tissue damage to restore homeostasis. Recent studies have identified associations between various women’s reproductive disorders, particularly in pregnancy, and inflammasome expression and activation [2, 7,8,9,10,11]. More recently, the discovery of inflammasomes has peaked research interest in investigating the roles of this novel immune modulating complex in these reproductive and pregnancy-associated disorders and complications. This review will summarize the recent studies investigating the role of inflammasome activation in reproductive disorders with a special emphasis on preeclampsia (PreE). The advances in our understanding of how inflammasomes contribute to these women’s health-related issues may provide novel targets and therapeutic strategies to improve women’s reproductive health and pregnancy-related outcomes.
Inflammasomes and the Immune System
Normal pregnancy requires a controlled state of inflammation in order for proper placentation and vascular remodeling to occur during the initial stages of pregnancy [12]. These immune changes promote tolerance of the semi-allogenic fetus, while also still protecting the mother from external infectious diseases. In pregnancy-related disorders and complications, the immune changes that occur are associated with chronic immune activation and inflammation that contribute to pathological changes in reproductive tissue and pathophysiology in women and their offspring. Both clinical and preclinical studies have identified the roles of various factors of the immune system including innate and adaptive immune cells and cytokines in contributing to these disorders.
Inflammasomes are formed by a complex of proteins consisting of a sensor protein, an adaptor protein, and caspase-1. The sensor proteins are named based on their structural domain: (1) the nucleotide-binding domain and leucine-rich repeat containing proteins (NLRs); (2) the absence in melanoma 2 (AIM2)-like receptors (ALRs); and (3) the pyrin receptor. The adaptor protein, apoptosis-associated speck-like protein containing a caspase activation and recruitment domain (CARD), also known as Pycard (ASC) contains the PYD (pyrin domain) and CARD (caspase activation and recruitment domain) which serves as the connector protein to bring the sensor protein and caspase-1 together in the inflammasome complex [5, 6, 13•]. The inflammasomes that have been described to date include NLRP1, NLRP3, NLRC4, NLRP7, NLRP12, AIM2, and PYD. Other sensor proteins that have been proposed include human NLRP2, NLRP7, and IF116, and murine NLRP6 and NLRP9b in mouse [13•, 14]. These inflammasomes have recently been reviewed elsewhere [13•].
Canonical activation of inflammasomes includes the recruitment of the sensor protein, ASC, and pro-caspase 1 into a single multi-protein complex within the cytoplasm. After the inflammasome is assembled, caspase-1 is autocleaved into enzymatically active caspase-1 p20 and p10 subunits [13•, 15]. The active caspase then goes on to cleave inactive forms of the pleiotropic cytokines interleukin- 1 beta (IL-1β) and IL-18 into their active forms to be secreted from cells. More recently, it has been discovered that caspase-1 also cleaves a protein, gasdermin D, which initiates pyroptosis, inflammatory cell death that is induced following inflammasome activation [16].
Inflammasomes and Preeclampsia
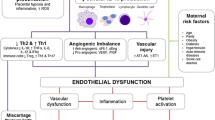
PreE is a disease defined by new onset hypertension after 20 weeks of gestation in combination with organ dysfunction and is a major contributor to maternal and fetal morbidity worldwide [17, 18]. The exact mechanisms underlying the development of PreE are not known. However, endothelial dysfunction and a pro-inflammatory state resulting from placental ischemia caused by shallow trophoblast invasion and insufficient uterine spiral artery remodeling is a well-accepted mechanism [19, 20]. Recent studies are beginning to report elevations in inflammasomes or related mediators among women with PreE or women who are at risk for developing PreE [21,22,23]. As much of the data and studies have focused primarily on NLRP3 inflammasomes, the remainder of this review will also be composed of mostly NLRP3 studies.
NLRP3 and PreE
NLRP3 inflammasomes are intracellular protein complexes associated with the innate immune system. Overactivation of NLRP3 inflammasomes contributes to a variety of disorders such as atherosclerosis, diabetes, and obesity-induced insulin resistance [24]. NLRP3 inflammasomes can be activated via transcriptional dependent and independent pathways through endogenous or exogenous damage-associated molecular patterns (DAMPs) [25•] (Fig. 1). Regardless of the activation pathway, women with PreE have evidence of a number of inflammatory events that can activate each component of the NLRP3 inflammasome, which may provide some foundation as to why immune system dysfunction is prevalent among women with PreE [26].
Mechanisms of NLRP3 inflammasome assembly via priming and activation. The priming signal works to activate nuclear factor kappa B (NF-κB) which in turn stimulates translation of NLRP3 and release from the nucleus. Once NLRP3 is in the cytoplasm, it can be activated via a variety of activation signals or DAMPs (i.e., uric acid, cholesterol, extracellular debris, extracellular vesicles, reactive oxygen species). Upon activation, there is a conformational change leading to formation of the NLRP3 inflammasome. The CARD-CARD interaction leads to the cleavage of caspase-1, which in turn activates IL-1β, IL-18, and gasdermin D
There have been numerous reports of elevations in placental and systemic NF-κB among women with PreE compared to normotensive women [27]. From these studies one can theorize that with elevated levels of NF-κB, there is also an increase in the translation of NLRP3. Women with PreE have increased levels of circulating cellular debris, protein aggregates, hypoxia factors and more soluble factors such as uric acid and cholesterol; all of which have been reported to activate NLRP3 at a higher rate in comparison to other inflammasomes [28, 29]. In regard to women with PreE, studies have reported that cholesterol and uric acid can cause placental and decidual inflammation by activating NLRP3 [28, 30,31,32]. Along similar lines, Weel et al. reported that PreE women had significantly higher placental expression of NLRP3, caspase-1, and IL-1β compared to normotensive women [21]. In addition to uterine and placental tissues expressing NLRP3, a recent study by Ozeki et al. reported that human umbilical vein endothelial cells (HUVECs) isolated directly from women with PreE had evidence of a greater NLRP3 response relative to HUVECs isolated from normotensive women [33], suggesting that circulating factors, in particular S100A9, directly stimulate NLRP3 activity in endothelial cells.
HELLP (hemolysis elevated liver enzyme low platelet) syndrome is a severe obstetric complication that affects 15–20% of women with PreE and 1–2% of women without PreE [34]. Unlike PreE, the diagnosis of HELLP requires evidence of significant organ, thrombosis, and coagulopathy via a series of laboratory diagnoses. Even though at the time of this review, there are not any published reports of inflammasome activity among women with HELLP syndrome, there is also evidence to support a role for NLRP3 inflammasome activation in the pathogenesis of this disorder. Heme, which is increased in women with HELLP syndrome, has been found to stimulate activation of HUVEC NLRP3 inflammasomes [35]. Women with HELLP also have a a high degree of apoptosis which is mediated though the death receptor Fas ligand [36]. Activation of this pathway contributes to DAMPs which lead to activation of the NLRP3 inflammasome and eventually pyroptosis [37].
Preclinical Studies
Similar to what has been reported among pregnant women, NLRP3 inflammasomes are also activated in rodents due to numerous factors. A variety of PreE animal models have been used to provide more insight into immunological mechanisms associated with PreE [38,39,40]. A study by Zeng et al. which utilized a PreE rat model reported that PreE rats had higher mRNA expression of NLRP3 in uterine tissues compared to normal pregnant rats [41]. This group also found that both uterine protein expression of caspase-1 along with mRNA expression of caspase-1 and IL-1β were increased, leading them to conclude that the NLRP3 inflammasome has a key role in regulating uterine inflammation. Similarly IL-17, which we have previously reported to have a key role in mediating the hypertensive and immune response in PreE was recently reported to also regulate NLRP3 inflammasome activation [42, 43]. Chang et al. reported that in a PreE mouse model inhibition of fatty acid binding protein 4 prevents the Treg (T regulatory)/Th17 (T helper) imbalance, IL-17A production, and NLRP3 inflammasome activation [44].
Inflammasome, Spontaneous Miscarriage, and Preterm Labor
In addition to their roles in pregnancy disorders such as PreE and HELLP syndrome, inflammasomes have also been linked to recurrent pregnancy loss as well as missed abortions and spontaneous preterm labor. It is estimated that 21% of preterm births from women in the USA occur in women with PreE, a risk factor for spontaneous preterm labor [45, 46]. Several studies have suggested that inflammasome activation is an important component driving spontaneous preterm labor. Elevated levels of pro-inflammatory mediators that are downstream of inflammasome activation such as HMBGI, caspase-1, IL-1β, and IL-18 were found in women that underwent spontaneous preterm labor [47–49]. Direct evidence of increased NLRP1, NLRP3, and NLRC4 expression have been found in chorioamniotic membranes from women that experienced acute histologic chorioamnionitis in spontaneous preterm labor [47]. The authors in those studies proposed that inflammation associated with spontaneous preterm labor is driven by inflammasome activation, triggering production of IL-1β and IL-18 [47, 48]. These findings suggest that inflammasome-driven inflammation in the chorioamniotic membrane can induce spontaneous preterm labor. Given the amount of immunological crosstalk between reproductive disorders, the role of inflammasomes provides yet another avenue of potential linkage among women affected by reproductive complications.
Coronavirus Disease 2019 (COVID-19), Inflammasome Activation and PreE
Inflammasomes have a role in regulating inflammation which makes them crucial in inflammatory diseases or diseases where inflammation plays a role [50]. The exact role and incidence of this becomes evident when focusing on COVID-19, a disease commonly associated with hyperinflammation. Among the first clues for inflammasome activation in patients with COVID-19 was the noted cytokine storm in patients with severe COVID-19 which is composed of cytokines often activated via NF-κB and IL-1β pathways [51••]. As data began emerging, there was also a direct correlation between high circulating IL-18 levels, COVID-19 severity and increased mortality [52]. The specific mechanism by which SARS-Co-V2 activates inflammasomes, and NLRP3 in particular, is still unknown. Previous studies examining the SARS-Co-V-2 virus have indicated that NLRP3 is assembled and activated in response to changes in plasma permeability to calcium and potassium ions and increases in mitochondrial reactive oxygen species [53, 54].
Pan et al. recently reported that the N protein of SARS-CoV-2 selectively interacts with NLRP3 and not with NLRP1 or NLRC4 or AIM2 proteins [55]. This group also reports that the N protein promotes the assembly of the NLRP3 inflammasome through promotion of ASC oligomerization. The N protein is responsible for packaging the viral genome into a nucleocapsid protein located within the phospholipid bilayers, which is covered by spike proteins [56]. Due to COVID-19, there has been an upsurgence of research into this virus and into the N protein. A recent study [62] has suggested that the N protein itself can regulate immune function to either an immunosuppressive state or an overactive state. Along these same lines, it has been suggested that NLRP3 inflammasome–mediated pyroptosis and the cytokine storm only occur in individuals with an impaired immune system, suggestive of an initial low grade inflammation prior to the onset of infection [62]. This theory has been used to explain some of the differences in symptoms (asymptomatic vs symptomatic) that has been reported between patients with COVID-19 [58]. The combination of these studies, along with the fact that COVID-19 is associated with an increased risk of PreE or HELLP syndrome (both published studies [59•] and observations from our own patient population), led us to question if there was evidence of NLRP3 activation among women with COVID-19 and PreE.
To determine if there was evidence of inflammasome activation among pregnant women with COVID-19, we measured caspase-1 activity in the cell culture media. Previous studies have reported that circulating factors from women with PreE stimulate HUVECs in vitro to produce a variety of vasoconstrictive and inflammatory markers [60]. We conducted this assay to see if (1) pregnant women diagnosed with COVID-19 at term had evidence of inflammasome activation, (2) if PreE in the presence of a COVID-19 diagnosis at term was associated with inflammasome activation, and (3) if there were differences between symptomatic vs. asymptomatic patients. As shown in Fig. 2, serum from women with PreE induced more caspase-1 activity in cultured HUVECs relative to normotensive women. There was also a difference in caspase-1 activity between symptomatic and asymptomatic women regardless of their PreE diagnosis. Specifically, inflammasome activation is increased in women who were symptomatic for COVID-19. Furthermore, only COVID-19 positive symptomatic women diagnosed with PreE had caspase-1 levels higher than PreE women without COVID-19 (mean caspase-1 activity is denoted by black line). As caspase-1 is activated by inflammasome complex formation and activated via both the non-canonical and canonical pathways, it serves as an essential marker of inflammasome function and activity [61].
Caspase-1 activity in endothelial cells exposed to sera from COVID pregnant patients. Serum was collected from women consented and enrolled in an IRB-approved study and placed over semi-confluent HUVECs for 24 h, as previously described [60]. Following 24 h of exposure to experimental media (50% Dulbecco modified Eagle’s medium (Invitrogen), 50% medium 199 (Invitrogen), 1% antimycotic-antibotic solution (Invitrogen), and 10% patient serum) basal media (media without any serum) were placed on cells for 24 h before a sample of the media was collected for caspase-1 evaluation. All cell culture experiments were performed in duplicate, and media samples were assayed in duplicate for caspase-1 activity via the Caspase-Glo 1 Inflammasome assay (Promega, Madison, WI). Luminescence was recorded after 90 min. The number of patients whose serum was evaluated is represented in white within the respective bar located on the bar graph. All the data are represented as mean ± standard error mean. Gestational age at serum collection for normotensive women was 39.1 ± 0.27 weeks (range 37.1–40 weeks), 34.58 ± 0.99 weeks (range 30.2–38.4 weeks) for COVID positive preeclamptic women, and 34.8 ± 2.1 weeks (range 30.6–38.4 weeks) for non-COVID positive preeclamptic women
Inflammasome Targeted Therapy
Not only has NLRP3 activation been shown to increase inflammation, but several in vivo studies have also shown inhibition of NLRP3 activation can reduce the abnormal inflammatory cascade seen in PreE [44, 65,66,67,68]. Currently, there are several potential therapeutic approaches for inhibiting the inflammasome or targeting pro-inflammatory cytokines. However, as many of these therapies pose a potential danger to the growing fetus; there is often no direct treatment that can be safely administered during pregnancy. There is also a large body of evidence indicating a decrease in the maternal immune response shortly after delivery of the placenta, which decreases the need for pharmaceutical therapy. However, there are a few therapies that are administered during pregnancy that may have an indirect effect on inflammasome activity (Table 1).
Conclusions
The pathophysiology of PreE is still unclear; however, there is a clear consensus on the involvement of the immune system in the disease process. Understanding the role of the inflammasome(s) and how potential inflammasome inhibition could mitigate other immune pathways and pyroptosis warrants further investigation. New data, demonstrating a link between inflammasome activation and COVID-19 and the increased risk for women with COVID-19 to develop PreE, further highlights the need to better understand the role of inflammasomes in PreE to possibly identify new and novel therapeutic interventions thereby potentially decreasing maternal and fetal mortality and morbidity.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Mattina GF, Van Lieshout RJ, Steiner M. Inflammation, depression and cardiovascular disease in women: the role of the immune system across critical reproductive events. Ther Adv Cardiovasc Dis. 2019;13:1753944719851950. https://doi.org/10.1177/1753944719851950.
Tersigni C, Vatish M, D’Ippolito S, Scambia G, Di Simone N. Abnormal uterine inflammation in obstetric syndromes: molecular insights into the role of chemokine decoy receptor D6 and inflammasome NLRP3. Mol Hum Reprod. 2020;26(2):111–21. https://doi.org/10.1093/molehr/gaz067.
Cornelius DC, Cottrell J, Amaral LM, LaMarca B. Inflammatory mediators: a causal link to hypertension during preeclampsia. Br J Pharmacol. 2019;176(12):1914–21. https://doi.org/10.1111/bph.14466.
LaMarca B, Cornelius DC, Harmon AC, Amaral LM, Cunningham MW, Faulkner JL, et al. Identifying immune mechanisms mediating the hypertension during preeclampsia. Am J Physiol Regul Integr Comp Physiol. 2016;311(1):R1-9. https://doi.org/10.1152/ajpregu.00052.2016.
Stutz A, Golenbock DT, Latz E. Inflammasomes: too big to miss. J Clin Invest. 2009;119(12):3502–11. https://doi.org/10.1172/JCI40599.
Festjens N, Cornelis S, Lamkanfi M, Vandenabeele P. Caspase-containing complexes in the regulation of cell death and inflammation. Biol Chem. 2006;387(8):1005–16. https://doi.org/10.1515/BC.2006.124.
Murthi P, Rajaraman G. Inflammasomes in the pathophysiology of maternal obesity: potential therapeutic targets to reduce long-term adverse health outcomes in the mother and offspring. Curr Vasc Pharmacol. 2021;19(2):165–75. https://doi.org/10.2174/1570161118666200603131536.
Rogers LM, Serezani CH, Eastman AJ, Hasty AH, Englund-Ogge L, Jacobsson B, et al. Palmitate induces apoptotic cell death and inflammasome activation in human placental macrophages. Placenta. 2020;90:45–51. https://doi.org/10.1016/j.placenta.2019.12.009.
Rostamtabar M, Esmaeilzadeh S, Karkhah A, Amiri M, Rahmani A, Bakouei F, et al. Elevated expression of IL-18 but not IL-1beta gene is associated with NALP3 and AIM2 inflammasome in Polycystic Ovary Syndrome. Gene. 2020;731: 144352. https://doi.org/10.1016/j.gene.2020.144352.
Murthi P, Pinar AA, Dimitriadis E, Samuel CS. Inflammasomes-a molecular link for altered immunoregulation and inflammation mediated vascular dysfunction in preeclampsia. Int J Mol Sci. 2020;21(4). https://doi.org/10.3390/ijms21041406.
Gomez-Lopez N, Motomura K, Miller D, Garcia-Flores V, Galaz J, Romero R. Inflammasomes: their role in normal and complicated pregnancies. J Immunol. 2019;203(11):2757–69. https://doi.org/10.4049/jimmunol.1900901.
Wang Z, Yang R, Zhang J, Wang P, Wang Z, Gao J, et al. Role of extracellular vesicles in placental inflammation and local immune balance. Mediators Inflamm. 2021;2021:5558048. https://doi.org/10.1155/2021/5558048.
• Place DE, Kanneganti TD. Recent advances in inflammasome biology. Curr Opin Immunol. 2018;50:32–8. https://doi.org/10.1016/j.coi.2017.10.011. This review focuses on how inflammasomes are activated and what is known about their mechanisms of action.
Mathur A, Hayward JA, Man SM. Molecular mechanisms of inflammasome signaling. J Leukoc Biol. 2018;103(2):233–57. https://doi.org/10.1189/jlb.3MR0617-250R.
Broz P, von Moltke J, Jones JW, Vance RE, Monack DM. Differential requirement for caspase-1 autoproteolysis in pathogen-induced cell death and cytokine processing. Cell Host Microbe. 2010;8(6):471–83. https://doi.org/10.1016/j.chom.2010.11.007.
Man SM, Karki R, Kanneganti TD. Molecular mechanisms and functions of pyroptosis, inflammatory caspases and inflammasomes in infectious diseases. Immunol Rev. 2017;277(1):61–75. https://doi.org/10.1111/imr.12534.
Abalos E, Cuesta C, Grosso A, Chou D, Say L. Global and regional estimates of preeclampsia and eclampsia: a systematic review. Eur J Obstet Gynecol Reprod Biol. 2013;170(1):1–7.
Duley L. The global impact of pre-eclampsia and eclampsia. Semin Perinatol. 2009;33:130–7.
Pankiewicz K, Fijalkowska A, Issat T, Maciejewski T. Insight into the key points of preeclampsia pathophysiology: uterine artery remodeling and the role of MicroRNAs. Int J Mol Sci. 2021;22(6):3132.
Redman C, Sargent I. Immunology of pre-eclampsia. Am J Reprod Immunol. 2010;63(6):534–43. https://doi.org/10.1111/j.1600-0897.2010.00831.x.
Weel IC, Romão-Veiga M, Matias ML, Fioratti EG, Peraçoli JC, Borges VT, Araujo Jr JP, Peraçoli MT. Increased expression of NLRP3 inflammasome in placentas from pregnant women with severe preeclampsia. J Reprod Immunol. 2017;123:40-7. https://doi.org/10.1016/j.jri.2017.09.002.
Xu L, Li S, Liu Z, Jiang S, Wang J, Guo M, et al. The NLRP3 rs10754558 polymorphism is a risk factor for preeclampsia in a Chinese Han population. J Matern Fetal Neonatal Med. 2019;32:1792–9.
Pontillo A, Reis E, Bricher P, Vianna P, Dinz S, Fernandes K, et al. NLRP1 L155H Polymorphism is a risk factor for preeclampsia development. Am J Reprod Immunol. 2015;73:577–81.
Zheng D, Liwinski T, Elinav E. Inflammasome activation and regulation: toward a better understanding of complex mechanisms. Cell Discovery. 2020;6:36.
• Yang Y, Wang H, Kouadir M, Song H, Shi F. Recent advances in the mechanisms of NLRP3 inflammasome activation and its inhibitors. Cell Death Dis. 2019;10:128. The mechanisms of NLRP3 inflammasome activation and potential avenues for therapeutic intervention are discussed.
Harmon A, Cornelius D, Amaral L, Faulkner J, Cunningham M Jr, Wallace K, et al. The role of inflammation in the pathophysiology of preeclampsia. Clin Sci. 2016;130(6):409–19.
Armistead B, Kadam L, Drewlo S, Kohan-Ghadr H. The role of NFKB in health and preeclamptic placenta: trophoblasts in the spotlight. Int J Mol Sci. 2020;21(5):1775.
Mulla MJ, Myrtolli K, Potter J, Boeras C, Kavathas PB, Sfakianaki AK, et al. Uric acid induces trophoblast IL-1beta production via the inflammasome: implications for the pathogenesis of preeclampsia. Am J Reprod Immunol. 2011;65(6):542–8. https://doi.org/10.1111/j.1600-0897.2010.00960.x.
Cheng S, Nakashima A, Huber W, Davis S, Banerjee S, Huang Z, et al. Pyroptosis is a critical inflammatory pathway in the placenta from early onset preeclampsia and in human trophoblasts exposed to hypoxia and endoplasmic reticulum stressors. Cell Death Dis. 2019;10(12):927.
Matias ML, Romao M, Weel IC, Ribeiro VR, Nunes PR, Borges VT, et al. Endogenous and uric acid-induced activation of NLRP3 inflammasome in pregnant women with preeclampsia. PLoS ONE. 2015;10(6): e0129095. https://doi.org/10.1371/journal.pone.0129095.
Silva GB, Gierman LM, Rakner JJ, Stodle GS, Mundal SB, Thaning AJ, et al. Cholesterol crystals and NLRP3 mediated inflammation in the uterine wall decidua in normal and preeclamptic pregnancies. Front Immunol. 2020;11: 564712. https://doi.org/10.3389/fimmu.2020.564712.
Stodle GS, Silva GB, Tangeras LH, Gierman LM, Nervik I, Dahlberg UE, et al. Placental inflammation in pre-eclampsia by Nod-like receptor protein (NLRP)3 inflammasome activation in trophoblasts. Clin Exp Immunol. 2018;193(1):84–94. https://doi.org/10.1111/cei.13130.
Ozeki A, Oogaki Y, Henmi Y, Karasawa T, Takahashi M, Takahashi H, et al. Elevated S100A9 in preeclampsia induces soluble endoglin and IL-1B secretion and hypertension via the NLRP3 inflammasome. J Hypertension. 2021. https://doi.org/10.1097/HJH.0000000000002981.
Wallace K, Harris S, Addison A, Bean C. HELLP syndrome: pathophysiology and current therapies. Curr Pharm Biotechnol. 2018;19(10):816–26.
Erdei J, Toth A, Balogh E, Nyakundi B, Banyai E, Ryffel B, et al. Induction of NLRP3 inflammasome activation by heme in endothelial cells. Oxid Med Cell Longev. 2018;2018:4310816.
Prusac I, Zekic T, Roje D. Apoptosis, proliferation and Fas ligand expression in placental trophoblast from pregnancies complicated by HELLP syndrome for pre-eclampsia. Acta Obstetricia Gynecologica Scandinavica. 2011;90(10):1157–63.
Bertheloot D, Latz E, Franklin B. Necroptosis, pyroptosis and apoptosis: an intricate game of cell death. Cell Mol Immunol. 2021;18(5):1106–21.
Cornelius D, Amaral L, Harmon A, Wallace K, Thomas A, Campbell N, et al. An increased population of regulatory T cells improves the pathophysiology of placental ischemia in a rat model of preeclampsia. Am J Physiol Regul Integr Comp Physiol. 2015;309(8):R884–91.
Li Z, Wang L, Liu H, Muyayalo K, Huang X, Mor G, et al. Galectin-9 alleviates LPS-induced preeclampsia-like impairment in rats via switching decidual macrophage polarization to M2 Subtype. Front Immunol. 2019;9:3142.
Taylor E, George E, Ryan M, Garrett M, Sasser J. Immunological comparison of pregnant Dahl salt-sensitive and Sprague-Dawley rats commonly used to model characteristics of preeclampsia. Am J Physiol Regul Integr Comp Physiol. 2021;321(2):R125–38.
Zeng H, Han X, Zhu Z, Yu S, Mei S, Cheng X, et al. Increased uterine NLRP3 inflammasome and leucocyte infiltration in a rat model of preeclampsia. Am J Reprod Immunol. 2021. https://doi.org/10.1111/aji.13493.
Travis O, White D, Pierce W, Ge Y, Stubbs C, Spradley F, et al. Chronic infusion of interleukin-17 promotes hypertension, activation of cytolytic natural killer cells, and vascular dysfunction in pregnant rats. Physiol Rep. 2019;7(7):14038.
Cornelius D, Amaral L, Wallace K, Campbell N, Thomas A, Scott J, et al. Reduced uterine perfusion pressure T-helper 17 cells cause pathophysiology associated with preeclampsia during pregnancy. Am J Physiol Regul Integr Comp Physiol. 2016;311(6):R1192–9.
Chang G, Yang X, Liu W, Lin S, Yang S, Zhao M. FABP4 facilitates inflammasome activation to induce the Treg/Th17 imbalance in preeclampsia via forming a positive feedback with IL-17A. Mol Ther Nucleic Acids. 2021;24:743–54.
Jayaram A, Collier C, Martin J Jr. Preterm parturition and pre-eclampsia: the confluence of two great gestational syndromes. Int J Gynaecol Obstet. 2020;150(1):10–6.
Shinar S, Melamed N, Abdulaziz K, Ray J, Riddell C, Barrett J, et al. Changes in rate of preterm birth and adverse pregnancy outcomes attributed to preeclampsia after introduction of a refined definition of preeclampsia: a population-based study. Acta Obstet Gynecol Scand. 2021. https://doi.org/10.1111/aogs.14199.
Gomez-Lopez N, Romero R, Xu Y, Plazyo O, Unkel R, Leng Y, et al. A role for the inflammasome in spontaneous preterm labor with acute histologic chorioamnionitis. Reprod Sci. 2017;24(10):1382–401. https://doi.org/10.1177/1933719116687656.
Plazyo O, Romero R, Unkel R, Balancio A, Mial TN, Xu Y, et al. HMGB1 Induces an inflammatory response in the chorioamniotic membranes that is partially mediated by the inflammasome. Biol Reprod. 2016;95(6):130. https://doi.org/10.1095/biolreprod.116.144139.
Romero R, Chaiworapongsa T, Alpay Savasan Z, Xu Y, Hussein Y, Dong Z, et al. Damage-associated molecular patterns (DAMPs) in preterm labor with intact membranes and preterm PROM: a study of the alarmin HMGB1. J Matern Fetal Neonatal Med. 2011;24(12):1444–55. https://doi.org/10.3109/14767058.2011.591460.
Wang Z, Zhang S, Xiao Y, Zhang W, Wu S, Qin T, et al. NLRP3 Inflammasome and inflammatory diseases. Oxid Med Cell Longev. 2020;2020:4063562. https://doi.org/10.1155/2020/4063562.
•• Vora S, Lieberman J, Wu H. Inflammasome activation at the crux of severe COVID-19A. Nat Rev Immunol. 2021:1–10. https://doi.org/10.1038/s41577-021-00588-x. This review provides insight into the role of inflammasomes in severe COVID-19.
Rodrigues TS, de Sá KSG, Ishimoto AY, Becerra A, Oliveira S, Almeida L, et al. Inflammasomes are activated in response to SARS-CoV-2 infection and are associated with COVID-19 severity in patients. J Exp Med. 2021;218(3). https://doi.org/10.1084/jem.20201707.
Nieto-Torres J, Verdia-Baguena C, Jimenez-Guardeno J, Regla-Nava J, Castano-Rodriquez C, Fernandez-Delgado R, et al. Severe acute respiratory syndrome and coronavirus E protein transports calcium ions and activates the NLRP3 inflammasome. Virology. 2015;485:330–9.
Chen I, Moriyama M, Chang M, Ichinohe T. Severe acute respiratory syndrome coronavirus viroporin 3A activates the NLRP3 Inflammasome. Front Microbiol. 2019;10:50.
Pan P, Shen M, Yu Z, Ge W, Chen K, Tian M, et al. SARS-CoV-2 N protein promotes NLRP3 inflammasome activation to induce hyperinflammation. Nat Commun. 2021;12(1):4664. https://doi.org/10.1038/s41467-021-25015-6.
Surjit M, Lal S. The nucleocapsid protein of the SARS coronavirus: structure, function and therapeutic potential. Molecular Biology of the SARS-Coronavirus. 2009.
Latz E, Duewell P. NLRP3 inflammasome activation in inflammaging. Semin Immunol. 2018;40:61–73.
van den Berg D, Velde A. Severe COVID-19: NLRP3 inflammasome. Front Immunol. 2020;11:1580.
• Conde-Agudelo A, Romero R. SARS-COV-2 infection during pregnancy and risk of preeclampsia: a systematic review and meta-analysis. Am J Obstet Gynecol. 2021. https://doi.org/10.1016/j.ajog.2021.07.009. This systematic review and meta-analysis surveyed all recent COVID-19 and pregnancy studies to find an association between PreE and COVID-19.
Kiprono L, Wallace K, Moseley J, Martin J Jr, Lamarca B. Progesterone blunts vascular endothelial cell secretion of endothelin-1 in response to placental ischemia. Am J Obstet Gynecol. 2013;209(1):44.e1-6.
Man S, Kanneganti T. Converging roles of caspases in inflammasome activation, cell death and innate immunity. Nat Rev Immunol. 2016;16:7–21.
Liu Z, Zhao X, Shan H, Gao H, Wang P. microRNA-520c-3p suppresses NLRP3 inflammasome activation and inflammatory cascade in preeclampsia by downregulating NLRP3. Inflamm Res. 2019;68(8):643–54. https://doi.org/10.1007/s00011-019-01246-8.
Park S, Shin J, Bae J, Han D, Park SR, Shin J, et al. SIRT1 Alleviates LPS-Induced IL-1beta Production by Suppressing NLRP3 Inflammasome Activation and ROS Production in Trophoblasts. Cells. 2020;9(3). https://doi.org/10.3390/cells9030728.
Zhao X, Zhang X, Wu Z, Mei J, Li L, Wang Y. Up-regulation of microRNA-135 or silencing of PCSK6 attenuates inflammatory response in preeclampsia by restricting NLRP3 inflammasome. Mol Med. 2021;27(1):82. https://doi.org/10.1186/s10020-021-00335-x.
Wolfe K, Synder C, Gisslen T, Kemp M, Newnham J, Kramer B, et al. Modulation of lipopolysaccharide-induced chorioamnionitis in fetal sheep by maternal betamethasone. Reprod Sci. 2013;20(12):1447–54.
Gil-Villa A, Alvarez A, Velasquez-Berrio M, Rojas-Lopez M, Cadavid A. Role of aspirin-triggered lipoxin A4, aspirin and salicylic acid in the modulation of the oxidative and inflammatory responses induced by plasma from women with pre-eclampsia. Am J Reprod Immunol. 2020;83(2): e13207.
Chang Y, Kao M, Lin J, Chen T, Cheng C, Wong C, et al. Effects of MgSO4 on inhibiting Nod-like receptor protein 3 inflammasome involve decreasing intracellular calcium. J Surg Res. 2018;221:257–65.
Amash A, Holcberg G, Sapir O, Huleihel M. Placental secretion of interleukin-1 and interleukin-1 receptor antagonist in preeclampsia: effect of magnesium sulfate. J Interferon Cytokine Res. 2012;32:432–41.
Acknowledgements
Thank you to Lorena Amaral, PhD for conducting the HUVEC assays.
Funding
Research supported in this publication was supported in part by the National Institutes of Health (NIH) under Award Numbers R01HL151407 to DCC, T32HL105324 to AG, and P20GM121334 and R01MH116027 to KW.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Denise C. Cornelius, Xi Wang, Ashley Griffin, Rachael Morris, and Kedra Wallace declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with animal subjects performed by any of the authors. Human samples were collected after informed consent was signed and women were enrolled in an Institutional Review Board approved study 2020–0134 (COVID + patients) and 2014–0256 (COVID − patients).
Disclaimer
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Preeclampsia
Rights and permissions
About this article
Cite this article
Cornelius, D.C., Wang, X., Griffin, A. et al. Preeclampsia and COVID-19: the Role of Inflammasome Activation. Curr Hypertens Rep 24, 341–348 (2022). https://doi.org/10.1007/s11906-022-01195-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11906-022-01195-4