Abstract
Introduction
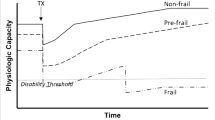
Frailty is a clinical syndrome characterized by a decrease in strength, resistance and body physiological condition, making the individual more vulnerable, and increasing his/her risk of dependence and death. Kidney transplant (KT) is currently the best end-stage renal disease therapeutic alternative for certain individuals. Frailty status occurs in approximately 20% of KT patients. Thus, it was evaluated if there would be any change in frailty status level in a population of adult patients on chronic HD after receiving KT.
Material and method
A cross-sectional study was conducted on a population of adult hemodialysis patients (n: 57), with the objective of evaluating if there was a significant change in their clinical frailty score (CFS) after 6 months of KT. For the statistical analysis, the Student’s t-test, and the test of statistical significance between two proportions were applied.
Results
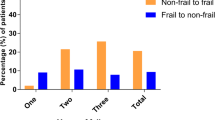
Mean CFS before KT was 4 (vulnerable), and after KT was 3 (robust). CFS value was significantly lower after KT (p value < 0.01).
Conclusion
A significant improvement was found between pre- and post-transplant clinical frailty scores in hemodialysis adult patients.
Similar content being viewed by others
References
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al (2010) Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 39(4):412–423. https://doi.org/10.1093/ageing/afq034
Johansen KL, Delgado C, Bao Y, Tamura MK (2013) Frailty and dialysis initiation. Semin Dial 26(6):690–696. https://doi.org/10.1111/sdi.12126
Aiello F, Dueñas E, Musso C (2017) Senescent nephropathy: the new renal syndrome. Healthcare 5(4):81. https://doi.org/10.3390/healthcare5040081
Musso CG, Jauregui JR, Macías Núñez JF (2015) Frailty phenotype and chronic kidney disease: a review of the literature. Int Urol Nephrol 47(11):1801–1807. https://doi.org/10.1007/s11255-015-1112-z
Yamamoto S, Matsuzawa R, Kamitani T et al (2020) Efficacy of exercise therapy initiated in the early phase after kidney transplantation: a pilot study. J Ren Nutr 30(6):518–525
García-García FJ, Carcaillon L, Fernandez-Tresguerres J et al (2014) A new operational definition of frailty: the frailty trait scale. J Am Med Dir Assoc 15(5):371.e7-371.e13. https://doi.org/10.1016/j.jamda.2014.01.004
Rockwood K, Andrew M, Mitnitski A (2007) A comparison of two approaches to measuring frailty in elderly people. J Gerontol A Biol Sci Med Sci 62(7):738–743. http://www.ncbi.nlm.nih.gov/pubmed/17634321
Huamán CL, Postigo OC, Contreras CC (2016) Epidemiological characteristics of patients starting chronic hemodialysis at Alberto Sabogal Sologuren Hospital 2015. Horiz Médico 16:6–12
Santamaría-olmo R, Gorostidi-pérez M (2013) Blood pressure and progression of chronic kidney disease. NefroPlus 5(1):4–11. https://doi.org/10.3265/NefroPlus.pre2013.May.12105
Candelaria-Brito JC, Gutiérrez-Gutiérrez C, Bayarre-Vea HD et al (2018) Characterization of chronic kidney disease in older adults. Rev Colomb Nefrol 5(2):166–178. https://doi.org/10.22265/acnef.0.0.308
Kehler DS, Ferguson T, Stammers AN et al (2017) Prevalence of frailty in Canadians 18 – 79 years old in the Canadian Health Measures Survey. BMC Geriatr. 1–8. https://doi.org/10.1186/s12877-017-0423-6
Capotondo M, Musso CG (2019) Nephroprevention in the elderly. In Musso CG, Jauregui J, Macías-Núñez JF, Covic A (Eds.) Clinical Nephrogeriatrics. Cham Springer pp. 133–146
McAdams-DeMarco MA, King EA, Luo X et al (2016) Frailty, length of stay, and mortality in kidney transplant recipients. A National Registry and Prospective Cohort Study. Ann Surg 20(20):1–7
Chu NM, Gross AL, Shaffer AA et al (2019) Frailty and changes in cognitive function after kidney transplantation. J Am Soc Nephrol 30(2):336–345
Quint EE, Schopmeyer L, Banning LBD et al (2020) Transitions in frailty state after kidney transplantation. Langenbeck’s Arch Surg 405(6):845–850. https://doi.org/10.1007/s00423-020-01936-6
McAdams-DeMarco M, Ying H, Olorundare I et al (2017) Individual frailty components and mortality in kidney transplant recipients. Transplantation 101(9):2126–2132
Alfieri C, Malvica S, Cesari M et al (2022) Frailty in kidney transplantation: a review on its evaluation, variation and long-term impact. Clin Kidney J 15(11):2020–2026. https://doi.org/10.1093/ckj/sfac149
Haugen CE, Chu NM, Ying H et al (2019) Frailty and access to kidney transplantation. Clin J Am Soc Nephrol 14(4):576–582. https://doi.org/10.2215/CJN.12921118
Lorenzo-López L, López-López R, Maseda A et al (2019) Changes in frailty status in a community-dwelling cohort of older adults: the VERISAÚDE study. Maturitas 119:54–60
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from the patient.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
If dementia, the degree of frailty usually corresponds to the degree of dementia.
-
Mild dementia: includes forgetting the details of recent events though still remembering the event itself, repeating the same question/story and social withdrawal
-
Moderate dementia: recent memory is very impaired, even though they seemingly can remember their past life events well. They can do personal care with prompting
-
Severe dementia: they cannot do personal care without help
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Aroca-Martinez, G., Hernandez-Agudelo, S., Castro-Hernández, C. et al. Frailty status improvement after kidney transplantation. Ir J Med Sci 192, 2501–2505 (2023). https://doi.org/10.1007/s11845-022-03264-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-022-03264-8