Abstract
Purpose
To identify trajectories of depressive symptoms in older breast cancer survivors and demographic, psychosocial, physical health, and cancer-related predictors of these trajectories.
Methods
Recently diagnosed nonmetastatic breast cancer survivors (n = 272), ages 60–98 years, were evaluated for depressive symptoms (Center for Epidemiological Studies Depression Scale, CES-D; scores ≥16 suggestive of clinically significant depressive symptoms). CES-D scores were analyzed in growth-mixture models to determine depression trajectories from baseline (post-surgery, pre-systemic therapy) through 3-year annual follow-up. Multivariable, multinomial logistic regression was used to identify baseline predictors of depression trajectories.
Results
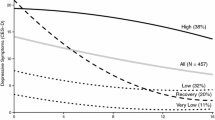
Survivors had three distinct trajectories: stable (84.6%), emerging depressive symptoms (10.3%), and recovery from high depressive symptoms at baseline that improved slowly over time (5.1%). Compared to stable survivors, those in the emerging (OR = 1.16; 95% CI = 1.08–1.23) or recovery (OR = 1.26; 95% CI = 1.15–1.38) groups reported greater baseline anxiety. Greater baseline deficit accumulation (frailty composite measure) was associated with emerging depressive symptoms (OR = 3.71; 95% CI = 1.90–7.26). Less social support at baseline (OR = 0.38; 95% CI = 0.15–0.99), but greater improvement in emotional (F = 4.13; p = 0.0006) and tangible (F = 2.86; p = 0.01) social support over time, was associated with recovery from depressive symptoms.
Conclusions
Fifteen percent of older breast cancer survivors experienced emerging or recovery depressive symptom trajectories. Baseline anxiety, deficit accumulation, and lower social support were associated with worse outcomes.
Implications for Cancer Survivors
Our results emphasize the importance of depression screening throughout the course of cancer care to facilitate early intervention. Factors associated with depressive symptoms, including lower levels of social support proximal to diagnosis, could serve as intervention levers.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Pilevarzadeh M, Amirshahi M, Afsargharehbagh R, Rafiemanesh H, Hashemi SM, Balouchi A. Global prevalence of depression among breast cancer patients: a systematic review and meta-analysis. Breast Cancer Res Treat. 2019;176:519–33.
Mitchell AJ, Chan M, Bhatti H, Halton M, Grassi L, Johansen C, et al. Prevalence of depression, anxiety, and adjustment disorder in oncological, haematological, and palliative-care settings: a meta-analysis of 94 interview-based studies. Lancet Oncol. 2011;12:160–74.
Krebber AMH, Buffart LM, Kleijn G, Riepma IC, De Bree R, Leemans CR, et al. Prevalence of depression in cancer patients: a meta-analysis of diagnostic interviews and self-report instruments. Psychooncology. 2014;23:121–30.
Burgess C, Cornelius V, Love S, Graham J, Richards M, Ramirez A. Depression and anxiety in women with early breast cancer: five year observational cohort study. Br Med J. 2005;330:702.
Colleoni M, Mandala M, Peruzzotti G, Robertson C, Bredart A, Goldhirsch A. Depression and degree of acceptance of adjuvant cytotoxic drugs. Lancet. 2000;356:1326–7.
Nyrop KA, Deal AM, Shachar SS, Basch E, Reeve BB, Choi SK, et al. Patient-reported toxicities during chemotherapy regimens in current clinical practice for early breast cancer. Oncologist. 2019;24:762–71.
Satin JR, Linden W, Phillips MJ. Depression as a predictor of disease progression and mortality in cancer patients: A meta-analysis. Cancer. 2009;115:5349–61.
Wang X, Wang N, Zhong L, Wang S, Zheng Y, Yang B, et al. Prognostic value of depression and anxiety on breast cancer recurrence and mortality: a systematic review and meta-analysis of 282,203 patients. Mol Psychiatry. 2020;25:3186–97.
Clough-Gorr KM, Ganz PA, Silliman RA. Older breast cancer survivors: factors associated with change in emotional well-being. J Clin Oncol. 2007;25:1334–40.
Taira N, Shimozuma K, Shiroiwa T, Ohsumi S, Kuroi K, Saji S, et al. Associations among baseline variables, treatment-related factors and health-related quality of life 2 years after breast cancer surgery. Breast Cancer Res Treat. 2011;128:735–47.
Avis NE, Levine BJ, Case LD, Naftalis EZ, Van Zee KJ. Trajectories of depressive symptoms following breast cancer diagnosis. Cancer Epidemiol Biomark Prev. 2015;24:1789–95.
Charles C, Bardet A, Larive A, Gorwood P, Ramoz N, Thomas E, et al. Characterization of depressive symptoms trajectories after breast cancer diagnosis in women in France. JAMA Netw Open. 2022;5:e225118.
Brandão T, Schulz MS, Matos PM. Psychological adjustment after breast cancer: a systematic review of longitudinal studies. Psychooncology. 2017;26:917–26.
Nakamura ZM, Deal AM, Nyrop KA, Chen YT, Quillen LJ, Brenizer T, et al. Serial assessment of depression and anxiety by patients and providers in women receiving chemotherapy for early breast cancer. Oncologist. 2021;26:147–56.
So WKW, Marsh G, Ling WM, Leung FY, Lo JCK, Yeung M, et al. Anxiety, depression and quality of life among Chinese breast cancer patients during adjuvant therapy. Eur J Oncol Nurs. 2010;14:17–22.
Andersen BL, DeRubeis RJ, Berman BS, Gruman J, Champion VL, Massie MJ, et al. Screening, assessment, and care of anxiety and depressive symptoms in adults with cancer: an American Society of Clinical Oncology guideline adaptation. J Clin Oncol. 2014;32:1605–19.
Nakamura ZM, Damone EM, Herrick HP, Nyrop KA, Deal AM, Brenizer AT, et al. Anticipating mental health needs after chemotherapy in early-stage breast cancer using patient-reported symptom screening. Support Care Cancer. 2022;30:3933–41.
Bluethmann SM, Mariotto AB, Rowland JH. Anticipating the “Silver Tsunami”: prevalence trajectories and co-morbidity burden among older cancer survivors in the United States. Cancer Epidemiol Biomark Prev. 2016;25:1029–36.
Miller KD, Nogueira L, Devasia T, Mariotto AB, Yabroff KR, Jemal A, et al. Cancer treatment and survivorship statistics, 2022. CA Cancer J Clin. 2022;72:409–36.
Dunn LB, Cooper BA, Neuhaus J, West C, Paul S, Aouizerat B, et al. Identification of distinct depressive symptom trajectories in women following surgery for breast cancer. Health Psychol. 2011;30:683.
Dunn LB, Aouizerat BE, Langford DJ, Cooper BA, Dhruva A, Cataldo JK, et al. Cytokine gene variation is associated with depressive symptom trajectories in oncology patients and family caregivers. Eur J Oncol Nurs. 2013;17:346–53.
Bidstrup PE, Christensen J, Mertz BG, Rottmann N, Dalton SO, Johansen C. Trajectories of distress, anxiety, and depression among women with breast cancer: looking beyond the mean. Acta Oncol (Madr). 2015;54:789–96.
Stanton AL, Wiley JF, Krull JL, Crespi CM, Hammen C, Allen JJB, et al. Depressive episodes, symptoms, and trajectories in women recently diagnosed with breast cancer. Breast Cancer Res Treat. 2015;154:105–15.
Nelson CJ, Cho C, Berk AR, Holland J, Roth AJ. Are gold standard depression measures appropriate for use in geriatric cancer patients? A systematic evaluation of self-report depression instruments used with geriatric, cancer, and geriatric cancer samples. J Clin Oncol. 2010;28:348.
Cataldo JK, Paul S, Cooper B, Skerman H, Alexander K, Aouizerat B, et al. Differences in the symptom experience of older versus younger oncology outpatients: a cross-sectional study. BMC Cancer. 2013;13:1–16.
Kurtz M, Kurtz J, Stommel M, Given C, Given B. Predictors of depressive symptomatology of geriatric patients with colorectal cancer: a longitudinal view. Support Care Cancer. 2002;10:494–501.
Aarts JWF, Deckx L, van Abbema DL, Tjan-Heijnen VCG, van den Akker M, Buntinx F. The relation between depression, coping and health locus of control: differences between older and younger patients, with and without cancer. Psychooncology. 2015;24:950–7.
Duc S, Rainfray M, Soubeyran P, Fonck M, Blanc JF, Ceccaldi J, et al. Predictive factors of depressive symptoms of elderly patients with cancer receiving first-line chemotherapy. Psychooncology. 2017;26:15–21.
Hurria A, Li D, Hansen K, Patil S, Gupta R, Nelson C, et al. Distress in older patients with cancer. J Clin Oncol. 2009;27:4346.
Cohen M. Depression, anxiety, and somatic symptoms in older cancer patients: a comparison across age groups. Psychooncology. 2014;23:151–7.
Thomé B, Hallberg IR. Quality of life in older people with cancer–a gender perspective. Eur J Cancer Care (Engl). 2004;13:454–63.
Weiss Wiesel TR, Nelson CJ, Tew WP, Hardt M, Mohile SG, Owusu C, et al. The relationship between age, anxiety, and depression in older adults with cancer. Psychooncology. 2015;24:712–7.
Erlangsen A, Stenager E, Conwell Y. Physical diseases as predictors of suicide in older adults: a nationwide, register-based cohort study. Soc Psychiatry Psychiatr Epidemiol. 2015;50:1427–39.
Misono S, Weiss NS, Fann JR, Redman M, Yueh B. Incidence of suicide in persons with cancer. J Clin Oncol. 2008;26:4731.
Mandelblatt JS, Small BJ, Luta G, Hurria A, Jim H, McDonald BC, et al. Cancer-related cognitive outcomes among older breast cancer survivors in the Thinking and Living With Cancer Study. J Clin Oncol. 2018;36:JCO1800140.
Radloff LS. The CES-D scale: A self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1:385–401.
Vilagut G, Forero CG, Barbaglia G, Alonso J. Screening for depression in the general population with the Center for Epidemiologic Studies Depression (CES-D): a systematic review with meta-analysis. PLoS One. 2016;11:e0155431.
Stafford L, Judd F, Gibson P, Komiti A, Quinn M, Mann GB. Comparison of the Hospital Anxiety and Depression Scale and the Center for Epidemiological Studies Depression Scale for detecting depression in women with breast or gynecologic cancer. Gen Hosp Psychiatry. 2014;36:74–80.
Spielberger CD. State-trait anxiety inventory for adults. 1983;
Carroll JE, Small BJ, Tometich DB, Zhai W, Zhou X, Luta G, et al. Sleep disturbance and neurocognitive outcomes in older patients with breast cancer: interaction with genotype. Cancer. 2019;125:4516–24.
Stewart A, Ware J, editors. Measuring functioning and well-being: the Medical Outcomes Study approach. Durham, NC: Duke University Press; 1992.
Hurria A, Gupta S, Zauderer M, Zuckerman EL, Cohen HJ, Muss H, et al. Developing a cancer-specific geriatric assessment. Cancer. 2005;104:1998–2005.
Cella DF, Tulsky DS, Gray G, Sarafian B, Linn E, Bonomi A, et al. The Functional Assessment of Cancer Therapy scale: development and validation of the general measure. J Clin Oncol. 1993;11:570–9.
Jenkinson C, Layte R, Jenkinson D, Lawrence K, Petersen S, Paice C, et al. A shorter form health survey: can the SF-12 replicate results from the SF-36 in longitudinal studies? J Public Health (Bangkok). 1997;19:179–86.
Cohen HJ, Smith D, Sun C, Tew W, Mohile SG, Owusu C, et al. Frailty as determined by a comprehensive geriatric assessment-derived deficit-accumulation index in older patients with cancer who receive chemotherapy. Cancer. 2016;122:3865–72.
Guida JL, Ahles TA, Belsky D, Campisi J, Cohen HJ, DeGregori J, et al. Measuring aging and identifying aging phenotypes in cancer survivors. J Natl Cancer Inst. 2019;111:1245–54.
Mitnitski A, Rockwood K. Aging as a process of deficit accumulation: its utility and origin. Interdiscip Top Gerontol. 2015;40:85–98.
Ram N, Grimm KJ. Methods and measures: Growth mixture modeling: a method for identifying differences in longitudinal change among unobserved groups. Int J Behav Dev. 2009;33:565–76.
Grimm KJ, Ram N, Estabrook R. Growth modeling: structural equation and multilevel modeling approaches. Guilford Publications; 2016.
Searle SD, Mitnitski A, Gahbauer EA, Gill TM, Rockwood K. A standard procedure for creating a frailty index. BMC Geriatr. 2008;8:1–10.
Sjöberg L, Karlsson B, Atti A-R, Skoog I, Fratiglioni L, Wang H-X. Prevalence of depression: comparisons of different depression definitions in population-based samples of older adults. J Affect Disord. 2017;221:123–31.
Mohebbi M, Agustini B, Woods RL, McNeil JJ, Nelson MR, Shah RC, et al. Prevalence of depressive symptoms and its associated factors among healthy community-dwelling older adults living in Australia and the United States. Int J Geriatr Psychiatry. 2019;34:1208–16.
Champion VL, Wagner LI, Monahan PO, Daggy J, Smith L, Cohee A, et al. Comparison of younger and older breast cancer survivors and age-matched controls on specific and overall quality of life domains. Cancer. 2014;120:2237–46.
Götze H, Friedrich M, Taubenheim S, Dietz A, Lordick F, Mehnert A. Depression and anxiety in long-term survivors 5 and 10 years after cancer diagnosis. Support Care Cancer. 2020;28:211–20.
Kuswanto CN, Stafford L, Sharp J, Schofield P. Psychological distress, role, and identity changes in mothers following a diagnosis of cancer: a systematic review. Psychooncology. 2018;27:2700–8.
Tiedtke C, de Rijk A, Dierckx de Casterlé B, Christiaens M, Donceel P. Experiences and concerns about ‘returning to work’for women breast cancer survivors: a literature review. Psychooncology. 2010;19:677–83.
Crowley SA, Foley SM, Wittmann D, Jagielski CH, Dunn RL, Clark PM, et al. Sexual health concerns among cancer survivors: testing a novel information-need measure among breast and prostate cancer patients. J Cancer Educ. 2016;31:588–94.
Gorman JR, Su HI, Roberts SC, Dominick SA, Malcarne VL. Experiencing reproductive concerns as a female cancer survivor is associated with depression. Cancer. 2015;121:935–42.
Avis NE, Levine B, Naughton MJ, Case DL, Naftalis E, Van Zee KJ. Explaining age-related differences in depression following breast cancer diagnosis and treatment. Breast Cancer Res Treat. 2012;136:581–91.
Hannum SM, Clegg Smith K, Coa K, Klassen AC. Identity reconstruction among older cancer survivors: age and meaning in the context of a life-altering illness. J Psychosoc Oncol. 2016;34:477–92.
Huang G, Wu Y, Zhang G, Zhang P, Gao J. Analysis of the psychological conditions and related factors of breast cancer patients. Chinese-German J Clin Oncol. 2010;9:53–7.
Weyerer S, Eifflaender-Gorfer S, Köhler L, Jessen F, Maier W, Fuchs A, et al. Prevalence and risk factors for depression in non-demented primary care attenders aged 75 years and older. J Affect Disord. 2008;111:153–63.
Oerlemans S, Issa DE, van den Broek EC, Nijziel MR, Coebergh JW, Mols F, et al. Impact of therapy and disease-related symptoms on health-related quality of life in patients with follicular lymphoma: results of the population-based PHAROS-registry. Eur J Haematol. 2014;93:229–38.
Perkins EA, Small BJ, Balducci L, Extermann M, Robb C, Haley WE. Individual differences in well-being in older breast cancer survivors. Crit Rev Oncol Hematol. 2007;62:74–83.
Nelson CJ, Weinberger MI, Balk E, Holland J, Breitbart W, Roth AJ. The chronology of distress, anxiety, and depression in older prostate cancer patients. Oncologist. 2009;14:891–9.
Weinberger MI, Roth AJ, Nelson CJ. Untangling the complexities of depression diagnosis in older cancer patients. Oncologist. 2009;14:60–6.
Magnuson A, Sattar S, Nightingale G, Saracino R, Skonecki E, Trevino KM. A practical guide to geriatric syndromes in older adults with cancer: a focus on falls, cognition, polypharmacy, and depression. Am Soc Clin Oncol Educ Book. 2019;39:e96–109.
Saracino RM, Weinberger MI, Roth AJ, Hurria A, Nelson CJ. Assessing depression in a geriatric cancer population. Psychooncology. 2017;26:1484–90.
Mandelblatt JS, Cai L, Luta G, Kimmick G, Clapp J, Isaacs C, et al. Frailty and long-term mortality of older breast cancer patients: CALGB 369901 (Alliance). Breast Cancer Res Treat. 2017;164:107–17.
Williams GR, Deal AM, Sanoff HK, Nyrop KA, Guerard EJ, Pergolotti M, et al. Frailty and health-related quality of life in older women with breast cancer. Support Care Cancer. 2019;27:2693–8.
Wildiers H, Heeren P, Puts M, Topinkova E, Janssen-Heijnen MLG, Extermann M, et al. International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer. J Clin Oncol. 2014;32:2595.
Morley JE, Vellas B, Van Kan GA, Anker SD, Bauer JM, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14:392–7.
Mandelblatt JS, Zhou X, Small BJ, Ahn J, Zhai W, Ahles T, et al. Deficit accumulation frailty trajectories of older breast cancer survivors and non-cancer controls: the thinking and living with cancer study. J Natl Cancer Inst. 2021;113:1053–64.
Ahles TA, Schofield E, Li Y, Ryan E, Root JC, Patel SK, et al. Relationship between cognitive functioning and frailty in older breast cancer survivors. J Geriatr Oncol. 2022;13:27–32.
Hann DM, Oxman TE, Ahles TA, Furstenberg CT, Stuke TA. Social support adequacy and depression in older patients with metastatic cancer. Psychooncology. 1995;4:213–21.
Chochinov HM. Depression in cancer patients. Lancet Oncol. 2001;2:499–505.
Goldzweig G, Baider L, Andritsch E, Rottenberg Y. Hope and social support in elderly patients with cancer and their partners: an actor–partner interdependence model. Future Oncol. 2016;12:2801–9.
Courtens AM, Stevens FCJ, Crebolder H, Philipsen H. Longitudinal study on quality of life and social support in cancer patients. Cancer Nurs. 1996;19:162–9.
Rizalar S, Ozbas A, Akyolcu N, Gungor B. Effect of perceived social support on psychosocial adjustment of Turkish patients with breast cancer. Asian Pac J Cancer Prev. 2014;15:3429–34.
Cicero V, Lo Coco G, Gullo S, Lo VG. The role of attachment dimensions and perceived social support in predicting adjustment to cancer. Psycho-Oncology: Journal of the Psychological, Social and Behavioral Dimensions of. Cancer. 2009;18:1045–52.
Alfano CM, Day JM, Katz ML, Herndon JE, Bittoni MA, Oliveri JM, et al. Exercise and dietary change after diagnosis and cancer-related symptoms in long-term survivors of breast cancer: CALGB 79804. Psycho-Oncology: Journal of the Psychological, Social and Behavioral Dimensions of. Cancer. 2009;18:128–33.
Kornblith AB, Dowell JM, Herndon JE, Engelman BJ, Bauer-Wu S, Small EJ, et al. Telephone monitoring of distress in patients aged 65 years or older with advanced stage cancer: a cancer and leukemia group B study. Cancer: Interdisciplinary International Journal of the American Cancer. Society. 2006;107:2706–14.
Acknowledgements
We would like to thank the participants in the Thinking and Living With Cancer (TLC) study for the sharing of their time and experiences; without their generosity, this study would not have been possible. We are also indebted to Sherri Stahl, Naomi Greenwood, Margery London, and Sue Winarsky, patient advocates from the Georgetown Breast Cancer Advocates, for their insights and suggestions on study design and methods to recruit and retain participants. We thank the TLC staff who contributed by ascertaining, enrolling, and participants.
Funding
This research was supported by the National Cancer Institute of the National Institutes of Health via grants R01CA129769, R35CA197289, and R35CA283926 (J.S.M.). This study was also supported in part by the National Institutes of Health via grant P30CA51008 to the Georgetown Lombardi Comprehensive Cancer Center for support of the Biostatistics and Bioinformatics Resource and the Non-Therapeutic Shared Resource, grants R56AG068086 (J.E.C. and J.S.M.), R01AG068193 (J.S.M. and A.J.S.), R01CA237535 (J.E.C.), K01AG065485 (K.E.R.), P30AG028716 (H.J.C.), K01CA212056 (T.N.B.), K08CA241337 (K.V.D.), R01CA172119 (T.A.A. and J.C.R.), U54CA137788 and P30CA008748 (T.A.A.), K99CA270294 (D.B.T.), R01CA244673 (B.C.M.), P30AG010133 and P30AG072976 (A.J.S.), and R01CA261793 (S.K.P.), T32AG000029 (A.L.A), and grants to the UCLA Cousins Center for Psychoneuroimmunology (J.E.C.).
Author information
Authors and Affiliations
Contributions
Zev M. Nakamura: conceptualization, investigation, writing, and editing. Brent J. Small: Supervision, methodology, formal analysis, data curation, and writing. Wanting Zhai: formal analysis, data curation, and writing. Ashley L. Artese: investigation, writing, and editing. Tim A. Ahles: conceptualization, investigation, resources, writing, project administration, and funding acquisition. Jaeil Ahn: supervision, methodology, formal analysis, data curation, and writing. Traci N. Bethea: investigation, writing, and editing. Elizabeth C. Breen: investigation, writing, and editing. Harvey J. Cohen: conceptualization, writing, and editing. Martine Extermann: investigation, writing, and editing. Deena Graham: investigation, resources, writing, and editing. Michael Irwin: Investigation, writing, and editing. Claudine Isaacs: investigation, resources, writing, and editing. Heather S. L. Jim: investigation, resources, writing, editing, project administration, and funding acquisition. Kate Kuhlman: investigation, writing, and editing. Brenna C. McDonald: investigation, resources, writing, editing, project administration, and funding acquisition. Sunita K. Patel: Investigation, resources, writing, editing, and project administration. Kelly E. Rentscher: investigation, writing, and editing. James C. Root: investigation, supervision, writing, and editing. Andrew J. Saykin: investigation, resources, writing, editing, project administration, and funding acquisition. Danielle B. Tometich: investigation, writing, and editing. Kathleen Van Dyk: investigation, writing, and editing. Xingtao Zhou: formal analysis, data curation, and writing. Jeanne S. Mandelblatt: conceptualization, investigation, resources, writing, editing, supervision, project administration, and funding acquisition. Judith E. Carroll: conceptualization, investigation, supervision, project administration, writing, and editing.
Corresponding author
Ethics declarations
Competing interests
Elizabeth C. Breen has been a consultant for Georgetown University. Martine Extermann has been a consultant for Aileron and Alnylam and has received honoraria from OncLive. Claudine Isaacs has been a consultant for Genentech, AstraZeneca, Gilead Sciences, Novartis, Puma Biotechnology, Seagen, and Pfizer and received royalties from McGraw-Hill Companies and Wolter Kluwer; other disclosures are available at https://coi-asco-org.libproxy.lib.unc.edu/share/KZZ-5URC/Claudine%20Isaacs. Heather S. L. Jim has been a consultant for SBR Bioscience. Andrew J. Saykin has received support from Avid Radiopharmaceuticals, a subsidiary of Eli Lilly (in-kind contribution of a positron emission tomography tracer precursor), Bayer Oncology (scientific advisory board), Eisai (scientific advisory board), Siemens Medical Solutions USA (dementia advisory board), and Springer–Nature Publishing (editorial office support as editor in chief, Brain Imaging and Behavior). All other authors have declared no conflicts of interest.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
N/A. No individual person’s data is presented in any form in this manuscript.
Disclaimer
The study sponsor did not have any role in the design of the study, the collection, analysis, and interpretation of the data, the writing of the manuscript, or the decision to submit the manuscript for publication. The content is solely the responsibility of the authors and does not represent the official views of the National Institutes of Health.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 15 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nakamura, Z.M., Small, B.J., Zhai, W. et al. Depressive symptom trajectories in older breast cancer survivors: the Thinking and Living with Cancer Study. J Cancer Surviv (2023). https://doi.org/10.1007/s11764-023-01490-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11764-023-01490-2