Abstract
Purpose
This study aimed to test the efficacy of a 6-month intervention on weight loss in a group of overweight or obese breast cancer (BC) survivors. We promoted adherence to a healthy diet or/and to increase physical activity, making use of a step counter device. Here we present results regarding the change in anthropometric measures and blood parameters.
Methods
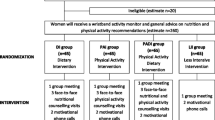
266 women treated for BC with a BMI ≥ 25 kg/m2 were randomized to a 6-month intervention into four arms: Dietary Intervention (DI); Physical Activity Intervention (PAI); Physical Activity and Dietary Intervention (PADI); Minimal Intervention (MI). Women were offered individualized counseling by a dietitian, a physiotherapist and a psychologist. Participants were followed up for an additional 18 months.
Results
231 women completed the 6-month intervention and 167 completed the additional 18-month follow-up. Respectively, 37.5% and 36.7% of women included in the DI and PADI arm reached the objective of the trial (weight reduction > 5%). Significant weight and circumferences decrease was observed at 6-month in the four arms. Weight decrease was more pronounced in the DI (-4.7% ± 5.0%) and PADI (-3.9% ± 4.5%) arms, persisted over time (at 12 and 24 months), where counseling was mainly focused on the dietic component. The intervention had an effect on the glucose level with a significant reduction in whole population (-0.9 ± 11.7 p-value 0.02) and most pronounced in the PADI arm (-2.4 ± 7.8 p-value 0.03).
Conclusions
Lifestyle intervention mainly focused on the dietetic component and making use of a step counter improved body weight, circumferences and glucose levels.
Implications for Cancer Survivors
A personalized approach yields a potential clinical benefit for BC survivors.




Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Associazione Italiana di Oncologia Medica. ‘I NUMERI DEL CANCRO IN ITALIA 2022’. Dec. 2022. https://www.aiom.it/wp-content/uploads/2022/12/2022_AIOM_NDC-web.pdf
Cheng KKF, Lim YTE, Koh ZM, Tam WWS. Home-based multidimensional survivorship programmes for breast cancer survivors. Cochrane Database Syst Rev. 2017;8:2017. https://doi.org/10.1002/14651858.CD011152.pub2.
Thomson ZO, Reeves MM. Can weight gain be prevented in women receiving treatment for breast cancer? A systematic review of intervention studies. Obes Rev. 2017;18(11):1364–73. https://doi.org/10.1111/OBR.12591.
Deluche E, Leobon S, Desport JC, Venat-Bouvet L, Usseglio J, Tubiana-Mathieu N. Impact of body composition on outcome in patients with early breast cancer. Support Care Cancer. 2018;26(3):861–8. https://doi.org/10.1007/S00520-017-3902-6.
Shaikh H, Bradhurst P, Ma LX, Tan SYC, Egger SJ, Vardy JL. Body weight management in overweight and obese breast cancer survivors. Cochrane Database Syst Rev. 2020;12(12):CD012110. https://doi.org/10.1002/14651858.CD012110.pub2.
Chan DSM, Vieira R, Abar L, Aune D, Balducci K, Cariolou M, Greenwood DC, Markozannes G, Nanu N, Becerra-Tomás N, Giovannucci EL, Gunter MJ, Jackson AA, Kampman E, Lund V, Allen K, Brockton NT, Croker H, Katsikioti D, McGinley-Gieser D, Mitrou P, Wiseman M, Cross AJ, Riboli E, Clinton SK, McTiernan A, Norat T, Tsilidis KK. Postdiagnosis body fatness, weight change and breast cancer prognosis: global Cancer Update Program (CUP global) systematic literature review and meta-analysis. Int J Cancer. 2023;152(4):572–99. https://doi.org/10.1002/ijc.34322.
World Cancer Research Fund and American Institute for Cancer Research. Diet, nutrition, physical activity and cancer: a global perspective. A summary of the third expert report; 2018. Available at https://wcrf.org.
Barbieri M, et al. Obesity-related mortality in France, Italy, and the United States: a comparison using multiple cause-of-death analysis. Int J Public Health 2017 62:6. 2017;62(6):623–9. https://doi.org/10.1007/S00038-017-0978-1.
Reeves MM, Terranova CO, Eakin EG, Demark-Wahnefried W. Weight loss intervention trials in women with breast cancer: a systematic review. Obes Rev. 2014;15(9):749–68. https://doi.org/10.1111/OBR.12190.
Ligibel JA, Basen-Engquist K, Bea JW. Weight Management and Physical Activity for Breast Cancer Prevention and Control. Am Soc Clin Oncol Educ Book. 2019;39(39):e22–33. https://doi.org/10.1200/EDBK_237423.
Runowicz CD, et al. American Cancer Society/American Society of Clinical Oncology Breast Cancer Survivorship Care Guideline. CA Cancer J Clin. 2016;66(1):43–73. https://doi.org/10.3322/CAAC.21319.
Wang S, Yang T, Qiang W, Zhao Z, Shen A, Zhang F. Benefits of weight loss programs for breast cancer survivors: a systematic reviews and meta-analysis of randomized controlled trials. Support Care Cancer. 2022;30(5):3745–60. https://doi.org/10.1007/S00520-021-06739-Z.
Bruinsma TJ, Dyer AM, Rogers CJ, Schmitz KH, Sturgeon KM. Effects of Diet and Exercise-Induced Weight Loss on Biomarkers of Inflammation in Breast Cancer Survivors: A Systematic Review and Meta-analysis. Cancer Epidemiol Biomarkers Prev. 2021;30(6):1048–62. https://doi.org/10.1158/1055-9965.EPI-20-1029.
Barchitta M, Maugeri A, Magnano San Lio R, Quattrocchi A, Degrassi F, Catalano F, Basile G, Agodi A. The effects of diet and dietary interventions on the quality of life among breast cancer survivors: a cross-sectional analysis and a systematic review of experimental studies. Cancers (Basel). 2020;12(2):322. https://doi.org/10.3390/cancers12020322.
Rock CL, et al. Nutrition and physical activity guidelines for cancer survivors. CA Cancer J Clin. 2012;62(4):242–74. https://doi.org/10.3322/CAAC.21142.
Rock CL, et al. American Cancer Society nutrition and physical activity guideline for cancer survivors. CA Cancer J Clin. 2022;72(3):230–62. https://doi.org/10.3322/CAAC.21719.
Stanton AL, et al. Outcomes from the Moving Beyond Cancer psychoeducational, randomized, controlled trial with breast cancer patients. J Clin Oncol. 2005;23(25):6009–18. https://doi.org/10.1200/JCO.2005.09.101.
Howard-Anderson J, Ganz PA, Bower JE, Stanton AL. Quality of life, fertility concerns, and behavioral health outcomes in younger breast cancer survivors: a systematic review. J Natl Cancer Inst. 2012;104(5):386–405. https://doi.org/10.1093/JNCI/DJR541.
Mazzarella L, et al. Obesity increases the incidence of distant metastases in oestrogen receptor-negative human epidermal growth factor receptor 2-positive breast cancer patients. Eur J Cancer. 2013;49(17):3588–97. https://doi.org/10.1016/J.EJCA.2013.07.016.
Esposito A, et al. Body mass index, adiposity and tumour infiltrating lymphocytes as prognostic biomarkers in patients treated with immunotherapy: A multi-parametric analysis. Eur J Cancer. 2021;145:197–209. https://doi.org/10.1016/J.EJCA.2020.12.028.
Gnagnarella P, Dragà D, Baggi F, Simoncini MC, Sabbatini A, Mazzocco K, Bassi FD, Pravettoni G, Maisonneuve P. Promoting weight loss through diet and exercise in overweight or obese breast cancer survivors (InForma): study protocol for a randomized controlled trial. Trials. 2016;17:363. https://doi.org/10.1186/s13063-016-1487-x.
World Cancer Research Fund/American Institute for Cancer Research. Diet, nutrition, physical activity and cancer: a global perspective. In: Continuous Update Project Expert Report. Washington (DC): American Institute for Cancer Research; 2007.
CREA. Dossier Scientifico Linee Guida per Una Sana Alimentazione. Roma: CREA; 2018. p. 1570. Available online: https://www.crea.gov.it/web/alimenti-e-nutrizione/-/dossier-scientifico-linee-guida-per-una-sana-alimentazione-2018.
Seagle HM, Strain GW, Makris A, Reeves RS. Position of the American Dietetic Association: weight management. J Am Diet Assoc. 2009;109(2):330–46. https://doi.org/10.1016/J.JADA.2008.11.041.
Spencer JC, Wheeler SB. A systematic review of Motivational Interviewing interventions in cancer patients and survivors. Patient Educ Couns. 2016. https://doi.org/10.1016/j.pec.2016.02.003.
Malins S, et al. Reducing dropout in acceptance and commitment therapy, mindfulness-based cognitive therapy, and problem-solving therapy for chronic pain and cancer patients using motivational interviewing. Br J Clin Psychol. 2020;59(3):424–38. https://doi.org/10.1111/BJC.12254.
Hayes C. What is physical activity and why should we do it? Perspect Public Health. 2009;129(3):111–2. https://doi.org/10.1177/1757913908103804.
Miller WR, Rollnick S. Motivational interviewing: preparing people for change. New York, NY: The Guilford Press; 2002.
S Miller, WR Rollnick, Motivational Interviewing: Preparing People for Change. New york, 2002.
Piccoli A, Rossi B, Pillon L, Bucciante G. A new method for monitoring body fluid variation by bioimpedance analysis: the RXc graph. Kidney Int. 1994;46(2):534–9. https://doi.org/10.1038/KI.1994.305.
Buffa R, Mereu E, Comandini O, Ibanez ME, Marini E. Bioelectrical impedance vector analysis (BIVA) for the assessment of two-compartment body composition. Eur J Clin Nutr. 2014;68(11):1234–40. https://doi.org/10.1038/EJCN.2014.170.
Bach-Faig A, et al. Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr. 2011;14(12A):2274–84. https://doi.org/10.1017/S1368980011002515.
Dunbar-Jacob J, Erlen JA, Schlenk EA, Ryan CM, Sereika SM, Doswell WM. Adherence in chronic disease. Annu Rev Nurs Res. 2000;18:48–90. https://doi.org/10.1891/0739-6686.18.1.48.
Singh B, Zopf EM, Howden EJ. Effect and feasibility of wearable physical activity trackers and pedometers for increasing physical activity and improving health outcomes in cancer survivors: A systematic review and meta-analysis. J Sport Health Sci. 2022;11(2):184–93. https://doi.org/10.1016/J.JSHS.2021.07.008.
Bruno E, et al. Adherence to Dietary Recommendations after One Year of Intervention in Breast Cancer Women: The DIANA-5 Trial. Nutrients. 2021;13:9. https://doi.org/10.3390/NU13092990.
Cortesi L, Sebastiani F, Iannone A, Marcheselli L, Venturelli M, Piombino C, Toss A, Federico M. Lifestyle intervention on body weight and physical activity in patients with breast cancer can reduce the risk of death in obese women: the EMILI study. Cancers (Basel). 2020;12(7):1709. https://doi.org/10.3390/cancers12071709.
Finocchiaro C, et al. Effect of specific educational program on dietary change and weight loss in breast-cancer survivors. Clin Nutr. 2016;35(4):864–70. https://doi.org/10.1016/J.CLNU.2015.05.018.
Nimptsch K, Konigorski S, Pischon T. Diagnosis of obesity and use of obesity biomarkers in science and clinical medicine. Metabolism. 2019;92:61–70. https://doi.org/10.1016/J.METABOL.2018.12.006.
Alfano CM, Molfino A, Muscaritoli M. Interventions to promote energy balance and cancer survivorship: priorities for research and care. Cancer. 2013;119(11):2143–50. https://doi.org/10.1002/CNCR.28062.
Iwase T, Wang X, Shrimanker TV, Kolonin MG, Ueno NT. Body composition and breast cancer risk and treatment: mechanisms and impact. Breast Cancer Res Treat. 2021;186(2):273–83. https://doi.org/10.1007/S10549-020-06092-5.
Chan DSM, et al. Body mass index and survival in women with breast cancer-systematic literature review and meta-analysis of 82 follow-up studies. Ann Oncol. 2014;25(10):1901–14. https://doi.org/10.1093/ANNONC/MDU042.
Protani M, Coory M, Martin JH. Effect of obesity on survival of women with breast cancer: systematic review and meta-analysis. Breast Cancer Res Treat. 2010;123(3):627–35. https://doi.org/10.1007/S10549-010-0990-0.
Machado VMQ, Justa RMDE, Lopes da Costa S, Barbosa MC, Damasceno NRT, Verde SMML. Bioelectrical impedance vector applied to body composition evaluation of women survivors of breast cancer: A longitudinal study. Clin Nutr ESPEN. 2021;44:247–53. https://doi.org/10.1016/J.CLNESP.2021.06.008.
Brown JC, et al. A randomized trial of exercise and diet on body composition in survivors of breast cancer with overweight or obesity. Breast Cancer Res Treat. 2021;189(1):145–54. https://doi.org/10.1007/S10549-021-06284-7.
Djuric Z, et al. Combining weight-loss counseling with the weight watchers plan for obese breast cancer survivors. Obes Res. 2002;10(7):657–65. https://doi.org/10.1038/OBY.2002.89.
Ryan D, Heaner M. Guidelines (2013) for managing overweight and obesity in adults. Preface to the full report. Obesity (Silver Spring). 2014;22(Suppl 2):S1–3. https://doi.org/10.1002/OBY.20819.
Löf M, Bergström K, Weiderpass E. Physical activity and biomarkers in breast cancer survivors: A systematic review. Maturitas. 2012;73(2):134–42. https://doi.org/10.1016/J.MATURITAS.2012.07.002.
Acknowledgements
We would like to acknowledge and thank the participants who volunteered to take part, AKERN s.r.l for providing the disposable electrodes necessary for bioelectrical impedance measures during the trial, Allegramente Walking, ASD for providing support for physical activity interventions, William Russell-Edu for help with the literature and for editing the manuscript, and the association “La forza e il sorriso” for allowing us to host our groups in their meeting room (www.laforzaeilsorriso.it). We would also like to acknowledge and thank Sabina Sieri for help with nutritional assessment and Greta Pettini for help with the group meetings.
Funding
The trial is funded by the Associazione Italiana per la Ricerca sul Cancro (AIRC) (Grant n. 15963). This work was also partially supported by the Italian Ministry of Health with Ricerca Corrente and 5 × 1000 funds.
Author information
Authors and Affiliations
Contributions
PM: Study conception, Funding acquisition, Formal analysis, Writing—Review & Editing; PG: Study conception, Funding acquisition, Writing—Original Draft, Supervision; DD, SR, KM, MM GP: Investigation; FB, MCS, AS, GP: Methodology; FDB, NP, LZ: Supervision; ML: Writing—Review & Editing.
Corresponding author
Ethics declarations
Ethics approval
The study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethics Committee of the European Institute of Oncology (Reference number: n. R233/15 –IEO 244—Protocol version 3).
The trial has been registered at ClinicalTrials.gov (NCT02622711) and at the ISRCTN registry (ISRCTN53325751).
Consent to participate
All participants provided written informed consent.
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Trial Registration: ISRCTN53325751; ClinicalTrials.gov NCT02622711.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gnagnarella, P., Dragà, D., Raja, S. et al. Physical activity and/or dietary intervention in overweight or obese breast cancer survivors: results of the InForma randomized trial. J Cancer Surviv (2023). https://doi.org/10.1007/s11764-023-01415-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11764-023-01415-z