Abstract
Purpose
To review the empirical qualitative literature on cancer survivor’s experiences with loneliness to inform assessments and interventions for improving cancer survivors’ social well-being.
Methods
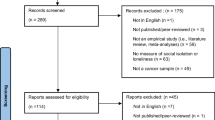
A rigorous systematic review of qualitative studies published in five databases between 1993 and 2016 was conducted. Three coders reviewed 285 titles and abstracts and, after applying a critical review process, 20 manuscripts were synthesized using meta-ethnography.
Results
The synthesis of the 20 studies provided a framework for understanding survivors’ layers of loneliness at the level of the individual, their social support system, the healthcare system, and society. Internally, survivors described loneliness resulting from feelings of inauthenticity, of being alone in their cancer experience, and of lack of control. In their social networks, survivors attributed loneliness to others’ avoidance, misperceptions of cancer, and others’ failure to recognize the effects of cancer after active treatment. Unmet needs after treatment contributed to feelings of loneliness within the healthcare system. Further, societal stigma around cancer and pressures to experience growth after cancer created another layer of loneliness. The results suggest the need to move beyond an individual level perspective in assessing and treating loneliness in cancer survivors.
Conclusions
This meta-ethnography presents an integrated framework of loneliness in cancer survivors as a multi-layered experience. Implications for Cancer Survivors Conceptualizing loneliness from a systemic perspective adds missing pieces to the loneliness puzzle by encouraging assessment and intervention at interacting levels of functioning; considering how individuals respond to and are affected by their social systems can deepen our understanding of cancer survivorship.

Similar content being viewed by others
References
Jung C. Memories, dreams, reflections. Rev. ed. New York: Pantheon Books; 1973.
Peplau LA, Perlman D, editors. Loneliness: a sourcebook of current theory, research and therapy. New York: Wiley-Interscience; 1982.
Hawkley LC, Cacioppo JT. Loneliness matters: a theoretical and empirical review of consequences and mechanisms. Ann Behav Med. 2010;40:218–27.
Laird BJA, Scott AC, Colvin LA, McKeon AL, Murray GD, Fearon KCH, et al. Pain, depression, and fatigue as a symptom cluster in advanced cancer. J Pain Symptom Manag. 2011;42:1–11. https://doi.org/10.1016/j.jpainsymman.2010.10.261.
Pinquart M, Duberstein PR. Associations of social networks with cancer mortality: a meta-analysis. Oncol Hemotol. 2010;75(2):122–37.
Michael YL, Kawachi I, Berkman LF, Holmes MD, Colditz A. The persistent impact of breast carcinoma on functional health status: prospective evidence from the nurses’ health study. Cancer. 2000;89:2176–86. https://doi.org/10.1002/1097-0142(20001201)89:11%3C2176::AID-CNCR5%3E3.0.CO;2-6.
Peplau LA, Russel D, Heim M. The experience of loneliness. In: Frieze IH, Bar-Tal D, Carroll JS, editors. New approaches to social problems: applications of attribution theory. San Francisco: Jossey-Bass; 1979. p. 53–78.
Edmondson B. All the lonely people. AARP: The Magazine 2010;83.
Perissinotto CM, Cenzer IS, Covinsky KE. Loneliness in older persons: a predictor of functional decline and death. Arch Intern Med. 2012;172(14):1078–84. https://doi.org/10.1001/archinternmed.2012.
Cacioppo JT, Patrick W. Loneliness: Human nature and the need for social connection. WW Norton & Company; 2008.
Stuewe-Portnoff G. Loneliness: lost in the landscape of meaning. J Psychol. 1988;122(6):545–55.
Lepore SJ, Silver RC, Wortman CB, Wayment HA. Social constraints, intrusive thoughts, and depressive symptoms among bereaved mothers. J Pers Soc Psychol. 1996;70(2):271–82.
Young JE. Loneliness, depression, and cognitive therapy: Theory and application. In: Peplau LA, Perlman D, editors. Loneliness: A sourcebook of current theory, research and therapy. New York: Wiley-Interscience; 1982. p. 379–406.
Deckx L, van den Akker M. Buntix F. Risk factors for loneliness in patients with cancer: a systematic literature review and meta-analysis. Eur J Oncol Nurs. 2014;18:466–77. https://doi.org/10.1016/j.ejon.2014.05.002.
Raque-Bogdan TL, Gissen M, Lamphere BR, Beranek M. Kostiuk M. Meta-ethnography on loneliness in older cancer survivors: layers of silencing. Podium presentation at the American Psychosocial Oncology Society annual meeting, Orlando, FL. 2017.
Russell DW. UCLA loneliness scale (version 3): reliability, validity, and factor structure. J Pers Assess. 1996;66(1):20–40. https://doi.org/10.1207/s15327752jpa6601_2.
de Jong-Gierveld J, Kamphuls F. The development of a Rasch-type loneliness scale. Appl Psychol Meas. 1985;9(3):289–99.
McCarthy I, Dowling M. Living with a diagnosis of non-small cell lung cancer: patients’ lived experiences. Int J Palliat Nurs. 2009;15(12):579–87. https://doi.org/10.12968/ijpn.2009.15.12.45862.
Rosedale M. Survivor loneliness of women following breast cancer. Oncol Nurs Forum. 2009;36(2):175–83. https://doi.org/10.1188/09.ONF.175-183.
Masi CM, Chen HY, Hawkley LC, Cacioppo JT. A meta-analysis of interventions to reduce loneliness. Personal Soc Psychol Rev. 2011;15(3):219–66. https://doi.org/10.1177/1088868310377394.
Britten N, Campbell R, Pope C, Donovan J, Morgan M, Pill R. Using meta ethnography to synthesise qualitative research: a worked example. J Health Serv Res Policy. 2002;7:209–15.
Atkins S, Lewin S, Smith H, Engel M, Fretheim A, Volmink J. Conducting a meta-ethnography of qualitative literature: lessons learnt. BMC Med Res Methodol. 2008;8(1):21. https://doi.org/10.1186/1471-2288-8-21.
Noblit GW, Hare RD. Meta-ethnography: synthesizing qualitative studies. Newbury Park: Sage Publications Inc; 1988.
Campbell R, Pound P, Morgan M, Daker-White G, Britten N, Pill R, et al. Evaluating meta ethnography: systematic analysis and synthesis of qualitative research. Health Technol Assess. 2012;5(43):1–164. https://doi.org/10.3310/hta15430.
Toye F, Seers K, Allcock N, Briggs M, Carr E, Barker K. Meta-ethnography 25 years on: challenges and insights for synthesizing a large number of qualitative studies. BMC Med Res Methodol. 2014;14:80. https://doi.org/10.1186/1471-2288-14-80.
Lagerdahl AS, Moynihan M, Stollery B. An exploration of existential experiences of patients following curative treatment for cancer: Reflections from a U.K. sample. J Psychosoc Oncol. 2014;32(5):555–75. https://doi.org/10.1080/07347332.2014.936647.
Halldorsdottir S, Hamrin E. Experiencing existential changes: the lived experience of having cancer. Cancer Nurs. 1996;19(1):29–36.
Wyatt G, Kurtz ME, Liken M. Breast cancer survivors: an exploration of quality of life issues. Cancer Nurs. 1993;16(6):440–48.
Moore KA, Ford PJ, Farah, CS. “I have quality of life...but...”: exploring support needs important to quality of life in head and neck cancer. Eur J of Oncol Nurs.2014;18:192–200. https://doi.org/10.1016/j.ejon.2013.10.010.
Jefferies H, Clifford C. Aloneness: the lived experience of women with cancer of the vulva. Eur J Cancer Cancer. 2011;20:738–46. https://doi.org/10.1111/j.1365-2354.2011.01246.x.
Lloyd PA, Briggs EV, Kane N, Jeyarajah AR, Shepherd JH. Women’s experiences after a radical vaginal trachelectomy for early stage cervical cancer. A descriptive phenomenological study. Eur J Oncol Nurs. 2014;18:363–71. https://doi.org/10.1016/j.ejon.2014.03.014.
Sinding C, Grassau P, Barnoff L. Community support, community values: the experiences of lesbians diagnosed with cancer. Women Health. 2007;44(2):59–79. https://doi.org/10.1300/J013v44n02_04.
McGrath P, Patterson C, Yates P, Treloar S, Oldenburg B, Loos C. A study of postdiagnosis breast cancer concerns for women living in rural and remote Queensland. Part I: personal concerns. Aust J Rural Health. 1999;7:34–42.
Sekse RJT, Raaheim M, Blaaka G, Gjengedal E. Life beyond cancer: women’s experiences 5 years after treatment for gynaecological cancer. Scand J Caring Sci. 2010;24(4):799–807. https://doi.org/10.1111/j.1471-6712.2010.00778.x.
Hauken MA, Larsen TMB, Holsen I. Meeting reality: young adult cancer survivors’ experiences reentering everyday life after cancer treatment. Cancer Nurs. 2013;36(5):17–26. https://doi.org/10.1097/NCC.0b013e318278d4fc.
Lepore SJ, Revenson TA. Social constraints on disclosure and adjustment to cancer. Soc Personal Psychol Compass. 2007;1(1):313–33.
Cohee AA, Adams RN, Johns SA, Von Ah D, Zoppi K, Fife B, ... Champion VL. Long-term fear of recurrence in young breast cancer survivors and partners. Psychooncology 2017;26(1):22–28. https://doi.org/10.1002/pon.4008.
Wu H, Harden JK. Symptom burden and quality of life in survivorship: a review of the literature. Cancer Nurs. 2015;38(1):E29–54. https://doi.org/10.1097/NCC.0000000000000135.
Adams RN, Mosher CE, Abonour R, Robertson MJ, Champion VL, Kroenke K. Cognitive and situational precipitants of loneliness among patients with cancer: a qualitative analysis. Oncol Nurs Forum. 2016;43(2):156–63. https://doi.org/10.1188/16.ONF.156-163.
Mosher CE, Lepore SJ, Wu L, Austin J, Valdimarsdottir H, Rowley S, et al. Social correlates of distress following hematopoietic stem cell transplantation: exploring the role of loneliness and cognitive processing. J Health Psychol. 2012;17(7):1022–32. https://doi.org/10.1177/1359105311432490.
Revenson TA, Lepore SJ. Coping in social context. In: Baum A, Revenson TA, Singer J, editors. Handbook of health psychology. 2nd ed. New York: Psychology Press; 2012. p. 193–217.
Manne SL, Rubin S, Edelson M, Rosenblum N, Bergman C, Hernandez E, et al. Coping and communication-enhancing intervention versus supportive counseling for women diagnosed with gynecological cancers. J Consult Clin Psychol. 2007;75(4):615–28. https://doi.org/10.1037/0022-006X.75.4.615.
Porter LS, Keefe FJ, Baucom DH, Hurwitz H, Moser B, Patterson E, et al. Partner-assisted emotional disclosure for patients with gastrointestinal cancer. Cancer. 2009;115(S18):4326–38. https://doi.org/10.1002/cncr.24578.
Northouse LL, Katapodi MC, Song L, Zhang L, Mood DW. Interventions with family caregivers of cancer patients: meta-analysis of randomized trials. CA Cancer J Clin. 2010;60(5):317–39. https://doi.org/10.3322/caac.20081.
McLean LM, Walton T, Rodin G, Esplen MJ, Jones JM. A couple-based intervention for patients and caregivers facing end-stage cancer: outcomes of a randomized controlled trial. Psycho-Oncology. 2013;1:28–38. https://doi.org/10.1002/pon.2046.
Wong AG, Ki P, Maharaj A, Brown E, Davis C, Apolinsky F. Social support sources, types, and generativity: a focus group study of cancer survivors and their caregivers. Soc Work Health Care. 2014;53:214–32. https://doi.org/10.1080/00981389.2013.873515.
Blanch-Hartigan D, Chawla N, Moser RP, Rutten LJF, Hesse BW, Arora NK. Trends in cancer survivors’ experience of patient-centered communication: results from the health information National Trends Survey (HINTS). J Cancer Surviv. 2016;10(6):1067–77.
Forsythe LP, Alfano CM, Leach CR, Ganz PA, Stefanek ME, Rowland JH. Who provides psychosocial follow-up care for post-treatment cancer survivors? A survey of medical oncologists and primary care physicians. J Clin Oncol. 2012;30(23):2897–905. https://doi.org/10.1200/JCO.2011.39.9832.
Ganz PA, Earle CC, Goodwin PJ. Journal of clinical oncology update on progress in cancer survivorship care and research. J Clin Oncol. 2012;30(30):3655–6. https://doi.org/10.1200/JCO.2012.45.3886.
Parker PA, Davison BJ, Tishelman C, Brundage MD. What do we know about facilitating patient communication in the cancer setting? Psycho-Oncology. 2005;14:848–58. https://doi.org/10.1002/pon.946.
Pehrson C, Banerjee SC, Manna R, Johnson Shen M, Hammonds S, Coyle N, et al. Responding empathically to patients: development, implementation, and evaluation of a communication skills training module for oncology nurses. Patient Educ Couns. 2016;99(4):610–6. https://doi.org/10.1016/j.pec.2015.11.021.
Raque-Bogdan TL, Hoffman MA, Ginter AC, Piontkowski S, Schexnayder K, White R. The work life and career development of young breast cancer survivors. J Couns Psychol. 2015;62:655–69. https://doi.org/10.1037/cou0000068.
Kaiser K. The meaning of the survivor identity for women with breast cancer. Soc Sci Med. 2008;67:79–87. https://doi.org/10.1016/j.socscimed.2008.03.036.
Trusson D, Pilnick A. Between stigma and pink positivity: women’s perceptions of social interactions during and after breast cancer treatment. Sociol Health Ill. 2017;39(3):458–73. https://doi.org/10.1111/1467-9566.12486.
Funding
This project was supported by the University of Denver Faculty Research Fund grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors state that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Raque-Bogdan, T.L., Lamphere, B., Kostiuk, M. et al. Unpacking the layers: a meta-ethnography of cancer survivors’ loneliness. J Cancer Surviv 13, 21–33 (2019). https://doi.org/10.1007/s11764-018-0724-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-018-0724-6