Abstract
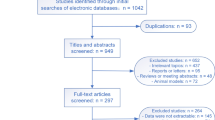
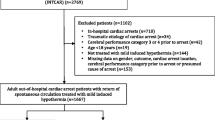
Patients who experience out-of-hospital cardiac arrest (OHCA) have unacceptably high mortality rates. It remains unclear whether gender has an association with survival in this regard. Hence, we aimed to investigate the association between gender and survival by conducting a systematic review and meta-analysis. The databases of PubMed, Embase, and Cochrane Database of Systematic Reviews were searched from inception to 17 March, 2020. Studies assessing the association between gender and survival to discharge or 30-day survival after OHCA were included. Two reviewers independently assessed the eligibility of the identified studies. The random-effects model was used to pool data, and the outcome was reported as odds ratios (ORs) and 95% confidence intervals, as the relative measure of association. Twenty-three eligible studies enrolling 897,805 patients were included in this systematic review. Overall, women were older and less likely to experience arrest in public places. When arrest occurred, women had less initial shockable rhythm, were less likely to be witnessed by bystanders, and were less likely provided with CPR compared with men. After admission, women underwent less coronary angiography, percutaneous coronary angiography, and targeted temperature management therapy. Eleven studies with ORs were pooled, showing a significant survival benefit in women (OR = 1.08, p < 0.05, I2 = 52.3%). In the subgroup analysis, both premenopausal women (< 50 years) (OR = 1.42, p < 0.001, I2 = 0%) and postmenopausal women (≥ 50 years) (OR = 1.07, p < 0.05, I2 = 16.4%) had higher odds of survival compared with age-matched men. Despite the unfavorable factors, the pooled results showed a significant survival benefit in women after OHCA, especially in premenopausal women.




Similar content being viewed by others
References
Ro YS, Shin SD, Song KJ, Lee EJ, Kim JY, Ahn KO, Chung SP, Kim YT, Hong SO, Choi JA, Hwang SO, Oh DJ, Park CB, Suh GJ, Cho SI, Hwang SS (2013) A trend in epidemiology and outcomes of out-of-hospital cardiac arrest by urbanization level: a nationwide observational study from 2006 to 2010 in South Korea. Resuscitation 84(5):547–557. https://doi.org/10.1016/j.resuscitation.2012.12.020
Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, Cushman M, Das SR, de Ferranti S, Després JP, Fullerton HJ, Howard VJ, Huffman MD, Isasi CR, Jiménez MC, Judd SE, Kissela BM, Lichtman JH, Lisabeth LD, Liu S, Mackey RH, Magid DJ, McGuire DK, Mohler ER 3rd, Moy CS, Muntner P, Mussolino ME, Nasir K, Neumar RW, Nichol G, Palaniappan L, Pandey DK, Reeves MJ, Rodriguez CJ, Rosamond W, Sorlie PD, Stein J, Towfighi A, Turan TN, Virani SS, Woo D, Yeh RW, Turner MB (2016) Heart disease and stroke statistics-2016 update: a report from the American Heart Association. Circulation 133(4):e38-360. https://doi.org/10.1161/cir.0000000000000350
Berdowski J, Berg RA, Tijssen JG, Koster RW (2010) Global incidences of out-of-hospital cardiac arrest and survival rates: systematic review of 67 prospective studies. Resuscitation 81(11):1479–1487. https://doi.org/10.1016/j.resuscitation.2010.08.006
Blom MT, Oving I, Berdowski J, Van Valkengoed IGM, Bardai A, Tan HL (2019) Women have lower chances than men to be resuscitated and survive out-of-hospital cardiac arrest. Eur Heart J 40(47):3824–3834. https://doi.org/10.1093/eurheartj/ehz297
Dicker B, Conaglen K, Howie G (2018) Gender and survival from out-of-hospital cardiac arrest: a New Zealand registry study. Emerg Med J 35(6):367–371. https://doi.org/10.1136/emermed-2017-207176
Goto Y, Funada A, Maeda T, Okada H, Goto Y (2019) Sex-specific differences in survival after out-of-hospital cardiac arrest: a nationwide, population-based observational study. Crit Care 23(1):263. https://doi.org/10.1186/s13054-019-2547-x
Lindgren E, Covaciu L, Smekal D, Lagedal R, Nordberg P, Elfwén L, Svensson L, Jonsson M, James S, Rubertsson S (2019) Gender differences in utilization of coronary angiography and angiographic findings after out-of-hospital cardiac arrest: a registry study. Resuscitation 143:189–195. https://doi.org/10.1016/j.resuscitation.2019.07.015
Bougouin W, Mustafic H, Marijon E, Murad MH, Dumas F, Barbouttis A, Jabre P, Beganton F, Empana JP, Celermajer DS, Cariou A, Jouven X (2015) Gender and survival after sudden cardiac arrest: a systematic review and meta-analysis. Resuscitation 94:55–60. https://doi.org/10.1016/j.resuscitation.2015.06.018
Bougouin W, Dumas F, Marijon E, Geri G, Champigneulle B, Chiche JD, Varenne O, Spaulding C, Mira JP, Jouven X, Cariou A (2017) Gender differences in early invasive strategy after cardiac arrest: insights from the PROCAT registry. Resuscitation 114:7–13. https://doi.org/10.1016/j.resuscitation.2017.02.005
Winther-Jensen M, Hassager C, Kjaergaard J, Bro-Jeppesen J, Thomsen JH, Lippert FK, Kober L, Wanscher M, Soholm H (2018) Women have a worse prognosis and undergo fewer coronary angiographies after out-of-hospital cardiac arrest than men. Eur Heart J Acute Cardiovasc Care 7(5):414–422. https://doi.org/10.1177/2048872617696368
Bosson N, Kaji AH, Fang A, Thomas JL, French WJ, Shavelle D, Niemann JT (2016) Sex differences in survival from out-of-hospital cardiac arrest in the era of regionalized systems and advanced post-resuscitation care. J Am Heart Assoc 5(9):e004131. https://doi.org/10.1161/JAHA.116.004131
Kitamura T, Iwami T, Nichol G, Nishiuchi T, Hayashi Y, Nishiyama C, Sakai T, Kajino K, Hiraide A, Ikeuchi H, Nonogi H, Kawamura T (2010) Reduction in incidence and fatality of out-of-hospital cardiac arrest in females of the reproductive age. Eur Heart J 31(11):1365–1372. https://doi.org/10.1093/eurheartj/ehq059
Akahane M, Ogawa T, Koike S, Tanabe S, Horiguchi H, Mizoguchi T, Yasunaga H, Imamura T (2011) The effects of sex on out-of-hospital cardiac arrest outcomes. Am J Med 124(4):325–333. https://doi.org/10.1016/j.amjmed.2010.10.020
Cline SL, von Der Lohe E, Newman MM, Groh WJ (2005) Factors associated with poor survival in women experiencing cardiac arrest in a rural setting. Heart Rhythm 2(5):492–496. https://doi.org/10.1016/j.hrthm.2005.01.018
Ng YY, Wah W, Liu N, Zhou SA, Ho AF, Pek PP, Shin SD, Tanaka H, Khunkhlai N, Lin CH, Wong KD, Cai WW, Ong ME (2016) Associations between gender and cardiac arrest outcomes in Pan-Asian out-of-hospital cardiac arrest patients. Resuscitation 102:116–121. https://doi.org/10.1016/j.resuscitation.2016.03.002
Mahapatra S, Bunch TJ, White RD, Hodge DO, Packer DL (2005) Sex differences in outcome after ventricular fibrillation in out-of-hospital cardiac arrest. Resuscitation 65(2):197–202. https://doi.org/10.1016/j.resuscitation.2004.10.017
Teodorescu C, Reinier K, Uy-Evanado A, Ayala J, Mariani R, Wittwer L, Gunson K, Jui J, Chugh SS (2012) Survival advantage from ventricular fibrillation and pulseless electrical activity in women compared to men: The oregon sudden unexpected death study. J Interv Cardiac Electrophysiol 34(3):219–225. https://doi.org/10.1007/s10840-012-9669-2
Safdar B, Stolz U, Stiell IG, Cone DC, Bobrow BJ, Deboehr M, Dreyer J, Maloney J, Spaite DW (2014) Differential survival for men and women from out-of-hospital cardiac arrest varies by age: results from the OPALS study. Acad Emerg Med 21(12):1503–1511. https://doi.org/10.1111/acem.12540
Kim C, Fahrenbruch CE, Cobb LA, Eisenberg MS (2001) Out-of-hospital cardiac arrest in men and women. Circulation 104(22):2699–2703. https://doi.org/10.1161/hc4701.099784
Herlitz J, Engdahl J, Svensson L, Young M, Ängquist KA, Holmberg S (2004) Is female sex associated with increased survival after out-of-hospital cardiac arrest? Resuscitation 60(2):197–203. https://doi.org/10.1016/j.resuscitation.2003.09.012
Pell JP, Sirel J, Marsden AK, Cobbe SM (2000) Sex differences in outcome following community-based cardiopulmonary arrest. Eur Heart J 21(3):239–244. https://doi.org/10.1053/euhj.1999.1629
Arrich J, Sterz F, Fleischhackl R, Uray T, Losert H, Kliegel A, Wandaller C, Köhler K, Laggner AN (2006) Gender modifies the influence of age on outcome after successfully resuscitated cardiac arrest: a retrospective cohort study. Medicine 85(5):288–294. https://doi.org/10.1097/01.md.0000236954.72342.20
Bray JE, Stub D, Bernard S, Smith K (2013) Exploring gender differences and the “oestrogen effect” in an Australian out-of-hospital cardiac arrest population. Resuscitation 84(7):957–963. https://doi.org/10.1016/j.resuscitation.2012.12.004
Wissenberg M, Hansen CM, Folke F, Lippert FK, Weeke P, Karlsson L, Rajan S, Søndergaard KB, Kragholm K, Christensen EF, Nielsen SL, Køber L, Gislason GH, Torp-Pedersen C (2014) Survival after out-of-hospital cardiac arrest in relation to sex: a nationwide registry-based study. Resuscitation 85(9):1212–1218. https://doi.org/10.1016/j.resuscitation.2014.06.008
Johnson MA, Haukoos JS, Larabee TM, Daugherty S, Chan PS, McNally B, Sasson C (2013) Females of childbearing age have a survival benefit after out-of-hospital cardiac arrest. Resuscitation 84(5):639–644. https://doi.org/10.1016/j.resuscitation.2012.09.011
Ahn KO, Shin SD, Hwang SS (2012) Sex disparity in resuscitation efforts and outcomes in out-of-hospital cardiac arrest. Am J Emerg Med 30(9):1810–1816. https://doi.org/10.1016/j.ajem.2012.02.018
Morrison LJ, Schmicker RH, Weisfeldt ML, Bigham BL, Berg RA, Topjian AA, Abramson BL, Atkins DL, Egan D, Sopko G, Rac VE (2016) Effect of gender on outcome of out of hospital cardiac arrest in the Resuscitation Outcomes Consortium. Resuscitation 100:76–81. https://doi.org/10.1016/j.resuscitation.2015.12.002
Terman SW, Shields TA, Hume B, Silbergleit R (2015) The influence of age and chronic medical conditions on neurological outcomes in out of hospital cardiac arrest. Resuscitation 89:169–176. https://doi.org/10.1016/j.resuscitation.2015.01.006
Bunch TJ, White RD, Gersh BJ, Meverden RA, Hodge DO, Ballman KV, Hammill SC, Shen WK, Packer DL (2003) Long-term outcomes of out-of-hospital cardiac arrest after successful early defibrillation. N Eng J Med 348(26):2626–2633. https://doi.org/10.1056/NEJMoa023053
Wissenberg M, Lippert FK, Folke F, Weeke P, Hansen CM, Christensen EF, Jans H, Hansen PA, Lang-Jensen T, Olesen JB, Lindhardsen J, Fosbol EL, Nielsen SL, Gislason GH, Kober L, Torp-Pedersen C (2013) Association of national initiatives to improve cardiac arrest management with rates of bystander intervention and patient survival after out-of-hospital cardiac arrest. JAMA 310(13):1377–1384. https://doi.org/10.1001/jama.2013.278483
White RD, Hankins DG, Bugliosi TF (1998) Seven years’ experience with early defibrillation by police and paramedics in an emergency medical services system. Resuscitation 39(3):145–151. https://doi.org/10.1016/s0300-9572(98)00135-x
Nichol G, Thomas E, Callaway CW, Hedges J, Powell JL, Aufderheide TP, Rea T, Lowe R, Brown T, Dreyer J, Davis D, Idris A, Stiell I (2008) Regional variation in out-of-hospital cardiac arrest incidence and outcome. JAMA 300(12):1423–1431. https://doi.org/10.1001/jama.300.12.1423
Granfeldt A, Wissenberg M, Hansen SM, Lippert FK, Lang-Jensen T, Hendriksen OM, Torp-Pedersen C, Christensen EF, Christiansen CF (2016) Clinical predictors of shockable versus non-shockable rhythms in patients with out-of-hospital cardiac arrest. Resuscitation 108:40–47. https://doi.org/10.1016/j.resuscitation.2016.08.024
Nolan JP, Soar J, Cariou A, Cronberg T, Moulaert VR, Deakin CD, Bottiger BW, Friberg H, Sunde K, Sandroni C (2015) European Resuscitation Council and European Society of intensive care medicine guidelines for post-resuscitation care 2015: section 5 of the European Resuscitation Council Guidelines for Resuscitation 2015. Resuscitation 95:202–222. https://doi.org/10.1016/j.resuscitation.2015.07.018
Bernard SA, Gray TW, Buist MD, Jones BM, Silvester W, Gutteridge G, Smith K (2002) Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Eng J Med 346(8):557–563. https://doi.org/10.1056/NEJMoa003289
Hypothermia after Cardiac Arrest Study Group (2002) Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N Eng J Med 346(8):549–556. https://doi.org/10.1056/NEJMoa012689
Lundbye JB, Rai M, Ramu B, Hosseini-Khalili A, Li D, Slim HB, Bhavnani SP, Nair SU, Kluger J (2012) Therapeutic hypothermia is associated with improved neurologic outcome and survival in cardiac arrest survivors of non-shockable rhythms. Resuscitation 83(2):202–207. https://doi.org/10.1016/j.resuscitation.2011.08.005
Testori C, Sterz F, Behringer W, Haugk M, Uray T, Zeiner A, Janata A, Arrich J, Holzer M, Losert H (2011) Mild therapeutic hypothermia is associated with favourable outcome in patients after cardiac arrest with non-shockable rhythms. Resuscitation 82(9):1162–1167. https://doi.org/10.1016/j.resuscitation.2011.05.022
Peberdy MA, Callaway CW, Neumar RW, Geocadin RG, Zimmerman JL, Donnino M, Gabrielli A, Silvers SM, Zaritsky AL, Merchant R, Vanden Hoek TL, Kronick SL (2010) Part 9: post-cardiac arrest care: 2010 American Heart Association Guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 122(18 Suppl 3):S768-786. https://doi.org/10.1161/circulationaha.110.971002
Soar J, Callaway CW, Aibiki M, Böttiger BW, Brooks SC, Deakin CD, Donnino MW, Drajer S, Kloeck W, Morley PT, Morrison LJ, Neumar RW, Nicholson TC, Nolan JP, Okada K, O’Neil BJ, Paiva EF, Parr MJ, Wang TL, Witt J (2015) Part 4: Advanced life support: 2015 International Consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations. Resuscitation 95:e71-120. https://doi.org/10.1016/j.resuscitation.2015.07.042
Albert CM, McGovern BA, Newell JB, Ruskin JN (1996) Sex differences in cardiac arrest survivors. Circulation 93(6):1170–1176. https://doi.org/10.1161/01.cir.93.6.1170
Tunstall-Pedoe H, Morrison C, Woodward M, Fitzpatrick B, Watt G (1996) Sex differences in myocardial infarction and coronary deaths in the Scottish MONICA population of Glasgow 1985 to 1991. Presentation, diagnosis, treatment, and 28-day case fatality of 3991 events in men and 1551 events in women. Circulation 93(11):1981–1992. https://doi.org/10.1161/01.cir.93.11.1981
Wigginton JG, Perman SM, Barr GC, McGregor AJ, Miller AC, Napoli AF, Safdar B, Weaver KR, Deutsch S, Kayea T, Becker L (2014) Sex- and gender-specific research priorities in cardiovascular resuscitation: proceedings from the 2014 academic emergency medicine consensus conference cardiovascular resuscitation research workgroup. Acad Emerg Med 21(12):1343–1349. https://doi.org/10.1111/acem.12541
Zhai P, Eurell TE, Cotthaus R, Jeffery EH, Bahr JM, Gross DR (2000) Effect of estrogen on global myocardial ischemia-reperfusion injury in female rats. Am J Physiol Heart Circ Physiol 279(6):H2766-2775. https://doi.org/10.1152/ajpheart.2000.279.6.H2766
Sivasinprasasn S, Tanajak P, Pongkan W, Pratchayasakul W, Chattipakorn SC, Chattipakorn N (2017) DPP-4 inhibitor and estrogen share similar efficacy against cardiac ischemic-reperfusion injury in obese-insulin resistant and estrogen-deprived female rats. Sci Rep 7:44306. https://doi.org/10.1038/srep44306
Noppens RR, Kofler J, Grafe MR, Hurn PD, Traystman RJ (2009) Estradiol after cardiac arrest and cardiopulmonary resuscitation is neuroprotective and mediated through estrogen receptor-beta. J Cereb Blood Flow Metab Off J Intern Soc Cereb Blood Flow Metab 29(2):277–286. https://doi.org/10.1038/jcbfm.2008.116
Hutchens MP, Nakano T, Kosaka Y, Dunlap J, Zhang W, Herson PS, Murphy SJ, Anderson S, Hurn PD (2010) Estrogen is renoprotective via a nonreceptor-dependent mechanism after cardiac arrest in vivo. Anesthesiology 112(2):395–405. https://doi.org/10.1097/ALN.0b013e3181c98da9
Lang JT, McCullough LD (2008) Pathways to ischemic neuronal cell death: are sex differences relevant? J Transl Med 6:33. https://doi.org/10.1186/1479-5876-6-33
Herson PS, Palmateer J, Hurn PD (2013) Biological sex and mechanisms of ischemic brain injury. Transl Stroke Res 4(4):413–419. https://doi.org/10.1007/s12975-012-0238-x
Semenas E, Nozari A, Wiklund L (2010) Sex differences in cardiac injury after severe haemorrhage and ventricular fibrillation in pigs. Resuscitation 81(12):1718–1722. https://doi.org/10.1016/j.resuscitation.2010.08.010
Cao Z, Liu L, Packwood W, Merkel M, Hurn PD, Van Winkle DM (2008) Sex differences in the mechanism of Met5-enkephalin-induced cardioprotection: role of PI3K/Akt. Am J Physiol Heart Circ Physiol 294(1):H302-310. https://doi.org/10.1152/ajpheart.00845.2007
Acknowledgements
We would like to thank Editage (www.editage.cn) for English language editing.
Funding
The work was supported by the National Key R&D Program of China (No. 2016YFC1301100). They funded the collection of the data and revision of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Statement of human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Feng, D., Li, C., Yang, X. et al. Gender differences and survival after an out-of-hospital cardiac arrest: a systematic review and meta-analysis. Intern Emerg Med 16, 765–775 (2021). https://doi.org/10.1007/s11739-020-02552-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-020-02552-4