Abstract
Background
Bariatric surgery (BS) can lead to bone loss and an increased fracture risk.
Methods
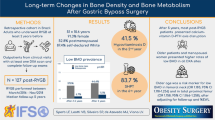
To determine the morphometric vertebral fracture (MVF) prevalence, and its relationship with bone mineral density (BMD), and biomarker’s turnover after Roux-en-Y gastric bypass (RYGB) and sleeve gastrectomy (SG), we analyzed post-surgery X-rays of the spine in 80 patients (88% female, 51% RYGB, age 41.2 [6.8] years) from 117 participants’ retrospective cohort (1–2 years, >2 and <5 years, and >5 years). We still analyzed body composition and BMD by dual-energy X-ray absorptiometry and bone parameters.
Results
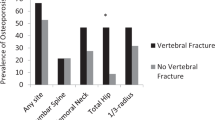
MVF prevalence was 17.5% (14/80), with no statistical difference between groups (p = 0.210). RYGB group had a higher prevalence of secondary hyperparathyroidism (SHPT) (PTH ≥ 65 pg/ml; 18.4% vs 7.8%, respectively, p = 0.04), PTH (61.3 vs 49.5 pg/ml, p = 0.001), CTX (0.766 [0.29] ng/ml vs 0.453 [0.30] ng/ml, p = 0.037), and AP (101.3 [62.4] U/L vs 123.9 [60.9] U/L, p = 0.027) than the SG group. Up to 5 years postoperatively, RYGB had a lower total (1.200 [0.087] vs 1.236 [0.100] g/cm2, p = 0.02), femoral neck (1.034 [0.110] vs 1.267 [0.105], p = 0.005), and total femur BMD (1.256 [0.155] vs 1.323 [0.167], p = 0.002) than SG group. We found no statistically significant difference between the MFV (+) and MVF (−) groups regarding age, sex, BMI, surgery time, BMD, or bone and metabolic parameters, including leptin.
Conclusion
We found a high prevalence of MVF after BS with no differences between RYGB and SG.
Graphical Abstract


Similar content being viewed by others
References
FAO, IFAD, UNICEF, WFP, WHO. 2019. The State of Food Security and Nutrition in the World 2019. Safeguarding against economic slowdowns and downturns. Rome, FAO. Licence: CC BY-NC-SA 3.0 IGO.
Di Cesare M, Sorić M, Bovet P, et al. The epidemiological burden of obesity in childhood: a worldwide epidemic requiring urgentaction. BMC Med. 2019;17(1):212. Epub 20191125. 10.1186/s12916-019-1449-8.PubMed PMID: 31760948; PubMed Central PMCID: PMC6876113
Blüher M. Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15(5):288–98. https://doi.org/10.1038/s41574-019-0176-8.
Welbourn R, Hollyman M, Kinsman R, et al. Bariatric surgery worldwide: baseline demographic description and one-year outcomes from the fourth IFSO Global Registry Report 2018. Obes Surg. 2019;29(3):782–95. Epub20181112. https://doi.org/10.1007/s11695-018-3593-1.
Zhang Q, Dong J, Zhou D, et al. Comparative risk of fracture for bariatric procedures in patients with obesity: a systematic review and Bayesian network meta-analysis. Int J Surg. 2020;75:13–23. Epub 20200121. https://doi.org/10.1016/j.ijsu.2020.01.018.
Marcil G, Bourget-Murray J, Shinde S, et al. The incidence of fractures following bariatric surgery: a systematic review. International Journal of Surgery Open. 2018; https://doi.org/10.1016/j.ijso.2018.08.005.
Rousseau C, Jean S, Gamache P, et al. Change infracture risk and fracture pattern after bariatric surgery: nested case-control study. BMJ. 2016;354:i3794. https://doi.org/10.1136/bmj.i3794. Epub 20160727. PubMed PMID:27814663; PubMed Central PMCID: PMC4964103
Holanda N, Crispim N, Carlos I, et al. Musculoskeletal effects of obesity and bariatric surgery - a narrative review. Arch. Endocrinol Metab. 2022;66(5):621–32. https://doi.org/10.20945/2359-3997000000551.
Pereira C, de Holanda N, de Lima CI, et al. Fracture risk after bariatric surgery: a systematic literature review and meta-analysis. EndocrPract. 2022;28(1):58–69. https://doi.org/10.1016/j.eprac.2021.09.007. Epub 20210923. PubMedPMID: 34563701
Yu EW, Bouxsein ML, Putman MS, et al. Two-year changes in bone density after Roux-en-Y gastric bypass surgery. J Clin Endocrinol Metab. 2015;100(4):1452–9. https://doi.org/10.1210/jc.2014-4341. Epub 20150203. PubMed PMID: 25646793; PubMed Central PMCID: PMC4399296
Gagnon C, Schafer AL. Bone health after bariatric surgery. JBMR Plus. 2018;2(3):121–33. https://doi.org/10.1002/jbm4.10048. Epub 20180501. PubMed PMID:30283897; PubMed Central PMCID: PMC6124196
Lindeman KG, Greenblatt LB, Rourke C, et al. Longitudinal 5-year evaluation of bone density and microarchitecture after Roux-en-Y gastric bypass surgery. J Clin Endocrinol Metab. 2018;103(11):4104–12. https://doi.org/10.1210/jc.2018-01496. PubMed PMID: 30219833; PubMed Central PMCID:PMC6194805
Bandeira F. Asymptomatic vertebral fracture: a wolf in sheep’s clothing? ArchEndocrinol Metab. 2015; https://doi.org/10.1590/2359-3997000000017
Johansson L, Sundh D, Magnusson P, et al. Grade 1 vertebral fractures identified by densitometric lateral spine imaging predict incident major osteoporotic fracture independently of clinical risk factors and bone mineral density in older women. J Bone Miner Res. 2020;35(10):1942–51. https://doi.org/10.1002/jbmr.4108.
Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. Hillsdale, NJ: Lawrence Erlbaum Associates, Publishers; 1988
Craig CL, Marshall AL, Sjöström M, et al. International physical activity questionnaire: 12-country reliability and validity. Med SciSports Exerc. 2003;35(8):1381–95. https://doi.org/10.1249/01.MSS.0000078924.61453.FB.PubMed.
Sichieri R, Everhart JE. O Validity of a Brazilian food frequency questionnaire against dietary recalls and estimated energy intake. Nutrition Research. 1998, ISSN 0271-5317,;18(10) https://doi.org/10.1016/S0271-5317(98)00151-1.
Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000;894:i-xii, 1-253
Genant HK, Wu CY, van Kuijk C, et al. Vertebral fracture assessment using asemiquantitative technique. J Bone Miner Res. 1993;8(9):1137–48. https://doi.org/10.1002/jbmr.5650080915.
Clark P, Cons-Molina F, Deleze M, et al. The prevalence of radiographic vertebral fractures in Latin American countries: the Latin American Vertebral Osteoporosis Study (LAVOS). Osteoporos Int. 2009;20(2):275–82. https://doi.org/10.1007/s00198-008-0657-4.
Blom-Høgestøl IK, Hewitt S, Chahal-Kummen M, et al. Bone metabolism, bone mineral density and low-energy fractures 10 years after Roux-en-Y gastric bypass. Bone. 2019;127:436–45. https://doi.org/10.1016/j.bone.2019.07.014. Epub 2019 Jul 16
Ferrar L, Jiang G, Cawthon PM, et al. Identification of vertebral fracture and non-osteoporotic short vertebral height in men: the MrOS study. J Bone Miner Res. 2007;22(9):1434–41. https://doi.org/10.1359/jbmr.070608.PubMed.
Nakamura KM, Haglind EG, Clowes JA, et al. Fracture risk following bariatric surgery: a population-based study. Osteoporos Int. 2014;25(1):151–8. https://doi.org/10.1007/s00198-013-2463-x.
Paccou J, Martignène N, Lespessailles E, et al. Gastric bypass but not sleeve gastrectomy increases risk of major osteoporotic fracture: French population-based cohort study. J Bone Miner Res. 2020;35(8):1415–23. Epub 20200416. https://doi.org/10.1002/jbmr.4012.
Maghrabi AH, Wolski K, Abood B, et al. Two-year outcomes on bone density and fracture incidence in patients with T2DM randomized to bariatric surgery versus intensive medical therapy. Obesity (Silver Spring). 2015;23(12):2344–8. https://doi.org/10.1002/oby.21150. PubMed PMID:26193177; PubMed Central PMCID: PMC4701611
Holanda NCP, Baad VMA, Bezerra LR, et al. Secondary hyperparathyroidism, bone density, and bone turn over after bariatric surgery: differences between Roux-en-Y gastric bypass and sleeve gastrectomy. Obes Surg. 2021;31(12):5367–75. Epub 20211012. https://doi.org/10.1007/s11695-021-05739-6.
Vix M, Liu KH, Diana M, et al. Impact of Roux-en-Y gastric bypass versus sleeve gastrectomy on vitamin D metabolism: short-term results from a prospective randomized clinical trial. Surg Endosc. 2014;28(3):821–6. Epub20131107. https://doi.org/10.1007/s00464-013-3276-x.
Bouxsein ML, Eastell R, Liu LY, et al. Reply to: Change in bone density and reduction in fracture risk: a meta-regression of published trials. J Bone Miner Res. 2019;34(10):1977–8. https://doi.org/10.1002/jbmr.3837.
Premaor MO, Ensrud K, Lui L, Parker RA, Cauley J, Hillier TA, et al. Risk factors for nonvertebral fracture in obese older women. J Clin Endocrinol Metab. 2011;96(8):2414–21. https://doi.org/10.1210/jc.2011-0076. Epub 20110615. PubMed PMID:21677038; PubMed Central PMCID: PMC3146794
Bandeira F. Does obesity really strengthens the bones? Arq Bras Endocrinol Metabol. 2007;51(6):895–7. https://doi.org/10.1590/s0004-27302007000600001.
Krez AN, Stein EM. The skeletal consequences of bariatric surgery. Curr Osteoporos Rep. 2020;18(3):262–72. https://doi.org/10.1007/s11914-020-00579-2. PubMedPMID: 32249380
Berardi G, Vitiello A, Abu-Abeid A, Schiavone V, Franzese A, Velotti N, Musella M. Micronutrients deficiencies in candidates of bariatric surgery: results from a single institution over a 1-year period. Obes Surg. 2023;33(1):212–8. https://doi.org/10.1007/s11695-022-06355-8. Epub 2022 Nov 4. PMID: 36331725; PMCID: PMC9834098
Funding
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior–Brasil (CAPES) [Finance Code 001].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• There was a high prevalence of MVF after BS (17.5%), with no differences between RYGB and SG.
• High serum CTX concentrations were independently associated with MVF.
• After 5 years, RYGB group had lower BMD and higher serum PTH than SG group.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Holanda, N.C.P., Silva, T.I.A.R., Cavalcante, A.G. et al. Prevalence of Morphometric Vertebral Fractures After Bariatric Surgery and Its Relationship with Bone Mineral Density and Bone Markers. OBES SURG 34, 733–740 (2024). https://doi.org/10.1007/s11695-023-07049-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-07049-5