Abstract
Introduction
Genetic obesity susceptibility in postoperative bariatric surgery weight regain (PBSWR) remains largely unexplored.
Methods
A retrospective case series of adult (N = 27) PBSWR patients who had undergone genetic obesity testing was conducted between Sept. 2020 and March 2022. Primary outcome: frequency of genetic variants in patients experiencing weight regain following bariatric surgery. Secondary outcomes: prevalence of obesity-related comorbidities, nadir BMI achieved post-bariatric surgery, and percent total body weight loss (%TBWL) achieved with obesity pharmacotherapies.
Results
Heterozygous mutations were identified in 22 (81%) patients, with the most prevalent mutations occurring in CEP290, RPGR1P1L, and LEPR genes (3 patients each). Median age was 56 years (interquartile range (IQR) 46.8–65.5), 88% female. Types of surgery were 67% RYGB, 19% SG, 4% gastric band, and 13% revisions. Median nadir BMI postoperatively was 34.0 kg/m2 (IQR 29.0–38.5). A high prevalence of metabolic derangements was noted; patients presented median 80 months (IQR 39–168.5) postoperative for medical weight management with 40% weight regain. BMI at initiation of anti-obesity medication (AOMs) was 41.7 kg/m2 (36.8–44.4). All received AOM and required at least 3 AOMs for weight regain. Semaglutide (N = 21), topiramate (N = 14), and metformin (N = 12) were most prescribed. Median %TBWL for the cohort at the first, second, and third visit was 1.7, 5.0, and 6.5 respectively. Fourteen (52%) achieved 5%TBWL, 10 (37%) achieved 10%TBWL, and 4 (15%) achieved 15%TBWL with combination AOMs and supervised medical intervention.
Conclusion
An unusually high prevalence of genetic obesity variants in PBSWR was found, warranting further research.
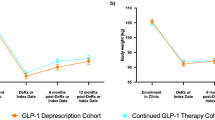
Graphical Abstract

Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, GS, upon reasonable request.
Abbreviations
- PBSWR:
-
Post-bariatric surgery weight regain
- GLP-1RA:
-
Glucagon-like peptide 1 receptor agonists
- MWL:
-
Medical weight loss clinic
- AOM:
-
Anti-obesity medications
- TBW:
-
Total body weight
- T2DM:
-
Type 2 diabetes mellitus
References
King WC, Hinerman AS, Courcoulas AP. Weight regain after bariatric surgery: a systematic literature review and comparison across studies using a large reference sample. Surg Obes Rel Dis. 2020;16(8):1133–44. https://doi.org/10.1016/j.soard.2020.03.034.
van Baak MA, Mariman ECM. Mechanisms of weight regain after weight loss - the role of adipose tissue. Nat Rev Endocrinol. 2019;15(5):274–87. https://doi.org/10.1038/s41574-018-0148-4.
Malhotra S, Sivasubramanian R, Srivastava G. Evaluation and management of early onset genetic obesity in childhood. J Pediatr Genet. 2021;10(3):194–204. https://doi.org/10.1055/s-0041-1731035.
Wardle J, Carnell S, Haworth CM, Plomin R. Evidence for a strong genetic influence on childhood adiposity despite the force of the obesogenic environment. Am J Clin Nutr. 2008;87(2):398–404. https://doi.org/10.1093/ajcn/87.2.398.
Clement K, Mosbah H, Poitou C. Rare genetic forms of obesity: from gene to therapy. Physiol Behav. 2020;227:113134. https://doi.org/10.1016/j.physbeh.2020.113134.
Malhotra S, Sivasubramanian R, Srivastava G. Evaluation and mangement of early onset genetic obesity in childhood. J Pediatr Genet. 2021. https://doi.org/10.1055/s-0041-1731035.
Farooqi S. Insights from the genetics of severe childhood obesity. Horm Res. 2007;68(Suppl 5):5–7. https://doi.org/10.1159/000110462.
Huvenne H, Dubern B, Clement K, Poitou C. Rare genetic forms of obesity: clinical approach and current treatments in 2016. Obes Facts. 2016;9(3):158–73. https://doi.org/10.1159/000445061.
Kleinendorst L, Abawi O, van der Kamp HJ, Alders M, Meijers-Heijboer HEJ, van Rossum EFC, et al. Leptin receptor deficiency: a systematic literature review and prevalence estimation based on population genetics. Eur J Endocrinol. 2020;182(1):47–56. https://doi.org/10.1530/EJE-19-0678.
Markham A. Setmelanotide: first approval. Drugs. 2021;81(3):397–403. https://doi.org/10.1007/s40265-021-01470-9.
Srivastava G, Buffington C. A Specialized medical management program to address post-operative weight regain in bariatric patients. Obes Surg. 2018;28(8):2241–6. https://doi.org/10.1007/s11695-018-3141-z.
Cooiman MI, Kleinendorst L, Aarts EO, Janssen IMC, van Amstel HKP, Blakemore AI, et al. Genetic obesity and bariatric surgery outcome in 1014 patients with morbid obesity. Obes Surg. 2020;30(2):470–7. https://doi.org/10.1007/s11695-019-04184-w.
Sivasubramanian R, Malhotra S. Genetic contributors to obesity. Gastroenterol Clin North Am. 2023;52(2):323–32. https://doi.org/10.1016/j.gtc.2023.03.005.
Tamaroff J, Williamson D, Slaughter JC, Xu M, Srivastava G, Shoemaker AH. Prevalence of genetic causes of obesity in clinical practice. Obes Sci Pract. 2023;9(5):508–15. https://doi.org/10.1002/osp4.671.
Sarzynski MA, Jacobson P, Rankinen T, Carlsson B, Sjostrom L, Bouchard C, et al. Associations of markers in 11 obesity candidate genes with maximal weight loss and weight regain in the SOS bariatric surgery cases. Int J Obes (Lond). 2011;35(5):676–83. https://doi.org/10.1038/ijo.2010.166.
Bonnefond A, Keller R, Meyre D, Stutzmann F, Thuillier D, Stefanov DG, et al. Eating behavior, low-frequency functional mutations in the melanocortin-4 receptor (MC4R) gene, and outcomes of bariatric operations: a 6-year prospective study. Diabetes Care. 2016;39(8):1384–92. https://doi.org/10.2337/dc16-0115.
Sket R, Kotnik P, Bizjan BJ, Kocen V, Mlinaric M, Tesovnik T, et al. Heterozygous genetic variants in autosomal recessive genes of the leptin-melanocortin signalling pathway are associated with the development of childhood obesity. Front Endocrinol. 2022;13:832911. https://doi.org/10.3389/fendo.2022.832911.
Campos A, Cifuentes L, Hashem A, Busebee B, Hurtado-Andrade MD, Ricardo-Silgado ML, et al. Effects of heterozygous variants in the leptin-melanocortin pathway on Roux-en-Y Gastric bypass outcomes: a 15-year case-control study. Obes Surg. 2022;32(8):2632–40. https://doi.org/10.1007/s11695-022-06122-9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
For this type of study, formal consent is not required.
Informed Consent
Informed consent does not apply.
Conflict of Interest
GS discloses consulting fees from Rhythm, Novo Nordisk, and Eli Lilly outside the submitted work. JMS, NUP, AR, and AM report no financial conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Heterozygous, Single-allele mutations are common in patients with childhood obesity.
• These mutations appear to impact weight loss after bariatric surgery.
• Early testing for monogenic causes of obesity may be warranted in this cohort.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Samuels, J.M., Paddu, N.U., Rekulapeli, A. et al. High Prevalence of Positive Genetic Obesity Variants in Postoperative Bariatric Surgery Patients with Weight Regain Presenting for Medical Obesity Intervention. OBES SURG 34, 170–175 (2024). https://doi.org/10.1007/s11695-023-06952-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06952-1