Abstract
Background
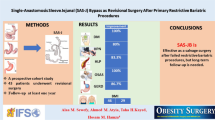
In comparison with purely restrictive procedures, combined restrictive and malabsorptive procedures seem to produce better weight loss and comorbidity control in patients with morbid obesity. Two-stage bariatric surgery is popular and is a safe and efficient strategy for patients with super obesity (BMI > 50 kg/m2) and super-super obesity (BMI > 60 kg/m2).
Methods
The patient in this video was a 36-year-old man with an initial BMI of 53.2 kg/m2. Two-stage bariatric surgery was planned. The patient underwent the first stage, laparoscopic sleeve gastrectomy, in 2018. Eighteen months after surgery, his lowest BMI was 38.8 kg/m2, and his excess weight loss was 50.9%. In 2021, he regained weight and reached a BMI of 42.4 kg/m2. Then, a second-stage bariatric surgery was performed.
Results
As shown in the video, combined re-sleeve and single anastomosis sleeve ileal (SASI) bypass constituted the second stage of bariatric surgery. During the operation, adhesiolysis was first performed, and the stomach was mobilized through a lateral-to-medial approach. Gastric transection was performed with a 36-Fr bougie. Then, the ileocecal junction was identified, and a location 250 cm from the cecum was selected as the anastomosis site. Gastro-ileal anastomosis (3 cm in diameter) was established with a stapler, and the two-layer suture method was used to close the defect. The postoperative period was uneventful, and the patient was discharged 5 days after surgery.
Conclusions
Combined re-sleeve and SASI bypass has a few surgical morbidities and is promising as an alternative to second-stage duodenal switch in patients with super obesity.
Similar content being viewed by others
References
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes - 5-year outcomes. N Engl J Med. 2017;376(7):641–51.
Hess DS, Hess DW. Biliopancreatic diversion with a duodenal switch. Obes Surg. 1998;8(3):267–82.
Angrisani L, Santonicola A, Iovino P, et al. IFSO worldwide survey 2016: primary, endoluminal, and revisional procedures. Obes Surg. 2018;28(12):3783–94.
Lauti M, Kularatna M, Hill AG, et al. Weight regain following sleeve gastrectomy-a systematic review. Obes Surg. 2016;26(6):1326–34.
Alexandrou A, Felekouras E, Giannopoulos A, et al. What is the actual fate of super-morbid-obese patients who undergo laparoscopic sleeve gastrectomy as the first step of a two-stage weight-reduction operative strategy? Obes Surg. 2012;22(10):1623–8.
Andalib A, Alamri H, Almuhanna Y, et al. Short-term outcomes of revisional surgery after sleeve gastrectomy: a comparative analysis of re-sleeve, Roux en-Y gastric bypass, duodenal switch (Roux en-Y and single-anastomosis). Surg Endosc. 2020.
AlSabah S, Alsharqawi N, Almulla A, et al. Approach to poor weight loss after laparoscopic sleeve gastrectomy: re-sleeve vs. gastric bypass. Obes Surg. 2016;26(10):2302–7.
Rayman S, Assaf D, Azran C, et al. Sleeve gastrectomy failure-revision to laparoscopic one-anastomosis gastric bypass or Roux-n-Y gastric bypass: a multicenter study. Obes Surg. 2021.
Lee Y, Ellenbogen Y, Doumouras AG, et al. Single- or double-anastomosis duodenal switch versus Roux-en-Y gastric bypass as a revisional procedure for sleeve gastrectomy: a systematic review and meta-analysis. Surg Obes Relat Dis : Off J Am Soc Bariatric Surg. 2019;15(4):556–66.
Shimon O, Keidar A, Orgad R, et al. Long-term effectiveness of laparoscopic conversion of sleeve gastrectomy to a biliopancreatic diversion with a duodenal switch or a Roux-en-Y gastric bypass due to weight loss failure. Obes Surg. 2018;28(6):1724–30.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Anderson B, Gill RS, de Gara CJ, et al. Biliopancreatic diversion: the effectiveness of duodenal switch and its limitations. Gastroenterol Res Pract. 2013;2013:974762.
Sánchez-Pernaute A, Rubio M, Conde M, et al. Single-anastomosis duodenoileal bypass as a second step after sleeve gastrectomy. Surg Obes Relat Dis : Off J Am Soc Bariatric Surg. 2015;11(2):351–5.
Hassan I. A337 single anastomosis sleeve ileal (SASI) bypass: an option for weight regain after sleeve gastrectomy. Surg Obesity Relat Dis. 2019;15(10):S138–9. https://doi.org/10.1016/j.soard.2019.08.281.
Mahdy T, Al Wahedi A, Schou C. Efficacy of single anastomosis sleeve ileal (SASI) bypass for type-2 diabetic morbid obese patients: gastric bipartition, a novel metabolic surgery procedure: a retrospective cohort study. Int J Surg. 2016;34:28–34.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Single anastomosis sleeve ileal (SASI) bypass is a novel bariatric procedure, containing restrictive and malabsorptive effects.
• Two-stage bariatric surgery has fewer surgical risks and is preferred in patients with BMI > 50 kg/m2.
• We present a practical approach of combined re-sleeve and SASI bypass as a 2nd-stage post laparoscopic sleeve gastrectomy.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 82451 KB)
Rights and permissions
About this article
Cite this article
Hsu, FC., Pan, HM., Wang, RT. et al. Combined Re-sleeve and Single Anastomosis Sleeve Ileal (SASI) Bypass as a Second Stage After Sleeve Gastrectomy (Video Report). OBES SURG 31, 5514–5516 (2021). https://doi.org/10.1007/s11695-021-05737-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05737-8