Abstract
Purpose
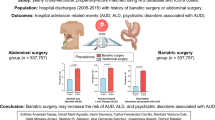
Individuals that undergo bariatric surgery are at higher risk for problematic alcohol use via pharmacokinetic changes in alcohol metabolism and cross addictions. Little data exists regarding post-bariatric surgery patients with alcohol-related liver disease (ALD) who ultimately require liver transplantation. The aim of this project was to better understand demographic, medical, and psychological characteristics of post-bariatric surgery patients who undergo liver transplantation due to ALD.
Methods
This retrospective clinical cohort identified 1416 patients who underwent ALD liver transplantation over a 10-year timespan at three academic medical centers. Electronic medical records were reviewed for patient characteristics, including sex, age, body mass index, surgery dates, Model for End Stage Liver Disease (MELD) scores, medical history, psychiatric history, and mortality rates.
Results
Within the sample of liver transplantation patients, 1.3% had undergone bariatric surgery prior to transplantation. Fifty percent of the post-bariatric surgery sample was female. The MELD score was higher and the median age at transplantation was younger in the post-bariatric surgery subgroup in comparison to that in the non-bariatric surgery patients. Mood and anxiety disorders were more common among those with a history of having bariatric surgery, with major depressive disorder having the largest difference between subgroups.
Conclusions
Among patients who require a liver transplantation due to ALD, those with a history of bariatric surgery are more likely to be female, younger, and diagnosed with mood disorders. Further studies with larger and more diverse samples are necessary to better understand how to prevent development of alcohol use disorder in the bariatric surgery population.
Graphical abstract

Similar content being viewed by others
References
Arterburn DE, Telem DA, Kushner RF, et al. Benefits and risks of bariatric surgery in adults: a review. Jama. 2020;324(9):879–87.
Klockhoff H, Näslund I, Jones AW. Faster absorption of ethanol and higher peak concentration in women after gastric bypass surgery. Br J Clin Pharmacol. 2002;54(6):587–91.
Hagedorn JC, Encarnacion B, Brat GA, et al. Does gastric bypass alter alcohol metabolism? Surg Obes Relat Dis. 2007;3(5):543–8. discussion 8
Maluenda F, Csendes A, De Aretxabala X, et al. Alcohol absorption modification after a laparoscopic sleeve gastrectomy due to obesity. Obes Surg. 2010;20(6):744–8.
Woodard GA, Downey J, Hernandez-Boussard T, et al. Impaired alcohol metabolism after gastric bypass surgery: a case-crossover trial. J Am Coll Surg. 2011;212(2):209–14.
King WC, Chen JY, Courcoulas AP, et al. Alcohol and other substance use after bariatric surgery: prospective evidence from a U.S. multicenter cohort study. Surg Obes Relat Dis. 2017;13(8):1392–402.
Ibrahim N, Alameddine M, Brennan J, et al. New onset alcohol use disorder following bariatric surgery. Surg Endosc. 2019;33(8):2521–30.
Cuellar-Barboza AB, Frye MA, Grothe K, et al. Change in consumption patterns for treatment-seeking patients with alcohol use disorder post-bariatric surgery. J Psychosom Res. 2015;78(3):199–204.
King WC, Chen J-Y, Mitchell JE, et al. Prevalence of alcohol use disorders before and after bariatric surgery. JAMA. 2012;307(23):2516–25.
Li L, Wu L-T. Substance use after bariatric surgery: a review. J Psychiatr Res. 2016;76:16–29.
Smith KE, Engel SG, Steffen KJ, et al. Problematic alcohol use and associated characteristics following bariatric surgery. Obes Surg. 2018;28(5):1248–54.
Lassailly G, Caiazzo R, Buob D, et al. Bariatric surgery reduces features of nonalcoholic steatohepatitis in morbidly obese patients. Gastroenterology. 2015;149(2):379–88. quiz e15-6
Mittal S, Sada YH, El-Serag HB, et al. Temporal trends of nonalcoholic fatty liver disease-related hepatocellular carcinoma in the veteran affairs population. Clin Gastroenterol Hepatol. 2015;13(3):594–601. e1
Nguyen DM, El-Serag HB. The big burden of obesity. Gastrointest Endosc. 2009;70(4):752–7.
Mathurin P, Gonzalez F, Kerdraon O, et al. The evolution of severe steatosis after bariatric surgery is related to insulin resistance. Gastroenterology. 2006;130(6):1617–24.
Mathurin P, Hollebecque A, Arnalsteen L, et al. Prospective study of the long-term effects of bariatric surgery on liver injury in patients without advanced disease. Gastroenterology. 2009;137(2):532–40.
Caiazzo R, Lassailly G, Leteurtre E, et al. Roux-en-Y gastric bypass versus adjustable gastric banding to reduce nonalcoholic fatty liver disease: a 5-year controlled longitudinal study. Ann Surg. 2014;260(5):893–8. discussion 8-9
Addolorato G, Mirijello A, Leggio L, et al. Management of alcohol dependence in patients with liver disease. CNS Drugs. 2013;27(4):287–99.
National Institute on Alcohol Abuse and Alcoholism. Drinking Levels Defined: National Institutes of Health; 2021 [Available from: https://www.niaaa.nih.gov/alcohol-health/overview-alcohol-consumption/moderate-binge-drinking. Accessed 23 Oct 2020
van der Meer AJ, Veldt BJ, Feld JJ, et al. Association between sustained virological response and all-cause mortality among patients with chronic hepatitis C and advanced hepatic fibrosis. Jama. 2012;308(24):2584–93.
Stepanova M, Wai H, Saab S, et al. The portrait of an adult liver transplant recipient in the United States from 1987 to 2013. JAMA Intern Med. 2014;174(8):1407–9.
Carlsson LMS, Sjöholm K, Jacobson P, et al. Life expectancy after bariatric surgery in the Swedish Obese Subjects study. N Engl J Med. 2020;383(16):1535–43.
Safwan M, Collins KM, Abouljoud MS, et al. Outcome of liver transplantation in patients with prior bariatric surgery. Liver Transpl. 2017;23(11):1415–21.
Clark MM, Hanna BK, Mai JL, et al. Sexual abuse survivors and psychiatric hospitalization after bariatric surgery. Obes Surg. 2007;17(4):465–9.
Goetze RE, Clark MM, Rakocevic DB, et al. Cannabis use and bariatric surgery psychology practice: survey and insights. Surg Obes Relat Dis. 2021;17(4):701–10.
Nielsen JK, Olafsson S, Bergmann OM, et al. Lifetime drinking history in patients with alcoholic liver disease and patients with alcohol use disorder without liver disease. Scand J Gastroenterol. 2017;52(6-7):762–7.
Ivezaj V, Benoit SC, Davis J, et al. Changes in alcohol use after metabolic and bariatric surgery: predictors and mechanisms. Curr Psychiatry Rep. 2019;21(9):85.
Reaves DL, Dickson JM, Halford JCG, et al. A qualitative analysis of problematic and non-problematic alcohol use after bariatric surgery. Obes Surg. 2019;29(7):2200–9.
Holgerson AA, Clark MM, Frye MA, et al. Symptoms of bipolar disorder are associated with lower bariatric surgery completion rates and higher food addiction. Eat Behav. 2021;40:101462.
Cunningham JL, Merrell CC, Sarr M, et al. Investigation of antidepressant medication usage after bariatric surgery. Obes Surg. 2012;22(4):530–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
For this type of study, formal consent is not required.
Consent to Participate
Informed consent does not apply.
Conflict of Interest
Matthew M. Clark, Ph.D., is a consultant for Roche Diabetes Care GmbH. All other authors declare that they have no potential conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Individuals that undergo bariatric surgery are at higher risk for problematic alcohol use via pharmacokinetic changes in alcohol metabolism and cross addictions.
• Little data exists regarding post-bariatric surgery patients with alcohol-related liver disease (ALD) who ultimately require liver transplantation.
• From the results of this retrospective clinical cohort: Among patients who require a liver transplantation due to ALD, those with a history of bariatric surgery are more likely to be younger, be female, have higher MELD scores, and be diagnosed with mood disorders.
Rights and permissions
About this article
Cite this article
Fipps, D.C., Goetze, R.E., Clark, M.M. et al. Liver Transplantation After Bariatric Surgery: a Clinical Cohort Study. OBES SURG 31, 3700–3706 (2021). https://doi.org/10.1007/s11695-021-05483-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05483-x